April 23, 2004
Immune and Inflammatory Responses in the Central Nervous System
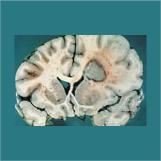 Welcome
Welcome
The contribution of inflammation-related processes to neurological diseases has been increasingly recognized in recent years. Studies of primary neuroimmunological diseases such as Multiple Sclerosis as well as neurodegenerative disorders with an inflammatory component, including Alzheimer's Disease and Parkinson's Disease, have received particular attention in basic research and clinical arenas. Inflammatory aspects of CNS trauma, toxin exposure and psychological disorders are also currently under investigation. Furthermore, the immunological/inflammatory consequence of gene therapy in the CNS is a timely and important issue.
This Symposium addressed the roles of innate and adaptive immunity in response to CNS insults and various disease processes. Specific topics included the immune functions of glial cells, factors controlling blood brain barrier integrity, leukocyte trafficking to the CNS, CNS cytokine/chemokine production, animal models of neuroinflammatory/ neuroimmunological diseases and clinical application of basic research findings.
Speakers
 Intravascular Alzheimer's amyloid-B Linked to AB Deposition in the Brain
Intravascular Alzheimer's amyloid-B Linked to AB Deposition in the Brain
Berislav Zlokovic, M.D., Ph.D., University of Southern California formerly University of Rochester
Dr. Berislav Zlokovic is Director, Zilkha Neurogenetic Institute; Professor and Chair, Department of Physiology & Biophysics; Director, Center for Neurodegeneration & Regeneration Zilkha Neurogenetic Institute Keck School of Medicine of USC
Dr. Zlokovic's research links intravascular Alzheimer's amyloid-β (Aβ) to Aβ deposition in brain, transport across the blood-brain barrier (BBB) and neuroinflammation as a primary mechanism in Alzheimer's disease pathogenesis. Faulty clearance due to dysregulated transport of Aβ is shown to potentiate neuroinflammation and cerebral β-amyloidosis associated with reduced cerebral blood flow (CBF), triggering "silent strokes" in models of Alzheimer's disease. From the therapeutic prospective, his investigations show that new peripheral Aβ binding agents protect brain from Aβ/amyloid accumulation, neuroinflammation and suppression of CBF. In addition, his work on activated protein C (APC) in the CNS demonstrates that APC prevents leukocyte trafficking across the BBB and protects brain from injury and/or apoptosis.
 Communication between Immune System and the CNS via Cytokine/Chemokine Networks
Communication between Immune System and the CNS via Cytokine/Chemokine Networks
Etty (Tika) Benveniste, Ph.D., University of Alabama-Birmingham
Dr. Etty Benveniste is Professor and Chairman of the Department of Cell Biology and Anatomy; and Professor in the Departments of Neurobiology and Physiology and Biophysics
Dr. Benveniste’s research is directed toward understanding how the immune system and central nervous system (CNS) communicate with each other via cytokine/chemokine networks. Specifically, her laboratory examines the mechanisms by which cytokines modulate class II major histocompatibility complex (MHC) class II transactivator (CIITA), intercellular adhesion molecule-1 (ICAM-1), and CD40 expression in CNS-resident cells, and the transcription factors involved in their respective gene expression. Other investigations include the ability of glial cells to secrete immunoregulatory molecules (tumor necrosis factor, interleukin-6, interleukin-10, chemokines), the intracellular signaling events involved in the response and the effects of HIV gene products on glial function.
 Initiation of Inflammation in the CNS and Regulation of Blood Brain Barrier Integrity
Initiation of Inflammation in the CNS and Regulation of Blood Brain Barrier Integrity
William F. Hickey, M.D., Dartmouth Medical School
Dr. William Hickey is Chairman of Pathology at Dartmouth Medical School
Dr. Hickey's laboratory effort focuses on the mechanisms for the initiation of inflammation in the central nervous system and regulation of blood brain barrier (BBB) integrity. Specifically, this work includes animal research with experimental autoimmune models, the kinetics and principles of lymphocyte and myeloid cell trafficking to the CNS and molecular changes in the CNS during inflammatory responses.
 Involvement of Chemokines and Their Receptors in Leukocyte Invasion, Differentiation, Activation, Tissue Destruction, and Repair in the CNS
Involvement of Chemokines and Their Receptors in Leukocyte Invasion, Differentiation, Activation, Tissue Destruction, and Repair in the CNS
Richard Ransohoff, M.D., Cleveland Clinic
Dr. Richard Ransohoff is Director of Neuroinflammation Research Center in Lerner Research Institute
The core hypothesis of Dr. Ransohoff’s research is that chemokines and their receptors are significantly involved in leukocyte invasion, differentiation, activation, tissue destruction and repair in the CNS. Furthermore, resident neural cells respond to locally produced chemokines. To address this hypothesis and identify molecular targets for therapy, his laboratory examines chemokine production and function. These studies comprise tissue culture systems, disease models and material from patients with neurological disease. They make extensive use of transgenic and knockout mice to clarify how chemokines exert remarkably specific effects in vivo, in the face of apparent functional redundancy in vitro.
 Models of Multiple Sclerosis, Experimental Allergic Encephalomyelitis, Mediated by CD4+ T Cells Specific for Myelin Peptides
Models of Multiple Sclerosis, Experimental Allergic Encephalomyelitis, Mediated by CD4+ T Cells Specific for Myelin Peptides
Benjamin Segal, M.D., University of Rochester
Dr. Benjamin Segal is Assistant Professor of Neurology and NeuroImmunology
Dr. Segal’s research focuses on a mouse model of multiple sclerosis (MS), experimental allergic encephalomyelitis (EAE), mediated by CD4+ T cells specific for myelin peptides. His studies on cytokine networks demonstrated that production of the pro-inflammatory cytokine, IL-12, promotes development of EAE, whereas production of the immunosuppressive cytokine, IL-10, is protective. Using the EAE model, his laboratory also investigates the role of chemokines in leukocyte trafficking to the CNS, the function of adhesion molecules in lymphocyte migration across the BBB and mechanisms of tolerance to self-antigens. One of the goals of his lab is to devise new strategies for the treatment of autoimmune diseases such as MS.
 Mechanisms of Tolerance and Autoimmunity, Experimental Allergic Encephalomyelitis
Mechanisms of Tolerance and Autoimmunity, Experimental Allergic Encephalomyelitis
Joan M. Goverman, Ph.D., University of Washington
Dr. Joan Goverman is Associate Professor of Immunology
Dr. Goverman's research centers on investigating mechanisms of tolerance and autoimmunity and employs an animal model for autoimmunity, experimental allergic encephalomyelitis (EAE). EAE is triggered by generating T cell-mediated immunity to myelin antigens. Dr. Goverman's work has shown that portions of some myelin proteins induce T cell tolerance, while T cells specific for other regions of these proteins escape tolerance and mediate disease. T cell receptor transgenic models have been developed to investigate how tolerance to myelin antigens is established, maintained and broken. These transgenic models have allowed investigation into triggers of spontaneous central nervous system autoimmune disease and as well as active and passive mechanisms that function to prevent disease. Recently, her laboratory has demonstrated that, in addition to CD4+ T cells, myelin-specific cytotoxic CD8+ T cells can mediate EAE. This work extends the potential of animal models to define the full range of effector cells that may contribute to multiple sclerosis.
Coverage of the Event
 Neuroscience Graduate Student Irah King (right) opened the 2004 Schmitt Symposium by welcoming the speakers and the audience. Irah did a great job all day, as he introduced each speaker and shuttled Symposium participants from discussions to lunch to panels to dinner.
Neuroscience Graduate Student Irah King (right) opened the 2004 Schmitt Symposium by welcoming the speakers and the audience. Irah did a great job all day, as he introduced each speaker and shuttled Symposium participants from discussions to lunch to panels to dinner.


Etty Benveniste and William Hickey presenting
People chatting after a talk (left) and a group getting ready for the symposium talk (right).