Case of the Month: Metastasis or Two Primary Neoplasms?
Author: Leah Nash, MS3
Faculty mentor: Dr. Xiaolan Ou, M.D., Ph.D.
Clinical History
A 65-year-old male presents with one-month history of shortness of breath that is worsened by deep breathing, exertion, and activity. Over the past few days, he developed a non-productive cough. He has associated pains in his chest, upper abdomen, and middle back.
Past Medical History
Former smoker (40 pack-year history) with GERD.
Recent History
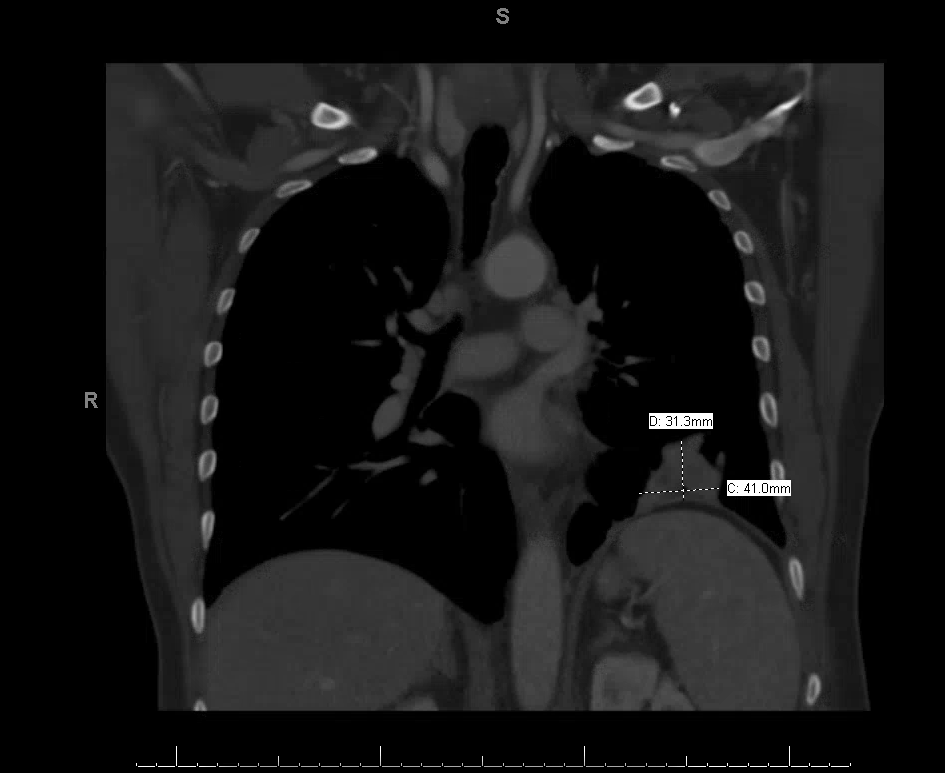
CT chest with contrast showed a large left pleural effusion with total collapse of the left lower lobe, as well as a right kidney lesion. Subsequent imaging demonstrated a left lower lobe mass (3.4 cm) with numerous left-sided pleural-based nodules and one pleural-based mass (4.1 cm), with imaging characteristics concerning for metastatic disease (Figure 1). CT abdomen and pelvis with contrast showed a solid hyperdense mass in the mid pole of the right kidney (Figure 2). PET scan showed numerous hypermetabolic left pulmonary nodules, most consistent with pleural metastasis, including diffuse hypermetabolic pleural thickening throughout the left hemithorax and multiple hypermetabolic pleural-based nodules. PET scan also showed a solid right renal lesion (2.8 cm) with low-grade FDG uptake most suggestive of renal cell carcinoma.
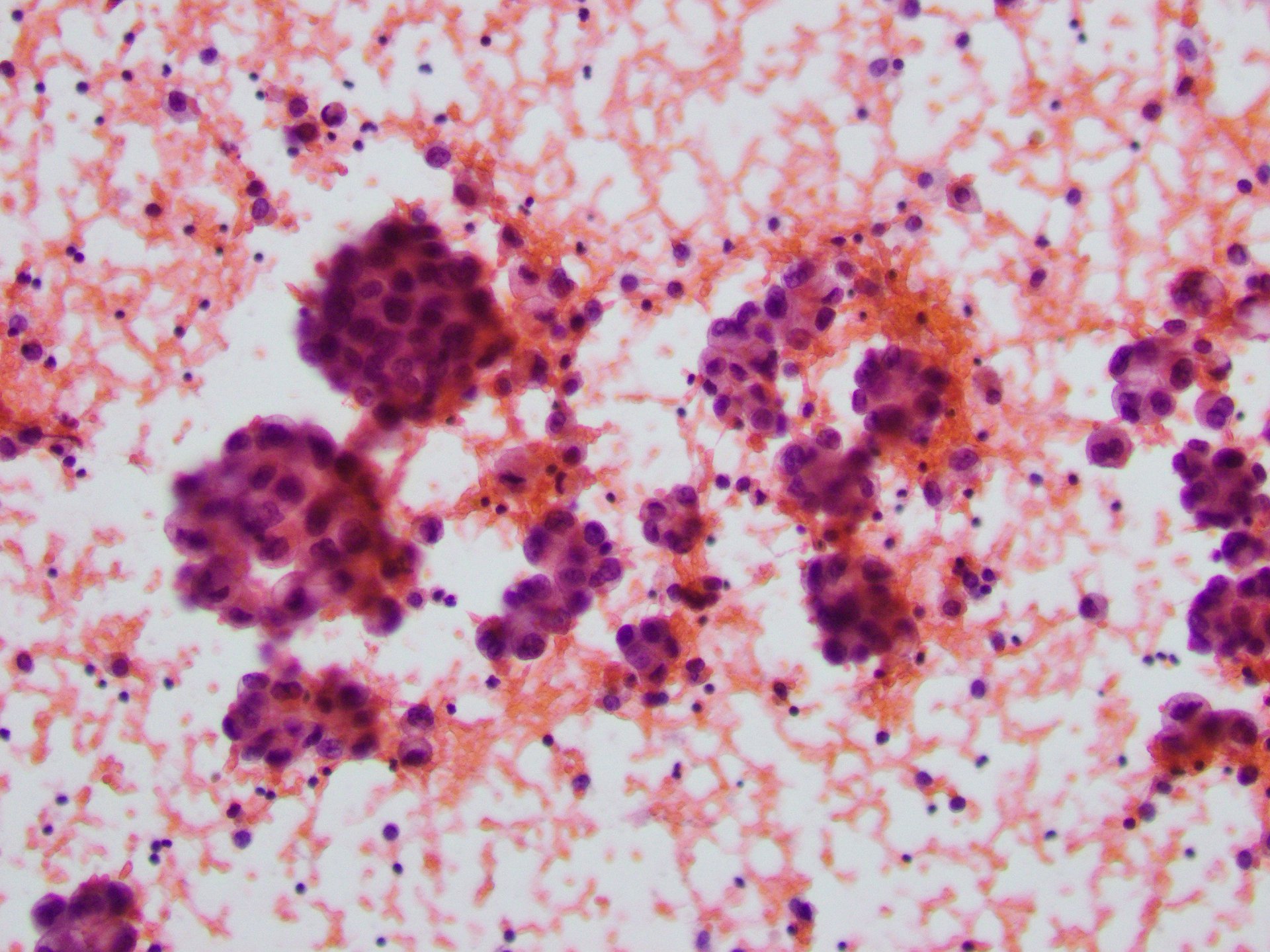
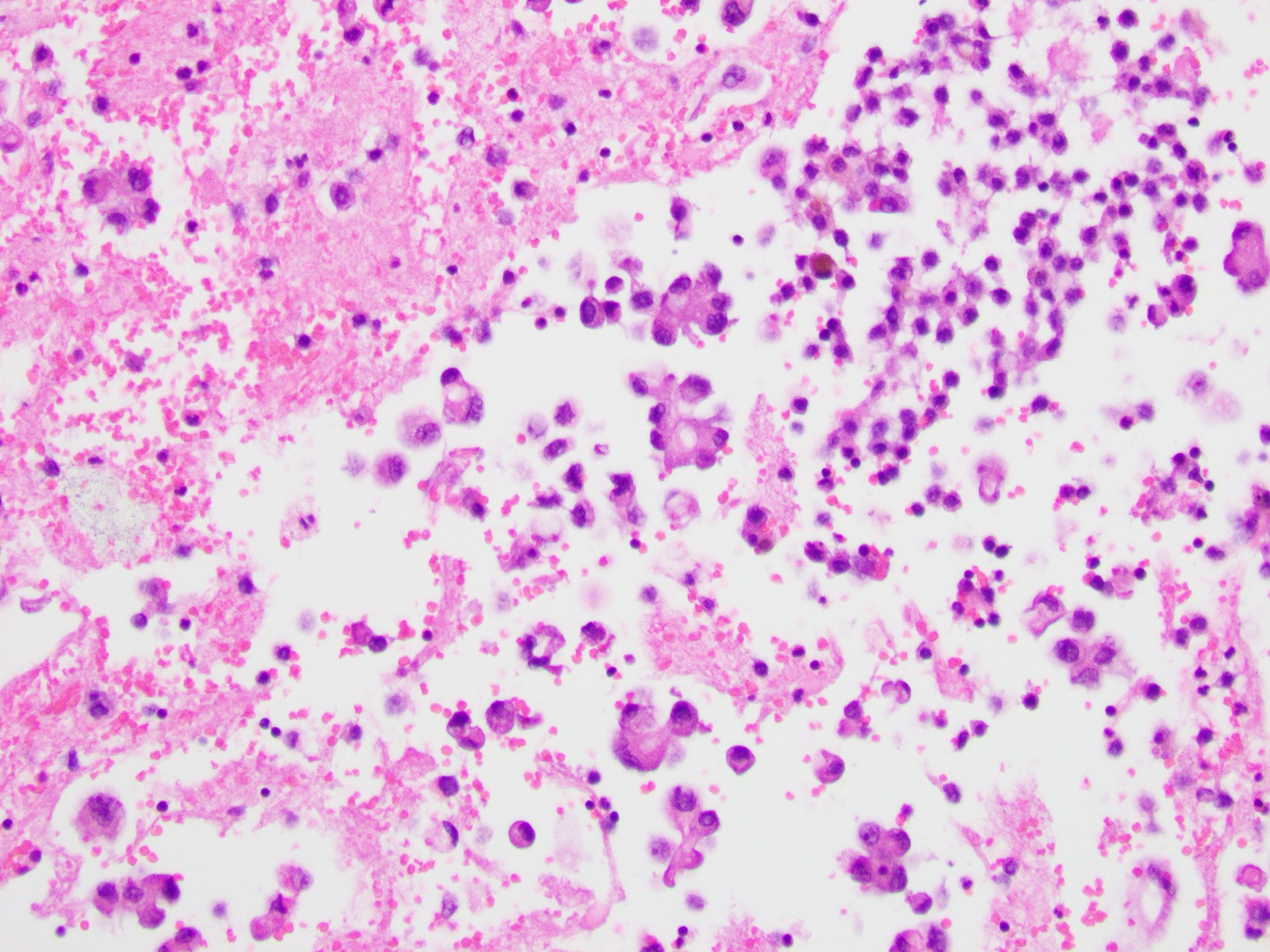
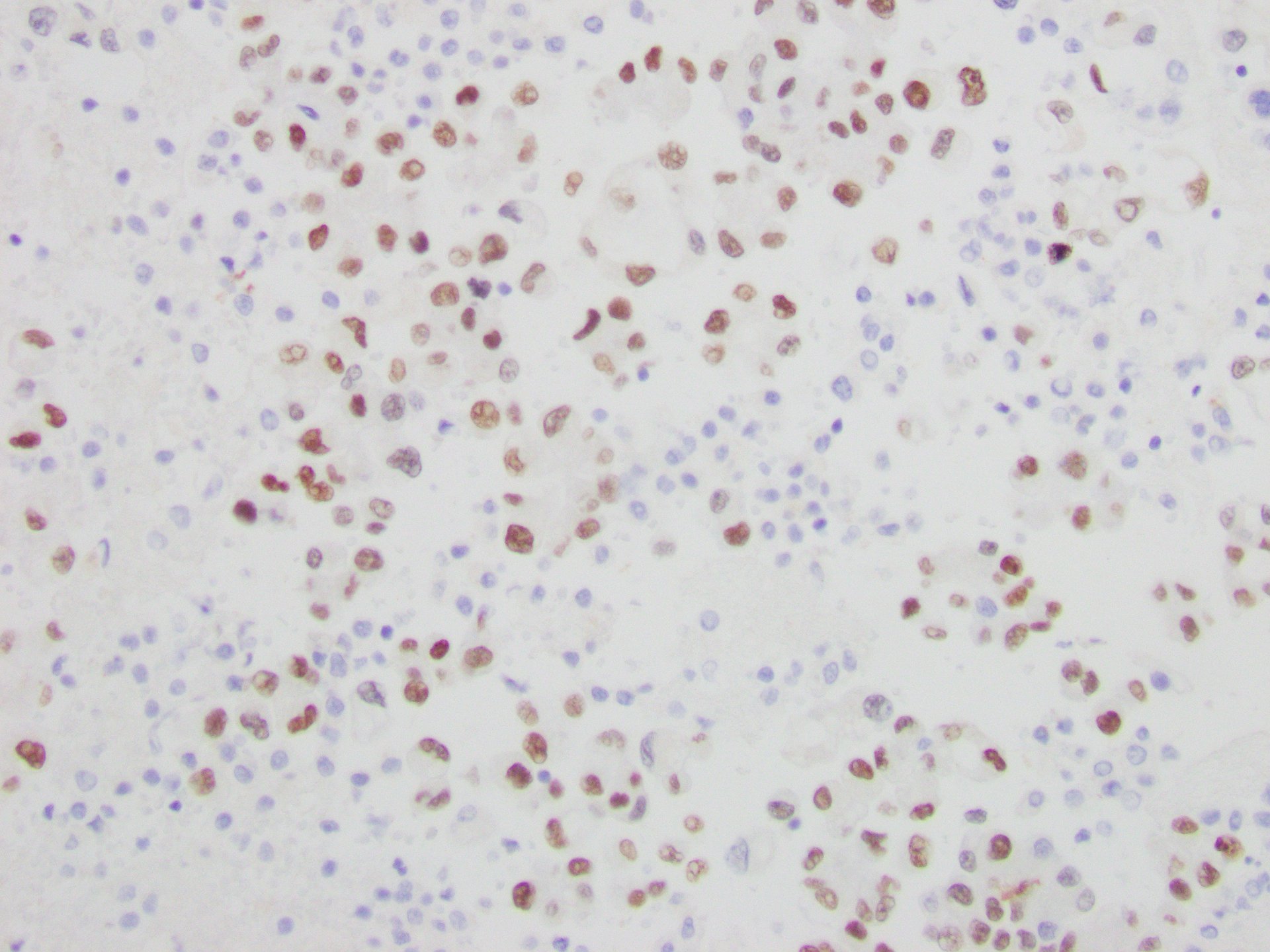
Pleural fluid demonstrated clusters of tumor cells with a high nuclear:cytoplasmic ratio, prominent nucleoli, and granular cytoplasm, consistent with adenocarcinoma (Figures 3 and 4). Immunohistochemical stains showed that the tumor cells were positive for TTF-1 (Figure 5) and Napsin A staining, supporting the diagnosis of pulmonary adenocarcinoma.
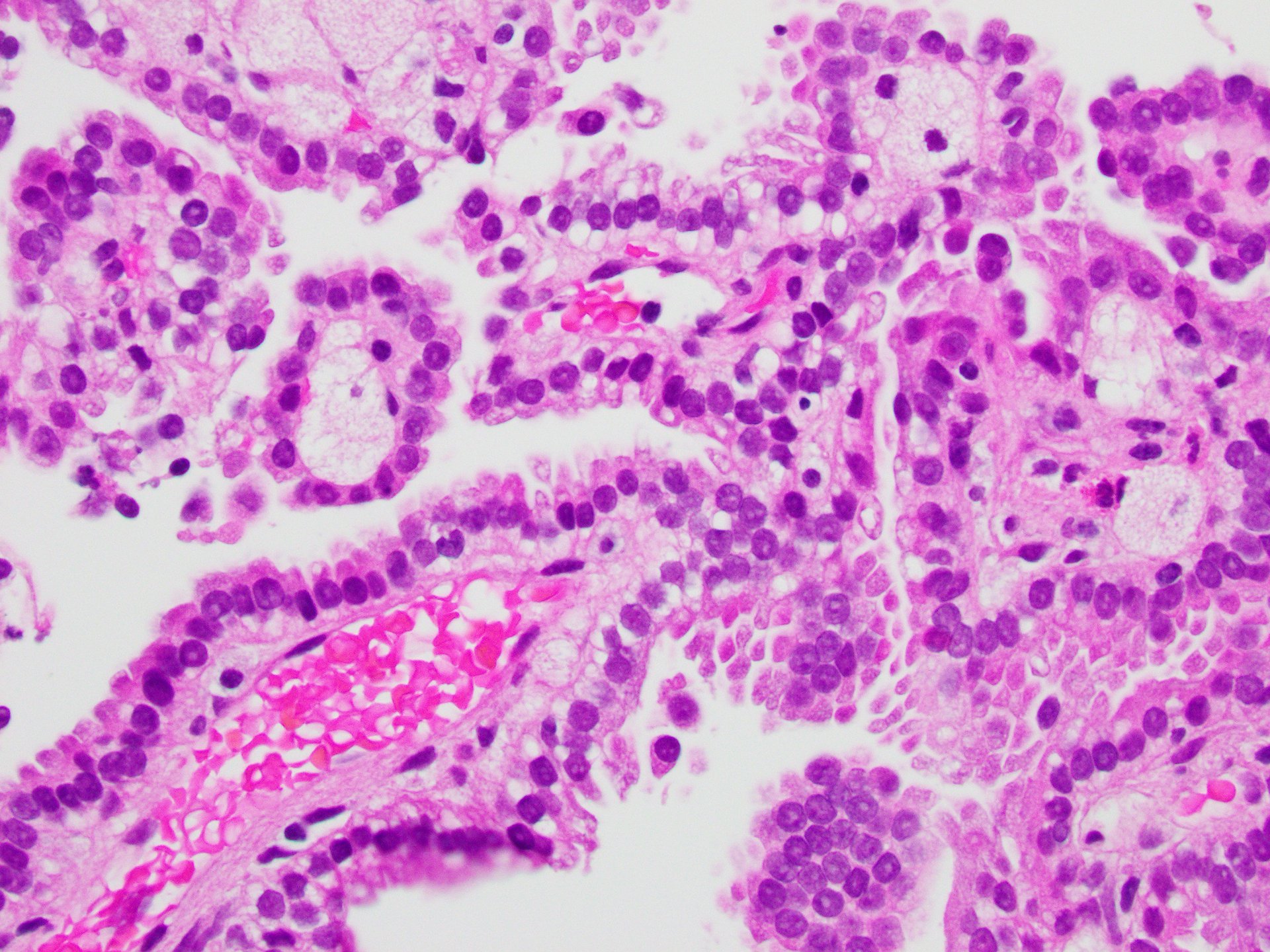
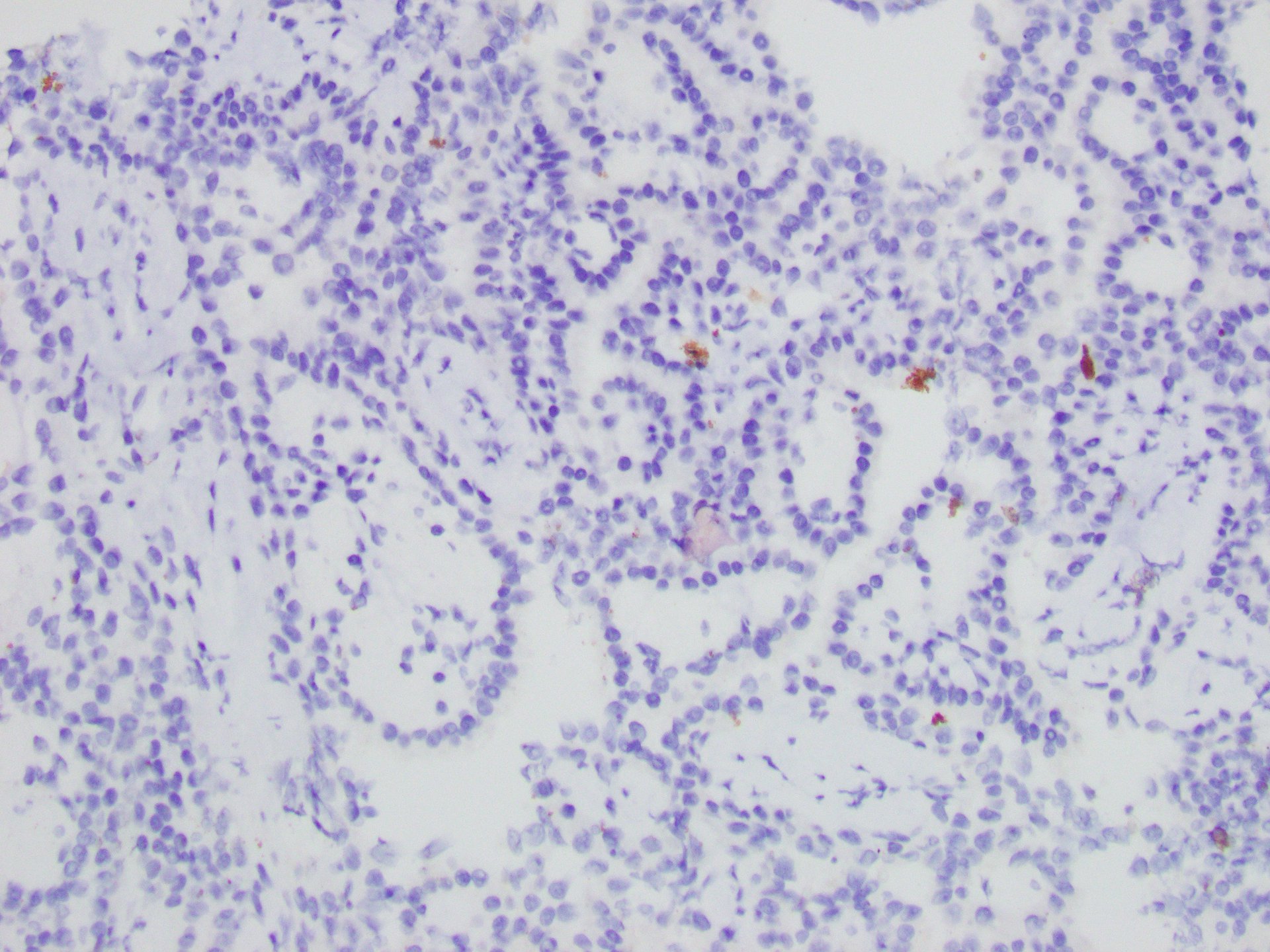
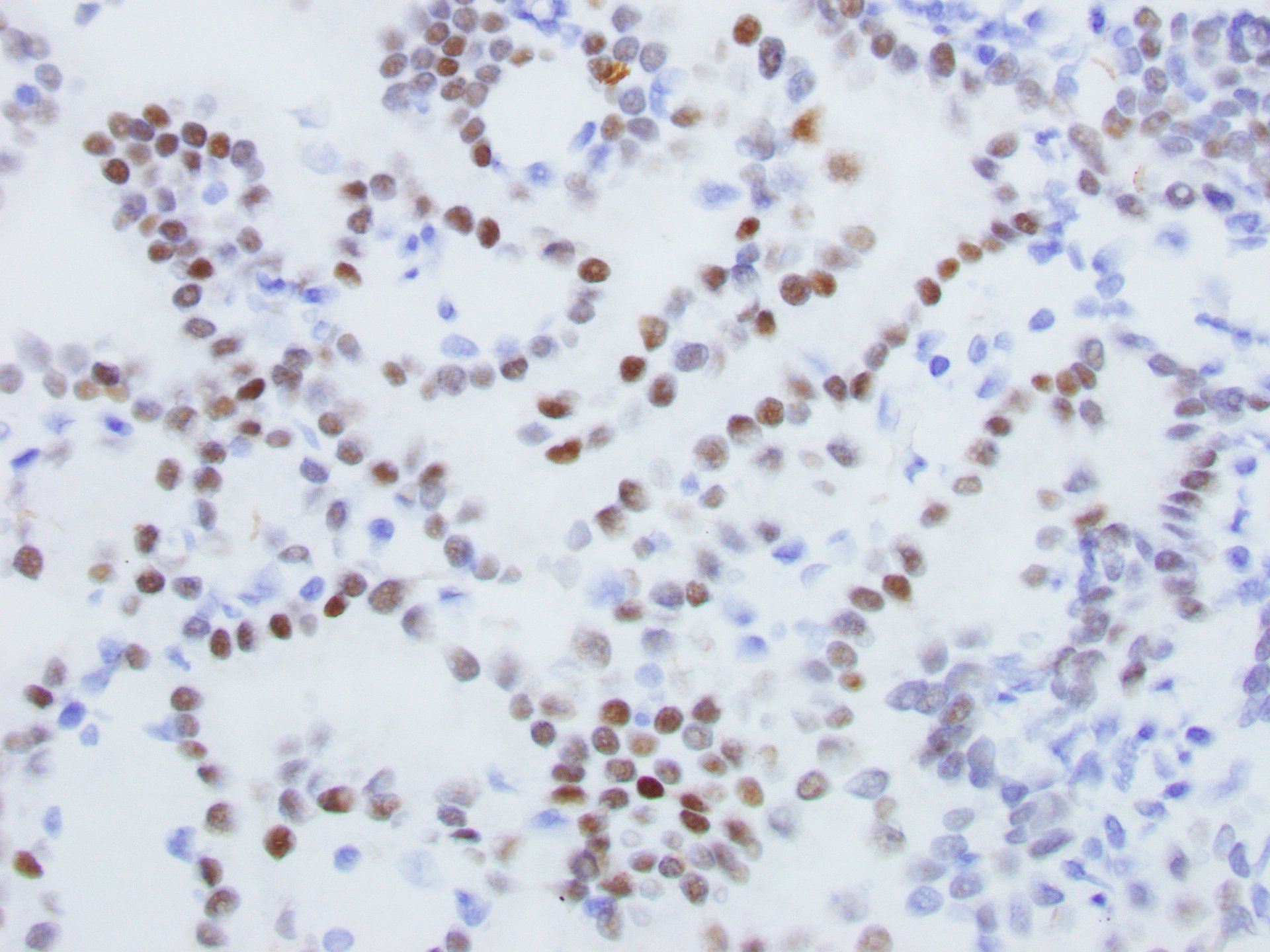
The right kidney core biopsy demonstrated relatively uniform neoplastic cells arranged in papillae with fibrovascular cores and foam cells. Immunohistochemical stains showed that the renal tumor cells were positive for PAX-8 (Figure 6) and negative for TTF-1 (Figure 7) staining, supporting the diagnosis of primary papillary renal cell carcinoma and not metastatic lung adenocarcinoma.