Kidney Transplantation
What is a kidney transplant?
A kidney transplant is a surgical procedure. It's done to implant a healthy kidney
from another person. The kidney may come from a deceased donor or from a living donor.
A person getting a transplant often receives only one kidney. But in rare cases, they
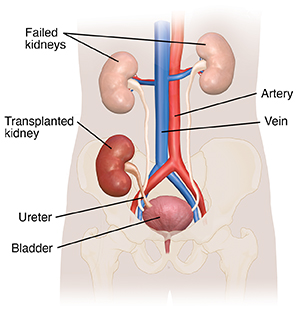
may receive two kidneys. Often, the diseased kidneys are left in place during the
transplant. The transplanted kidney is put in the lower abdomen on the front side
of the body.
Why is a kidney transplant recommended?
A kidney transplant is advised for people who have end-stage kidney disease and will
not be able to live without dialysis or a transplant. In the U.S., the most common
causes of end-stage kidney disease are diabetes and high blood pressure. There are
also many other causes of this disease. Always talk with your healthcare provider
for a diagnosis.
How many people in the U.S. need kidney transplants?
Visit United Network for Organ Sharing (UNOS) to find statistics of patients awaiting a kidney transplant. You can also see the
number of patients who had a transplant this year.
Where do transplanted organs come from?
Most kidneys that are transplanted come from deceased organ donors. Organ donors are
adults who have become critically ill and are pronounced dead because their brain
or heart has stopped working permanently. Kidneys are taken after these adults are
pronounced dead. The family of the dead person needs to agree to donate the person's
organs. Donors can come from any part of the U.S. This type of transplant is called
a deceased donor transplant.
A person having a transplant often gets only one kidney. But in rare cases, they may
receive two. Medical experts are working to see if they can split one kidney for two
recipients.
Family members or individuals who are unrelated, but make a good match, may also be
able to donate one of their kidneys. This type of transplant is called a living transplant
(living donor). People who donate a kidney can live healthy lives with one kidney.
A child older than 2 years can generally get an adult kidney. There is often enough
space in the belly for the new kidney to fit.
How are transplanted organs allocated?
UNOS is responsible for transplant organ distribution in the U.S. UNOS oversees the
allocation of many different types of transplants. These include kidney, liver, pancreas,
heart, lung, cornea, bone, and skin.
UNOS gets data from hospitals and medical centers throughout the country regarding
adults and children who need organ transplants. The medical transplant team that currently
follows you is in charge of sending your data to UNOS and updating it as your condition
changes.
As of December 4, 2014, the newly revised kidney allocation system (KAS) has been
in place. This new system was designed to improve transplant opportunities for all
candidates. It gives better access to patients who often wait longer due to blood
type or other reasons. If you were already on a waiting list before the new KAS was
put into effect, you will not lose your place in line. Talk with your healthcare provider
about the new KAS guidelines.
When a donor organ becomes available, a computer searches all the people on the waiting
list and sets aside those who are not good matches for the kidney. A new list is made
from the remaining candidates. The person at the top of the list is considered for
the transplant. If they are not a good candidate, for whatever reason, the next person
is considered, and so forth. Some reasons that people lower on the list might be considered
before a person at the top include the size of the donor organ and the geographic
distance between the donor and the recipient.
How am I placed on the waiting list for a new kidney?
An extensive evaluation must be done before you can be placed on the transplant list.
Testing includes:
Blood tests are done to gather information that will help determine how urgent it
is that you are placed on the transplant list. They also make sure that you get a
donor organ that is a good match. Some of the tests you may already be familiar with.
You may have had them to evaluate the health of your kidney and other organs. These
tests may include:
-
Blood chemistries. These may include serum creatinine, electrolytes (such as sodium and potassium),
cholesterol, and liver function tests.
-
Clotting studies, such as prothrombin time (PT) and partial thromboplastin time (PTT).
These tests measure the time it takes for blood to clot.
Other blood tests will help improve the chances that the donor organ will not be rejected.
They may include:
-
Your blood type. Each person has a specific blood type: type A+, A-, B+, B-, AB+, AB-, O+, or O-. When
getting a transfusion, the blood received must be a compatible type with your own.
Or an allergic reaction will happen. The same allergic reaction will happen if the
blood contained within a donor organ enters your body during a transplant. Allergic
reactions can be prevented by matching the blood types of you and the donor.
-
Human leukocyte antigens and panel reactive antibody (PRA). These tests help determine the likelihood of success of an organ transplant. They
check for antibodies in your blood. Antibodies are made by the body's immune system
in reaction to a foreign substance, such as a blood transfusion or a virus. Antibodies
in the bloodstream will try to attack transplanted organs. So people who get a transplant
will take medicines that decrease this immune response. The higher your PRA, the more
likely that an organ will be rejected.
-
Viral studies. These tests see if you have viruses that may increase your chance of rejecting the
donor organ, such as cytomegalovirus. Many other infectious diseases are also tested
for, including HIV and hepatitis.
Diagnostic tests are done to understand your complete medical status. Many of these
tests are decided on an individual basis:
-
Renal ultrasound. During this noninvasive test, a transducer is passed over the kidney. It makes sound
waves that bounce off the kidney, sending a picture of the organ to a video screen.
The test is used to determine the size and shape of the kidney. It can also find a
mass, kidney stone, cyst, or other obstruction or abnormalities.
-
Kidney biopsy. For this procedure, tissue samples are removed (with a needle or during surgery)
from the kidney. They are examined under a microscope. This test is done to determine
if cancer or other abnormal cells are present.
-
Intravenous pyelogram. This is a series of X-rays of the kidney, ureters, and bladder. A contrast dye is
injected into a vein to find tumors, abnormalities, kidney stones, or any obstructions.
The transplant team will consider all information from interviews, your medical history,
physical exam, and diagnostic tests in deciding whether you can be a candidate for
a kidney transplant. After you have been accepted to have a kidney transplant, you
will be placed on the UNOS list.
If you are getting a kidney donated by a living donor, the donor will have a similar
evaluation.
The transplant team
During the evaluation process, you will be interviewed by many members of the transplant
team, such as:
-
Transplant surgeons. Healthcare providers who specialize in organ transplants and who will be doing the
surgery.
-
Nephrologist. A healthcare provider who specializes in disorders of the kidneys. Nephrologists
will help manage your condition before and after the surgery.
-
Transplant nurse coordinator. A nurse who organizes all aspects of care provided to you before and after the transplant.
The nurse coordinator will provide education and coordinate the diagnostic testing
and follow-up care.
-
Social workers. Experts who will help your family deal with many issues that may come up, such as
lodging and transportation, finances, and legal issues.
-
Dietitians. Experts who will help you meet your nutritional needs before and after the transplant.
-
Physical therapists. Healthcare providers who will help you become strong and independent with movement
and endurance after the transplant.
-
Pastoral care. Chaplains who provide spiritual care and support.
-
Other team members. Several other team members will evaluate you before the transplant and will make recommendations
to the team. These include:
How long will it take to get a new kidney?
There is no definite answer to this question. If you have a compatible and healthy
living donor, you may be able to get a transplant within a few weeks or months. If
no living-related donor is available, it may take months or years on the waiting list
before a suitable donor organ is available. During this time, you will receive close
follow-up with your healthcare providers and the transplant team. Support groups are
also available to help you during this waiting time.
How am I notified when a kidney is available?
Each transplant team has its own specific guidelines regarding waiting on the transplant
list and being notified when a donor organ is available. In most cases, you will be
notified by phone or pager that an organ is available. You will be told to come to
the hospital right away so that you can be prepared for the transplant.
What is rejection?
Rejection is a normal reaction of the body to foreign tissue. When a new kidney is
placed in a person's body, the body sees the transplanted organ as a threat and tries
to attack it. The immune system makes antibodies to try to kill the new organ. It
does not realize that the transplanted kidney is beneficial. To allow the organ to
successfully live in a new body, medicines must be given to trick the immune system
into accepting the transplant and not thinking it is a foreign object.
What is done to prevent rejection?
Medicines must be given for the rest of your life to fight rejection. Each person
is individual, and each transplant team has preferences for different medicines. The
antirejection medicines most commonly used singly or in combination include:
-
Cyclosporine
-
Tacrolimus
-
Azathioprine
-
Mycophenolate mofetil
-
Prednisone
-
OKT3
-
Antithymocyte Ig
New antirejection medicines are continually being approved. Healthcare providers tailor
medicine regimes to meet the needs of each individual.
Often several antirejection medicines are given initially. The doses of these medicines
may change often as your response to them changes. Because antirejection medicines
affect the immune system, people who receive a transplant will be at higher risk for
infections or even certain types of cancer. A balance must be kept between preventing
rejection and making you very prone to infection. Blood tests to measure the amount
of medicine in the body are done periodically. They make sure you do not get too much
or too little of the medicines. White blood cells are also an important indicator
of how much medicine you need.
The risk of infection is especially great in the first few months. That's because
higher doses of antirejection medicines are given during this time. You will most
likely need to take medicines to prevent other infections from happening.
What are the signs of rejection?
These are some of the most common symptoms of rejection:
Your transplant team will instruct you on who to call right away if any of these symptoms
happen.
Long-term outlook for a person after a kidney transplant
Living with a transplant is a lifelong process. You must take medicines to trick the
immune system so it will not attack the transplanted organ. You must also take other
medicines to prevent side effects of the antirejection medicines, such as infection.
You will have frequent visits to and contact with your transplant team. It's important
that you know the signs of organ rejection and watch for them on every day.
Every person is different and every transplant is different. The new antirejection
medicines that are being approved are promising. Results improve continually as healthcare
providers and scientists learn more about how the body deals with transplanted organs
and search for ways to improve the success of transplants.