Pacemaker Insertion- Transvenous
What is a pacemaker?
A pacemaker is a small electronic device that helps maintain or restore a normal heart
rate and rhythm. The pacemaker is usually implanted in the chest, just below the collarbone.
Your healthcare provider may recommend this device to keep your heartbeat from slowing
down to a dangerously low rate.
The heart is a pump made up of muscle. The muscle is stimulated by electrical signals.
These signals normally follow a specific circuit within the heart. These signals organize
contractions of the different parts of the heart. This makes it beat at a rate that
keeps blood flowing around the body the way it should. A pacemaker may be needed when
there are problems with the electrical signals in the heart. Your heart may sometimes
beat too slowly, or at an irregular rate.
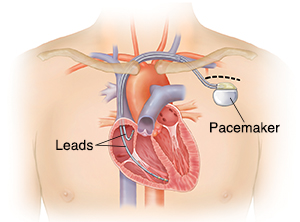
A pacemaker is made of three parts. They include a pulse generator, one or more leads,
and an electrode on each lead. A pacemaker signals the heart to beat when the natural
heartbeat is too slow or irregular.
Why might I need a pacemaker?
Your healthcare provider may advise a pacemaker when your heart beats too slowly and
this can't be fixed with other treatments. A pacemaker will help you maintain a normal
heart rate.
Problems with the heart rhythm may mean your heart is not pumping enough blood to
the body. If your heart rate is too slow, the blood is pumped too slowly. If the heart
rate is too fast or too irregular, the heart chambers are unable to fill up with enough
blood to pump out with each beat. Medicines are often used to slow down these fast
heart rhythms. But the medicines can also result in slow heart rates when the rhythm
is normal. When the body does not get enough blood, symptoms such as tiredness, dizziness,
fainting, or chest pain may occur.
Some examples of problems for which a pacemaker might be needed include:
-
Bradycardia. This is when the heart beats too slowly.
-
Tachy-brady syndrome. Also known as sick sinus syndrome and sinus node dysfunction. This is characterized
by alternating fast and slow heartbeats.
-
Heart block. This occurs when the electrical signal is delayed or blocked as it travels through
the heart muscle. There are several types of heart blocks.
Your healthcare provider may have other reasons to advise pacemaker insertion.
What are the risks of pacemaker insertion?
Risks of pacemaker insertion include:
-
Reaction to the anesthetic or sedatives used during the procedure
-
Swelling or bruising in the upper chest area where the pacemaker device is placed
-
Bleeding from the cut (incision) or sheath insertion site
-
Damage to the vessel where the sheath is put into the body
-
Infection of the incision or catheter site
-
Collapsed lung
-
Blood clots
-
Bleeding that can occur from the heart with blood accumulating in the sac (pericardium)
surrounding the heart (pericardial effusion)
-
Lead displacement. This means the wires of leads of the pacemaker become disconnected
or displaced. You may need another procedure to reposition them.
-
Mechanical problems with the pacemaker device
For some people, having to lie still on the procedure table for the length of the
procedure may cause some discomfort or pain.
There may be other risks. This depends on your specific health condition. Be sure
to discuss any concerns with your healthcare provider before the procedure.
How do I get ready for pacemaker insertion?
-
Your healthcare provider will explain the procedure to you and ask if you have any
questions.
-
You will be asked to sign a consent form. This gives your permission to do the procedure.
Read the form carefully. Ask questions if anything is not clear.
-
Tell your healthcare provider if you are sensitive to or are allergic to any medicines,
iodine, latex, tape, or anesthetic agents (local and general).
-
You will need to fast (not eat or drink) for a certain period before the procedure.
Your healthcare provider will tell you how long to fast, usually overnight or at least
8 hours before the procedure.
-
Tell your healthcare provider if you are pregnant or think you might be, or if you
are breastfeeding.
-
Be sure your healthcare provider knows about all medicines, vitamins, herbs, and supplements
that you are taking. This includes both prescription and over-the-counter medicines.
-
Tell your healthcare provider if you have a history of bleeding disorders or if you
are taking any anticoagulant (blood-thinning) medicines. This includes aspirin, or
other medicines that affect blood clotting. You may need to stop taking some of these
medicines before the procedure.
-
Tell your healthcare provider if you have heart valve disease. You may need to take
antibiotics before the procedure.
-
You may need a blood test before to the procedure as well as chest X-ray
-
You may get a sedative before the procedure. This is to help you relax. If a sedative
is used and you go home right afterward, plan to have someone to drive you home. You
will likely spend at least one night in the hospital after the procedure. This is
to watch your heart and make sure the pacemaker is working the way it should.
-
Based on your health condition, your healthcare provider may ask for other specific
preparation.
What happens during pacemaker insertion?
A pacemaker insertion may be done on an outpatient basis. Or it may be done as part
of your hospital stay. The procedure may vary depending on your health and how your
healthcare provider does the procedure.
Generally, a pacemaker insertion follows this process:
-
You will be asked to remove any jewelry or other objects.
-
You will be asked to remove your clothing and will be given a medical gown to wear.
-
You will be asked to empty your bladder before the procedure.
-
If there is a lot of hair at the incision site, it may be shaved off.
-
An IV (intravenous) line will be started in your hand or arm before the procedure.
This is to give you medicine and fluids.
-
You will lie on your back on the procedure table.
-
You will be connected to an electrocardiogram monitor. This records the electrical
activity of your heart. It monitors your heart during the procedure using small, plastic
electrodes that stick to your skin. Your vital signs will also be watched during the
procedure. These include your heart rate, blood pressure, breathing rate, and oxygen
level.
-
You will get a sedative in your IV line before the procedure to help you relax.
-
The skin at the pacemaker insertion site will be cleaned with antiseptic soap.
-
Sterile towels and a sheet will be placed around this area.
-
A local anesthetic will be injected into the skin of the chest at the insertion site.
-
Once the area is numb, the healthcare provider will make a small cut (incision) at
the insertion site.
-
A sheath is put into a large blood vessel. The sheath is also called an introducer.
It's usually put under the collarbone. The sheath is a small plastic tube. The provider
will thread the pacer lead wire or wires through this tube into the blood vessel and
advance them into the heart.
-
It will be very important for you to stay still during the procedure. This is so that
the catheter does not move. This helps to prevent damage at the insertion site.
-
The provider will thread the lead wire through the sheath into the blood vessel. They
will advance the lead wire through the blood vessel into the heart. A type of moving
X-ray is displayed on a TV screen (fluoroscopy) may be used to help check the location
of the leads.
-
Once the lead wire is inside the heart, it will be tested to be sure it’s in the right
location and it works. There may be 1, 2, or 3 lead wires inserted. This depends on
the type of device your healthcare provider has chosen for your needs.
-
The lead wire is attached to the pacemaker generator. Then the provider will slip
the generator under your skin through the incision just below the collarbone. The
generator is often placed on the nondominant side. This means if you are right-handed,
the device will be placed in your upper left chest. If you are left-handed, the device
may be placed in your upper right chest.
-
The pacemaker will be checked to be sure that it's working correctly.
-
The skin incision will be closed with stitches, adhesive strips, or a special glue.
-
A sterile bandage or dressing will be applied.
What happens after pacemaker insertion?
In the hospital
After the procedure, you may be taken to the recovery room or returned to your hospital
room. A nurse will watch your vital signs.
Tell your nurse right away if you feel chest pain or tightness, trouble breathing,
or pain at the insertion site.
After a period of bed rest, you may get out of bed with help. The nurse will be with
you the first time you get up. They will check your blood pressure while you are lying
in bed, sitting, and standing. Move slowly when getting up from the bed. This is to
prevent dizziness.
You will be able to eat or drink once you are fully awake.
The insertion site may be sore or painful. You can take pain medicine if needed. Your
arm may be placed in a sling overnight. Your provider will give you specific instructions
about activities you can and can’t do. They will talk with you about how to keep your
arm from moving after the procedure. You will have a chest X-ray to make sure your
lung was not injured during the procedure, and to check the device position. You may
be prescribed antibiotics. These are to help prevent an infection around your pacemaker
or at the incision site.
Once your blood pressure, pulse, and breathing are stable and you are alert, you will
be taken to your hospital room. Or you may be allowed to go home. It’s common to spend
at least one night in the hospital after a pacemaker implantation. This is to keep
track of your heartbeat and make sure your pacemaker is working well. Make sure to
have someone drive you home when you are discharged.
At home
You should be able to return to your normal daily routine within a few days. Your
healthcare provider will tell you if you will need to wait. Don't lift or pull anything
for a few weeks. You may also need to limit movement of your arm on the side that
the pacemaker was placed.
You will most likely be able to go back to your usual diet, unless your healthcare
provider tells you differently.
Keep the insertion site clean and dry. You will be told when and how to bathe or shower
safely.
Your healthcare provider will give you specific instructions about driving.
Ask your healthcare provider when you will be able to return to work. The nature of
your work, your overall health, and your progress after surgery will determine how
soon you may go back to work.
Call 911 or get immediate medical care at the nearest emergency department if you have any of the following:
-
Severe or unusual chest pain or pressure
-
Trouble breathing, shortness of breath
-
Dizziness, lightheadedness, fainting
-
Uncontrolled or heavy bleeding from the insertion site
-
Unusual or profuse sweating
Contact your healthcare provider right away if you have any of the following:
-
Fever of 100.4°F (38°C) or higher, or as advised by your healthcare provider
-
Chills
-
Increased pain, redness, swelling, or slight bleeding or other drainage from the insertion
site
-
Nausea or vomiting
-
Lack of energy
-
Rapid or pounding heartbeat (palpitations)
-
Swelling in the arms or hands on the side of the incision
-
Hiccups that will not stop
-
Muscle twitching in your belly (abdomen)
After a pacemaker insertion, you will need to keep regular appointments to make sure
that the pacemaker is working the way it should. The healthcare provider uses a special
computer, called a programmer, to review the pacemaker's activity and adjust the settings
when needed. A remote monitor may also be used to allow the pacemaker to be checked
at your home via the internet or telephone.
Your healthcare provider may give you other instructions after the procedure, depending
on your particular situation.
Things to keep in mind
Always consider the following precautions. Discuss these in detail with your healthcare
provider, or call the company that made your device:
-
Always carry an ID card that states you have a pacemaker. You may want to wear a medical
ID bracelet or necklace saying that you have a pacemaker.
-
Let security screeners know you have a pacemaker before going through security detectors
at the airport or court house. In general, airport detectors are safe for pacemakers,
but the small amount of metal in the pacemaker and leads may set off the alarm. If
you are selected for additional screening by handheld detector devices, tell the screeners
that the detector wand should not be held over your pacemaker for more than a few
seconds. This is because the detector wand contains magnets that may affect the function
or programming of your pacemaker.
-
Most modern pacemakers are safe in an MRI machine. Check with your healthcare provider
before having an MRI scan.
-
Don't go near large magnetic fields, such as power generation sites, and industrial
sites, such as automobile junkyards that use large magnets.
-
Don't use short-wave or microwave diathermy that uses high-frequency, high-intensity
signals. This may be used in physical therapy to treat muscles. The signals can interfere
with or damage your pacemaker.
-
Turn off large motors, such as cars or boats, when working close to them. This is
because they may create a magnetic field.
-
Don't go near high-voltage or radar machinery, such as radio or television transmitters,
electric arc welders, high-tension wires, radar installations, or smelting furnaces.
-
If you need a surgery in the future, tell the surgeon that you have a pacemaker well
before the operation. Ask your cardiologist if you need to do anything before, during,
or after the surgery. Ask about the safety of the electrocautery device often used
during surgery to control bleeding. This may interfere with the pacemaker. In some
cases, the pacemaker's programming will be temporarily changed with a magnet during
the surgery. This is done to lessen the risk of interference from the electrocautery.
-
During any physical or sports activity, protect yourself from trauma to the pacemaker.
A blow to the chest near the pacemaker can affect its function. If you are hit in
that area, see your healthcare provider to make sure your pacemaker is working the
way it should be.
-
Talk with your healthcare provider if you feel ill after any activity, or if you have
questions about starting a new activity.
-
Always contact your healthcare provider if you have any questions about using any
equipment near your pacemaker. Your healthcare provider may give you a list of other
devices and procedures to stay away from.
Cell phones and other electronic devices
Be careful when you use a cell phone or other electronic devices. Follow these tips:
-
Keep them at least 6 inches away from your pacemaker.
-
It's safest to hold all cell phones to the ear farthest from your pacemaker or use
the speaker mode setting.
-
Don’t carry your phone or electronic device in your chest pocket, over the pacemaker.
Instead, carry your cell phone or other electronics in a pocket or bag below your
waist.
Most cell phones and electronic devices don't interfere with pacemakers. But some
cell phones and electronic devices, such as smart watches, use powerful magnets for
wireless charging. This may interfere with the normal function of your pacemaker.
The charging device itself and other magnet accessories can also interfere with the
normal function of your pacemaker. Store these devices at least 15 inches away from
your pacemaker.
Follow any other instructions given to you by your healthcare provider or from the
manufacturer of your pacemaker.
Next steps
Before you agree to the test or procedure make sure you know:
-
The name of the test or procedure
-
The reason you are having the test or procedure
-
What results to expect and what they mean
-
The risks and benefits of the test or procedure
-
What the possible side effects or complications are
-
When and where you are to have the test or procedure
-
Who will do the test or procedure and what that person’s qualifications are
-
What would happen if you did not have the test or procedure
-
Any alternative tests or procedures to think about
-
When and how will you get the results
-
Who to call after the test or procedure if you have questions or problems
-
How much you will have to pay for the test or procedure