About the Program
Program Highlights

Our Focus
The Anesthesiology Residency Program at the University of Rochester Medical Center is dedicated to the education and development of the next generation of anesthesiologists. Our program has a proven track record of graduating highly trained and qualified doctors who have completed 2-3 times the required ACGME clinical case load and who score above the national average on board examinations.
Our Program at a Glance


Top 10 Reasons for Choosing Our Program
1. Integrated Program
First year residents (CBY) have early and extended experience in the OR (at least 13 weeks) with several months of CBY "floor" rotations deferred to CA1 and 2 years and paired with anesthesiology subspecialty rotations.
2. Non-Clinical Residency Tracks
Residents can complete graduate course work while working towards a master’s degree or certificate in Medical Education, Medical Management, Translational Research, and more. The clinical schedule is adjusted to accommodate for classes and course work. As University employees, residents are eligible for a 95% tuition waver!
3. Case Variety, Complexity, and Exposure
We house the only Level 1 trauma and burn center, liver and heart transplant center, high-risk OB ward, and pediatric hospital in the region. Our residents routinely complete 2-3 times the minimum number of index cases required by the ACGME:
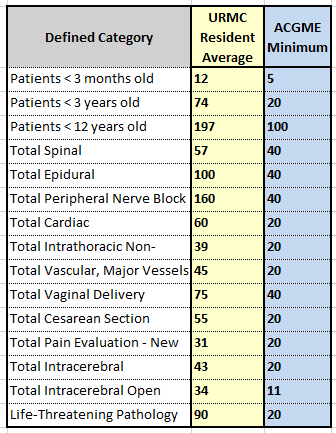
4. Friendly, Family-Oriented Atmosphere
Rochester has a Midwest feel... on steroids! People are super nice, almost annoyingly so. It’s an adjustment coming from the East Coast. Here is what our residents said about the work atmosphere in an anonymous survey:
“There are fantastic faculty who are always willing to teach and serve as mentors for residents.”
“Collegial, supportive, provides ample resources towards furthering resident education.”
“Great support staff, willing to listen and make changes.”
“The teaching is phenomenal, and the attendings are approachable.”
“Friendly working environment...”
“Responsive to concerns, feel heard.”
“This program is within an intimate community of healthcare providers. Great mentorship and feedback.”
5. Anesthesiology Residency Education Innovators!
Our mission is to be a leader and innovator in anesthesiology education. This is evident in our curriculum with the integrated, categorical residency program, CBY rotations which emphasize perioperative medicine, non-clinical residency tracks, protected didactic time, Point-of-Care Ultrasound (POCUS) training, our approach to resident wellness, and so much more. We rolled out a rural/community anesthesia elective during the 2020-21 academic year, and hope to start a rural residency track based in our rural affiliated community hospitals in the near future. We are also considering offering a “European” style residency track which will incorporate a Critical Care fellowship in an innovative 5 year residency program.
6. Interactive and Experiential Educational Activities
Death by PowerPoint is an excruciatingly painful way to go. All of our non-clinical educational activities are designed to be as hands-on and interactive as possible. From PBLDs and case discussions to simulations, OSCEs, task training on mannequins, and POCUS, interdisciplinary activities are valued since we work with healthcare professionals from so many disciplines. We incorporate many interactive experiences into our residents’ education to make it interesting and meaningful.
Protected didactic time allows a class of residents to focus on interactive and experiential learning activities dedicated to subspecialty and other focused anesthesia topics free from clinical distractions.
Confession sessions are a staple of our curriculum and allow residents to raise concerns and feedback anonymously and discuss them openly with the program director.
8. One Central Location
90% of clinical rotations occur on the University of Rochester Medical Center campus with the rest of the required clinical experiences taking place within a 1 mile radius.
9. Geography
Rochester isn’t Westchester! It’s affordable. It’s family friendly. There is no congestion. It is clean, and has wonderful parks and lakes. And, we naturally enjoy our social distance! Rochester is within driving distance to major metropolitan areas, such as New York City, Philadelphia, Boston, Toronto, and Montreal.
10. National ACGME Reputation
The University of Rochester was one of the original 8 institutions nationally to receive Innovator status by the ACGME. This status enables us to promote creative and innovative approaches to your training and education.
Follow us on 

