For Nurses, Many Hands (and a Single Handoff Tool) Make Safe Work
There’s no arguing that a big job whose tasks are divvied up among many people goes faster than if one person tackles it. But making the pieces of those tasks come back together unruffled can be tricky when they’re complex, as health issues often are.
As of March, nurses at UR Medicine’s Strong Memorial and Highland Hospitals added a handoff tool in eRecord to their proverbial tool belts. This one aggregates patient info from different sections and screens of the electronic medical record into an elegant profile outlining the most important nuggets for handoff. That goes for any and all handoffs between nurses: when one is cycling off duty and another is coming on, as well as when a patient transitions through different units, services, or departments.
“The beauty here is in the standardization: An incoming nurse can be certain that she’ll have an accurate, up-to-date synopsis of who she’ll be caring for. It’s just safer,” said Anna Lambert, associate director of Cardiovascular and Thoracic Nursing at UR Medicine’s Strong Memorial Hospital. Before meeting her patient, that just-on-the-clock/new-to-the-patient nurse will have taken a look at the diagnosis, contact info, medical history, most recent pain scores, and meds, alongside other info.
These are crystal-clear categories that must be filled in before any nurse wraps up her shift or passes the patient along, which means the screen tells an objective patient story—not the patient story as perceived by someone else—with all of the must-have “DATAS” information (that’s nursing lingo for description, active issues, to do, anticipatory guidance, and special needs). Here's an example of what the screen looks like (using hypothetical patient data):
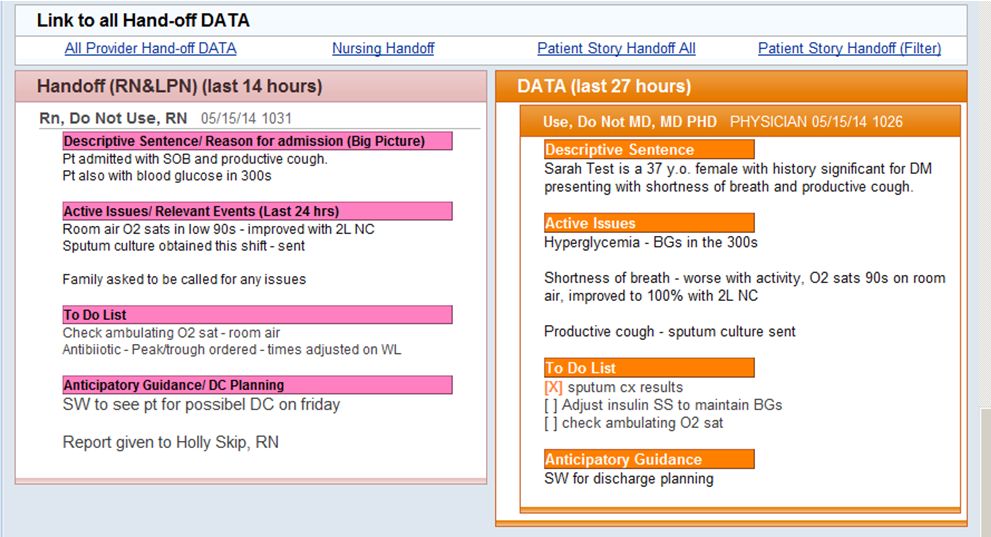
“From our pediatric to our geriatric patients, and everyone between, this tool is absolutely relevant,” said Lambert. “Keeping tabs on exactly this patient info is nothing new for our nurses—the tool simply saves them from venturing into eRecord’s wild and hunting it down. Their screen time is cut, so they can spend that time caring for patients in-person.”
About a year ago, UR Medicine providers adopted a tool the nurses’ is based on. Development of the nursing one took place on these grounds, with nurses from Strong and Highland Hospital putting their heads together to elaborate on what the providers were using, and altering it to fit nurses’ workflow. Two UR Medicine eRecord specialists, Sarah Davila and Mary Lou Heinrich, built and tweaked the tool, as workgroups tested it out intermittently.
Doubling the relief that the handoff tool is now in place is the fact that it’s been in the cooker for some time; even pre-eRecord, Lambert and Michael S. Leonard, M.D., M.S., had such systematic communication on their wish list. That was back when handoffs varied, even from unit to unit. As far as what details transmit—and in what order—it really used to boil down to personal preference. The biggest change from then to now? Handoffs then were oral, relying on the memories of two people.
On any given day, a nurse never knew what background he’d be given to work with. If he felt that there were holes, it was up to him to mine the patient record to dig up what he sought.
According to Lambert, it was a widespread challenge in hospitals across the country, and yet when faced with murmurs of a solution such as this one, there was general resistance. Change is hard, and folks didn’t see the reason behind it here.
For the time being, concrete data comparing life before the tool and life after the tool is yet to come, since it made its debut only weeks ago. But, Lambert noted, “We know for sure that it’s already touching patients positively. Our communication among care teams is sharper—and we always welcome such improvement with open arms.”
Jennifer Fortin | 5/19/2014



