Echocardiogram
What is an echocardiogram?
An echocardiogram (echo) is a noninvasive procedure. This means it does not pierce
the skin. It's used to check the heart's function and structures. During the procedure,
a transducer (like a microphone) sends out sound waves at a frequency too high to
be heard. When the transducer is placed on the chest at certain locations and angles,
the sound waves move through the skin and other body tissues to the heart tissues.
The waves bounce or "echo" off the heart structures. These sound waves are sent to
a computer that can create moving images on the screen of the heart walls and valves.
There are several special types of echocardiography:
-
M-mode echo. This is the simplest type of echo. It makes an image similar to a tracing rather than
an actual picture of heart structures. M-mode echo is useful for measuring or viewing
heart structures, such as the heart's pumping chambers, the size of the heart itself,
and the thickness of the heart walls.
-
Doppler echo. This method is used to measure and evaluate the flow of blood through the heart's
chambers and valves. The amount of blood pumped out with each beat shows how well
the heart is functioning. It can also find abnormal blood flow within the heart, which
can mean there is a problem with 1 or more of the heart's valves, or with the heart's
walls.
-
Color Doppler. Color Doppler is an enhanced form of Doppler. With color Doppler, different colors
are used to designate the direction and quantity of blood flow. This simplifies the
interpretation of the Doppler method.
-
2-D (2-dimensional) echo. This method is used to "see" the actual motion of the heart structures. A 2-D echo
view appears cone-shaped on the monitor, and the real-time motion of the heart's structures
can be seen. This lets the provider see the various heart structures at work.
-
3-D (3-dimensional) echo. 3-D echo method captures 3-dimensional views of the heart structures with greater
detail than 2-D echo. The live or "real time" images allow for a more accurate evaluation
of heart function by using measurements taken while the heart is beating. 3-D echo
shows enhanced views of the heart's anatomy and can be used to plan treatment for
a person with heart disease.
Why might I need an echocardiogram?
An echocardiogram may be done for further evaluation of signs or symptoms that may
suggest:
-
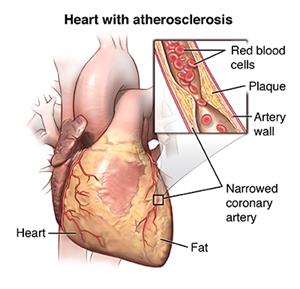
Atherosclerosis. A gradual clogging of the arteries by fatty materials and other substances in the
blood stream. It can lead to problems in the wall motion or pumping function of your
heart.
-
Cardiomyopathy. An enlargement of the heart due to thick or weak heart muscle
-
Congenital heart disease. Defects in 1 or more heart structures that occur during formation of the fetus, such
as a ventricular septal defect (hole in the wall between the 2 lower chambers of the
heart).
-
Heart failure. A condition in which the heart muscle has become weakened or stiff during heart relaxation
and blood can't be pumped efficiently. This can cause fluid buildup (congestion) in
the blood vessels and lungs, and edema (swelling) in the feet, ankles, and other parts
of the body.
-
Aneurysm. A widening and weakening of a part of the heart muscle or the aorta (the large artery
that carries oxygenated blood out of the heart to the rest of the body). The aneurysm
may be at risk for rupture.
-
Heart valve disease. Malfunction of 1 or more of the heart valves that may cause an abnormality of the
blood flow within the heart. The valves can become narrowed and prevent blood from
flowing through the heart or out to the lungs and body. The valves can also become
leaky with blood flow leaking backwards. An echocardiogram can also check for infection
of the heart valve tissue.
-
Cardiac tumor. A tumor of the heart that may occur on the outside surface of the heart, within 1
or more chambers of the heart, or within the muscle tissue (myocardium) of the heart.
-
Pericarditis. An inflammation or infection of the sac that surrounds the heart.
-
Pericardial effusion or tamponade. The sac around the heart can become filled with fluid, blood, or infection. This can
compress the heart muscle and prevent it from beating and pumping blood normally. This
can cause symptoms of feeling dizzy, lightheaded, or a dangerous drop in blood pressure.
-
Atrial or ventricular septal wall defects. Irregular channels between the right and left sides of the heart may be present at
birth, or may occur form trauma, or after a heart attack. These defects occur in the
upper filling chambers (atria) or the lower pumping chambers (ventricles). This may
cause heart failure or poor blood flow. Or increase your risk for stroke.
-
Shunts. Shunts can be seen in atrial and ventricular septal defects. And when irregular blood
flow is pushed through the circulation from the lungs and liver.
An echocardiogram may also be done to evaluate the heart’s overall function and general
structure.
Your healthcare provider may have other reasons to recommend an echocardiogram.
What are the risks of an echocardiogram?
This imaging procedure is not invasive and carries little to no risks. You may have
discomfort from the positioning of the transducer because it can put pressure on the
surface of the body. For some people, having to lie still on the exam table for the
length of the procedure may cause some discomfort or pain.
You may have other risks depending on your specific health condition. Discuss any
concerns with your healthcare provider before the procedure.
How do I get ready for an echocardiogram?
-
Your healthcare provider will explain the procedure to you and ask if you have any
questions.
-
Generally, you don't need to do any preparation, such as fasting or having sedation.
-
Tell your healthcare provider of all prescription and over-the-counter medicines and
herbal supplements that you are taking.
-
Tell your healthcare provider if you have a pacemaker.
-
Based on your medical condition, your healthcare provider may request other specific
preparation.
-
Wear a loose-fitting top that is easy to remove or able to be unbuttoned.
What happens during the procedure?
An echocardiogram (Echo) may be done on an outpatient basis or as part of your stay
in a hospital. Procedures may vary depending on your condition, type of echo, and
your healthcare provider’s practices.
Generally, an echocardiogram follows this process:
-
You will remove any jewelry or other objects that may interfere with the procedure.
You may wear your glasses, dentures, or hearing aids if you use any of these.
-
You will remove clothing from the waist up and will be given a gown to wear.
-
You will lie on a table or bed, on your left side. A pillow or wedge may be placed
behind your back for support.
-
You will be connected to an ECG monitor that records the electrical activity of the
heart and keeps track of the heart during the procedure using small, adhesive electrodes.
The ECG tracings that record the electrical activity of the heart will be compared
with the images displayed on the echocardiogram monitor.
-
The room will be darkened so that the images on the echo monitor can be seen by the
technologist.
-
The technologist will place warmed gel on your chest and then place the transducer
probe on the gel. You will feel a slight pressure as the technologist positions the
transducer to get the desired images of your heart.
-
During the test, the technologist will move the transducer probe around and apply
varying amounts of pressure to get images of different locations and structures of
your heart. The amount of pressure behind the probe should not be uncomfortable. If
it does make you uncomfortable, let the technologist know. You may be asked to hold
your breath, take deep breaths, or even sniff through your nose during the procedure.
-
If the structures of your heart are hard to see, the technologist may use an intravenous
(IV) contrast that helps the heart chambers show up better. This is not an iodine-based
contrast, so you don't have to worry if you have an allergy to shrimp or shellfish
with this type of contrast.
-
After the procedure, the technologist will wipe the gel from your chest and remove
the ECG electrode pads. You may then put on your clothes.
What happens after an echocardiogram?
You may resume your usual diet and activities unless your healthcare provider tells
you differently.
Generally, there is no special type of care after an echo. Your healthcare provider
may give you other directions after the procedure, depending on your situation. A
cardiologist will interpret the images and send their final impression to your healthcare
provider.
Next steps
Before you agree to the test or procedure make sure you know:
-
The name of the test or procedure
-
The reason you are having the test or procedure
-
What results to expect and what they mean
-
The risks and benefits of the test or procedure
-
What the possible side effects or complications are
-
When and where you are to have the test or procedure
-
Who will do the test or procedure and what that person’s qualifications are
-
What would happen if you did not have the test or procedure
-
Any alternative tests or procedures to think about
-
When and how you will get the results
-
Who to call after the test or procedure if you have questions or problems
-
How much you will have to pay for the test or procedure