Forensic Pathology in the News
The national shortage of forensic pathologists in municipal medical examiners' offices was addressed in the local news last week.
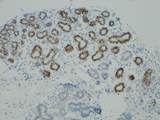
Are We on the Heels of a Gene Signature for High-Grade Breast Cancer?
A pathology researcher at the University of Rochester Medical Center believes she’s discovered an important phenomenon in normal-looking breast tissue that could foreshadow an aggressive tumor known as triple-negative breast cancer.