Core Clinical Rotations and Experiences
Core Clinical Rotations and Experiences
The fellow's role is oriented towards training for an academic career in Maternal-Fetal Medicine and obtaining board subspecialty certification. The fellow's clinical responsibilities are similar to those of the full-time faculty and include outpatient care, ultrasound consultation, and inpatient management.
There are two MFM specialty clinics, UR Maternal-Fetal Medicine at Red Creek and the UR Maternal-Fetal Medicine at Lattimore, which provide comprehensive prenatal care for pregnancies affected by maternal, fetal, or obstetric concerns.
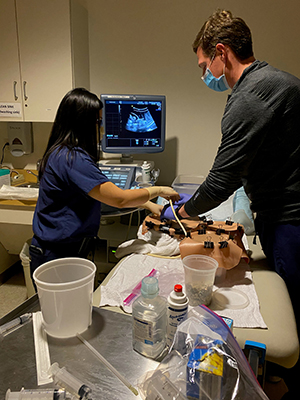
MFM fellows Dr. Mather and Dr. Liew simulating and learning amniocentesis with Dr. Drennan
UR Maternal-Fetal Medicine at Lattimore
The UR Maternal-Fetal Medicine at Lattimore is housed within UR Medicine Gender Wellness, Obstetrics & Gynecology, and provides longitudinal resident experience with high-risk patient populations, and includes support staff from nutrition, psychiatry, and social work.
UR Maternal-Fetal Medicine at Red Creek
UR Maternal-Fetal Medicine at Red Creek is the MFM faculty practice and is staffed by faculty, fellows, nurse practitioners, and a dietician. It offers consultation, co-management, and comprehensive prenatal care to patients from Rochester and the surrounding regions.
Cardiology Co-management
For patients with complex heart disease, there is a quarterly meeting with the MFM, anesthesia, adult cardiology, adult congenital cardiology, and ICU teams to review pregnant patients with cardiac disease. This close collaboration between these services allows our team to effectively care plan for patients with complex heart disease who are considering pregnancy or who are currently pregnant. In collaboration with cardiology, a postpartum preeclampsia follow up clinic was established. ( Highland Hospital - University of Rochester Medical Center)
Ultrasound
Level II OB/GYN ultrasound, including Perinatal sonography and fetal echocardiography, is available on-site at multiple locations (both our Red Creek and Lattimore offices, as well as Highland Hospital) and provides an excellent source of patients for clinical experience and research endeavors.
We perform over 25,000 scans annually in our AIUM ob, gyn, and fetal echo accredited unit. We have a staff of dedicated MFM sonographers, most of whom are also fetal echocardiography certified. This provides both depth and breadth in this important area of perinatology.
Fellows become proficient in both obstetric and gynecologic ultrasound, as well as advanced fetal imaging techniques and fetal echocardiography. Fetal procedures are performed at these locations including fetal transfusion (PUBS), shunts, amniocentesis, and CVS. Both ultrasound locations also have reproductive genetic counseling on-site.
Genetics
The ACGME and ABOG have added a requirement for genetics experiences (2 months) into the fellowship. At URMC we are fortunate to have two MFM/Genetics boarded faculty, as well as multiple genetic counselors, cytogeneticists, and medical geneticists to help provide this experience.
The genetics education and experience in the fellowship is arranged in a combination of continuity and rotation experiences. There is on-line and self-study based "prelearning" for these rotations as well, and fellows are given time to complete this work. Fellows are encouraged to take at least one genetic course, and complete a genetic disorders "log" on their depth and breadth of exposures.
The genetics clinical experience consists of:
- Time with genetic counselors when on ultrasound rotations, attending selected sessions, especially for more rarely seen disorders
- Performing genetic counseling with the genetics counselors and MFM faculty on new diagnoses found during ultrasound
- Dedicated rotation time with genetic counselors
- Medical Genetics rotation with the medical genetics division
- Cytogenetics and Microarray experience with cytogenetics division
- Neonatal Genetics consult service with Dr. Ho (MFM faculty)
- Post-loss/Genetics clinic
Electives
The MFM fellowship at URMC offers a wide variety of clinical experiences to allow fellows to tailor their fellowship to their eventual career goals. Further options and rotations can be structured as individual fellows needs arise within the elective time, however, some of the common electives include:
- NICU genetics and dysmorphology (with our MFM geneticist)
- Adult reproductive genetics (with genetics faculty)
- Adult congenital heart disease (with adult congenital team)
- Fetal echocardiography (with pediatric cardiology)
- Breastfeeding medicine (with fellowship trained specialist)
- Family planning/complex contraception (with family planning specialists)
- Additional ultrasound experiences (beyond the core rotations)
- Additional research months (beyond the core 12-month rotation)