News
20242023202220212020
Subscribe to Neuroscience LISTSERV
Mini Strokes Can Cause Brain Damage, Lead To Dementia And Cognitive Impairment: Study
Thursday, December 13, 2012
Chances are if you're a senior managing your health, you've already had a conversation with your doctor about stroke risk. While many patients know the warning signs of stroke -- slurred speech, weakness on one side of the body, coordination problems, double vision, and headaches -- health care providers often fail to educate patients about their risk for silent or mini-strokes,
which can cause progressive, permanent damage and lead to dementia.
A new study published in the Journal of Neuroscience, examined the effects of these so-called mini-strokes. They frequently are not diagnosed or detected by a doctor because a patient does not immediately present with stroke signs. Mini-strokes may lead to permanent neurological damage and increase risk for full blown stroke.
Maiken Nedergaard, MD, lead author of the study and professor of neurosurgery at the University of Rochester Medical Center, says at least half of individuals over the age of 60 will experience one mini-stroke in their lifetime. She calls the prevalence of mini-strokes "an epidemic."
Study Details Brain Damage Triggered by Mini-Strokes
Wednesday, December 12, 2012
A new study appearing today in the Journal of Neuroscience details for the first time how "mini-strokes" cause prolonged periods of brain damage and result in cognitive impairment. These strokes, which are often imperceptible, are common in older adults and are believed to contribute to dementia.
"Our research indicates that neurons are being lost as a result of delayed processes following a mini-strokes that may differ fundamentally from those of acute ischemic events," said Maiken Nedergaard, M.D., D.M.Sc., the lead author of the study and professor of Neurosurgery at the University of Rochester Medical Center. "This observation suggests that the therapeutic window to protect cells after these tiny strokes may extend to days and weeks after the initial injury."
Registration Open for Annual Neurosciences Retreat
Thursday, November 1, 2012
The annual Neurosciences Retreat will be held from 9 a.m. to 6 p.m. Friday, Nov. 16, at the Memorial Art Gallery. The retreat will feature talks from University faculty and graduate students. Lorna Role, chair of the department of neurobiology and behavior at SUNY Stony Brook, will present the keynote address. The retreat is sponsored by the Neuroscience Graduate Program, the University Committee for Interdisciplinary Studies, the Department of Neurobiology and Anatomy, and the John Bartlett Memorial Fund. Registration is free and open to the University community.
Scientists Create Endless Supply
of Myelin-Forming Cells
Thursday, November 1, 2012
In a new study appearing this month in the Journal of Neuroscience, researchers have unlocked the complex cellular mechanics that instruct specific brain cells to continue to divide. This discovery overcomes a significant technical hurdle to potential human stem cell therapies; ensuring that an abundant supply of cells is available to study and ultimately treat people with diseases.
One of the major factors that will determine the viability of stem cell therapies is access to a safe and reliable supply of cells,
said University of Rochester Medical Center (URMC) neurologist Steve Goldman, M.D., Ph.D., lead author of the study. This study demonstrates that -- in the case of certain populations of brain cells -- we now understand the cell biology and the mechanisms necessary to control cell division and generate an almost endless supply of cells.
Endless Supply
of Myelin-Forming CellsMichele Saul wins a travel award to International Society for Developmental Psychobiology Annual Meeting
Thursday, September 20, 2012
Michele, an NBA graduate student in the Fudge Lab, has just received a stipend to travel to New Orleans and present her work entitled, Differential numbers of bromodeoxyuracil (BrdU) positive cells in the amygdala of normal adolescent and young adult rats. This work shows that cell proliferation is one mechanism of plasticity in the rat amygdala, and that it occurs at a higher rate in young animals.
NGP Student, Heather Natola Receives 2012 Merritt and Marjorie Cleveland Fellowship Award
Wednesday, September 12, 2012
NGP first year student, Heather Natola is 2012 recipient of the UR Merritt and Marjorie Cleveland Fellowship Award. She was selected based on her outstanding credentials and the faculty opinion that she has unusual potential for future meritorious contributions in neuroscience field.
NGP Student, Julianne Feola Awarded Pre-doctoral Fellowship from the National Institutes of Health
Tuesday, September 11, 2012
Julianne Feola, 3rd year NGP student in Dr. Gail Johnson-Voll lab was awarded a pre-doctoral fellowship from the National Institutes of Health, National Institute of Neurological Disordered and Stroke for her project entitled: The Role of Astrocytic Transglutaminase 2 in Mediating Ischemic Stroke Damage.
2012 NGP Students Receive Funding From NINDS
Tuesday, August 21, 2012
Recently the National Institute of Neurological Disorders and Stroke (NINDS) awarded several of our Neuroscience Graduate Program students training grants. This year, first year NGP students, Lauren Cummings, Heather Natola, and Matthew Cavanaugh, as well as second year students, Ryan Dawes and Laura Yunes-Medina received funding. Jennifer Stripay who was appointed last year, will continue on the grant. NINDS is funded by the National Institutes of Health (NIH), with it's continuing mission to reduce the burden of neurological disease - a burden borne by every age group, by every segment of society, by people all over the world.
NGP Student Adam Pallus Awarded a Competitive Graduate Fellowship From CVS
Tuesday, August 21, 2012
Adam Pallus, a Neuroscience graduate student in Dr. Ed Freedman's lab, was awarded a competitive graduate fellowship from the University of Rochester Center for Visual Science from 7/1/12 to 12/31/13. CVS offers competitive graduate fellowships for graduate students working in the lab of a CVS faculty member. Applications are made by a student's advisor to the vision training committee in CVS. Fellows receive full stipend support as well as funds to cover one academic conference per year.
NGP Student Revathi Balasubramanian Appointed to the Predoctoral NYSTEM Training Grant
Tuesday, August 21, 2012
Revathi Balasubramanian, a Neuroscience Graduate Program student in Dr. Lin Gan's lab, was appointed to the predoctoral NYSTEM Training Grant from 7/1/12 to 6/30/2013. NYSTEM training grant funds are utilized to provide up to two years of support to four graduate students and two postdoctoral fellows. The second year of support will be contingent on satisfactory progress in the first year. Graduate students will be supported at $23,000 per year, the maximum permitted in this application. Additional support in order to provide the standard University of Rochester graduate student stipends must be provided by the host laboratory, which will have to confirm the availability of funding to support the student through the completion of his/her degree.
Scientists Discover Previously Unknown Cleansing System in Brain
Wednesday, August 15, 2012
A previously unrecognized system that drains waste from the brain at a rapid clip has been discovered by neuroscientists at the University of Rochester Medical Center. The findings were published online August 15 in Science Translational Medicine.
The highly organized system acts like a series of pipes that piggyback on the brain's blood vessels, sort of a shadow plumbing system that seems to serve much the same function in the brain as the lymph system does in the rest of the body -- to drain away waste products.
"Waste clearance is of central importance to every organ, and there have been long-standing questions about how the brain gets rid of its waste," said Maiken Nedergaard, M.D., D.M.Sc., senior author of the paper and co-director of the University's Center for Translational Neuromedicine. "This work shows that the brain is cleansing itself in a more organized way and on a much larger scale than has been realized previously.
"We're hopeful that these findings have implications for many conditions that involve the brain, such as traumatic brain injury, Alzheimer's disease, stroke, and Parkinson's disease," she added.
Danielle deCampo is Awarded NRSA Individual Fellowship
Sunday, July 15, 2012
Congratulations to Danielle, who is in the Medical Scientist Training Program (MSTP), for receiving NIMH Fellowship support for her project, An Extended Amygdala Path with Implications for Early Life Stress. Using a variety of techniques, Danielle is examining a pathway through the amygdala that appears plays a role in development of stress responses and is affected by early life stress. Her project is an outgrowth of collaborations with Dr. Judy Cameron (University of Pittsburgh) and Dr. Karoly Mirnics (Vanderbilt University), and previous support of the URMCCTSI Pilot Program.
Danielle deCampo wins Travel Award to ACNP
Tuesday, July 10, 2012
Danielle has won a highly competitive travel award to the 2012 Annual Meeting of the American College of Neuropsychopharmacology (ACNP). This meeting brings together basic and clinical scientists in the field of psychiatric research, and is a wonderful opportunity to see the latest work in the field. Congrats!
Funding Awarded to Senior Design Project
Friday, June 15, 2012
The UR Technology Development fund has decided to invest approximately $50,000 toward the development of a product designed by a Senior Design Team in Biomedical Engineering. Benjamin Horowitz, Megan Makarski, William Sipprell, and Robert Handzel (Biomedical Engineering, '09), working with Strong Neonatologists Timothy Stevens, M.D., and Patricia Chess, M.D., designed and prototyped a respiration monitor for use on very low birth weight newborns. With this funding, which was awarded to Scott Seidman, Ph.D., Associate Professor of Biomedical Engineering and Neurobiology & Anatomy, a second-generation prototype ready for introduction into the Neonatal Intensive Care Unit will be constructed and tested, with the clear aim of getting this life-saving technology onto the market.
Dr. Tatiana Pasternak Elected Secretary of the Society for Neuroscience
Thursday, June 14, 2012
The department of Neurobiology & Anatomy is thrilled to announce the exciting new election results in which our own Tatiana Pasternak has been elected Secretary of the Society for Neuroscience. She joins a group of 5 top officers of the Society, which is among the largest and most extensive organizational entities dedicated to neuroscience in the world, with over 41,000 members. Please join us in offering a hearty congratulations to Tania in her new role.
Dr. Pasternak is also a Professor in the department of Brain & Cognitive Sciences at the Center for Visual Science at the University of Rochester. She has been a member of SfN for over 25 years. She has served as a member of the Committee on Committees as well the Program Committee and was Chair for both the Gruber International Research Award and Donald B. Lindsley Prize Selection Committees. Dr. Pasternak's research is focused on cortical circuitry underlying memory-guided sensory decision making.
A Pillar of Modern Neurology, Robert J. Joynt, Dies
Monday, April 16, 2012
Robert J. Joynt, M.D., Ph.D.
Robert J. Joynt, M.D., Ph.D., one of the most influential neurologists of the last half century and the founder of the Department of Neurology at the University of Rochester Medical Center, died April 13 at Strong Memorial Hospital. He was 86.
Dr. Joynt was a towering figure in international circles of neurology and headed both leading societies in neurology, the American Academy of Neurology and the American Neurological Association. He also served as president of the American Board of Psychiatry and Neurology. Beyond that, he was a beloved member of the Medical Center's community, which he had served through several top-level posts, including dean of the School of Medicine and Dentistry.
Once Considered Mainly ‘Brain Glue,’ Astrocytes’ Power Revealed
Thursday, March 29, 2012
A type of cell plentiful in the brain, long considered mainly the stuff that holds the brain together and oft-overlooked by scientists more interested in flashier cells known as neurons, wields more power in the brain than has been realized, according to new research published today in Science Signaling.
Neuroscientists at the University of Rochester Medical Center report that astrocytes are crucial for creating the proper environment for our brains to work. The team found that the cells play a key role in reducing or stopping the electrical signals that are considered brain activity, playing an active role in determining when cells called neurons fire and when they don't.
That is a big step forward from what scientists have long considered the role of astrocytes -- to nurture neurons and keep them healthy.
"Astrocytes have long been called housekeeping cells -- tending to neurons, nurturing them, and cleaning up after them," said Maiken Nedergaard, M.D., D.M.Sc., professor of Neurosurgery and leader of the study. "It turns out that they can influence the actions of neurons in ways that have not been realized."
Lynne Maquat Named 2012 Batsheva de Rothschild Fellow
Friday, March 23, 2012
Professor of Biochemistry & Biophysics and Director for the Center for RNA Biology, Lynne Maquat, Ph.D., has been
named a 2012 Batsheva de Rothschild Fellow of the Israel Academy of Sciences and Humanities. Batsheva de Rothschild (1914-1999) was a
biologist, trained at the Sorbonne, Paris and at Columbia University, New York. She worked for a while at the Pasteur
Institute in Paris.
The Batsheva Fund was established as a private endowment fund, first in New York City and afterwards, in 1965, in
Israel. In 1993 she generously transferred the fund to the Israel Academy of Sciences and Humanities. In 1958 she
became the only one ever, from her legendary family, to settle in Israel and became active in public life. Science
and the arts were the two loves of this exceptional woman. In 1989 she was awarded the prestigious Israel Prize for
her many contributions to Israeli society, among them the founding of Israel’s Batsheva and Bat Dor Dance Companies.
The Batsheva Fund's purpose is to further Science in Israel for the people of Israel.
Former Biophysics Chair and Senior Dean of Graduate Studies Dies
Tuesday, March 13, 2012
Paul L. LaCelle, M.D., a University of Rochester Medical Center faculty member for more than 40 years, a former department chair and former senior dean, died March 9. He was 82.
Dr. LaCelle, a 1959 graduate of the University's School of Medicine and Dentistry, joined the faculty in 1964 as an instructor of what was then the Department of Radiation Biology and Biophysics. He was named a professor in 1974 and chaired what is now the Department of Biochemistry and Biophysics from 1977 to 1996.
Each Flick of a Digit Is a Job for All 5
Monday, February 27, 2012
You may think you're pretty familiar with your hands. You may think you know them like the back of your hand. But as the following exercises derived from the latest hand research will reveal, your pair of bioengineering sensations still hold quite a few surprises up their sleeve.
Our fingers can seem like restless Ariels, so fast and dexterous you'd think they had plans and options of their own. Yet as scientists who study the performance, circuitry and evolution of the human hand have lately determined, the appearance of digital independence is deeply deceptive.
Even when you think you're moving just one finger,
said Marc H. Schieber, a professor of neurology and neurobiology at the University of Rochester Medical Center, you're really controlling your entire hand.
The pianist playing Ravel or the typist clacking on Blogspot? People tend to think, they're hitting one key at a time, so they must be moving one finger at a time to hit that key,
Dr. Schieber said. But really, all the fingers are in motion all the time.
Antipsychotic Meds Tied to Diabetes in Kids
Wednesday, November 23, 2011
The antipsychotic drugs that are increasingly being used to treat bipolar disorder, autism and other mental disorders in children may come with an increased risk of diabetes, a new study suggests. Previous research has linked the so-called second-generation antipsychotics to an increased risk of diabetes in adults. And there's been some evidence that the drugs can cause weight gain in children.
The new findings, published in the Journal of Pediatrics, add to concerns that the medications may ultimately lead to diabetes in some kids. And it's the growing use of the drugs in kids—particularly for conditions in which the benefit is unclear—that makes the potential diabetes risk concerning, according to Dr. Jonathan Mink, chief of child neurology at the University of Rochester Medical Center in New York.
These medications can be very helpful in certain settings,
said Mink, who is also part of a pediatric advisory panel to the U.S. Food and Drug Administration. In September, the panel recommended that the agency keep monitoring the risks of weight gain and diabetes in children on antipsychotics.
Autistic Children May Have Too Many Brain Cells, Study Says
Tuesday, November 8, 2011
The brains of autistic children have far more neurons in the prefrontal cortex than the brains of kids without autism, finds a new study that could advance research into the disorder. For the first time, we have the potential to understand why autism gets started,
said study author Eric Courchesne, a professor of neurosciences at the University of California, San Diego School of Medicine and director of the Autism Center of Excellence.
The prefrontal cortex is key to complex thoughts and behaviors, including language, social behavior and decision-making. The dorsolateral prefrontal cortex is closely linked with executive function,
including planning, reasoning and very high level cognition,
said Lizabeth Romanski, an associate professor of Neurobiology & Anatomy at the University of Rochester Medical Center, who was not involved with the research. The medial prefrontal cortex is thought to be important to social and other behavior and emotions.
Jacqueline Williams, Major Lab Collaborator, Appointed to Prestigious Leadership Positions
Thursday, November 3, 2011
Jacqueline P. Williams, Ph.D., a University of Rochester faculty member and internationally recognized expert in radiation biology, has been named to leadership positions at three of the leading radiation oncology and research organizations in the world.
The American Society for Radiation Oncology (ASTRO) named Williams chair of its Scientific Research Council at the Society's 53rd annual meeting, held in Miami Beach, Fla. Williams was also recognized as one of 21 distinguished members that received ASTRO's Fellow designation at a ceremony during the meeting.
Neuroscience Holds Annual Retreat
Wednesday, October 19, 2011

Faculty members, students, staff, and postdoctoral
fellows at the 2011 Neuroscience Retreat.
On October 17, 2011, the 2011 Neuroscience retreat was held at the Memorial Art Gallery in Rochester, NY. There was a great turnout for the event with 147 faculty, staff, postdoctoral fellows, and students in attendance.
Some of the highlights included M.D./Ph.D. student, Mike Wu, winning the award for the best student poster, Sustained Interleukin-1β Expression Severely Impairs Adult Hippocampal Neurogenesis Despite Voluntary Running and Emily Kelly, an NBA post-doctoral fellow, winning the award for the best postdoc poster, Ultrastructural Distribution of ICAM-5 (Telencephalin) in Mouse Visual Cortex.
The retreat was capped off by several intriguing lectures and presentations, a poster session, great food, and a terrific keynote/Notter lecture by Dr. Carol Barnes.
MSTP Student Elected to Board of SNMA
Thursday, October 6, 2011
Bisi Lawal, an M.D./Ph.D. student at the University of Rochester School of Medicine and Dentistry, has been elected to the board of directors of the Student National Medical Association (SNMA). Lawal, a native of Houston, is the regional director for medical schools in New York and New Jersey. The SNMA is the nation's oldest and largest, independent, student-run organization focused on the needs and concerns of medical students of color.
NBA Associate Professor, Dr. Barbara Davis, Ph.D., Honored for Excellence in Teaching
Tuesday, October 4, 2011
Associate Professor Barabara Davis, Ph.D., in the department of Neurobiology & Anatomy, has once again been honored for excellence in teaching. She has been honored six times recently (five years in a row) for Commendations for Excellence in Teaching in the First Year (2006, 2008, 2009, 2010, 2011, 2012), and was the recipient of the Alumni Association Gold Medal Award for Excellence in Teaching in 2006. A faculty member at the University of Rochester since 1984, this is Dr. Davis's 16th teaching award since 1995.
Dr. Davis is currently the course director for the anatomic sciences strand of HSF where she teaches anatomy and histology. She also teaches the carbohydrate metabolism section of Molecules to Cells, teaches in the Mind Brain Behavior course, a human anatomy course (BME 258) for the Biomedical Engineering department, the anatomy component of the SURF program, and runs the Prematriculation Human Biology course. Additionally, she is also the director of the Medical Education Pathway.
NBA Assistant Professor, David Kornack, Ph.D., Awarded Goldman Prize for Excellence in Teaching
Tuesday, October 4, 2011
![David]()
Dr. David Kornack as he receives his award
from Alexis Pilato, Class of 2014
Assistant Professor David Kornack, Ph.D., in the department of Neurobiology & Anatomy, has received The Manuel D. Goldman Prize for Excellence in First Year Teaching. This prize was established in 1981 in memory of Manuel D. Goldman and is awarded each year by the first year class to recognize a member of the faculty for excellence in first year teaching.
Dr. Kornack, who is very popular among the NBA and NGP students, teaches the first year medical course, Human Structure and Function and the neuroscience course, Mind, Brain & Behavior. He also co-directs a course with Dr. Kathy Nordeen for the Neuroscience majors called NSC 203: Laboratory in Neurobiology and directs the course NSC 302: Senior Seminar in Neuroscience. In addition, he lectures in the undergraduate courses, BCS 249: Developmental Neurobiology and BME 258: Human Anatomy.
MSTP, NSC Graduate Student Receives F30 Fellowship
Thursday, September 8, 2011
MSTP, NSC graduate student, Adrianne Chesser, has received an F30 Fellowship from the National Institute of Environmental Health Sciences, for her project entitled: Mitochondrial Dynamics Underlie Gene-Environment Interactions in Parkinson's.
The mission of the NIEHS is to reduce the burden of human illness and disability by understanding how the environment influences the development and progression of human disease.
Healthy Living: Batten Disease
Monday, August 29, 2011
Staring at a computer screen wasn't exactly what Nicole Newhouse envisioned for her career. It didn't take long for her to find a subject that sparked a new passion. Newhouse said, You have children that are dying. Point blank, you have children that are dying.
Newhouse is enrolling patients in the first controlled clinical trial for batten disease. We don't have a cure right now. We can't tell parents 'you take this and your child's going to be ok,
said Newhouse.
Batten disease is a neurological disorder that usually appears in children ages four to eight years old. Early symptoms of the disease include sudden vision problems. That's quickly followed by a loss of motor skills, mental impairment and eventually death. Try to imagine what it's like for the parents to watch their child basically dying before their eyes. Over many years, it's the kind of thing that as a physician you see and think you know I want to do something to help,
said Dr. Jonathan Mink, professor in the departments of Neurology, Neurobiology & Anatomy, Pediatrics, and Brain and Cognitive Sciences at the University of Rochester Medical Center.
Award to Neuroscientist Boosts Mental Health Research
Wednesday, August 17, 2011
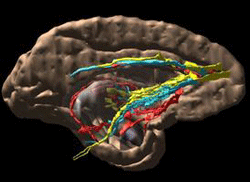
Brain areas involved in making decisions
about rewards are highlighted.
A Rochester neuroscientist whose laboratory research has already helped patients has received a prestigious award to explore new opportunities to help people with conditions like schizophrenia, depression, obsessive-compulsive disorder, and addiction.
Suzanne Haber, Ph.D., professor of Pharmacology and Physiology at the University of Rochester Medical Center, has received a Distinguished Investigator Grant from the Brain and Behavior Research Foundation. She is one of 15 scholars nationwide to receive the award, also known as a NARSAD award (the foundation was previously known as the National Alliance for Research in Schizophrenia and Depression). Each recipient receives $100,000 toward new research aimed at alleviating the suffering caused by mental illness.
Haber is a world leader uncovering and understanding the wiring in a highly sophisticated part of the brain known as the prefrontal cortex -- the part of the brain involved in decision-making that involves reward and potential risk. The prefrontal cortex is what prompts us to forego a box of cookies for breakfast, for instance, so we can reach our long-term weight-loss goal, or that helps keep a student studying late at night in the quest to obtain her college degree, instead of partying with friends.
UR Research Group Wins Provost Multidisciplinary Research Award
Friday, June 3, 2011
A current study by researchers at the University of Rochester entitled, Perception of Music and Language through Auditory Interference, has been selected as the recipient of the Provost Multidisciplinary Research Award.
The work is based on the ability to filter interfering auditory signals from a primary stream is a basic aspect of social and musical communication. Musical performance requires continuous attention to a complex auditory signal: how does this expertise interface with the processing of linguistic signals? Is auditory filtering ability facilitated by musical training?
In order to explore the above questions, this study brings together researchers with expertise in the following fields:
First Controlled Clinical Trial for Juvenile Batten Disease to Start
Tuesday, May 31, 2011
After years of building hope for a treatment, Rochester researchers and clinicians will begin the first controlled clinical trial for Juvenile Batten disease this summer, thanks to $1 million in grants from the Food and Drug Administration (FDA) and the Batten Disease Support and Research Association (BDSRA). The trial will examine whether mycophenolate mofetil, a drug FDA-approved to suppress the immune system and prevent organ rejection in children, is safe for these children and whether it can slow or halt the progression of the fatal neurodegenerative disease.
“Families have been anxiously awaiting word on when we could launch this clinical trial,” said Frederick Marshall, M.D., principal investigator of the trial and Associate Professor of Neurology. “Juvenile Batten Disease is very rare, but the families are very close and well-informed about potential treatments. They have been watching the progress of this research and hoping for the day when we could launch the trial.”
Juvenile Batten disease is a lysosomal-storage disease that strikes seemingly healthy children and progressively robs them of their abilities to see, reason and move. It ultimately kills them in late adolescence or young adulthood. Batten disease is in the same family of diseases as Krabbe disease to which former Buffalo Bills quarterback Jim Kelly lost his son, Hunter, in 2005.
Laurel Carney Awarded Engineering Professor of the Year
Sunday, May 1, 2011
Congratulations to Professor Laurel Carney, who was recognized by the Student Association as the Engineering Professor of the Year at the prestigious annual University of Rochester Undergraduate Research Symposium. Undergrad Travis Bevington, BME '12, said, in presenting the award, Even with all of her research, Professor Carney manages to find time to spend countless hours with students on projects and it really proves how much she cares about our success as students. She really serves as an outlet to different opportunities that students might be unaware of, such as finding a lab position or research opportunity. Beyond the classroom, Professor Carney is always in high demand for letters of recommendation—students really feel like she takes the time to get to know all of us, even if her deck of cards in class can be quite intimidating!
(Dr. Carney has a deck of playing cards, with one card for each student. Cards are drawn during class to direct questions to the students.)
Said Professor Carney about the award, Since coming to UR 4 years ago, I've been greatly impressed by the quality of the undergraduates here and have really enjoyed my classes. Receiving this recognition from the students is a great honor. On the other hand, I think it provides objective evidence that my courses are too easy; I intend to remedy this situation as quickly as I can!
Pre-Conception and Early Pregnancy Iron Deficiency Harms Brain
Tuesday, March 22, 2011
A mother's iron deficiency early in pregnancy may have a profound and long-lasting effect on the brain development of the child, even if the lack of iron is not enough to cause severe anemia, according to a University of Rochester Medical Center study published in the scientific journal PLoS One.
What convinced us to conduct the present study were our preliminary data suggesting that cells involved in building the embryonic brain during the first trimester were most sensitive to low iron levels,
said Margot Mayer-Proschel, Ph.D., the lead researcher and an associate professor of Biomedical Genetics at URMC.
Co-author Anne Luebke, Ph.D., an associate professor of Biomedical Engineering and Neurobiology & Anatomy at UR, suggested and directed the use of ABR testing, which can detect the speed of information moving from the ear to the brain.
Robert Doty, Eminent Neuroscientist, Dies at 91
Tuesday, January 18, 2011

Robert Doty
It is with deep personal sadness that I inform the Department of Neurobiology and Anatomy, as well as the broader neuroscience and UR community, that our own Bob Doty passed away on Friday, January 14th, 2011. Bob had been a monumental presence in our midst for decades, and was arguably our most eminent neuroscientist on campus. A friend to many, and admired by all who knew him, we will miss his remarkable and steadfast presence among us, as well as his routine appearance at seminars--always with that extraordinary flair for insightful questions and comments. It was truly fitting that our last departmental winter banquet was held in honor and celebration of Bob near his 90th birthday. At the wishes of Bob's family, plans for a memorial will be considered in the spring.
- Gary D. Paige, M.D., Ph.D., Chair Department of Neurobiology & Anatomy
Microglia: A Standing Ovation, Please!
Friday, January 14, 2011
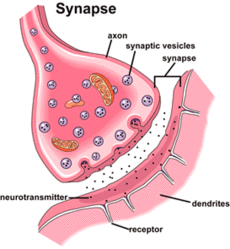
Structure of a Synapse
New research from the Majewska Lab at University of Rochester Medical Center is revealing even more reasons to stand up and applaud the microglia. It turns out that microglia serve more than immune functions. They are essential to learning and memory. This research suggests that a lot of what is going on in that synaptic gap is engineered by the microglia.
The research team, led by Ania Majewska, Ph.D., Assistant Professor in the department of Neurobiology & Anatomy, used two imaging techniques to study the microglia in the animals' brains during these various stages. When the lights were off, microglia contacted more synapses, were more likely to reach toward a particular type of synapse, tended to be larger, and were more likely to destroy a synapse. When the lights came back on, most of those activities reversed.
The finding that activity among microglia changed in response to visual inputs was, in itself, surprising. Just the fact that microglia can sense that something has changed in the environment is a novel idea,
says Majewska.
Professor Laurel Carney Receives a 2010 R01 Grant
Monday, November 15, 2010
Biomedical Engineering and Neurobiology & Anatomy Professor Laurel Carney has received funding for her 2010 R01 grant entitled: Developing and Testing Models for the Auditory System with & without Hearing Loss
. This study involves testing listeners with both normal hearing and hearing loss. The project focusses on the development of computational models that will assist in the testing of signal processing strategies for hearing aids.
She also received a renewal for five years of support from the NIH-NIDCD to study Auditory Processing of Complex Sounds; this renewal extends this research program to 20 consecutive years of NIH funding. Her research has resulted in better understanding of the physiological response to sound in the healthy auditory system, and may contribute to the improvement of hearing aids for those with hearing loss.
Majewska Lab Research Featured in Nature Highlights
Wednesday, November 10, 2010
The Majewska Lab's current research on learning and memory has been featured in the current issue of Nature Highlights. The research details immune cells called microglia help to protect the brain after an injury. They may also be involved in pruning the connections, or synapses, between neurons — a key process in learning and memory formation.
Using electron microscopy, Marie-Ève Tremblay, Rebecca Lowery and Ania Majewska at the University of Rochester in New York imaged mouse brain slices and reconstructed the interactions between microglia and synapses in three dimensions. Most of the microglia were directly adjacent to the synapses, and in particular to dendritic spines — neuronal structures — that were small and were often pruned away later on.
How Some Brain Cells Hook Up Surprises Researchers
Tuesday, November 2, 2010

Marie-Ève Tremblay, Ph.D., and Ania Majewska, Ph.D.
Immune cells known as microglia, long thought to be activated in the brain only when fighting infection or injury, are constantly active and likely play a central role in one of the most basic, central phenomena in the brain -- the creation and elimination of synapses.
The finding, reported in the Nov. 2 issue of PloS Biology, catapults the humble microglia cell from its well-recognized duty of protecting the brain to direct involvement in creating the cellular networks at the core of brain behavior.
When scientists talk about microglia, the talk is almost always about disease. Our work suggests that microglia may actively contribute to learning and memory in the healthy brain, which is something that no one expected,
said Ania Majewska, Ph.D., assistant professor in the Department of Neurobiology & Anatomy who led the work.
The group's paper, co-authored by post-doctoral associate, Marie-Ève Tremblay, Ph.D., is a remarkably detailed look at how brain cells interact with each other and react to their environment swiftly, reaching out constantly to form new links or abolish connections.
Associate Professors in NBA Receive Teaching Awards
Friday, September 3, 2010
Associate Professors, in the department of Neurobiology & Anatomy, Martha Gdowski and Barbara Davis have both received awards for excellence in teaching. Dr. Davis received a Commendation for First Year Teaching from the class of 2013 and Dr. Gdowski received The Manuel D. Goldman Prize for Excellence in First Year Teaching. This prize was established in 1981 in memory of Manuel D. Goldman and is awarded each year by the first year class to recognize a member of the faculty for excellence in first year teaching.
Jacqueline Williams, Major Lab Collaborator, Awarded $15M to Expand Bioterrorism Research
Wednesday, August 11, 2010
The University of Rochester Medical Center has received $15 million in federal bioterrorism funding that allows investigators to build on several discoveries made during the past five years to improve the ability to treat radiation injuries, especially from an act of terrorism.
URMC was awarded an initial grant of $21 million in 2005 to become part of a national research network, Centers for Medical Countermeasures Against Radiation. The centers were charged with researching how best to respond to a dirty bomb or other radiological or nuclear attack.
A second, $15 million, five-year award, received this month from the National Institutes of Health/National Institute of Allergy and Infectious Disease, will allow URMC researchers to focus on testing known drugs and experimental agents and their ability to ward off systemic radiation injury that affects the lungs, brain, skin and bone marrow.
Scientists Rate University a Best Place To Work
Wednesday, June 30, 2010
The University has been ranked one of the top 15 institutions in the nation for scientists to work, according to The Scientist magazine, which has published its annual survey of Best Places to Work for Scientists in Academia.
"Photons and Neurons": 27th CVS Symposium
Thursday, June 17, 2010
Earlier this month, the Center for Visual Science (CVS) held its 27th symposium. The theme of this year's symposium was Photons and Neurons
and it brought together scientists who develop and use optical imaging methods from all over the world.
Optical imaging promises to revolutionize neuroscience by offering minimally-invasive, direct recording of neural activity at single cell resolution in the intact working brain. Optical imaging of neural activity, however, has yet to deliver the ultimate prize of recording the activity of many individual neurons in real time throughout the depth of a brain structure such as the cerebral cortex. Achieving such a goal will require the coordinated effort of experts from disparate backgrounds, including neuroscientists, optical engineers, biochemists and molecular biologists.
The symposium brought together this diverse group of scientists and provided a platform for discussion of the latest developments in optical imaging of neuronal function. Discussions were long and lively and allowed the exchange of ideas, identification of pressing neurobiological questions, discussion of current limitations, and developing of ideas for possible solutions. The symposium was supported by the National Eye Institute (R13EY020691) and the Center for Visual Science, and was co-organized by David Williams, Ania Majewska and Tony Movshon (NYU).
Youngsun Cho is Awarded NRSA Individual Training Grant
Friday, June 11, 2010
Youngsun Cho, a first year MSTP student in the Fudge Lab was recently awarded a Ruth Kirschstein National Research Service Award (F30) for three years of training. Youngsun's proposed studies involve examining circuitry that may underlie modulation of approach behavior in anxious adolescents. She will first detail connections between specific regions of the prefrontal cortex the amygdala in animals, based on her work in Rochester. This data will then be used to design studies investigating functional connectivities between these regions in anxious adolescents. The latter studies are being conducted in partnership with Dr. Monique Ernst at the NIMH intramural program.
Anne Luebke, Ph.D. and Loisa Bennetto, Ph.D. Awarded Collaborative Pilot Grant
Thursday, June 3, 2010
Anne Luebke, Ph.D., Associate Professor in Neurobiology & Anatomy and Biomedical Engineering, and Loisa Bennetto, Ph.D., Chair of the Department of Clinical and Social Psychology, have been awarded a collaborative pilot grant to study whether physiological-based biomarkers of cochlear efferent strength will be impaired in the autism spectrum disorder (ASD) population.
The specific aim of the project is to determine efferent feedback strength in children and adolescents with ASD when compared with typical controls (age, gender, and IQ matched). The project will build on existing measures of MOC strength using two different otoacoustic emission-based tests with short and sustained binaural broadband suppression to obtain maximal efferent feedback strength in both ears of all participants.
Acupuncture’s Molecular Effects Pinned Down
Sunday, May 30, 2010
Scientists have taken another important step toward understanding just how sticking needles into the body can ease pain.
In a paper published online May 30 in Nature Neuroscience, a team at the University of Rochester Medical Center identifies the molecule adenosine as a central player in parlaying some of the effects of acupuncture in the body. Building on that knowledge, scientists were able to triple the beneficial effects of acupuncture in mice by adding a medication approved to treat leukemia in people.
The new findings add to the scientific heft underlying acupuncture, said neuroscientist Maiken Nedergaard, M.D., D.M.Sc., who led the research. Her team is presenting the work this week at a scientific meeting, Purines 2010, in Barcelona, Spain.
URMC Named Batten Disease Center of Excellence by BDSRA
Wednesday, May 12, 2010
Lance Johnston, Executive Director of the BDSRA, awarding Dr. Jonathan Mink with the Batten Disease Center of Excellence plaque.
The largest Batten Disease research and support organization in North America named the University of Rochester Medical Center (URMC) as a Batten Disease Center of Excellence today. The Ohio-based organization, Batten Disease Support and Research Association, has chosen URMC because of its comprehensive services for patients and its long clinical and research history with the disease.
Batten Disease is a rare neurodegenerative syndrome that erupts with little warning. It first steals sight, then cripples cognitive and motor capacities, and while different variations of the disease brings a difference age of onset and progression, it is, ultimately, terminal. The most common form is juvenile, in which symptoms begin between 5 and 8 years of age. There are between 500 and 1,000 people with Batten Disease in the United States and only a few thousand in the world.
Finding treatment with a comprehensive team that has experience with the disease is incredibly hard for families,
said Jonathan Mink, M.D., Ph.D., chief of Child Neurology and professor of Neurology, Neurobiology & Anatomy and Pediatrics at URMC. The Batten Disease Support and Research Association is hoping to streamline families’ search for expertise by endorsing centers like ours.
MD/PhD student Youngsun Cho leaves to begin "mini-sabbatical" training at NIMH
Thursday, April 1, 2010
Youngsun Cho, an MD/PhD student in the laboratory of Dr. Julie Fudge, leaves to begin "mini-sabbatical" training in functional MRI and studies in anxious adolescents at with colleagues at NIMH. Youngsun is interested in structural and functional brain connections that influence reward and punishment anticipation in adolescents, and she will take anatomical studies from the laboratory to the next phase of her training with Dr. Monique Ernst in the Section on Mood and Anxiety Disorders at NIMH.
NBA Students Win First Prize at 8th Annual Collier Mental Health Poster Session
Wednesday, March 31, 2010
Michele Saul (NBA graduate student) and Dan Tylee (undergraduate assistant) each won first prize honors at the 8th Annual Collier Mental Health Poster Session, sponsored by the Department of Psychiatry. Michele presented new work on the effects of stress on amygdala development in adolescent animals. Dan's showed that a coping behavior during stress ameliorates subsequent anxiety behavior in adult animals.
Undergraduate Neuroscience Student Awarded a deKiewiet Fellowship
Wednesday, March 24, 2010
We are delighted to announce that Kathryn Cooper, an undergraduate Neuroscience student at UR, has been awarded a deKiewiet Fellowship to support a research project with NBA faculty members Bill O'Neill and Gary Paige. Katie began her work in the Paige/O'Neill lab through the University's GEBS Summer Scholars Program in 2009. She continues to work on important aspects of a novel phenomenon discovered in this lab by which changes in eye position shift auditory spatial perception in the same direction as eye movement over time.
The Undergraduate Program in Biology and Medicine (UPBM) invites students in their junior year to submit competitive applications for deKiewiet Fellowships. Awardees receive a $4000 stipend to work for ten weeks during the summer in the lab of their research mentors. They present their research in the UPBM Poster Session in October.
New NIH Training Grant for Hearing, Balance, and Spatial Orientation Research
Friday, March 5, 2010
The University of Rochester has recently been awarded a Training Grant (T32) from the NIH National Institute on Deafness and Other Communication Disorders entitled Training in Hearing, Balance, and Spatial Orientation.
This Training Grant involves the collaborative efforts of the Departments of Otolaryngology, Biomedical Engineering, and Neurobiology & Anatomy. The Grant will support PhD students, MD-PhD students, Post-doctoral fellows and Medical Residents in BME, Neuroscience, and Otolaryngology who are involved in research related to the auditory and vestibular systems. This Training Grant is an important resource for the University of Rochester's Center for Navigation and Communication Sciences, which provides technical and administrative support for 25 faculty members who are conducting research in this area. The 5-year grant will provide approximately $1.5 million dollars of support for several trainees each year. In association with the Training Grant, a new graduate-level course entitled Hearing and Balance: Structure, Function and Disease
will be offered starting in Fall 2010. This new Training Grant is an exciting advance for the strong and growing community of auditory and vestibular researchers at the University of Rochester.
Dr. Robert Doty Honored at 2010 NBA Winter Party
Saturday, February 27, 2010
The 2010 Neurobiology & Anatomy Winter Party was a truly special event celebrating the 90th birthday of Professor Robert W. Doty, PhD. On hand to honor Dr. Doty were University President Joel Seligman, Dean of the University of Rochester Medical Center, Mark Taubman, MD, and Provost, Ralph Kuncl. The celebration included remarks and anecdotes by department chair, Dr. Gary Paige and President Seligman, as well as a rousing speech from the guest of honor. President Seligman was especially impressed by an autobiographical SFN publication that Dr. Doty had written. The department of Neurobiology & Anatomy would like to thank Dr. Doty for his many contributions over the years and wish him a very happy 90th birthday!
MD/PhD Student Danielle deCampo Wins URMC CTSI Travel Award
Friday, February 5, 2010
Danielle deCampo, an MD/PhD student in the laboratory of Dr. Julie Fudge, has won a URMC CTSI Travel Award. Danielle will now be able to pursue training opportunities in performing laser capture microscopy and microarray analysis with collaborators at University of Pittsburgh. This is an opportunity to add to her "technical toolbox" as she tries to characterize specific neuronal populations that may play a role in mood disorders.
Dr. Patricia M. White Joins NBA Faculty
Monday, February 1, 2010
It is a pleasure to welcome Patricia M. White, PhD to our faculty as Assistant Professor of Neurobiology & Anatomy and Otolaryngology. Her work fits solidly within a key research initiative in Neurobiology and Anatomy that we refer to as sensory-motor neuromedicine. Pat carries an important new area to the University in sensory regeneration of the inner ear, or hair-cell regeneration. This promising area of translational research targets cultured stem/progenitor cells to restore hearing through implantation into damaged cochlea and/or vestibule, or alternatively, exploits existing supporting cells to reenter the cell cycle, effectively become progenitors once again, and ultimately restore sensory structure and function.
Jacqueline Williams, Major Lab Collaborator, Chairs National Space Biomedical Research Institute Science Committee
Wednesday, January 27, 2010
Jacqueline Williams, Ph.D., was named chair of the National Space Biomedical Research Institute's Scientific Advisory Committee for its Center of Acute Radiation Research. Williams is grant director and core leader of the Center for Biophysical Assessment and Risk Management Following Irradiation at the University of Rochester Medical Center.
NSBRI is a NASA-funded consortium of institutions studying the health risks related to long-duration spaceflight and developing countermeasures to mitigate the risks. The CARR, which is headed at the University of Pennsylvania School of Medicine, is responsible for studying the acute effects of exposure to space radiation during exploration missions. The Scientific Advisory Committee provides advice on the Center's productivity and effectiveness.
Dr. John Hansen Receives Presidential Diversity Award
Friday, January 22, 2010

Dr. John Hansen accepts his award from Dr. Vivian Lewis and President Joel Seligman
The University of Rochester Presidential Diversity Awards were created in 2009 by President Joel Seligman to recognize faculty, staff, students, units, departments or teams that demonstrate a commitment to diversity and inclusion through recruitment and retention efforts, teaching, research, multi-cultural programming, cultural competency, community outreach activities, or other initiatives.
Among the first recipients was Dr. John Hansen, professor and associate chair of Neurobiology & Anatomy and associate dean for admissions at the School of Medicine and Dentistry. Dr. Hansen, was honored for his more than 20 years of dedicated efforts to increase the recruitment, retention, and graduation of medical school candidates from diverse backgrounds. He also has been honored nationally for his teaching and has received the Gold Medal Award of the medical school's Alumni Association.
NSC Graduate Student, Cory Hussar, Publishes an Article in December 2009 Edition of Neuron
Monday, December 14, 2009
Cory Hussar, a 5th year Neuroscience graduate student in Dr. Tania Pasternak's lab (NBA) has published an article in this month's edition of Neuron
. The article, entitled Flexibility of sensory representations in prefrontal cortex depends on cell type,
reports that neurons in prefrontal cortex (PFC) represent visual motion with precision comparable to cortical neurons at early stages of motion processing, and readily adapt this representation to behavioral context. Furthermore, results show that flexible sensory representation during active discrimination tasks is achieved in the PFC by a specialized neuronal network of both NS neurons readily adjusting their selectivity to behavioral context, and BS neurons capable of maintaining relatively stable sensory representation.
Helen Wei and Youngsun Cho Accepted into MSTP Program
Wednesday, December 9, 2009
Congratulations to Helen Wei and Youngsun Cho, both recently accepted into the MSTP (MD-PhD program) from the MD-MS Program in Medical Neurobiology. We are delighted to welcome them to a continued and augmented commitment to neuroscience research as they now pursue their PhD candidacy and thesis projects.
Scientists Create a 'Golden Ear' Mouse with Great Hearing as It Ages
Tuesday, November 10, 2009
What do you get when you cross a mouse with poor hearing and a mouse with even worse hearing? Ironically, a new strain of mice with golden ears
- mice that have outstanding hearing as they age.
The work by one of the world's foremost groups in age-related hearing loss, or presbycusis, marks the first time that scientists have created the mouse equivalent of a person with golden ears
- people who are able to retain great hearing even as they grow older. The research at the University of Rochester Medical Center was published online recently in the journal Neurobiology of Aging.
The new mouse is expected to offer clues about how these lucky folks are able to retain outstanding hearing even through old age. Researchers estimate that approximately 5 percent of people, mainly women, fall into this category. The new mice created in the laboratory of Robert Frisina, Ph.D., embody many of the same traits of human golden ears
because of an astute cross of two types of mice long popular with researchers.
Dr. Gary Paige has been elected President & Conference Chair of the Society for the Neural Control of Movement
Wednesday, October 28, 2009
Gary D. Paige, M.D., Ph.D., professor and chair of Neurobiology and Anatomy, has been elected President and Conference Chair of the Society for the Neural Control of Movement. The Society serves as an international forum for scientists, physicians, educators and students bound by a common interest in the neural systems that underlie the control of movement, and in disorders of these systems. The NCM Annual Conference, held each spring, is the premier international conference dedicated to the presentation of novel research and interchange of ideas related to major issues in the field.
Dr. Kerry O'Banion featured in NASA Fall Newsletter
Thursday, October 1, 2009
The son of two educators, Kerry O’Banion has always adopted a broad view in his scientific pursuits. As an undergraduate at the University of Illinois in Urbana-Champaign, he investigated pair bonding behavior in common prairie voles, but chose Microbiology for his PhD work because of the promise of immersing himself in molecular biology. Indeed, at the same time he was learning about human pathophysiology and how to do a proper neurological examination as an MD-PhD trainee in the nascent Medical Scholars Program, also at the University of Illinois in Urbana-Champaign, Kerry entertained working with Carl Woese, who had established the existence of a new kingdom of organisms (Archaea) by sequencing rRNA. Ultimately Kerry carried out his thesis work with Manfred Reichmann in Microbiology and John Sundberg in the Department of Veterinary Pathobiology to characterize and clone novel animal papillomaviruses. All together, he cloned viruses from six animal species and witnessed at national and international conferences the recognition that oncogenic human papillomaviruses caused cervical and other epithelial cancers.
$10.5 Million in Funding Creates Center to Study OCD
Wednesday, September 30, 2009
A new research center exploring the science underlying a potential new treatment for obsessive-compulsive disorder has been established at the University of Rochester Medical Center, thanks to a $10.5 million award from the National Institute of Mental Health.
Rochester will serve as the hub of a five-year collaborative effort that includes six institutions around the nation and in Puerto Rico. The prestigious Silvio O. Conte Center will link more than 50 researchers who will focus on how deep brain stimulation affects people with obsessive-compulsive disorder.
Obsessive-compulsive disorder is a truly debilitating disease for some patients,
said Rochester neuroscientist Suzanne Haber, Ph.D., professor of Pharmacology and Physiology, who heads the center. While treatment helps most patients lead fulfilling lives, there are a few for whom today's therapies simply don't work. Our center is designed to explore the science and the effects of deep-brain stimulation, which has been effective for some other diseases involving the brain, such as Parkinson's disease.
Dr. Edward Brown Receives an NIH Director's New Innovator Award
Wednesday, September 30, 2009
Dr. Edward Brown has received an NIH Director's New Innovator Award to support a 5 year/$1.5M study that seeks to understand the cells and signals responsible for collagen organization in tumor-draining lymph nodes (TDLNs). This study exploits an optical phenomenon called Second Harmonic Generation (SHG) which allows for the microscopic imaging of ordered collagen fibers within living tissue. Tumor cells can exploit these ordered fibers during metastasis, and Dr. Brown hopes to determine the cells and signals which influence the SHG+ fibers in order to disrupt their production and inhibit metastasis via the TDLN, which is a primary route. He will also explore the ability of SHG imaging of TDLN biopsies to predict metastatic ability, to aid in customization of postoperative therapy. This project continues work that has been previously funded by a D.o.D. Era of Hope
Scholar Award and a Pew Scholar in the Biomedical Sciences Award, and complements a recently awarded D.o.D. Era of Hope
Scholar Research Award.
Dr. Edward Brown Receives a D.o.D. Breast Cancer Research Program Grant
Friday, August 28, 2009
Dr. Edward Brown has received funding from the Department of Defense Breast Cancer Research Program to support a 5 year/$2M study that seeks to understand the cells and signals responsible for collagen organization in breast tumors. This study exploits an optical phenomenon called Second Harmonic Generation which allows for the microscopic imaging of ordered collagen fibers within breast tumor models. Breast tumor cells exploit these ordered fibers to escape the tumor mass, and Dr. Brown hopes to determine the cells and signals which influence the SHG+ fibers in order to disrupt their production and inhibit metastasis. He will also explore the ability of SHG imaging of breast tumor biopsies to predict metastatic ability, to aid in customization of postoperative therapy. This project continues work that has been previously funded by a D.o.D. Era of Hope
Scholar Award and a Pew Scholar in the Biomedical Sciences Award.
The annual Elizabeth Doty Lecture at the University of Rochester, Consciousness from Neurons, will be given by Randy L Buckner
Wednesday, August 19, 2009
The annual Elizabeth Doty Lecture at the University of Rochester, Consciousness from Neurons, will be given by Randy L Buckner, Depts of Psychology & Neuroscience, Harvard University: The Brain’s Default Network: Implications for Consciousness
, Monday, 2 November 2009.
Blue Dye May Hold Promise in Treating Spinal Cord Injury
Tuesday, July 28, 2009
A compound strikingly similar to the common food additive that gives M&Ms and Gatorade their blue tint may offer
promise for preventing the additional – and serious – secondary damage that immediately follows a traumatic injury
to the spinal cord. In an article published online today in the Proceedings of the
National Academy of Sciences, researchers report that the compound Brilliant Blue G (BBG) stops the
cascade of molecular events that cause secondary damage to the spinal cord in the hours following a spinal cord
injury, an injury known to expand the injured area in the spinal cord and permanently worsen the paralysis for
patients.
This research builds on landmark laboratory
findings first reported five years ago by researchers at the University of Rochester Medical Center. In the
August 2004 cover story of Nature Medicine, scientists detailed how ATP, the vital energy source that keeps our
body’s cells alive, quickly pours into the area surrounding a spinal cord injury shortly after it occurs, and
paradoxically kills off what are otherwise healthy and uninjured cells.
This surprising discovery marked a milestone in establishing how secondary injury occurs in spinal cord patients. It
also laid out a potential way to stop secondary spinal injury, by using oxidized ATP, a compound known to block
ATP’s effects. Rats with damaged spinal cords who received an injection of oxidized ATP were shown to recover much
of their limb function, to the point of being able to walk again, ambulating effectively if not gracefully.
MD-MS Students Continue Their Graduate Education in the NBA PhD Program
Friday, June 12, 2009
Congratulations to MD-MS students Helen Wei and Youngsun Cho who have each chosen to continue their graduate education and research in the NBA PhD program before returning to medical school, and have each received additional support from the Clinical Translational Science Institute (CTSI).
Greg Gdowski, PhD, elected Chair of the Rochester Section of the Society for Engineering in Medicine and Biology
Wednesday, April 1, 2009
Greg Gdowski, Ph.D., has been elected Chair of the Rochester Section of the Society for Engineering in Medicine and Biology. The Society is an organization within the framework of the Institute of Electrical and Electronics Engineers (IEEE) whose members maintain principal professional interest in biomedical engineering.
Rigorous Visual Training Teaches the Brain to See Again After Stroke
Wednesday, April 1, 2009
By doing a set of vigorous visual exercises on a computer every day for several months, patients who had gone partially blind as a result of suffering a stroke were able to regain some vision, according to scientists who published their results in the April 1st issue of the Journal of Neuroscience.
We were very surprised when we saw the results from our first patients,
said Krystel Huxlin, Ph.D., the neuroscientist and associate professor who led the study of seven patients at the University of Rochester Flaum Eye Institute. This is a type of brain damage that clinicians and scientists have long believed you simply can't recover from. It's devastating, and patients are usually sent home to somehow deal with it the best they can.
Astrocytes Help Separate Man from Mouse
Monday, March 23, 2009
A type of brain cell that was long overlooked by researchers embodies one of very few ways in which the human brain differs fundamentally from that of a mouse or rat, according to researchers who published their findings as the cover story in the March 11 issue of the Journal of Neuroscience.
Scientists at the University of Rochester Medical Center found that human astrocytes, cells that were long thought simply to support flashier brain cells known as neurons that send electrical signals, are bigger, faster, and much more complex than those in mice and rats.
"There aren’t many differences known between the rodent brain and the human brain, but we are finding striking differences in the astrocytes. Our astrocytes signal faster, and they’re bigger and more complex. This has big implications for how our brains process information," said first author Nancy Ann Oberheim, Ph.D., a medical student who recently completed her doctoral thesis on astrocytes.
Summit Promotes Engineering
Saturday, December 13, 2008
A summit at the U of R was aimed at encouraging interest among high school students and connecting college graduates to some cutting edge local jobs.
Ania Majewska, Ph.D. named a Kavli Fellow
Saturday, November 1, 2008
Congratulations to Ania Majewska, Ph.D. on being named a Kavli Fellow by the National Academy of Sciences (NAS). Each year the NAS conducts the Kavli Frontiers of Science Symposium with some 100 of the best and brightest of young American scientists attending to hear, discuss, and debate talks across a wide range of the natural sciences. Thus, many of the country's ablest scientists--those now rising to positions of leadership in their institutions and their professions--have gone through a seminar
on the value and potential of interdisciplinary research. Attendees are selected from a pool of young researchers who have made significant contributions to science.
Rochester Neuroscientist Honored By Danish Academy
Tuesday, September 23, 2008
Maiken Nedergaard, M.D., D.M.Sc., has been elected a member of the Royal Danish Academy of Sciences, the premier scientific society in Denmark. The society elects only six new members worldwide every other year.
Nedergaard has been a pioneer in brain research, demonstrating that brain cells known as astrocytes play a role in a host of human diseases. For decades, much of the attention of neuroscientists had been focused on brain cells known as neurons, which send electrical signals. Astrocytes were long considered cells whose primary function was to support the neurons.
Nedergaard has turned that notion on its head, showing that astrocytes themselves play an important role in epilepsy, spinal cord disease, migraine headaches, stroke, and Alzheimer's disease.
Summer students Excel in research
Friday, August 1, 2008
The GEBS summer scholars program is designed for Undergraduate students interested in the Ph.D. degree in the Biological or Biomedical Sciences and students with a potential interest in attending graduate school at the University of Rochester. Students choose from a list of mentors and fill out an application.
Chris Holt, Ph.D. Joins the University of Rochester
Sunday, June 1, 2008
The Departments of Neurobiology & Anatomy and Otolaryngology are pleased to welcome Dr. Chris Holt as a co-appointee effective June 1, 2008. Chris’ research interests are in the vestibular efferent system and the synaptic pharmacology and physiology by which efferents modulate vestibular input responses to head motion and orientation.
Having received his BS in Biology from Pembroke State University in 1991, Chris began work on his MS at Northeast Louisiana University but left in 1994 to pursue his PhD in Pharmacology and Toxicology at Tulane University School of Medicine. After completing his degree in 1999, Chris moved on to a postdoctoral fellowship and Research Associate position in the Department of Neurobiology, Pharmacology, and Physiology at the University of Chicago with Jay M. Goldberg, PhD. In 2005, he joined the faculty of the Department of Otolaryngology at the University of Texas Medical Branch as an Assistant Professor and established a close collaboration Shawn Newlands, MD, PhD.
Medical School Class of 2001 selects faculty members for special commendation
Thursday, May 15, 2008
The Medical School Class of 2001 has selected two NBA faculty members for special commendation for first year teaching during the 2007 - 2008 academic year.
Senior Design Team finishes 3rd
Tuesday, May 13, 2008
We are delighted to extend our congratulations to the 2008 Senior Design Team, AccessAPill, for their Third Place Finish in the RERC-AMI 2007 - 2008 Senior Design Competition Accessible Pill Cap Dispensing/Cutting Device competition. The participants, John DiRaddo, Peter van Hoff, Bobby Melenovici, Boston Nyer, and Julian Oshlag are all class of '08 graduates in BME and advised by Dr. Kevin Davis of NBA and BME. The team was awarded a $500 cash prize.
Nature Photographic Exhibit by Babak & Anne Razavi
Friday, May 9, 2008
Babak Razavi is a trainee in the Medical Scientist Training Program pursuing an M.D. as well as a Ph.D. in Biomedical Engineering. His passion with photography began at a young age when his father taught him how to take pictures using a Canon AE-1 back in Iran. Anne Razavi worked as a medical physicist at the Wilmot Cancer Center and Department of Radiation Oncology. She trained at the Charité Hospital, Humboldt University of Berlin, Germany. She is now a product marketing manager with Siemens Medical Solutions. Babak and Anne both enjoy capturing a variety of themes including abstracts, nature, candids, weddings, and each other.
BME Undergraduate wins National Science Foundation Graduate Fellowship
Monday, April 28, 2008
Graduating senior Rachel Hawe (B.S., Biomedical Engineering, 2008) has been selected to receive an NSF Graduate Research Fellowship to pursue her Ph.D. at Northwestern University. Rachel, who is from Alexandria, Virginia, pursued neuroengineering research with Martha Gdowski in the Neurobiology & Anatomy Department during all four of her years at the University of Rochester. She also had a summer research experience at Marquette University, and plans to pursue research in Neuroengineering and Rehabilitation at Northwestern University. When she wasn't in the research laboratory, Rachel was also very active in the Society of Women Engineers, serving as president during her junior year, and providing leadership and outreach all four years. The BME Department also awarded Rachel the BME Faculty Prize at our Annual Student / Faculty Dinner to recognize her outstanding contributions to the Biomedical Engineering Department.
Stopping a Receptor Called 'Nogo' Boosts the Synapses
Tuesday, March 18, 2008
Changing dendritic spines on a neuron - evidence of brain rewiring
New findings about a protein called the nogo receptor are offering fresh ways to think about keeping the brain sharp. Scientists have found that reducing the nogo receptor in the brain results in stronger brain signaling in mice, effectively boosting signal strength between the synapses, the connections between nerve cells in the brain. The ability to enhance such connections is central to the brain's ability to rewire, a process that happens constantly as we learn and remember. The findings are in the March 12 issue of the Journal of Neuroscience.
The work ties together several research threads that touch upon the health benefits of exercise. While those benefits are broadly recognized, how the gains accrue at a molecular level has been largely unknown. The new research gives scientists a way to produce changes in the brain that mirror those brought about by exercise, by reducing the effect of the nogo receptor.
The find comes as a surprise, because for much of the last decade, the nogo receptor has been a prime target of researchers trying to coax nerves in the spinal cord to grow again. They named the protein after its ability to stop neurons from growing. Its action in the brain has not been a hot topic of study.
Shawn D. Newlands, MD, PhD, MBA, FACS Joins the University of Rochester
Saturday, March 1, 2008
Dr. Shawn Newlands has been appointed Professor & Chair of Otolaryngology and Professor of Neurobiology and Anatomy effective March, 2008. Shawn is an expert in head and neck oncologic surgery and an accomplished neuroscientist. His appointment will serve as a basic science anchor as a neuroscientist within our Community and contributes to the mutual benefit of both departments and the growth of translational research interests at Rochester. His is currently studying normal and pathologic vestibular function in primates and humans.
Shawn comes to Rochester from the University of Texas Medical Branch, Galveston, where he served as Harry Carothers Wiess Professor and Chairman of the Department of Otolaryngology since 2003. Prior to joining the University of Texas in 1999, he served for three years on the faculty of the Division of Otolaryngology at the University of Mississippi Medical Center.
Shawn was among the first graduates of the combined MD, PhD program at the University of Texas Medical Branch, earning a PhD in neuroscience along with his medical degree. He completed an internship in general surgery at Virginia-Mason Medical Center in Seattle, followed by a residency in otolaryngology at the University of Washington in Seattle. Shawn holds bachelor’s and master’s degrees from the University of California in Santa Barbara, as well as a master’s in business administration from the University of Texas in Austin.
Sleep Chemical Central to Effectiveness of Deep Brain Stimulation
Monday, December 24, 2007
A brain chemical that makes us sleepy also appears to play a central role in the success of deep brain stimulation to ease symptoms in patients with Parkinson's disease and other brain disorders. The surprising finding is outlined in a paper published online Dec. 23 in Nature Medicine.
The work shows that adenosine, a brain chemical most widely known as the cause of drowsiness, is central to the effect of deep brain stimulation, or DBS. The technique is used to treat people affected by Parkinson's disease and who have severe tremor, and it's also being tested in people who have severe depression or obsessive-compulsive disorder.
Patients typically are equipped with a "brain pacemaker," a small implanted device that delivers carefully choreographed electrical signals to a very precise point in the patient's brain. The procedure disrupts abnormal nerve signals and alleviates symptoms, but doctors have long debated exactly how the procedure works.
"Certainly the electrical effect of the stimulation on neurons is central to the effect of deep brain stimulation," said Maiken Nedergaard, M.D., Ph.D., the neuroscientist and professor in the Department of Neurosurgery who led the research team. "But we also found a very important role for adenosine, which is surprising."
U.S. Navy Awards Grant to Study Neural Effects of Underwater Sound to John Olschowka, Ph.D. and Diane Dalecki, Ph.D.
Wednesday, September 19, 2007
John Olschowka (PI, Dept. of Neurobiology & Anatomy) and Diane Dalecki (co-I) received a two-year grant from the U.S. Navy titled Neural Effects of Underwater Sound.
Underwater sound fields are used for numerous commercial and military applications, including imaging, oil exploration, mapping the ocean, and harbor surveillance. Sponsored by the U.S. Navy, Drs. Olschowka and Dalecki have embarked on a new collaborative project that will investigate the interactions of continuous and impulsive underwater sound fields with the brain and spinal cord. The Olschowka lab, in the UR Department of Neurobiology and Anatomy, has long-standing expertise in examining injury to neural tissues, including trauma, using molecular, protein, and immunohistochemical techniques. Using the acoustic sources and technical expertise of the Dalecki lab, the team will investigate neural bioeffects of sound fields at frequencies ranging from 500 Hz-30 kHz. To also study the effects of acoustic impulses, the facilities and expertise available at Hydroacoustic, Inc. will be employed to generate underwater impulsive sound fields using an air gun system. Neural tissues of animals exposed to these continuous and impulsive underwater sound fields will be assessed for vascular damage, axonal injury, and glial activation. Results of this project will help to establish safe exposure guidelines for human divers and marine life exposed to underwater sound fields.
Spouses Awarded Prestigious Sloan, Pew Fellowships
Friday, August 3, 2007
This summer the University of Rochester Medical Center boasts winners of two of the most prestigious awards available to young scientists - and the winners are from the same family.
Edward Brown, Ph.D., has been named a Pew Scholar in the Biomedical Sciences, and his spouse Ania Majewska, Ph.D., has received an award from the Alfred P. Sloan Foundation. Brown, one of just 20 scientists in the nation to be recognized by the Pew Charitable Trusts this year, will receive $240,000 toward his research, while Majewska will receive $45,000 to continue her work.
Brain Inflammation May Be Friend, Not Foe, For Alzheimer’s Patients
Monday, June 4, 2007
In the June 1st issue of the Journal of Clinical Investigation, a team of scientists from the University of Rochester Medical Center shows that a key inflammatory regulator, a known villain when it comes to parsing out damage after a stroke and other brain injuries, seems to do the opposite in Alzheimer's disease, protecting the brain and helping get rid of clumps of material known as plaques that are a hallmark of the disease.
Cajal Club Explorer Award
Wednesday, October 11, 2006
A couple of weeks ago, Gary Paige, M.D., Ph.D., Chair of the Department of Neurobiology & Anatomy, was informed that Ania Majewska, Ph.D., an Assistant Professor who had recently joined the department, had won the Cajal Club Explorer Award. Receiving such a prestigious award is a cause for recognition and celebration. What make's this all the more special, however, is Ania's personal and professional story.
Speedsters’ Traffic Fines Fund New Research on Spinal Cord Injury
Friday, August 25, 2006
More than a dozen Rochester scientists seeking ways to reverse or lessen the effects of paralysis and other effects of spinal cord injury will begin new projects and continue promising research, thanks to motorists in New York State who push the gas medal a little too far.
Three research projects at the University of Rochester Medical Center are among the programs funded this year through the Spinal Cord Injury Research Program run by the New York State Department of Health. The program, created in 1998, uses fines paid by speeding motorists to fund research into spinal cord injury, whose number-one cause nationwide is motor vehicle accidents. In Rochester this year the grants are going to Roman Giger, Ph.D.; Maiken Nedergaard, M.D., Ph.D.; and Mark Noble, Ph.D.
Rochester Awarded New MS Research Center
Monday, June 12, 2006
A new research center whose scientists are working on better ways to treat multiple sclerosis has been established in Rochester by the National Multiple Sclerosis Society.
The University of Rochester Medical Center is bringing together experts who normally focus on Alzheimer’s disease, HIV vaccines, and spinal cord repair, as well as multiple sclerosis, in a unique center designed to stimulate MS research by drawing on the expertise of scientists from a wide array of disciplines. The new Collaborative Multiple Sclerosis Research Center Award – the only one in the nation established by the society this year – is headed by neurologist Benjamin Segal, M.D., associate professor of Neurology and director of Neuroimmunology Research. Segal has enlisted several of his colleagues to direct their attention on new ways to investigate the disease.
Also taking part in the project are neurologists Steven Schwid, M.D., and Andrew Goodman, M.D., who have extensive experience with clinical trials in MS; and Howard Federoff, M.D., Ph.D., and Tim Mosmann, Ph.D., who head research centers in aging and in vaccine biology, respectively.
Rochester Neuroscientist Awarded NSF Career Grant
Friday, June 2, 2006
David Pinto, Ph.D., assistant professor of Neurobiology and Anatomy and Biomedical Engineering, will receive $590,000 for his research during the next five years, as part of NSF's program to support promising scientists early in their careers.
Flick of Whiskers Helps Tease Out Brain’s ‘Shadow’ Signaling System
Monday, May 15, 2006
By blowing gentle puffs of air onto a mouse's whiskers and watching how its brain reacts, scientists are discovering that a long-overlooked signaling system in the brain is crucial to our everyday activity.
The work is the latest in a growing body of evidence that star-shaped brain cells known as astrocytes aren't simply support cells but are stars of the brain in their own right, say researchers at the University of Rochester Medical Center who did the study. The work will be reported in a paper in the June issue of Nature Neuroscience and is now available online.
"Now people have to take astrocytes seriously," said Maiken Nedergaard, M.D., Ph.D., professor in the Department of Neurosurgery and a member of the Center for Aging and Developmental Biology, whose team did the research. In the past few years she has found that the cells, long thought to simply nourish other cells and clean up their wastes, are central to diseases like epilepsy, spinal cord injury, and maybe even Alzheimer's disease.
$3.5 Million Grant To Support Research on New Treatment for Severe OCD
Thursday, February 23, 2006
As part of a five-year, $3.5 million grant from the National Institutes of Health (NIH), researchers will look at whether a breakthrough therapy for Parkinson's disease can also treat the worst cases of obsessive compulsive disorder (OCD). A research team led out of the University of Rochester Medical Center will measure whether Deep Brain Stimulation (DBS) can reduce the rampant anxiety that keeps some OCD patients homebound.
DBS is one of the most promising areas of OCD research because early studies show that it may help many within the approximately 20 percent of OCD patients for whom neither psychological nor drug therapy works,
said Suzanne Haber, Ph.D., a professor within the Department of Pharmacology and Physiology at the University of Rochester School of Medicine and Dentistry. Some patients have been able to venture out to work and school for the first time with DBS,
said Haber, who is lead investigator for the grant.
Blood Flow in Brain Takes a Twist, Affecting Views of Alzheimer’s
Friday, January 6, 2006
New findings that long-overlooked brain cells play an important role in regulating blood flow in the brain call into question one of the basic assumptions underlying today's most sophisticated brain imaging techniques and could open a new frontier when it comes to understanding Alzheimer's disease.
In a paper to appear in the February issue of Nature Neuroscience and now available on-line, scientists at the University of Rochester Medical Center demonstrate that star-shaped brain cells known as astrocytes play a direct role in controlling blood flow in the brain, a crucial process that allows parts of the brain to burst into activity when needed. The finding is intriguing for a disease like Alzheimer's, which has long been considered a disease of brain cells known as neurons, and certainly not astrocytes.
"For many years, astrocytes have been considered mainly as housekeeping cells that help nourish and maintain a healthy environment for neurons. But it's turning out that astrocytes may play a central role in many human diseases," said neuroscientist Maiken Nedergaard, M.D., Ph.D., who has produced a string of publications fingering astrocytes in diseases like epilepsy and spinal cord injury.
Roots of Epilepsy May Lie in Oft-Ignored Brain Cells
Monday, August 15, 2005
Star-shaped brain cells that are often overlooked by doctors and scientists as mere support cells appear to play a key role in the development of epilepsy, researchers say in a study published on-line August 14 in Nature Medicine. It's one of the first times scientists have produced firm evidence implicating the cells, known as astrocytes, in a common human disease.
Scientists found that astrocytes can serve as ground zero in the brain, setting off a harmful cascade of electrical activity in the brain by sending out a brain chemical that triggers other brain cells to fire out of control.
While it's impossible to tell at this early stage what effect the finding will have on treatment, the investigators at the University of Rochester Medical Center are hopeful the results will give doctors and pharmaceutical firms a new target in efforts to treat and prevent the disease.
"This opens up a new vista in efforts to treat epilepsy. It might be possible to treat epilepsy not by depressing or slowing brain function, as many of the current medications do, but by targeting brain cells that have been completely overlooked," says Maiken Nedergaard, M.D., Ph.D., professor in the Department of Neurosurgery and a researcher in the Center for Aging and Developmental Biology, who led the research. "We are hopeful that someday, this will be very beneficial to patients."
Scientists Finger Surprise Culprit in Spinal Cord Injury
Wednesday, July 28, 2004
ATP, the vital energy source that keeps our body's cells alive, runs amok at the site of a spinal cord injury, pouring into the area around the wound and killing the cells that normally allow us to move, scientists report in the cover story of the August issue of Nature Medicine.
The finding that ATP is a culprit in causing the devastating damage of spinal cord injury is unexpected. Doctors have known that initial trauma to the spinal cord is exacerbated by a cascade of molecular events over the first few hours that permanently worsen the paralysis for patients. But the finding that high levels of ATP kill healthy cells in nearby regions of the spinal cord that were otherwise uninjured is surprising and marks one of the first times that high levels of ATP have been identified as a cause of injury in the body.
While the work opens up a promising new avenue of study, the work is years away from possible application in patients, cautions Maiken Nedergaard, M.D., Ph.D., the researcher who led the study. In addition, the research offers promise mainly to people who have just suffered a spinal cord injury, not for patients whose injury is more than a day old. Just as clot-busting agents can help patients who have had a stroke or heart attack who get to an emergency room within a few hours, so a compound that could stem the damage from ATP might help patients who have had a spinal cord injury and are treated immediately.