Meningitis
Meningitis
Clinical History
A 3-day-old infant presented to the ED with a history of poor feeding and a tonic-clonic seizure. The infant was born at 37 weeks gestation. The pregnancy was uncomplicated and there was no history of maternal chorioamnionitis.
Results of blood and CSF cultures revealed E. coli. Although antibiotics and other medications were given, the baby’s condition worsened. The infant died five days after admission to the hospital.
Gross Examination
Outer examination revealed a normal infant. Internal examination showed a dilated cecum with fecal contents. The liver was enlarged with several areas of necrosis. The brain surface was covered with a purulent exudate (Figure 1).
Click an image to view larger format.
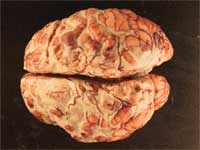
Figure 1: Gross examination reveals
a purulent exudate over surface of brain
Microscopic Examination
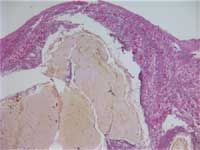
The diagnosis of meningitis was confirmed. The leptomeninges showed acute inflammation (Figure 2). The cecum was focally necrotic and the wall was markedly thinned (Figure 3). The liver showed centrilobular necrosis (Figure 4).
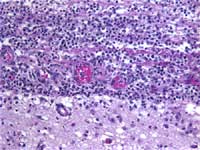
Figure 2: H & E stain shows
acute and chronic inflammation along
the leptomeninges (upper half) of
the brain (lower half)
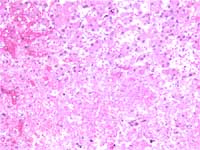
Figure 4: H & E stain of liver shows
areas of necrosis
Microbiology
The post-mortem blood and brain tissue cultures grew out E. coli.
Discussion
Neonatal meningitis is the inflammation of the linings of the brain and spinal cord. It affects 1/2000-4000 infants. It usually occurs simultaneously with sepsis (the blood poisoning form of the disease), whether it presents with early symptoms (within the first 2 days after birth) or late symptoms (usually in the second week of life). Early presentation typically occurs with prematurity or obstetrical complications; neonates show signs of decreased responsiveness, focal seizures and tight fontanelle, along with fever or feeding difficulty. Nuchal rigidity and extensor posturing are more commonly found with late symptoms, as are cranial nerve palsies.
Neonatal meningitis is usually bacterial or viral. Bacterial meningitis is often more serious.
Group B beta-hemolytic Streptococcus (Strep. agalactiae) is the most common cause of neonatal meningitis in the United States. It is followed by E. coli, Listeria monocytogenes and Klebsiella pneumoniae. In developing countries, Staphylococcus aureus and Streptococcus pyogenes, along with GBS, are the most common gram-positive bacteria causing neonatal meningitis. Salmonella species and E. coli are the most common gram-negative bacteria causing neonatal meningitis.
It is believed that infants may become inoculated with the bacteria from swallowing of infected amniotic fluid or maternal secretions during delivery by mothers who have vaginal colonization of certain bacteria. Later infections may be acquired through nosocomial transmission. Neonates are at increased risk of developing sepsis and meningitis than other age groups because of immaturity of their immune systems.
After the bacteria are introduced into the infant's body, it is believed that colonization occurs in the gastrointestinal tract. The GI tract is thought to be the portal of entry into the bloodstream (this may explain why the infant in this case had thinning and necrosis of the wall of the cecum). Once the bacteria enters the blood, it then travels through other organs of the body, such as the liver and brain, causing inflammation.
Bacterial meningitis requires therapy with antibiotics. Some infants may suffer long-term neurologic impairment. Catastrophic sequelae are rare.
Dr. Sandra Vella, May 2003