Keratoprosthesis (Artificial Corneas)
For many patients traditional cornea transplants work well in eliminating blindness due to cornea disease. This method involves suturing natural cornea tissue from a donor eye to replace the scarred one or replacing a specific layer of the cornea using one of several sutureless procedures. Cornea transplants may fail due to rejection, and may yield poor results in certain cases. When a natural cornea transplant is not a good option more and more surgeons are recommending the keratoprosthesis to restore vision. The concept of utilizing an artificial cornea originates from the 18th century when it was first proposed to substitute a piece of glass to substitute for the scarred cornea.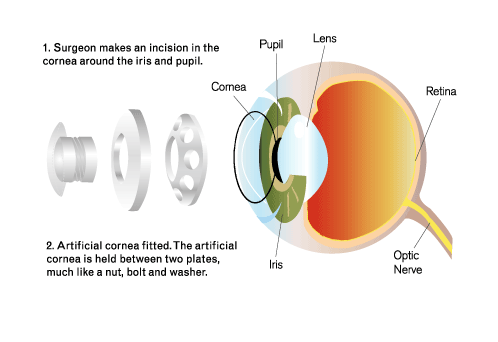
Did You Know?
Dr. Aquavella and the Eye Institute team provide hope to parents of children with blindness, including those with Peter's anomaly. The team has performed the procedure on infants as young as 6 weeks old.
Links to Articles
Artificial Cornea Offers Better Results for Infants, Some Blind Patients
University of Rochester Medical Center News
"How Aaron Gives Hope to Thousands"
Times of London
 Dr. Aquavella is an internationally recognized corneal surgeon who has been at the forefront of cornea research for decades. He recently evaluated a new artificial cornea device for implantation in cases of corneal blindness refractive to traditional keratoplasty and defined the indications for this keratoprosthesis in over 300 cases. He developed the techniques for use of this device in newborn infants and has treated babies from all over the world.
Dr. Aquavella is an internationally recognized corneal surgeon who has been at the forefront of cornea research for decades. He recently evaluated a new artificial cornea device for implantation in cases of corneal blindness refractive to traditional keratoplasty and defined the indications for this keratoprosthesis in over 300 cases. He developed the techniques for use of this device in newborn infants and has treated babies from all over the world.
The Boston Keratoprosthesis is assembled utilizing a central optical cylinder with a surface plate which functions as a new entrance pupil and cornea refracting surface. It is fixed to a ring of donor cornea stroma surrounding the 3 mm optical cylinder and fastened by a fenestrated back plate and locking titanium washer. The device can then be implanted into a recipient eye using standard cornea transplant techniques. A hydrophilic bandage lens, worn over the entire surface, has been effective in eliminating many ocular surface problems common to cornea transplants.
This technique is effective in instances where traditional transplantation has failed or carries a poor prognosis. It also can be utilized as an alternative to a cornea transplant in that the visual rehabilitation occurs within days, the visual acuity obtained is not subject to astigmatism, and there is no potential for allograft rejection to occur.
Since infants and children have a very active immune system most corneal surgeons consider standard cornea transplant is doomed to failure. Amblyopia can best be avoided or treated by establishing a clear visual axis early in life thus our team operates in newborns at 4-6 weeks of age. Many of the conditions which produce congenital cornea opacity also result in abnormalities of the lens, intraocular pressure elevation, as well as vitre-oretinal disease. Dr. Aquavella's infant team is composed of Drs. Matthew Gearinger, Shakeel Sharef, and Mina Chung. They have the largest series of infant keratoprosthesis cases coming from all over the world.
Surgery
The surgical procedure is performed on an ambulatory basis with the patient returning home—or to a hotel if the patient is coming from a distance—the same day. Most surgeries are performed with the use of local anesthesia, with the exception of infants and young children where general anesthesia may be indicated. Patients can expect to be in the operating room area for at least 3 hours for this procedure, including 1 hour and 20 minutes for surgery, as well as pre-operative and recovery time.
Follow-up Care
In all cases, patients return to the Eye Institute the day following surgery for reevaluation, necessary prescriptions, and post-operative care instructions. Additional follow-up exams are usually made after 1 week and every 3 months throughout the first year. For out-of-town patients, follow up visits after the 1 week interval can be made with a qualified ophthalmologist or corneal specialist who will be in frequent contact with Dr. Aquavella.
Risks and Discomforts
For patients with severe dryness or inflammation, keratoprosthesis can give excellent results but is more risky. In some instances a membrane can develop behind the keratoprosthesis and interfere with vision. This membrane can be opened using a tiny laser beam without requiring additional surgery. Rarely, tissue around the stem of the prosthetic device dissolves which can lead to the leakage of fluid from the eye leading to infection or even vision loss. In such instances the surgery may have to be repeated.
US Patient Costs
The cost of keratoprosthesis is covered by most major U.S. medical insurance plans. You should get in touch with them prior to scheduling surgery to check your policy, then contact the University of Rochester Medical Center price estimation service. This service will provide you with a highly accurate estimate of what your out-of-pocket costs are likely to be. They can be reached by phone or e-mail, Monday through Friday from 8 a.m. to 5 p.m. eastern standard time:
(585) 758-7801
URMCPriceEstimation@urmc.rochester.edu
International Patient Costs
For patients who do not have insurance coverage, including foreign patients, the Eye Institute has a package price of $55,000 U.S. for this procedure. This includes pre-operative visits, clinical testing, surgery, hospital fees and post-operative visits. Travel and out-of-pocket living expenses for out-of-town patients are not included in this fee and patients should plan accordingly.
More Information
Download a Keratoprosthesis brochure