Summer 2017 Newsletter
Fellow Research Spotlight
 Jenniffer Herrera, M.D., 3rd Year Developmental-Behavioral Pediatrics Fellow
Jenniffer Herrera, M.D., 3rd Year Developmental-Behavioral Pediatrics Fellow
“Advocacy for Autism Spectrum Disorder in Hispanic Children”
By Rachel Bills
In the United States, one in 68 children is diagnosed with an autism spectrum disorder (ASD) with the majority of diagnoses occurring after the age of four years (MMWR Surveillance Summaries). Jenniffer Herrera, MD, third year Developmental and Behavioral Pediatrics (DBP) fellow, has spent much of her medical career interested in health disparities and serving as an advocate for individuals with intellectual and developmental disabilities, with a particular focus on the Hispanic population. Her passion has motivated her to study systems of care to improve early diagnosis of ASD and entry into intervention for Hispanic children. Working with her mentor, Susan Hyman, M.D., Professor and Division Chief of DBP, Dr. Herrera devised a study that is the first of its kind in the northeast region of the United States.
Dr. Herrera’s research explores the influence of Hispanic ethnicity on diagnosis and intervention for children with ASD, particularly looking at age of diagnosis, symptom severity and utilization of early intervention (EI) services. Studying children ages 24-60 months with ASD in the Rochester region, she compared these factors between Hispanic and non-Hispanic white (NHW) child populations. Dr. Herrera initially hypothesized that Hispanic children in our community would be referred for an ASD initial diagnostic evaluation at a later age and also have a later age of entry into early intervention than NHW children, as is documented in the literature. However, her findings revealed a unique phenomenon in the Rochester region. She found the opposite to be true – though Hispanic children are receiving initial diagnostic evaluations after 36 months, there are no differences in the mean ages at referral, evaluation, or diagnosis between groups. Notably, Hispanic children appear to be receiving ASD diagnosis before age four, and earlier than their non-Hispanic white counterparts. She attributes this variation from the literature to a unique community environment in Rochester. DBP physicians at Golisano Children’s Hospital have close working relationships with the primary care providers, and these primary care providers are providing developmental screening in primary care and are able to navigate the public health system well. They are referring children to DBP services for earlier evaluations and to early intervention services, which is in contrast to many other regions across the U.S.
Recently awarded the departmental Clausen Fellowship Award to support her research, Dr. Herrera plans to continue her review and analysis in order to interpret symptom severity for children being evaluated for ASD. With the Hispanic population being the fastest growing minority, she hopes to achieve a greater understanding of health disparities within this population. Fellowship has given her the opportunity to do just that. She is also a part of Special Hope Foundation Grant directed by Stephen Sulkes, M.D., which is aimed at improving Spanish language interpreter education in order to better and more effectively serve those with intellectual and developmental disabilities in the medical environment. After fellowship, she plans to continue contributing to cultural diversity and inclusion advocacy at the local and national levels.
Congratulations To Our 2017 Fellowship Graduates!
On Friday, June 16th, fellows, faculty and family members gathered together to celebrate the accomplishments of our graduating fellows. Our annual fellowship graduation dinner was held at Ballroom 384, located in Rochester’s historic East Avenue district. Visit our Facebook page to view more photos from graduation. We wish each of our graduates the best of luck in their careers!

From left: Dr. Patty Chess, Vice Chair of Education and Neonatology Program Director; Dr. Javed Mannan, Neonatology; Dr. James Thomas, Neonatology; Dr. Marybeth Jones, Academic General Pediatrics; Dr. Elizabeth Nocera, Critical Care; Dr. Shanley Sifain, Neonatology; Dr. Nina Schor, Department Chair.
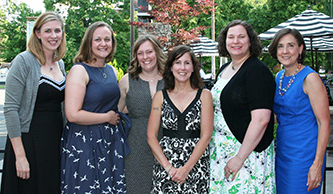
Pediatric Critical Care
Pediatric Critical Care faculty and fellows celebrate! Photo left to right: Drs. Erin Barker, Heather Reyes (3rd year fellow), Elizabeth Nocera (graduate), Jill Cholette, Melissa Cullimore (2nd year fellow), and Andrea Hinkle (Program Director).
- Elizabeth Nocera, D.O.
Pediatric Intensivist
St. Vincent Health
Peyton Manning Children’s Hospital
Indianapolis, IN

Pediatric Gastroenterology/Nutrition
Photo: Pediatric GI/Nutrition graduate, Dr. Walaa Elfar, with Program and Associate Program Directors, Drs. Thomas Rossi and Becky Abell.
- Walaa Elfar, M.B.Ch.B.
To be confirmed.
General Pediatrics
- Marybeth Jones, M.D.
Assistant Professor of Pediatrics, Division of General Pediatrics
Assistant Professor of Medicine
University of Rochester Medical Center
Rochester, NY
Neonatology
- Javed Mannan, M.D., M.P.H.
Assistant Professor of Pediatrics
Division of Neonatology
UMASS Memorial Medical Center
Worcester, MA
- Shanley Sifain, M.D.
Senior Instructor of Pediatrics
Division of Neonatology
University of Rochester Medical Center
Rochester, NY
- James Thomas, M.D., M.P.H.
Assistant Professor (Clinical) of Pediatrics
Division of Neonatology
University of Utah, Primary Children’s Hospital
Salt Lake City, UT
Welcome To Our Newest Fellows!

The Department of Pediatrics welcomed ten new fellows in the divisions of adolescent medicine, cardiology, critical care, gastroenterology/nutrition, general pediatrics, hematology/oncology, and neonatology. We look forward to a great three years!
2017-2019 Dean's Fellows
Each year, the Department of Pediatrics awards first year fellows the Dean’s Fellowship in recognition of their research pursuits. Congratulations to the most recent Dean’s Fellows!
 Carol Fries Simpson, M.D.
Carol Fries Simpson, M.D.
Hematology/Oncology
Topic: "Investigating intraclonal diversity in pediatric ALL"
Mentor: Richard Burack, M.D., Ph.D.
 Blair Germain, M.D.
Blair Germain, M.D.
Neonatology
Topic: "Effect of Lasix on metabolic bone disease of prematurity"
Mentor: Jeffrey Meyers, M.D.
Alumni Breaking New Ground
By Meghan Plog

Founding members of the URMC Project ECHO®
Eating Disorders team.
This past year, the University of Rochester Medical Center launched the world’s first Project ECHO tele-education hub focusing on eating disorders. Project ECHO (Extension for Community Healthcare Outcomes) is an initiative that allows specialists to interact with and support community-based health care providers via teleconferencing in an effort to expand access to evidence-based treatment to areas that may lack specialty-trained providers. Project ECHO has existed at the University since 2014, beginning with geriatric mental health, and has since grown to include eight more specialties. Due to the complex nature of eating disorders and the multidisciplinary care required, this was a great opportunity to expand its services.
Taylor Starr, D.O., M.P.H., Assistant Professor of Pediatrics and Adolescent Medicine Fellowship alumna is a member of the ECHO Eating Disorders expert team. This multidisciplinary team, overseen by Mary Tantillo, Ph.D., PMHCNS-BC, FAED, CGP, Professor of Clinical Nursing and Richard Kreipe, M.D., Professor of Pediatrics and fellowship alumnus, teleconferences with health care providers across the state twice a month. Included in the community of learners are primary care physicians, nurses, social workers, and college and university based health providers, to name a few. Each session is comprised of a patient case review and discussion, as well as a didactic presentation. Dr. Starr believes one of the most powerful aspects of this program is the collaborative learning environment it fosters with the opportunity to problem solve and learn together. Rather than reaching just one patient at a time, this model allows for knowledge to be shared with multiple community learners who, in turn, can share that information with their own practices and communities. “It exponentially improves care, knowledge and collaboration,” she said.


Richard Kreipe, M.D. and Taylor Starr, D.O., M.P.H. are both graduates from the Adolescent Medicine Fellowship Program at URMC.
This initiative also provides a profound experience for trainees. Dr. Starr includes adolescent medicine fellows and pediatric residents in ECHO sessions and welcomes their participation. Participation offers trainees the opportunity to work with a multidisciplinary group, to build expertise in taking care of patients with eating disorders, to serve in a consultant role, and to grow their own professional networks and collaborations with health care providers across the state. Furthermore, Starr says it can provide an empowering and transformative experience for fellows, as they quickly shift from an observer to an expert participant.
The University's program has gained national attention with URMC recently cited in a state Department of Health White Paper as a benchmark organization in telemedicine because of Project ECHO. Project ECHO® Eating Disorders is sponsored by the Western New York Comprehensive Care Center for Eating Disorders (WNYCCCED) for which Drs. Kreipe and Starr serve as the medical directors. The WNYCCCED, a partnership between the University of Rochester School of Nursing and Golisano Children's Hospital, is directed out of the University of Rochester School of Nursing and serves as the hub for eating disorder services in the 30-county Western NY region. The WNYCCCED receives funding for these services, including Project ECHO, through the NY State Department of Health.
Did You Know?
This September 2017, Phase II of the Golisano Children's Hospital will open. This new phase encompasses two new floors, which includes pediatric operating rooms, a pediatric cardiac surgery center, a gastroenterology procedure suite, and a new pediatric intensive care unit (PICU).
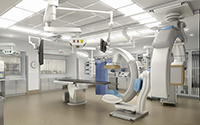
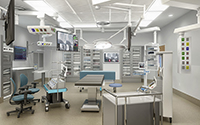

Learn more about Phase II - Golisano Children's Hospital!
Pediatric faculty, Drs. Walter Pegoli, Jeffrey Rubenstein and Jill Cholette give an inside look at the two new floors of Golisano Children's Hospital.

Supporting Fellow Research
CURE Childhood Cancer Association, longtime supporters of Golisano Children’s Hospital, generously donated $3,000 to be used towards research projects being led by our Pediatric Hematology/Oncology fellows. A big thank you to CURE for their support and contribution!
Pictured from left: Meghan Plog, M.S., Pediatric Hematology/Oncology Fellowship Coordinator; Craig A. Mullen, M.D., Ph.D., Pediatric Hematology/Oncology Division Chief and Fellowship Program Director; Holly Dutcher, Executive Director of CURE; and Kiersten Kunick, CURE Parent Advocate
Pediatric Fellows’ Event
Fellows, save the date for the next pediatric fellows’ event!
What: A fun night of bowling with your fellow fellows
When: Friday, October 20th from 6:00 - 8:00 p.m.
Where: Radio Social (20 Carlson Road, Rochester)
Seasonal Fun
Food Truck Rodeo
Check out the Food Truck Rodeo at Rochester’s Public Market. This event occurs on the last Wednesday of the month from April-September. Enjoy tastings from creative community food trucks while listening to the musical talents of local artists and bands. Also be sure to check out the Public Market throughout the year for local produce, meats, seafood, dairy products, prepared foods, and so much more. The market is open year-round on Tuesdays and Thursdays from 6:00 a.m. - 1:00 p.m. and on Saturdays from 5:00 a.m. - 3:00 p.m.
Sailing on the Finger Lakes
Check out Schooner Excursions, Inc. for sailing trips on Seneca Lake. With many wineries and spots for hiking, biking, boating and fishing, the Finger Lakes are a must-see in the summer and fall!
Rochester Red Wings
Enjoy an afternoon or evening of baseball cheering on Rochester’s Triple-A team, the Red Wings!
Current and Graduated Fellows – Please send us your news!