Results of STAR-NY
Results of STAR-NY
Successes of STAR-NY
- Provided the first complete snapshot of current stroke care practice, intervention rates and discharge outcomes in Rochester, NY STAR-NY has created the first ever mechanism for data/outcomes collection, sharing and comparative analysis across multiple healthcare institutions.
Current Results
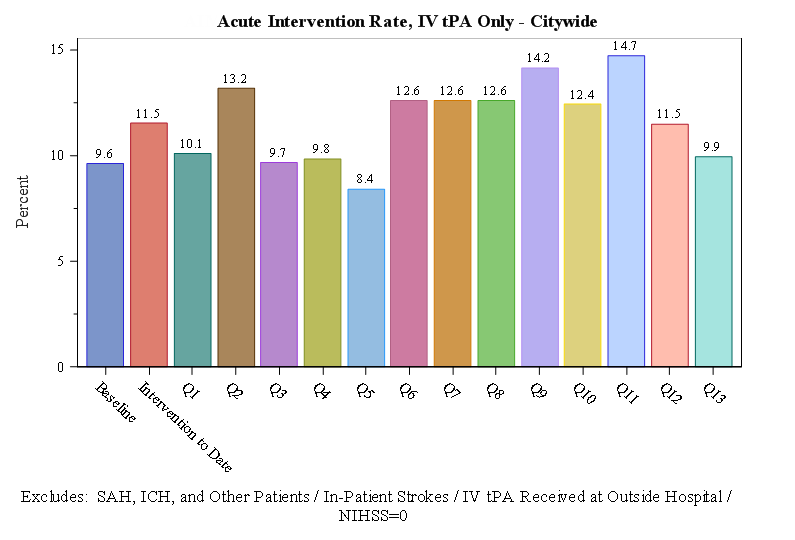
- Established a trajectory of increasing rates of acute intervention for acute stroke across the community (11.2% at baseline to 15.2% over entire intervention phase).
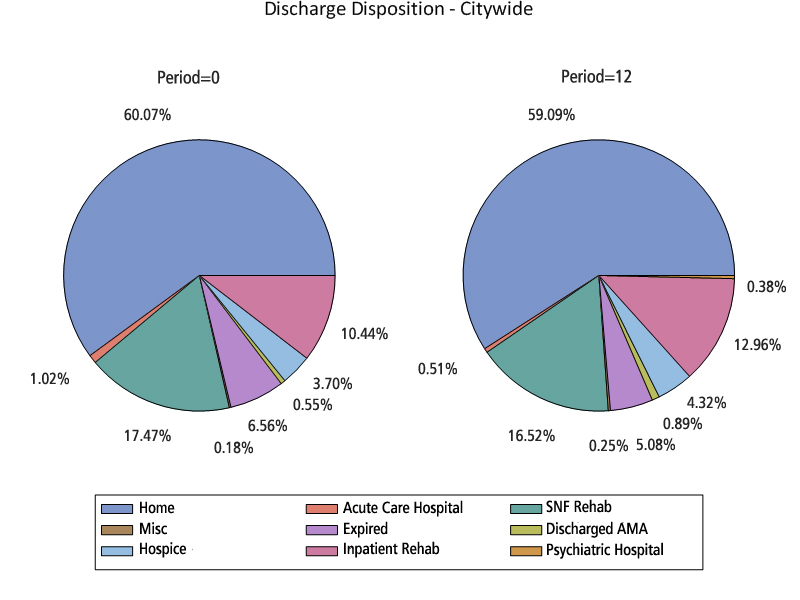
- Increase in rate of patient discharge to home (53% in baseline to 61% by end of 2012) without change in median length of in-hospital stay for acute ischemic stroke and TIA.
- STAR-NY has created a renewed focus in the community for increasing secondary stroke prevention rates for patients after first stroke/TIA.
Current & Future Efforts
- Expand focus from care processes to include physician practice patterns.
- Target populations for increased intervention (IV and/or IA):
- Patients arriving within tPA window but excluded based upon historically relative contraindications (which the AHA has now recognized as reasonable to treat - 2013 recommendations - primarily focusing on patients with low stroke severity and rapid improvement in stroke symptoms) - could account for 6% potential increase in acute intervention rates.
- Patients who are eligible candidates for endovascular treatment; those arriving within 4.5 hours but not eligible for IV tPa (7.0%), those arriving outside tPA window (>4.5 hours) but less than 8 hours of onset (8.3%) and those arriving with an unknown time of onset (4.4% assuming 10% of these patients are eligible based on imaging) = could account for potential 19% increase in acute intervention rates.
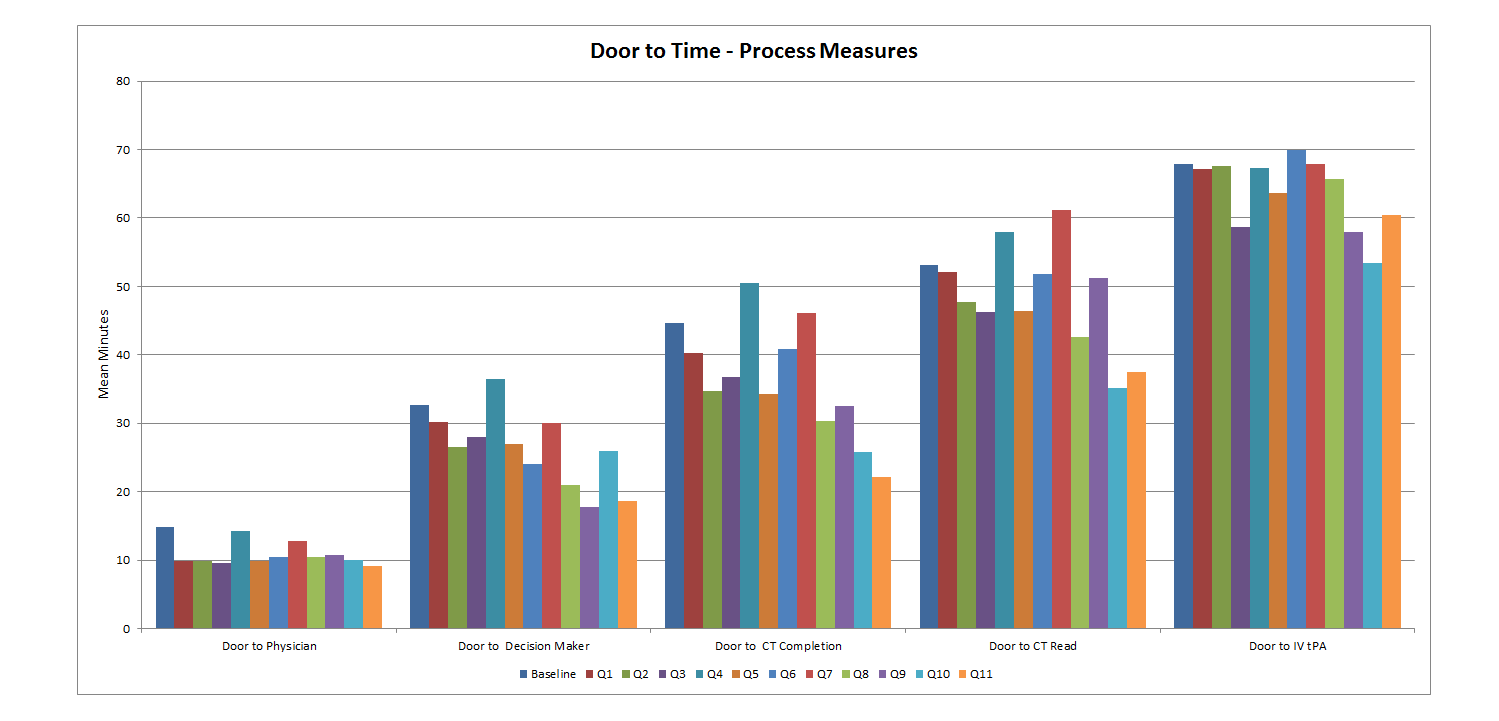
The following tables and graphs represent the most up to date STAR-NY results.