Bursitis
What is bursitis?
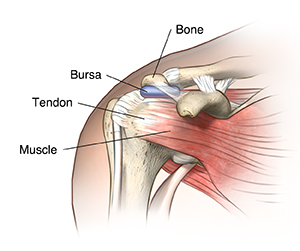
Bursitis is inflammation of a bursa. A bursa is a closed, fluid-filled sac. It works
as a cushion and gliding surface to reduce friction between tissues of the body. The
major bursae (this is the plural of bursa) are located next to the tendons near the
large joints, such as in the shoulders, elbows, hips, and knees.
Bursitis is often a short-term condition. It may limit motion. But usually does not
cause deformity.
Bursitis can happen in any bursa in the body. But there are some common types of bursitis.
These include:
-
Anterior Achilles tendon bursitis. This type of bursitis is also called Albert disease
or retromalleolar bursitis. It’s caused by things like injury, disease, or shoes with
rigid back support. These put extra strain on the lower part of the Achilles tendon,
which attaches the calf muscle to the heel. The extra strain can lead to inflammation
of the bursa where the tendon attaches to the heel.
-
Posterior Achilles tendon bursitis. This type of bursitis is in the bursa located
between the skin of the heel and the Achilles tendon. It is aggravated by walking
that presses the soft heel tissue into the hard back support of a shoe. Walking in
shoes that repeatedly put pressure on the heel can cause the bone to get bigger at
the back of the heel. Examples of these shoes are high heels or pumps. This enlargement
is called Haglund deformity.
-
Hip bursitis. This type is also called trochanteric bursitis. Hip bursitis is often
caused by injury, overuse, arthritis, or surgery. This type of bursitis is more common
in women and middle-aged and older adults.
-
Elbow bursitis. Elbow bursitis is caused by the inflammation of the bursa located
between the skin and bones of the elbow (olecranon bursa). Elbow bursitis can be caused
by injury or constant pressure on the elbow. For example, it can happen when leaning
on a hard surface.
-
Knee bursitis. Bursitis in the knee is also called goosefoot bursitis or Pes Anserine
bursitis. The Pes Anserine bursa is located between the shin bone and the 3 tendons
of the hamstring muscles, on the inside of the knee. This type of bursitis may be
caused by not stretching before exercise, tight hamstring muscles, being overweight,
arthritis, or out-turning of the knee or lower leg.
-
Kneecap bursitis. This type is also called prepatellar bursitis. It is common in people
who are on their knees a lot, such as carpet layers and plumbers.
What causes bursitis?
The most common causes of bursitis are injury or overuse. Infection may also cause
it.
Bursitis is also linked to other health problems. These include arthritis, gout, tendonitis,
diabetes, and thyroid disease.
What are the symptoms of bursitis?
The following are the most common symptoms of bursitis. But symptoms can occur a bit
differently in each person. Symptoms can include:
Long-term (chronic) bursitis may involve repeated attacks of pain, swelling, and tenderness.
These may lead to the breakdown of muscles and a limited range of motion in the affected
joint.
The symptoms of bursitis may look like other health problems. Always see a healthcare
provider for a diagnosis.
How is bursitis diagnosed?
Your healthcare provider will ask about your health history and do a physical exam.
You may also need tests such as:
-
X-ray. This test uses energy beams to make pictures of internal tissues, bones, and
organs on film.
-
MRI. This test uses large magnets, radio waves, and a computer to make detailed pictures
of organs and structures within the body.
-
Ultrasound. This test uses high-frequency sound waves to look at internal organs
and tissues.
-
Aspiration. For this test, the healthcare provider uses a thin needle to remove fluid
from the swollen bursa. The fluid is checked for infection or gout as causes of bursitis.
-
Blood tests. These tests may be done to confirm or rule out other conditions.
How is bursitis treated?
The treatment of any bursitis depends on whether it involves infection.
Aseptic bursitis. This inflammation results from soft-tissue trauma or strain injury.
The bursa is not infected. Treatment may include:
-
RICE, which stands for rest, ice, compression, and elevation
-
Anti-inflammatory and pain medicines, such as ibuprofen or aspirin
-
Shot (injection) of a steroid into the affected area to help ease pain and swelling
-
Splints or braces to limit movement of the affected joint
Septic bursitis. The bursa becomes infected with bacteria. This causes pain and swelling.
Treatment may include:
What can I do to prevent bursitis?
Try the following measures to prevent bursitis:
-
Warm up before exercising or before sports or other repetitive movements.
-
Start new exercises or sports slowly. Gradually increase the demands you put on your
body.
-
Take breaks often when doing repetitive tasks.
-
Cushion “at risk” joints by using elbow or knee pads.
-
Stop activities that cause pain.
-
Practice good posture. Position your body correctly when doing daily activities.
When should I call my healthcare provider?
Call your healthcare provider if you have any of these:
-
Pain or trouble moving that affects your regular daily activities
-
Pain that doesn’t get better or gets worse with treatment
-
A bulge or lump that develops at the affected joint
-
Redness or swelling that develops at the affected joint
-
Fever, chills, or night sweats
Key points about bursitis
-
Bursitis is inflammation of a bursa. This fluid-filled sac works as a cushion and
gliding surface to reduce friction between tissues of the body.
-
The most common causes of bursitis are injury or overuse. But it can also be caused
by infection.
-
Pain, swelling, and tenderness near a joint are the most common signs of bursitis.
-
Bursitis can be treated with rest and medicines to help with the inflammation. Antibiotics
are used if infection is found. If needed, surgery can be done to remove the bursa.
-
You can help prevent bursitis by doing things like warming up before exercise or sports,
increasing activity slowly, padding joints, taking rest breaks often, and stopping
activities that cause pain.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
-
Know the reason for your visit and what you want to happen.
-
Before your visit, write down questions you want answered.
-
Bring someone with you to help you ask questions and remember what your provider tells
you.
-
At the visit, write down the name of a new diagnosis and any new medicines, treatments,
or tests. Also write down any new instructions your provider gives you.
-
Know why a new medicine or treatment is prescribed and how it will help you. Also
know what the side effects are.
-
Ask if your condition can be treated in other ways.
-
Know why a test or procedure is recommended and what the results could mean.
-
Know what to expect if you do not take the medicine or have the test or procedure.
-
If you have a follow-up appointment, write down the date, time, and purpose for that
visit.
-
Know how you can contact your provider if you have questions.