Clinical Training
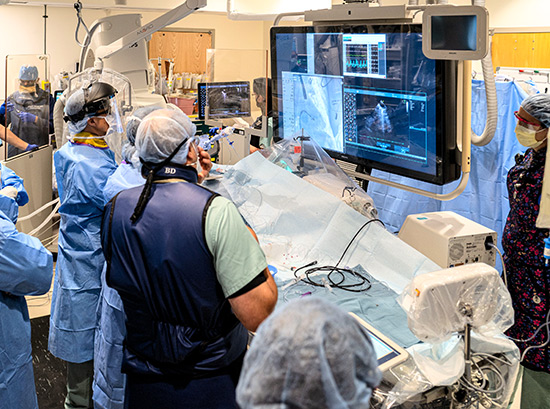
Clinical training forms the foundation of the Interventional Cardiology Fellowship at the University of Rochester. Fellows work closely with expert faculty in a high-volume academic environment, gaining progressive autonomy while mastering both routine and advanced interventional techniques.
Training Overview
- Primary Assisted Operator in the cardiac catheterization lab
- One-on-One Faculty Mentorship
- Balanced Supervision & Autonomy
- Weekly Outpatient Clinic – Evaluate patients before and after procedures
- Emphasis on:
- Procedural indications & appropriate use
- Technical excellence
- Decision-making & post-procedural care
Clinical Focus Areas
Coronary Artery Disease
The University of Rochester is a high-volume PCI center and tertiary referral hub, offering advanced coronary care:
- Radial-first approach for most procedures
- Active Primary PCI Program for acute MI
- Complex PCI (CHIP) and Heart Team collaboration
- Advanced imaging and tools: OCT, IVUS, FFR, atherectomy, thrombectomy, lithoplasty
 Peripheral Arterial Disease
Peripheral Arterial Disease
Fellows gain hands-on experience treating peripheral vascular disease, focusing on:
- Angiography and percutaneous revascularization
- Medical, endovascular, and surgical decision-making
- Comprehensive understanding of treatment indications
- Renal artery daeruahan for treatment of resistant hypertension
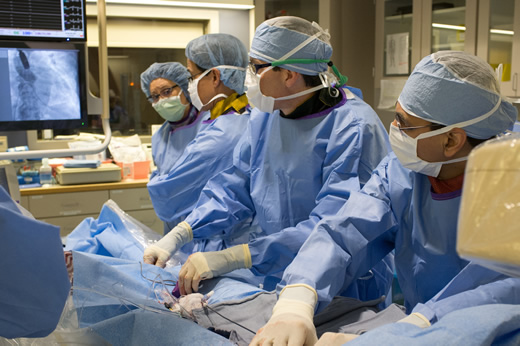 Structural Heart Disease
Structural Heart Disease
Robust structural heart training includes:
- TAVR – Transcatheter Aortic Valve Replacement
- TEER – Transcatheter Mitral Edge-to-Edge Repair
- TTVR – Transcatheter Tricuspid Valve Repair
- ASD/PFO closure
- Balloon valvuloplasty (aortic, mitral, pulmonic)
- Left atrial appendage closure
- Embolization procedures for cardiac anomalies
- Debulking therapy for right heart infections/thrombosis
Hypertrophic Cardiomyopathy
Fellows actively evaluate and treat patients through our busy Alcohol Septal Ablation program, a key intervention for obstructive hypertrophic cardiomyopathy.
Cardiogenic Shock & Advanced Heart Failure
As the only cardiac transplant center in Central and Western NY, our program offers:
- Management of acute cardiogenic shock
- Training in percutaneous LVAD, RVAD, and ECMO implantation
- Involvement in advanced mechanical circulatory support (MCS) programs
Pulmonary Embolism
Through our Pulmonary Embolism Response Team (PERT), fellows participate in:
- Aspiration thrombectomy
- Catheter-directed thrombolysis for high-risk PE patients