Mastectomy
What is a mastectomy?
A mastectomy is surgery to remove a breast. Sometimes other tissues near the breast,
such as lymph nodes, are also removed. This surgery is most often used to treat breast
cancer. A mastectomy might also be done to help prevent breast cancer in people who
have a very high risk for it.
Why might I need a mastectomy?
A mastectomy may be done as part of treatment for breast cancer. It might be suggested
if:
-
The tumor is large, or large compared to the size of your breast
-
You have more than 1 tumor and they're not near each other
-
You can't have radiation therapy. This may be the case if you're pregnant, have a
connective tissue disease, such as rheumatoid arthritis, or have had radiation in
the past.
-
You prefer this surgery instead of getting radiation
-
You've had radiation therapy to your breast in the past
-
You have inflammatory breast cancer
-
The cancer has come back after other treatment
-
You have a gene change, such as a BRCA mutation, that puts you at high risk for another
breast cancer
In some cases, people with a high risk for breast cancer may want to have a mastectomy
before cancer develops. This includes people with genes linked to breast cancer, such
as the BRCA1 or BRCA2 gene. In these cases, a mastectomy is done to try to keep breast
cancer from occurring.
There may be other reasons for your healthcare provider to advise a mastectomy.
What are the different types of mastectomies
Any type of mastectomy may include removing lymph nodes. These are small, bean-shaped
organs connected to lymph vessels. They are part of the lymphatic system, which is
part of your immune system. A clear fluid called lymph carries infection-fighting
white blood cells and cell waste all around your body through the lymphatic system.
The lymph nodes filter this waste. Cancer cells often spread into the lymphatic system
and collect in the nodes. Nodes removed during mastectomy are tested to see if there
are cancer cells in them. This information is used to plan your treatment after surgery.
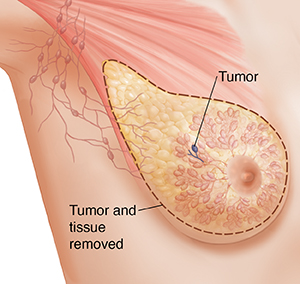
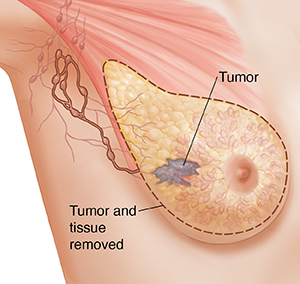
There are many types of mastectomy procedures. Your surgeon will talk with you about
the surgery that is advised for you. Choices tend to depend on where the tumor is
and how big it is. The size of your breast and your preferences will also help decide
what type of mastectomy is best.
-
Total (simple) mastectomy. This surgery removes the whole breast, including the nipple, the colored ring around
the nipple (called the areola), and most of the overlying skin. Sometimes a few lymph
nodes under arms are removed, too.
-
Modified radical mastectomy. The entire breast is removed. This includes the nipple, the areola, the overlying
skin, and the lining over the chest muscles. Some of the lymph nodes under the arm
are also removed. Breast cancer often spreads to these lymph nodes. It can then spread
to other parts of the body.
-
Radical mastectomy. The entire breast is removed, including the nipple, the areola, the overlying skin,
the lymph nodes under the arm, and the chest muscles under the breast. This was once
the standard surgery, but today it's rarely done. It may be needed for large tumors
that are growing into the chest muscles.
-
Skin-sparing mastectomy. The breast tissue, nipple, and areola are removed. But most of the skin over the breast
is saved. This type of surgery is used only when breast reconstruction is done right
after the mastectomy. It may not be a good choice for tumors that are large or near
the skin surface.
-
Nipple-sparing mastectomy. This is a lot like a skin-sparing mastectomy. All of the breast tissue, including
the ducts going all the way up to the nipple and areola, is removed. But the breast
skin and the nipple and areola are kept. During surgery, the tissues under and around
the nipple and areola are carefully cut away and checked for cancer cells. If no breast
cancer is found close to the nipple and areola, these areas can be saved. If cancer
is found, the nipple must be removed. Reconstruction is done right after this mastectomy.
Breast reconstruction surgery after mastectomy
You may worry about how your breast will look after a mastectomy. Most people can
have breast reconstruction surgery. This surgery rebuilds the breast so it's the size
and shape of your other breast. Some people have breast reconstruction done at the
same time as a mastectomy. Others wait and have it done later, as a second surgery.
Not all people want reconstruction. Some prefer a breast form (breast prosthesis),
a special mastectomy bra, or going flat.
The choice is yours. Talk with your healthcare provider about your choices.
What are the risks of a mastectomy?
All surgeries have some risk. Some complications of mastectomy include:
-
Short-term breast swelling
-
Breast pain, soreness, or both
-
Hardness or lumpiness because of scar tissue that can form at the site of the cut
(incision)
-
Wound infection or bleeding
-
Swelling (lymphedema) of the arm, chest, and neck, if lymph nodes were removed
-
Pain in the breast that has been removed (called phantom breast pain). This may be
helped with medicines, exercise, or massage.
-
Numbness or trouble moving the arm if nerves were damaged during surgery
A buildup of clear fluid (seroma) can happen in the breast after a mastectomy. If
this bothers you, it can be drained in the surgeon’s office. If needed, it can be
treated with compression. Or you may get an injection that helps to harden the space
in the breast to help keep fluid from collecting there.
You'll likely have a scar at the mastectomy site. Scar tissue may also cause a pulling
feeling near or under your arm after surgery.
You may have depression and feelings of loss of sexual identity after a mastectomy.
Your healthcare team will talk with you about the type of mastectomy you're getting
and the risks that come with it. Be sure to discuss any concerns with your healthcare
provider before surgery.
How do I get ready for a mastectomy?
-
Your healthcare provider will explain the surgery to you and give you a chance to
ask any questions that you might have.
-
You'll be asked to sign a consent form that gives permission to do the surgery. Read
the form carefully and ask questions if anything isn't clear.
-
Your healthcare provider will take your health history. A physical exam will be done.
This is to be sure you are in good health before the surgery. You may also need blood
tests, an EKG, or imaging scans.
-
You'll be asked to not eat or drink anything for some time before the surgery. Your
surgeon will give you instructions.
-
Tell your healthcare provider if you are pregnant or think you may be pregnant.
-
Tell your provider if you are sensitive to or allergic to any medicines, latex, tape,
and anesthesia medicines (local and general).
-
Tell your provider about all the medicines you take. This includes both over-the-counter
and prescription medicines. It also includes vitamins, herbs, other supplements, and
marijuana. Let your healthcare provider know if you use illegal drugs. Many of these
can cause problems during and after surgery.
-
Tell your provider if you have a history of bleeding problems. Let your provider know
if you are taking any blood thinners, aspirin, ibuprofen, or other drugs that affect
blood clotting. You may need to stop taking these before surgery.
-
Tell your provider if you smoke. You may need to stop before surgery, and your healthcare
provider can help with that. Smoking can slow your recovery and increase your chance
of problems after surgery.
-
You may be given medicine to help you relax (a sedative) before surgery.
-
Your healthcare provider may have other instructions for you based on your medical
condition. Be sure you know what you can and can't do as you get ready for surgery.
What happens during a mastectomy?
You will likely need to stay in the hospital for at least 1 night after mastectomy.
It depends on your overall health, how you feel after surgery, the type of mastectomy,
and your healthcare provider's practices.
For the most part, a mastectomy follows this process:
-
You'll be asked to remove your clothing and given a gown to wear.
-
An IV (intravenous) line will be started in your arm or hand. You'll be given medicine
through the IV. This will help you relax and put you into a deep sleep during the
surgery so you don't feel pain.
-
You will lie on your back on the operating table.
-
Your heart rate, blood pressure, breathing, and blood oxygen level will be watched
closely during the surgery.
-
The skin over your chest will be cleaned.
-
A cut (incision) will be made in your breast. The type of cut and where it is depends
on the type of mastectomy you have.
-
The surgeon will gently cut free and remove underlying tissue.
-
Lymph nodes might be removed after the breast or breast tissue has been removed.
-
If you 're having breast reconstruction along with the mastectomy, a plastic surgeon
will do the reconstruction after the mastectomy.
-
Breast tissue and any other tissues that are removed will be sent to the lab for testing.
-
One or more drainage tubes may be put in the breast to keep fluid from building up
as the area heals.
-
The skin will be closed with stitches, glue, or adhesive strips.
-
A sterile bandage or dressing will be placed over the site. A stretchy band will be
wrapped around your chest. This will stay on for a few days.
What happens after a mastectomy?
In the hospital
After surgery, you'll be taken to the recovery room and watched closely. Your recovery
process will depend on the type of mastectomy and the type of anesthesia used. Once
your blood pressure, pulse, and breathing are stable and you are awake, you'll be
taken to a hospital room.
You'll likely stay in the hospital for a day or so after your mastectomy. This will
depend on the extent of your surgery and if you had breast reconstruction done.
At home
Once you're home, keep the surgical area clean and dry. Your healthcare provider will
give you bathing instructions.
You'll also be taught how to take care of the drainage tubes. They're often taken
out after about 2 weeks or at the first follow-up exam.
The amount of pain you have will vary. It depends on the amount and location of tissue
removed during surgery. Most soreness lasts a few days. Take pain medicine as advised
by your healthcare provider. Aspirin and some other pain medicines may increase your
chance of bleeding. Be sure to take only advised medicines.
If lymph nodes were removed with your mastectomy, your healthcare provider may have
you see a physical therapist and will want you to do certain exercises. These can
help limber up your shoulder and arm and help prevent swelling. Soreness after surgery
may cause you to keep your arm and shoulder very still. This can make your arm and
shoulder stiff. But overdoing the exercises can also hurt you. Start the exercises
slowly. Do them regularly and progress a little each day. You may be asked to do these
exercises even if you didn’t have lymph nodes removed.
You can often go back to your normal activities in a few weeks, based on your healthcare
provider’s advice. In the meantime, don't do any strenuous activities, such as mowing
the lawn, using a vacuum cleaner, working out, or playing sports. Listen to your body.
If an activity causes pain, stop.
Your healthcare provider will tell you when you can start driving again and when you
can go back to work. You'll also be told when it's OK to start wearing a bra or prosthesis.
When to call your healthcare provider
Your healthcare provider will talk with you about when call. You may be told to call
if you have:
-
Fever of 100.4°F (38°C) or higher, or as advised by your healthcare provider
-
Chills
-
Cough or shortness of breath
-
Rapid, irregular heartbeat; new chest pain
-
Signs of infection around the incision, such as redness, drainage, warmth, and pain
-
Drainage from the incision site
-
Incision opens up or the edges pull apart
-
Increased pain around the incision site
-
Any abnormal bleeding or bleeding that soaks the bandage
-
Trouble passing urine or changes in how your urine looks or smells
-
Swelling, numbness, or tingling in your hand, arm, or chest that gets worse or is
not getting better a week or two after surgery
-
Pain, redness, swelling, or warmth in an arm or leg
Your healthcare provider may give you other instructions, too. Ask about signs you
should watch for and when you need to call. Know how to get help after office hours
and on weekends and holidays.
After lymph node removal
Removing lymph nodes can affect how lymph fluid drains from your arm, neck, and chest
on the affected side. Problems with lymph drainage can cause swelling in your arm.
This swelling is called lymphedema. You may also be at greater risk for infection
from injury to your arm. But it's important to use your arm like you normally would.
People who have many lymph nodes removed have a higher risk for lymphedema. Healthcare
providers try to limit the number of lymph nodes that need to be removed.
You'll have to follow certain safety steps for the rest of your life after lymph node
removal. Once lymphedema starts, it cannot be cured. But there are things you can
do to help keep it from starting and to prevent problems in your affected arm. Some
of these steps include:
-
Get to or stay at a healthy weight. Ask your healthcare team for help if needed.
-
Ask your healthcare provider if you should stay away from having your blood pressure
taken or needles used (for blood draws, shots, or IVs) on your affected arm.
-
Follow instructions about arm exercises carefully.
-
Prevent blocking the flow of fluids through your affected arm:
-
Don't wear any tight items on the affected arm. This includes elastic cuffs, tight
watches, or other jewelry.
-
Use your unaffected arm to carry bags or purses.
-
Wear loose-fitting bras with straps that don't dig into your shoulders.
-
Prevent injury, burns, and infections:
-
Don't expose your arm to extreme temperatures, such as ice packs or heating pads.
Don't use saunas or hot tubs.
-
Use lotion to keep your skin soft.
-
Clean any injuries right away and watch for signs of infection.
-
Wear gloves when gardening or doing any activity where there's a risk for getting
cuts in your fingers or hands. Also wear gloves when using strong or harsh chemicals,
such as detergents or household cleaners.
-
Protect your skin in the sun. Cover up, stay in the shade, and use sunscreen. Don't
get a sunburn.
-
If your arm aches or swells, raise (elevate) it, with your hand above your elbow,
to help drain lymphatic fluid.
Talk with your healthcare provider about seeing a lymphedema specialist to learn more
about what you can do to help protect yourself.
Next steps
Before you agree to a test or procedure, make sure you know:
-
The name of the test or procedure
-
The reason you're having the test or procedure
-
What results to expect and what they mean
-
The risks and benefits of the test or procedure
-
What the possible side effects or complications are
-
When and where you are to have the test or procedure
-
Who will do the test or procedure and what that person’s qualifications are
-
What would happen if you did not have the test or procedure
-
Any alternative tests or procedures to think about
-
When and how you will get the results
-
Who to call after the test or procedure if you have questions or problems, even at
night and on weekends
-
How much you will have to pay for the test or procedure