URMC / Labs / O'Banion-Olschowka Labs / Projects / Neuroinflammation-Following-Therapeutic-Radiation
Neuroinflammation Following Therapeutic Radiation
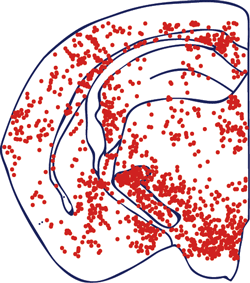
Activated MHC-II positive cells
6 months after therapeutic brain irradiation.
Radiation therapy is an important modality for treatment of primary and metastatic tumors in the CNS. Although radiotherapists take great care in selection of radiation doses and localization of delivered radiation, radiation exposure can lead to significant normal tissue damage, with the worst outcomes known as radiation necrosis. In addition, lower doses of radiation used for whole body ablation of bone marrow in preparation for therapeutic bone marrow transplantation or whole brain irradiation for treatment of CNS lymphomas have been associated with significant cognitive decline, particularly in children. Our overall hypothesis is that neuroinflammation contributes to these undesirable effects of radiation therapy.
To explore this hypothesis we are characterizing the molecular and cellular signatures of radiation exposure in mice up to 12 months after treatment. We find evidence of proinflammatory cytokine and chemokine expression as well as recruitment of cells from the peripheral circulation. Experiments with mice lacking specific chemokine or cytokine receptors are being carried out to establish key mediators of these neuroinflammatory endpoints in efforts to identify potential targets for preventing negative outcomes following radiation therapy. This work is being funded by a grant from the National Cancer Institute.
« back to all projects