The Noyes Newsroom
2024202320222021
Zach Mix named Director of Medical Imaging at Noyes Health
Monday, August 19, 2024
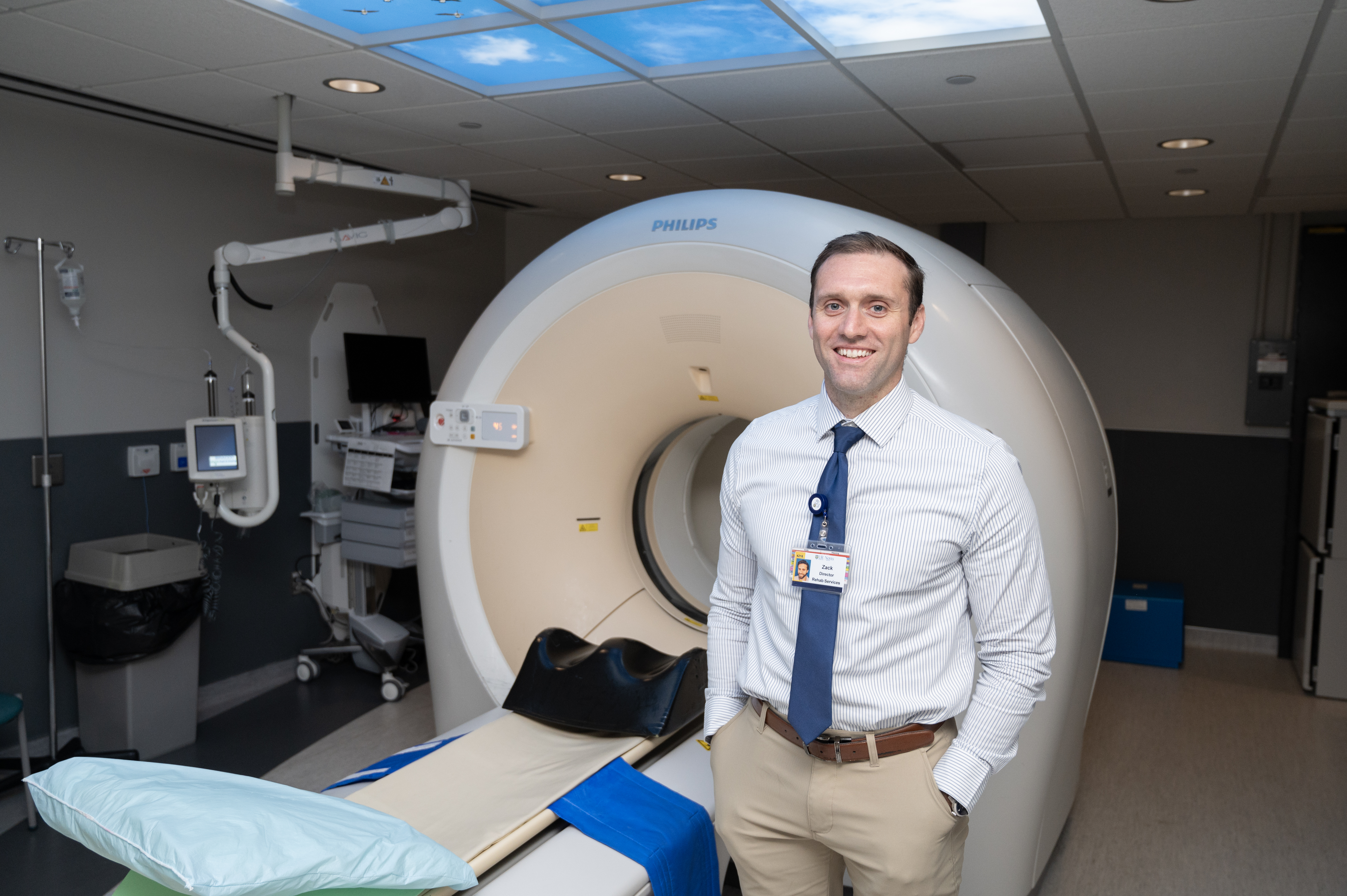 Zach Mix, Director of Medical Imaging at Noyes Health
Zach Mix, Director of Medical Imaging at Noyes Health
UR Medicine Noyes Health is happy to announce that Zach Mix has been promoted to Director of Medical Imaging and Rehab.
“Zach has been with Noyes’ Rehab Program for nine years, where he’s cultivated an incredibly talented, high-quality team, through sound decision-making and a focus on patient care,” said Michael Donegan, Vice President of Operations at UR Medicine Noyes Health. “He’ll transition out of clinical practice over the coming weeks, moving full time into leadership of both the Rehab and Medical Imaging Programs.”
Mix received his bachelor’s degree in athletic training from Alfred University before receiving his Doctorate of Physical Therapy from Nazareth University.
“I am very excited to be working with the imaging team,” said Mix. “I am very impressed with the professionalism and level of skill and dedication demonstrated by everyone on the team. It is a really strong group.”
Mix started as a staff physical therapist at Noyes before being promoted to site supervisor and has been overseeing the Physical Therapy, Occupational Therapy and Speech Therapy programs at both the Dansville and Geneseo locations since 2022.
“This is an exciting challenge for me,” said Mix of his promotion. “I am proud of the team I have developed in therapy. I want to foster an environment in the imaging department that promotes excellence and employee satisfaction. It is important that my team knows they are part of a highly skilled group, and that they enjoy their jobs. When people enjoy what they do, it translates to the patient care making for a better experience.”
Mix lives in Avon with his wife, a 2-year-old son and his 5-month-old daughter. In his spare time he is passionate about fitness, regularly attends church, and enjoys spending time with his family.
Empire Strikes Back Against Cancer Golf Tournament Raises $17,500 for Noyes
Tuesday, July 9, 2024
 From left: Bridgett Hoag, Empire Realty Group; Dr. Chad Teeters, President and CEO of Noyes Health; Justine Fox, Empire Realty Group.
From left: Bridgett Hoag, Empire Realty Group; Dr. Chad Teeters, President and CEO of Noyes Health; Justine Fox, Empire Realty Group.
DANSVILLE – The Empire Strikes Back Against Cancer Golf Tournament successfully raised $17,750 for UR Medicine Noyes Health during the 7th annual event. This brings the grand total raised to over $103,000. In addition, $900 was raised for The Vincent House in Wayland.
Organized by the Empire Realty Group in Dansville, the event was held Saturday, June 8 at Brae Burn Golf Course in Dansville. The nine-hole tournament saw four full flights of golfers, and had a unforgettable hole-in-one on hole #1 by Emily Crowell.
The event will return for its final year on June 14, 2025.
3D Tomosynthesis mammograms now available at Noyes Health in Geneseo
Monday, June 17, 2024
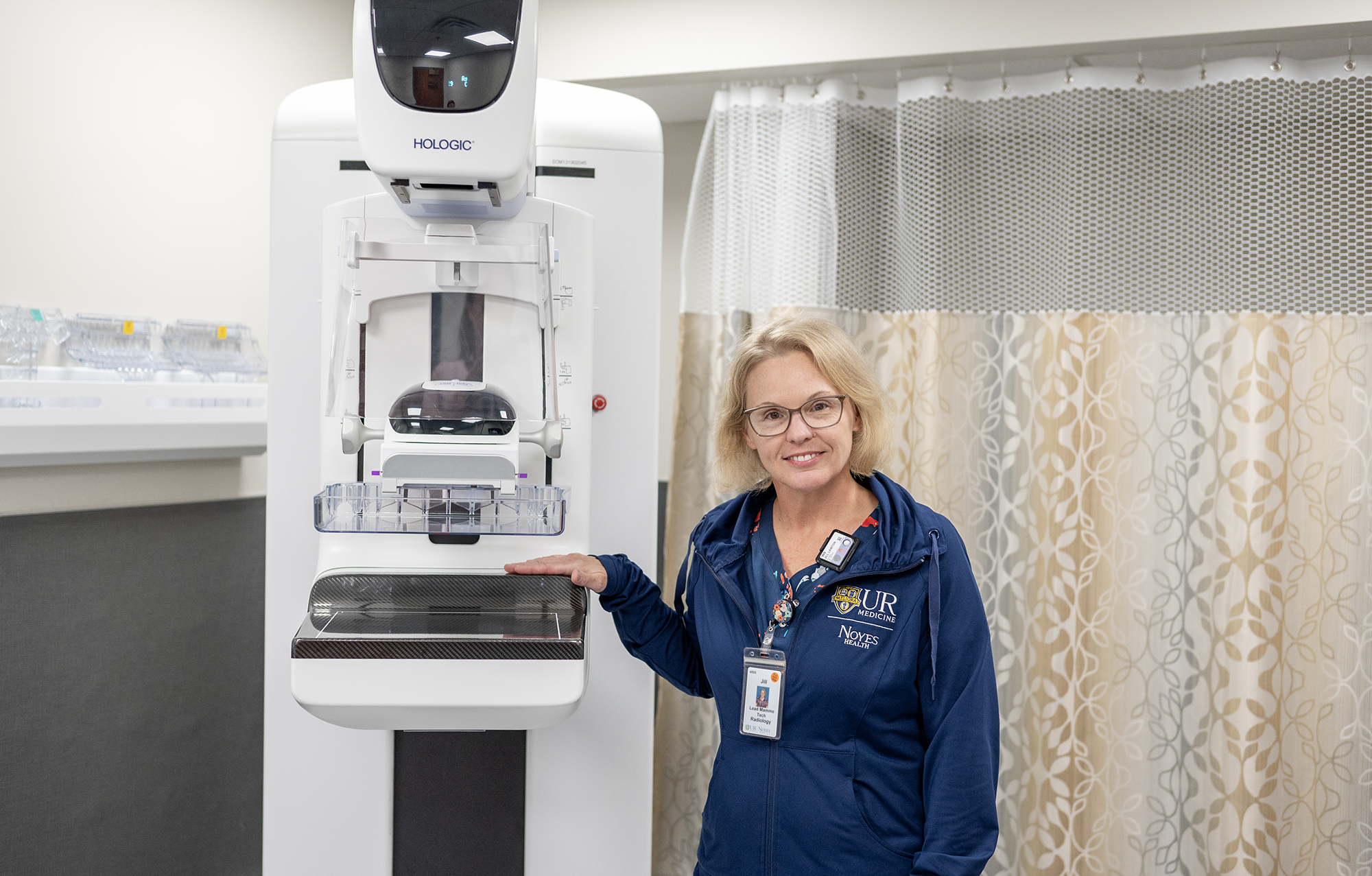 Jill Lawton poses for a photo with the new mammogram machine in Geneseo.
Jill Lawton poses for a photo with the new mammogram machine in Geneseo.
GENESEO -- UR Medicine Noyes Health is happy to offer 3D Tomosynthesis mammograms at Noyes Health Services in Geneseo.
“The new 3D mammogram machine is the newest technology in breast imaging,” said Jill Lawton, Lead Mammography Technologist at UR Medicine Noyes Health. “It is especially beneficial for women with dense breast tissue. The technology decreases the likelihood of patient having to be called back for additional imaging after a screening exam. Patients won’t notice a difference in the exam – the compression and exposure time are about the same as with a 2D mammogram.”
Funding for the project was made possible thanks to a $1.5M bipartisan omnibus-spending package for Fiscal Year 2023. The spending package, initially submitted to then-Rep. Chris Jacobs, was secured by U.S. Senate Majority Leader Charles E. Schumer and U.S. Senator Kirsten Gillibrand, provided over $250M of support for community-based projects in the Rochester-Finger Lakes Region.
The new mammogram machine in Geneseo is one of the many recent additions to Noyes Health to help further its mission to provide high quality healthcare to the Southern Tier and Finger Lakes regions.
Appointments for mammograms can be made by calling (585) 991-6016 for the Geneseo location, or (585) 335-4235 for the Dansville location. Walk-in appointments are also available at both locations.
EXTRAORDINARY NURSES RECOGNIZED AT UR MEDICINE NOYES HEALTH
Thursday, June 6, 2024

Linda Mathieson, RN, Nursing Supervisor at UR Medicine Noyes Health was recently honored with DAISY Nurse Leader Award, and Natalie Morabito, RN was honored with The DAISY Award® For Extraordinary Nurses.
 Linda Mathieson
Linda Mathieson
The DAISY Nurse Leader Award was created to shine a light on those who do not typically have direct patient care as part of their work, and those who create an environment where compassionate, skillful care thrives. This award recognizes Nurse Managers, Directors, Assistant Managers, Charge Nurses, Chief Nursing Officers, Informatics Nurses, and Patient Flow Nurses.
Mathieson’s nomination read: "Linda is an outstanding nurse who can always be counted on to help our staff. She is kind, compassionate, and a great communicator. She is a great teacher, leader, and loves to share her knowledge with anyone. She is an inspiration and has the respect of everyone in each department."
Morabito’s nomination read: “Natalie is the kindest nurse and is so good with my 93-year-old mother-in-law. She supported her in staying off pain medication so she could visit with her children, 12 grandchildren and 6 great-grandchildren. Natalie made all of us feel like we were at home and welcomed us with caring kindness.
 Natalie Morabito
Natalie Morabito
Morabito’s nomination read: “Natalie is the kindest nurse and is so good with my 93-year-old mother-in-law. She supported her in staying off pain medication so she could visit with her children, 12 grandchildren and 6 great-grandchildren. Natalie made all of us feel like we were at home and welcomed us with caring kindness.
The not-for-profit DAISY Foundation is based in Glen Ellen, CA, and was established by family members in memory of J. Patrick Barnes. Patrick died at the age of 33 in late 1999 from complications of Idiopathic Thrombocytopenic Purpura (ITP), a little known but not uncommon auto-immune disease. The care Patrick and his family received from nurses while he was ill inspired this unique means of thanking nurses for making a profound difference in the lives of their patients and patient families.
Said Bonnie Barnes, FAAN, CEO and Co-Founder of The DAISY Foundation, "When Patrick was critically ill, our family experienced first-hand the remarkable skill and care nurses provide patients every day and night. Yet these unsung heroes are seldom recognized for the super-human work they do. The kind of work the nurses at [hospital] are called on to do every day epitomizes the purpose of The DAISY Award.”
Glaucoma Q&A with Dr. Ruba Muhtaseb
Thursday, March 7, 2024
Learn more about Glaucoma with Dr. Ruba Muhtaseb of the Flaum Eye Institute. Dr. Muhtaseb performs procedures at Noyes Health Services in Geneseo.
 Caption
Caption
What is Glaucoma?
Glaucoma is a disease that damages the optic nerve. This usually happens when fluid builds up in the front part of the eye increasing the eye pressure.
Who is at greatest risk?
People are at increased risk of glaucoma include those who are over age of 40, who have family members previously diagnosed with glaucoma, certain ethnicities ( African American, Hispanic, Asian), have been on steroids, or previous eye trauma.
What are symptoms of Glaucoma?
Glaucoma has no symptoms in its early stages. In fact, half the people with glaucoma do not know they have it. Having regular eye exams can help the ophthalmologist find the disease before vision is lost.
How is Glaucoma treated?
Glaucoma is usually controlled with eye drops. Certain types of lasers and surgeries can be offered in certain situations. Damage from glaucoma is permanent and cannot be reversed. Medicine and surgery can help stop further damage.
ABOUT DR. RUBA MUHTASEB
Dr. Muhtaseb offers expert medical and surgical care to adults suffering from eye disease, as well as providing routine and preventative vision care. She earned her medical degree from the University of Jordan Medical School in Aman, Jordan. She remained there to complete her ophthalmology training, serving as Chief Resident during her senior year. Upon graduation, she pursued general ophthalmology in Jordan, working in hospital-based and private practices where she performed laser vision correction and cataract surgery. She came to America to continue her training and completed two specialty fellowships: the first in medical retina at the University of Miami’s top-ranked Bascom Palmer Eye Institute, and a second fellowship in Glaucoma at Tufts University in Boston.
Dr. Muhtaseb enjoys working with primary care providers, optometrists, and other specialists to promote and maintain vision health. She is fluent in both Arabic and English. Dr. Muhtaseb treats the following conditions:
- Cataracts
- Eye injuries
- Glaucoma
- Ocular infections
- Diabetic eye disease
- Dry eye disease
- Refractive Error
To make an appointment with Dr. Muhtaseb at the Flaum Eye Institute in Geneseo, call 585-273-3937.
Office for the Aging Collaborative Program Named Crown Communities Award Winner by American City & County
Monday, February 19, 2024
MOUNT MORRIS — American City & County has named the Home Away From Home Respite Program, a collaborative initiative from the Livingston County Office for the Aging and several local partners, as a 2023 winner of its annual Crown Communities Award. The award recognizes city or county projects from across the country that have had a positive impact on their local community as a whole.

Since its inception in 2015, the Home Away from Home Respite Program has provided vital caregiver respite services in Livingston County through innovative service delivery. The program identified and addressed a gap in existing local caregiver services by providing a secure environment for individuals requiring care to spend up to eight hours per week. This initiative offers caregivers a valuable break to tend to personal matters and avoid caregiver stress and burnout, symptoms commonly experienced by those dedicating time and energy to manage the health and safety of someone else.
“When local partners come together with a shared purpose they can effectively address and fulfill the diverse needs of a community,” said Livingston County Office for the Aging Director Sue Carlock. “This recognition underscores the program’s exceptional impact on our community, offering crucial support to caregiver and care receivers alike. This initiative’s success is directly related to the dedication of our partners and the resilience of our participants.”
The Home Away From Home Respite Program is a collaborative effort between the Livingston County Office for the Aging, Noyes Community Outreach Services, Livingston Cares, SUNY Geneseo, the Interfaith Center, Lifespan, and the New York State Caregiver Resource Center to address the needs of caregivers experiencing physical, mental or emotional exhaustion.
The program is funded through the Administration for Community Living, the New York State Office for the Aging, Livingston County, participant contributions, and grants. The involvement of SUNY Geneseo students as volunteers has made the program a cost-effective solution for caregivers. In-home respite services of a similar duration are often cost prohibitive for those in need. As a Crown Communities Award winner, the Home Away From Home Respite Program now serves as a model for community-driven initiatives nationwide.
Learn more about events and programs for older County residents at the Livingston County Office for the Aging website or by calling 585-243-7520.
Noyes Memorial Hospital Recognized for Higher Quality and Cost-Efficiency in Maternity Care
Thursday, January 4, 2024

Noyes Memorial Hospital – a part of UR Medicine Noyes Health -- is proud to be recognized by Excellus BlueCross BlueShield with a Blue Distinction® Centers+ (BDC+) for Maternity Care designation, as part of the Blue Distinction Specialty Care program. To earn this designation, each facility must deliver quality care, safely and cost-effectively.
The Blue Distinction Centers for Maternity Care program plays a key role in the Blue Cross Blue Shield Association’s (BCBSA) National Health Equity Strategy aimed at reducing racial health disparities across the care spectrum and improving patient outcomes for all Americans. To align with this strategy, the Blue Distinction Centers for Maternity Care program enhanced its quality and measurement standards to recognize higher-quality facilities that have taken action to respond effectively to obstetric emergencies, reduce racial disparities, and improve maternal health outcomes.
Based on data from the current designation cycle, facilities designated under the Blue Distinction Centers for Maternity Care program demonstrate higher-quality care compared to non-Blue Distinction Center facilities, with overall average rates of 26% lower episiotomies, 60% fewer elective deliveries and 17% lower cesarean births—all of which point to healthier outcomes for patients. BDC+ designated facilities also exhibited an average savings of 21% for maternity care.
“Noyes is the only hospital with a maternity department in Livingston County, and there are no hospitals in Steuben County with maternity services, so this is a vital service in our area,” said Dr. Chad Teeters, president and CEO of UR Medicine Noyes Health. “This designation reflects the high quality of service we are proud to provide to the community.”
The Blue Distinction Centers for Maternity Care program’s selection criteria was devised to close clinical care gaps and reduce inequities that persist throughout the maternal care spectrum. The selection criteria includes components of BCBSA’s Maternal Health Equity Actions, which dismantle the cultural, operational and structural barriers that have created inequities that persist in maternal care.
To be designated under this program, each applicant facility was evaluated on a combination of objective data on patient outcomes as well as the practices implemented to reduce racial disparities and improve maternal health outcomes, such as:
- Using evidence-based best practices to respond effectively to obstetric emergencies
- Offering unconscious bias training
- Participating in the regional Perinatal Quality Collaborative
- Having doula support available on the maternity care team
- Collecting race, ethnicity and language data
- Having a program dedicated to quality improvements in maternal care
- Running drills and simulations to prepare providers are prepared to deal with a range of obstetric emergencies
- Demonstrating health outcomes that exceed the selection criteria from our program’s previous evaluation cycle
Noyes Memorial Hospital is proud to be recognized by Excellus BCBS for meeting the rigorous quality selection criteria for maternity care set by the Blue Distinction Specialty Care program.
Since 2006, the Blue Distinction Specialty Care program has helped patients find quality specialty care at lower costs in the areas of bariatric surgery, cancer care, cardiac care, cellular immunotherapy, fertility care, gene therapy, knee and hip replacement, maternity care, spine surgery, substance use treatment and recovery, and transplants, while encouraging health care professionals to improve the care they deliver.
For more information about the program and for a complete listing of the designated providers, visit the Excellus BCBS website.
All companies and trademarks listed above are the property of their respective owners and used for identification purposes only, and are in no way associated or affiliated with the Blue Cross Blue Shield Association. Use of these trademarks does not imply endorsement. The Blue Cross® and Blue Shield® names and symbols and Blue Distinction® are registered trademarks of the Blue Cross Blue Shield Association.
UR Medicine Noyes Health is a diverse and comprehensive nonprofit health care system serving all of Livingston County and parts of Steuben, Allegany and Ontario counties in New York. The system includes Nicholas H. Noyes Memorial Hospital in Dansville, Noyes Health Services and Urgent Care in Geneseo, Noyes Kidney and Dialysis Center in Geneseo, and Noyes Mental Health and Wellness Services in Dansville and Avon. Nicholas H. Noyes Memorial Hospital is a full-service, 67-bed community the only 24-hour Emergency Department in Livingston County, and is accredited by the Joint Commission. The hospital is located off Interstate 390, Exit 4. For more information about UR Medicine Noyes Health, visit noyes.urmc.edu
Excellus BlueCross BlueShield, an independent licensee of the Blue Cross Blue Shield Association, is a nonprofit health plan with 1.5 million upstate New York members. The company's mission is to help people live healthier and more secure lives through access to high-quality, affordable health care. Its products and services include cost-saving prescription drug discounts, wellness tracking tools and access to telemedicine. With more than 4,200 employees, the company is committed to attracting and retaining a diverse workforce to foster innovation and better serve its members. It also encourages employees to engage in their communities by providing paid volunteer time off as one of many benefits. To learn more, visit ExcellusBCBS.com.
About the Blue Cross Blue Shield Association
The Blue Cross Blue Shield Association is a national federation of independent, community-based and locally operated Blue Cross and Blue Shield companies that collectively provide health care coverage for one in three Americans. BCBSA provides health care insights through The Health of America Report series and the national BCBS Health IndexSM. For more information on BCBSA and its member companies, please visit bcbs.com.
About Blue Distinction Centers
Blue Distinction Centers (BDC) met overall quality measures, developed with input from the medical community. A Local Blue Plan may require additional criteria for providers located in its own service area; for details, contact your Local Blue Plan. Blue Distinction Centers+ (BDC+) also met cost measures that address consumers’ need for affordable healthcare. Each provider’s cost of care is evaluated using data from its Local Blue Plan. Providers in CA, ID, NY, PA, and WA may lie in two Local Blue Plans’ areas, resulting in two evaluations for cost of care; and their own Local Blue Plans decide whether one or both cost of care evaluation(s) must meet BDC+ national criteria. National criteria for BDC and BDC+ are displayed on www.bcbs.com. Individual outcomes may vary. For details on a provider’s in-network status or your own policy’s coverage, contact your Local Blue Plan and ask your provider before making an appointment. Neither Blue Cross and Blue Shield Association nor any Blue Plans are responsible for noncovered charges or other losses or damages resulting from Blue Distinction or other provider finder information or care received from Blue Distinction or other providers.