Peripheral Neuropathy
What is peripheral neuropathy?
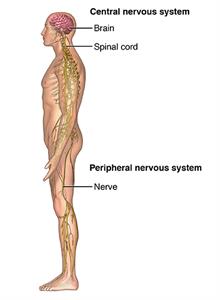
Peripheral neuropathy is a type of damage to the nervous system. Specifically, it's
a problem with your peripheral nervous system. This is the network of nerves that
sends information from your brain and spinal cord (central nervous system) to the
rest of your body. Peripheral nerves are the nerves that exit the spinal canal or
skull and go to your face, trunk, or arms and legs.
There are more than 100 types of peripheral neuropathy. Each has its own set of symptoms
and prognosis. To help healthcare providers classify them, they are often broken down
into these categories:
-
Motor neuropathy. This is damage to the nerves that control muscles and movement in the body, such
as moving your hands and arms or talking.
-
Sensory neuropathy. Sensory nerves control what you feel, such as pain, temperature, or a light touch.
Sensory neuropathy affects these groups of nerves.
-
Autonomic nerve neuropathy. Autonomic nerves control functions that you are not conscious of, such as breathing
and heartbeat. Damage to these nerves can be serious.
-
Combination neuropathies. You may have a mix of 2 or 3 of these other types of neuropathies, such as a sensory-motor
neuropathy.
What causes peripheral neuropathy?
Peripheral neuropathy has many different causes. Some people inherit the disorder
from their parents. Others develop it because of an injury or another disorder.
In many cases, a different type of problem, such as a kidney condition or a hormone
imbalance, leads to peripheral neuropathy. One of the most common causes of peripheral
neuropathy in the U.S. is diabetes. Nerves can also be damaged from:
-
Medicines, such as chemotherapy
-
Toxins, including alcohol and some illegal drugs
-
Infections like Lyme disease or HIV
Who is at risk for peripheral neuropathy?
These are risk factors for peripheral neuropathy:
What are the symptoms of peripheral neuropathy?
The symptoms of peripheral neuropathy vary based on the type that you have and what
part of the body is affected. Symptoms can range from tingling or numbness in a certain
body part to more serious effects, such as burning pain or paralysis. They may include:
-
Muscle weakness
-
Cramps
-
Muscle twitching
-
Loss of muscle and bone
-
Changes in skin, hair, or nails
-
Numbness
-
Loss of sensation or feeling in body parts
-
Loss of balance or other functions as a side effect of the loss of feeling in the
legs, arms, or other body parts
-
Emotional disturbances
-
Sleep disruptions
-
Loss of pain or sensation that can put you at risk, such as not feeling an impending
heart attack or limb pain
-
Inability to sweat correctly, leading to heat intolerance
-
Loss of bladder control, leading to infection or incontinence
-
Dizziness, lightheadedness, or fainting because of a loss of control over blood pressure
-
Diarrhea, constipation, or incontinence related to nerve damage in the intestines
or digestive tract
-
Trouble eating or swallowing
-
Life-threatening symptoms, such as trouble breathing or irregular heartbeat
The symptoms of peripheral neuropathy may look like other health problems. Always
see your healthcare provider for a diagnosis.
How is peripheral neuropathy diagnosed?
The symptoms and body parts affected by peripheral neuropathy are so varied that it
may be hard to make a diagnosis. If your healthcare provider suspects nerve damage,
they will ask about your medical history and do a number of neurological tests. These
can help determine the location and extent of your nerve damage. These may include:
Depending on what basic tests reveal, your healthcare provider may want to do more
in-depth scanning. You may need other tests to get a better look at your nerve damage,
such as:
How is peripheral neuropathy treated?
Often peripheral neuropathy can’t be cured. But you can do a lot of things to prevent
it from getting worse. If an underlying condition like diabetes is at fault, your
healthcare provider will treat that first. They will then treat the pain and other
symptoms of neuropathy.
In some cases, over-the-counter pain relievers can help. Other times, prescription
medicines are needed. Some of these medicines are:
-
Mexiletine, a medicine developed to correct irregular heart rhythms
-
Antiseizure medicines, such as gabapentin, phenytoin, and carbamazepine
-
Some classes of antidepressants including tricyclics, such as amitriptyline
Lidocaine injections and patches may help with pain in other cases. And in extreme
cases, surgery can be used to destroy nerves or fix injuries that are causing neuropathic
pain and symptoms.
Physical therapy can treat weakness and muscle loss. It can also treat problems with
balance. Some people may need splints or braces to help them walk.
What can I do to prevent peripheral neuropathy?
Lifestyle choices can play a role in preventing peripheral neuropathy. You can reduce
your risk for many of these conditions by:
If you have kidney disease, diabetes, or other chronic health conditions, work with
your healthcare provider to control your condition. It may prevent or delay the onset
of peripheral neuropathy.
Living with peripheral neuropathy
Even if you already have some form of peripheral neuropathy, healthy lifestyle steps
can help you feel your best. They can also reduce the pain and symptoms related to
the disorder. You’ll also want to quit smoking. And don't let injuries go untreated.
Be meticulous about caring for your feet and treating wounds to prevent complications,
such as the loss of a limb. Check your feet for red areas every day. Use a mirror
to check between your toes and the bottoms of your feet. Contact your provider if
you have an open sore.
In some cases, hand and foot braces can help you make up for muscle weakness. Orthotics
can help you walk better. Relaxation methods, such as yoga, may help ease emotional
as well as physical symptoms.
Key points about peripheral neuropathy
-
Neuropathy affects the body in many different ways. It can affect how well you’re
able to use your muscles. It can affect feeling and sensation, as well as other body
functions that are automatic, such as your heartbeat.
-
Medicines and lifestyle changes can improve your symptoms.
-
It's important that you control any other diseases you may have to reduce your risk
for peripheral neuropathy.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
-
Know the reason for your visit and what you want to happen.
-
Before your visit, write down questions you want answered.
-
Bring someone with you to help you ask questions and remember what your provider tells
you.
-
At the visit, write down the name of a new diagnosis, and any new medicines, treatments,
or tests. Also write down any new instructions your provider gives you.
-
Know why a new medicine or treatment is prescribed, and how it will help you. Also
know what the side effects are.
-
Ask if your condition can be treated in other ways.
-
Know why a test or procedure is recommended and what the results could mean.
-
Know what to expect if you do not take the medicine or have the test or procedure.
-
If you have a follow-up appointment, write down the date, time, and purpose for that
visit.
-
Know how you can contact your healthcare provider if you have questions.