Your Baby and Breastfeeding
Breastfeeding well
Here are some signs that your baby is breastfeeding well:
-
Your baby shows readiness (cues) for feedings
-
Your baby is in a good feeding position
-
Your baby latches-on deeply at the breast
-
Your baby transfers milk from the breast and into their mouth
-
Breastfeeding is comfortable for you
Feeding cues
Your baby has to wake up and let you know that they want to eat. This is called showing
feeding cues. A baby should show they are hungry 8 to 12 times in a 24-hour period.
Watch your baby and begin breastfeeding when you see your baby:
Crying is a late feeding cue. Many babies have problems latching on once they become
frustrated and begin to cry. Try to feed your baby before they cry. If your baby does
cry and can't latch on, calm your baby before trying again. Put your baby skin-to-skin
away from the breast or let them suck on your finger. Or have someone else hold the
baby for a while so your baby can calm down. Then offer to nurse again.
Feeding positions
It will be easier for your baby to latch-on if they're snugly and in a good position
for feeding. The most common feeding positions include:
-
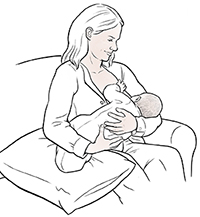
Cradle. The baby is held in the crook or elbow area of your arm on the same side as the breast
to be used for feeding. You support your breast with the opposite hand. Your baby's
body is rolled in toward your body so you are belly-to-belly. You should not be able
to see the baby's arm that's closest to your body. And your baby's chin should not
be down against their chest in this position.
-
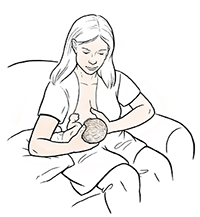
Cross-cradle. The baby's head is supported by your hand that is opposite the breast to be used for
feeding. You support your breast with your hand. The baby is rolled in toward your
body belly-to-belly. As in the cradle hold, you should not be able to see the baby's
arm that's closest to your body.
-
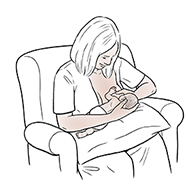
Football or clutch. Baby's head is supported by your hand that's on the same side as the breast to be
used for feeding. Your baby's body is supported on a pillow. The baby is tucked under
your arm on the same side as the breast to be used for feeding. Many women who have
had a cesarean-section delivery prefer this position. It keeps pressure off your belly.
-
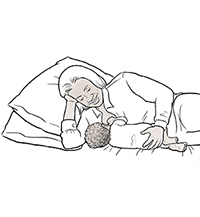
Side-lying using modified cradle. Your baby lies next to you. Your bodies are facing each other. If a pillow under your
arm is uncomfortable, try placing your baby in the crook of your arm. This position
also keeps the baby's head at a good angle to bring baby and breast together. The
baby's head is also higher than their tummy. This can be helpful for babies who are
more likely to spit up.
-
Laid-back breastfeeding. You are leaning back in a recliner or reclining in bed. Your baby is lying on their
stomach on top of you. You can support the side of your baby's head if your baby can't
hold it up. In this position, both you and your baby can relax. You can let your baby
explore your breast and latch on at their own pace.
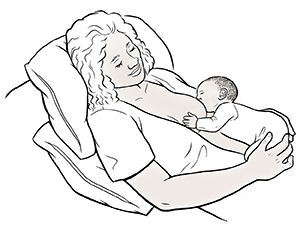
For all positions, bring your baby to the breast. Don't give your breast to the baby.
Start getting in a good position before you try to latch. It can help to sit in a
roomy and comfortable chair or sofa. Some women find it comfortable to use a pillow
on their lap to raise the baby to the breast. Your baby must be held in good alignment
if they are to suck, swallow, and breathe during feedings. When in good alignment,
you should be able to draw a straight line down your baby's body from earlobe to shoulder,
to hip, no matter which feeding position you use. For you, being in a comfortable
position means that your feet are supported, your back is supported, you are sitting
up straight and not leaning over your baby, and your shoulders are relaxed. You may
find it more comfortable to put a pillow under your arm or behind your back.
Deep latch-on
To help your baby get a deep latch, support your breast from below with your hand.
Here are 2 holds to try:
-
C-hold. Place your thumb on top of your breast and your fingers under your breast, at least
1-1/2 to 2 inches behind the nipple. A C-hold gives good support for the cradle or
cross-cradle feeding positions.
-
U-hold. This is a variation of the C-hold. It's often used when a baby is placed in the football
(clutch) position for feeding. For a U-hold, slide your hand so your thumb is on 1
side of the breast and your fingers on the other.
You may not have to keep using a C-hold or U-hold if your breasts are smaller. But
mothers with larger breasts often use these holds for the entire feeding.
Once you are both comfortable and your breast is supported, you are ready to help
your baby latch. To help your baby latch-on correctly, use your nipple to stroke the
baby from the nose to the lower lip in a downward motion. Wait for your baby to open
wide. Then bring the baby and your breast together in one quick motion. The baby should
have a big mouthful of your breast. Their chin should be buried into your breast,
and their nose should be close to or slightly touching your breast. Your baby's lips
should be flanged outward like a trumpet or fish lips. The lips should not be pursed
or rolled in. If you were to roll down your baby's lower lip, you should see the baby's
tongue gliding in front of the lower gum. The tongue should also cup your nipple and
areola.
Don't press down near the areola with your thumb. You may think this will help your
baby breathe. But this will pull your nipple from the back of your baby's mouth, where
it needs to be. Babies' noses are designed to press against their mother's breast
as they feed. That is why their noses are flat. This lets them latch on deeply to
the breast but still be able to breathe. If you are concerned about your baby's ability
to breathe, pull your baby's lower body in closer to you. Or lift your breast rather
than pressing down on your breast.
It's called breastfeeding, not nipple-feeding, for a reason. Sometimes a baby's latch
is shallow. This means it is not deep onto the areola. The baby may seem to be hanging
on the nipple tip. When this happens, your baby won't be able to remove milk from
your breast very well. This would decrease the amount of milk your baby drinks. So
feedings may take more than 45 minutes. And your baby may not gain weight as they
should. Also, your nipples are more likely to get very sore or cracked. Try the different
positions outlined above if you're worried your baby doesn't have a deep latch, or
if you have sore or cracked nipples. If this doesn't work, contact your baby's healthcare
provider or a certified lactation consultant for help.