Labor
What is labor?
Labor is when the uterus contracts again and again to help the cervix open (dilate)
and to thin (efface). The contractions get stronger with time. This causes the fetus
to move through the birth canal. Labor usually starts 2 weeks before or after the
estimated date of delivery. But no one knows exactly what triggers the start of labor.
What are the signs of labor?
Signs of labor vary from person to person to woman because each person has a slightly
different labor. Some common signs of labor are:
-
Bloody show. A small amount of mucus slightly mixed with blood may come out of the vagina.
-
Contractions. Contractions (uterine muscle spasms) occurring at intervals of less than 10 minutes
are often a sign that labor has started. Contractions may happen more often and get
stronger as labor progresses.
-
Rupture of amniotic sac (bag of waters). Labor sometimes starts with amniotic fluid gushing or leaking from the vagina. People
who have a rupture of the amniotic sac should go to the hospital right away and contact
their healthcare provider. Most people go into labor within hours after the amniotic
sac breaks. If your labor still has not started, you may need to stay in the hospital
to have labor induced. This step is often taken to prevent infections and delivery
problems.
If you are not sure if labor is starting, call your healthcare provider.
What are the different stages of labor?
Each labor is different. But it's typically divided into 3 stages:
First stage
This is the start of labor to complete dilation. It's divided into the latent phase and the active phase. People can have very strong, painful contractions during the latent phase. The cervix
opens (dilates) about 3 or 4 centimeters and thins out (effaces). Some people may
not know they are in labor if their contractions are mild and irregular.
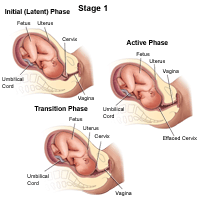
-
The latent phase is when contractions become more frequent (usually 5 to 20 minutes apart) and somewhat
stronger. This is usually the longest and least intense phase of labor. You may be
admitted to the hospital during this phase. The healthcare provider or midwife will
do pelvic exams to check the dilatation of the cervix.
-
The active phase is signaled by the more rapid dilatation of the cervix. It may start as early as
3 to 5 centimeters or as late as 6 centimeters. This continues until 10 centimeters.
Contractions become regular, longer, more severe, and more often (usually 3 to 4 minutes
apart). You often will feel the urge to push during this phase. In most cases, the
active phase is shorter than the latent phase.
Second stage
The second stage of labor starts when the cervix is completely opened. It ends with
the birth of the baby. The second stage is often called the "pushing" stage. During
the second stage, you become actively involved by pushing the baby through the birth
canal to the outside world. When the baby's head is visible at the opening of the
vagina, it's called "crowning." The second stage is shorter than the first stage.
It may take 30 minutes to 3 hours or longer for a woman's first pregnancy.
Third stage
After your baby is born, you enter the third and final stage of labor. This is delivery
of the placenta. This is the organ that has nourished your baby inside the uterus.
This stage often lasts just a few minutes up to a half-hour. In this stage, the placenta
passes out of the uterus and through the vagina.
Each labor experience is different. The amount of time in each stage will also vary.
But most people will deliver their baby within 10 hours after being admitted into
the hospital, if the labor is not induced. Labor is generally shorter for future pregnancies.
Induction of labor
In some cases, labor has to be "induced." This is a process of stimulating labor to
start. The reasons for induction vary. It's not done before 39 weeks of pregnancy
unless there is a problem. Some common reasons for induction are:
-
You or the fetus is at risk
-
The pregnancy has lasted too far past the due date
-
You have preeclampsia, eclampsia, or chronic high blood pressure
-
The fetus has poor growth
Some common ways to induce labor are:
-
Putting medicine in the vagina (suppository) that has prostaglandin. This will stimulate
contractions.
-
Giving an IV infusion of oxytocin or another medicine. Oxytocin is a hormone made
by the pituitary gland that stimulates contractions.
-
Rupturing (artificially) the amniotic sac
-
Putting a balloon in the cervix
Care at the hospital during labor
When you arrive at the hospital in labor, the nursing staff may do a physical exam
of the abdomen to determine the size and position of the fetus, and an exam of the
cervix. The nursing staff may also check:
IV fluids are sometimes given during labor. The IV line is a thin plastic tube put
into a vein, often in your forearm. It can also be used to give medicine. IV fluids
are usually given once active labor has started. You also need them if you have epidural
anesthesia.
The fetus is also carefully monitored during labor. A monitor may be placed over your
abdomen to keep track of the fetal heart rate.
How is pain managed during labor?
You have many choices for pain relief during labor and birth. Your healthcare provider
will want to use the safest method that works best for both you and your baby.
The choice will be determined by your preference and health, the health of the fetus,
and your provider's recommendation.
The 3 main types of pain management for labor and birth are discussed below.
Nonmedicine measures
These measures give comfort and ease stress. These are sometimes called natural childbirth.
Many people learn methods to help them feel more comfortable and in control during
labor and birth. Some of these methods are:
-
Relaxation. These methods can help you tell if you have tension and be better able to release
it. They include progressive relaxation. It's when you relax various muscle groups
in series.
-
Touch. This may include massage or light stroking to ease tension. A jetted bath or a shower
during labor may also help ease pain or tension. Ask your healthcare provider before
taking a tub bath in labor.
-
Heat or cold therapy. This is used to help relax tensed or painful areas. It might be a warmed towel or
a cold pack
-
Imagery. This method uses the mind to form mental pictures that help create relaxed feelings.
-
Meditation or focused thinking. Meditation focuses on an object or task, such as breathing. It helps direct the mind
away from the discomforts.
-
Breathing. These methods use different patterns and types of breathing to help direct the mind
away from the discomforts.
-
Positioning and movement. Many people find changing positions and moving around during labor helps ease discomfort.
It may even speed labor along. Rocking in a rocking chair, sitting in the "Tailor
sit" position, sitting on a special "birthing ball," walking, and swaying may be helpful.
Your healthcare provider can help you find comfortable positions that are also safe
for you and your baby.
Analgesics
These are medicines, such as meperidine, to ease pain. Small amounts are generally
safe during labor and are commonly used with very few problems. But if given in large
amounts or in repeated doses, analgesics can cause slowing of the breathing center
in the brain in mothers and babies.
Anesthesia
These are medicines that cause loss of sensation. They are:
Local block
This anesthesia is injected in the perineal area. This is the area between the vagina
and rectum. It numbs the area to fix a tear or episiotomy after giving birth.
Pudendal block
This local anesthesia is injected into the vaginal area (affecting the pudendal nerve).
It causes complete numbness in the area without affecting the contractions of the
uterus. You can remain active in pushing the baby through the birth canal. It's used
for vaginal deliveries.
Epidural anesthesia or epidural block
This anesthesia involves infusing numbing medicines through a thin catheter that has
been put into the space that surrounds the spinal cord in the lower back. It causes
loss of feeling in the lower body. Infusions of medicines may be increased or stopped
as needed. This type of anesthesia is used during labor and for vaginal and cesarean
(C-section) births. The most common problem of epidural anesthesia is low blood pressure
in the mother. Because of this, most people need to have an IV infusion of fluids
before it's given. A risk of this anesthesia is a postpartum headache. It may develop
if the epidural needle enters the spinal canal, instead of staying in the space around
the canal. The anesthesiologist or nurse anesthetist will discuss the risks and benefits
of this anesthesia.
Epidural analgesia
This is sometimes called a "walking" epidural. That's because the medicine infused
through the epidural is an analgesic. It eases pain but does not numb the body. You
are able to move. Combinations of medicines may be used in the epidural, part analgesic
and part anesthetic. The most common problem of epidural analgesia is low blood pressure
in the pregnant person. This type of anesthesia is used during labor and for vaginal
deliveries. A risk of epidural analgesia is a postpartum headache. It may develop
if the epidural needle enters the spinal canal, instead of staying in the space around
the canal. Epidural analgesia may be used for pain relief in labor and for vaginal
deliveries.
Spinal anesthesia
This anesthesia involves injecting a single dose of anesthetic medicine directly into
the spinal fluid. It acts very quickly and causes complete loss of feeling and movement
of the lower body. This type of anesthesia is often used for C-sections.
Spinal analgesia
This involves injecting an analgesic medicine into the spinal fluid to give pain relief
without numbing. It may be used in combination with epidural anesthesia or analgesia.
It may be used for pain relief during labor or after giving birth.
General anesthesia
This type of pain relief involves giving anesthetic medicine that causes you to go
to sleep. It may be used in emergency C-sections.