Double Helix Curriculum—Translations and Transitions
Double Helix Curriculum—Translations and Transitions
Over four years, the “Double Helix Curriculum—Translations and Transitions” teaches the scientific foundations and clinical medicine and how they translate to exceptional care. The scientific foundations of medicine over the four phases of the DHC-TT include basic, social, and informational sciences. Earlier in the curriculum the basic sciences are emphasized and as the curriculum progresses, the social and informational sciences become the more prominent scientific foundations content. Students develop communication and clinical skills quickly with our early clinical exposure. Drawing upon the University motto of “Meliora—ever better”, Meliora in Medicine is a curriculum thread across the four years that includes our Medical Humanities and three content pillars: Collaborative Practice, Technology in Medicine, and Professional Identity Formation. Ample elective time enables each student to tailor their experiences to meet educational and career goals. Guided by our educational program objectives (see below) and emphasizing Rochester’s Biopsychosocial Model, we educate and train outstanding physicians who are prepared to practice medicine caring for all patients in a dynamic, changing healthcare environment.
Using an iPad delivery platform, instructional methods include Problem Based Learning, Team Based Learning, large and small group skills sessions. Standardized patients and simulation provide direct hands on experiences. Clinical options in urban, rural, ambulatory and inpatient settings provide rich, broad clinical experiences.
The Double Helix Curriculum—Translations and Transitions highlights and facilitates the transition of accepted applicant to medical student to physician entering graduate medical education. Our Advisory Dean program provides students with access to a myriad of resources, academic and career counseling, wellness and resilience, and professional development. Facilitating the transitions begins with orientation and continues with defined activities throughout the curriculum culminating in our specialty specific competencies and capstone course in the final phase.
Our graduates are successful in careers encompassing academic medicine, rural medicine, research, administration, and community advocacy.
Educational Program Objectives
- Embody the Biopsychosocial model by integrating the foundational scientific knowledge of medicine with the personal, cultural, and social aspects of the patient in providing care and individualized education. (BPSM-1)
- Understand human structure, function, and development from molecular through cellular, organ system, and whole person levels.(NSS-1)
- Identify determinants of health and illness including psychological, interpersonal, familial, cultural, societal, and environmental factors, with attention to the impact of inequities and discrimination, in the care of all individuals and populations. (NSS-2)
- Recognize how disease processes can lead to or be caused by alterations in human structure and function, with an understanding of their epidemiology, etiology, pathogenesis, and pathology. (D-1)
- Apply the scientific principles underlying rational approaches to health promotion and disease prevention. (T-1)
- Apply the scientific principles underlying rational approaches to diagnostic, therapeutic, rehabilitative, and palliative interventions. (T-2)
- Recognize and critically evaluate the structural and organizational frameworks -and their interactions- within which health care is provided at global, national, and local levels. (SC-1)
- Recognize and apply the principles underlying approaches to providing high quality, safe, ethical, and high-value person-centered care. (SC-2)
- Understand the scientific method and the basic scientific and ethical principles of clinical and translational research, including the ways in which such research is conducted, evaluated, explained to patients, and applied to patient care. (TSM-1)
- Demonstrate under direct observation the ability to evaluate patients, including history and examination skills. (PE-1)
- Synthesize clinical findings to guide selection and interpretation of diagnostic tests including laboratory and imaging studies. (PE-2)
- Demonstrate the ability to communicate and collaborate with diverse patients and families, including the ability to listen empathetically and provide effective patient education. (C-1)
- Demonstrate the ability to collaborate with fellow students, physicians, and other health professionals using effective verbal and written communication. (C-2)
- Demonstrate the ability to communicate and collaborate with community-based organizations and health-related agencies. (C-3)
- Synthesize a clinical case and develop a prioritized differential diagnosis with a strategic plan for evaluation and management at a level required for entry into internship. (CRM-1)
- Exhibit intellectual curiosity by identifying personal knowledge gaps and retrieving, appraising and applying evidence to address those gaps. (IS-1)
- Exhibit a commitment to lifelong learning to improve individual medical practice and systems of care. (IS-2
- Understand the factors that influence one’s own health and well-being, demonstrate resilience by using healthy coping mechanisms in response to stress, and contribute to the health and well-being of peer professional communities. (IS-3)
- Develop an understanding of the utility and limitations of health-related technologies in patient care. (IS-4)
- Demonstrate the exemplary attitudes and humanistic behaviors expected of physicians, including integrity, reliability, compassion, accountability, ethical conduct, respect, anti-racism, cultural humility, selfless advocacy for patient and population health and appropriate management of potential conflicts of interest. (PH-1)
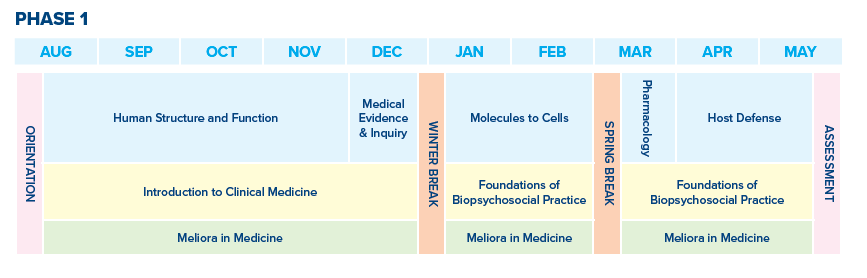
Phase One
Human Structure and Function. HSF is a 14‐week course that begins in August after student orientation. It is an integrated course that teaches gross anatomy, histology, embryology, and physiology. The course is taught through lectures, large group interactive discussions, small group problem based learning, laboratory experiences (gross anatomy, physiology and histology), and physiology problem set groups. Assessment is done through multiple choice and practical examinations and PBL performance.
Introduction to Clinical Medicine. ICM occurs during the first 18 weeks of Phase 1. Students learn skills of information acquisition in the clinical setting—the patient interview and physical exam with a focus on learning foundational skills. Applying principles of the Biopsychosocial Model, students interact with a group of standardized patients and scenarios, preparing them for the clinical courses that follow. Taught through lectures, live demonstrations, and small group instruction, students interact with standardized patients throughout the course. HSF and ICM are organized to align learning anatomy and physiology of specific body systems with relevant history and physical examination skills. Assessment in ICM is done through multiple choice exams, faculty observed performance in small group and summative SP encounters.
Medical Evidence & Inquiry. MEI is a 3-week course that provides opportunity for learners to develop and enhance their knowledge, skills, and experience with finding, evaluating, integrating, and communicating medical evidence into the process of patient and population level clinical reasoning. Course content spans biostatistics, epidemiology, translational medicine, research ethics, clinical testing, and population/public health topics. MEI provides a foundation for subsequent courses and clerkships in the URSMD curriculum and the practice of medicine. Assessment is done through multiple choice examinations and PBL/small group performance.
Molecules to Cells. MTC starts the second semester of Phase 1 continuing with the basic science strand. Providing foundations in biochemistry, genetics and cell biology curriculum, this nine-week course teachings through lectures, problem based learning cases and large group patient encounters. It is organized into seven theme blocks: biochemical basics and systems integration; intermediary metabolism; molecular genetics and cell biology; cell growth control, development, cancer and aging; medical genetics; genetic-‐ environmental interactions; nutrition. Assessment is done through multiple choice examinations and PBL performance.
Foundations of Biopsychosocial Practice. FBP is a 19-week course where students build on the history taking and physical examination skills learned in Introduction to Clinical Medicine. Designed to provide opportunities to practice the complete history and physical examination on patients across the lifespan from infants to older adults in a variety of care settings, this course includes outpatient primary care inpatient hospital settings, and rehabilitation clinics/units. The second half of the course focuses on wellness, prevention and health behavior counseling and provides students with hands-on practice honing interviewing skills with both actual and simulated patients. The course integrates aspects of both clinical practice and basic science and build upon concepts learned in Introduction to Clinical Medicine. Assessment is done through examinations, small group performance and clinical performance.
Pharmacology. Pharm is a two-•‐week course that teaches students the basic principles of pharmacokinetics, pharmacodynamics, and pharmacogenetics. Through lectures, large and small group discussion of case studies, and a human simulator exercise, students learn to apply these principles to select areas of clinical medicine including autonomic pharmacology, antihypertensive medicines, cancer chemotherapy, anesthetics, and drugs used for treating diabetes. The course provides students a strong foundation on which to build their knowledge of other important areas of pharmacology taught in subsequent courses. Assessment is done through a multiple choice exam and performance in simulation and problem sets.
Host Defense. HD is the final basic science course of Phase 1. This eight-week course introduces microbiology, immunology, inflammation, and pathology. Key topics within microbiology include: bacteriology, virology, mycology, antimicrobial pharmacology, and parasitology. The course is taught through lectures, problem based learning cases, and independent exercises. Assessment is done through multiple choice practical examinations, performance on independent exercises, and PBL performance.
The Phase 1 Assessment is a multi-day experience that emphasizes the integration of medical knowledge, communication, synthesis of information, and professionalism. Distinct from other aspects of the curriculum, the Phase 1 Assessment is designed to provide students with formative feedback on their knowledge, skills and attitudes as a physician in training through a series of structured activities including: standardized patient encounters, physical examination sessions, mock board examinations, written-assignments, self-reflection exercises, small group experiences, and multi-source feedback. The Phase 1 assessment culminates in the creation of an Individual Development Plan to guide students’ personal, professional, and career development goals.
Meliora in Medicine. The MiM course includes a longitudinal component during the 1st and 2nd phase, and a thread throughout all 4 phases of the curriculum based on Health Systems Science and three pillars: Collaborative Practice, Technology in Medicine, and Professional Identity Formation. Drawing upon the university motto of Meliora (ever better), MiM prepares students to flourish in the dynamic practice of medicine by developing their abilities to collaborate effectively in teams, work with other professions represented in team based care and incorporating emerging technologies such as telemedicine and ultrasound. MiM is anchored in Health Systems Science content and students are exposed to Patient Safety/Quality, Social Determinants of Health, and Team Science. The course integrates with and enhances the foundational science and clinical curriculum. Emphasis is made to foster the development of students’ professional identities. In addition to the three pillars, the course engages students and promotes thinking and reflection beyond the sciences to the human contexts and relationships involved in caring for all patients and families. The Medical Humanities & Bioethics thread further expands students' abilities to attend fully with patients and families while providing foundational humanistic and ethical learning.
Health Humanities Selectives. Students select two Health Humanities Selectives during the first two phases (one in the second semester of Phase 1 and one in the first semester of Phase 2). Representative topics include bioethics and law, philosophy, medical history, visual arts, literature and narratives in medicine, disability, spirituality, social and environmental perspectives in healthcare, complementary and alternative medicine, national healthcare reform, Latino health, deaf health, and others.
Phase Two
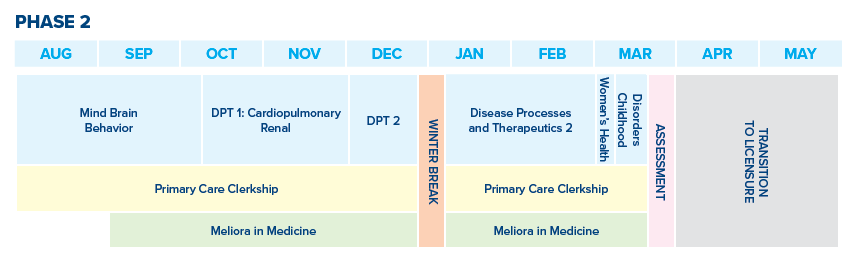
Mind/Brain/Behavior. MBB is a nine-week course that introduces the principles of neuroscience, neuropathology, neuropharmacology, psychopathology, and psychopharmacology. Nine PBL cases integrate these basic sciences with the clinical disciplines of neurology and psychiatry. In addition, fourteen laboratory and team-based learning sessions reinforce neuroanatomy, neuroradiology, and neuropathology through gross brain dissections and a review of neuroimages, gross and microscopic pathologic specimens, and direct application of neuroscience content to clinical cases. Assessment is done through multiple choice and practical examinations and PBL performance.
Primary Care Clerkship. PCC offers students the opportunity to practice skills learned during Phase 1 clinical strand coursework (ICM and FBP). It is a 31-week longitudinal clerkship based in the ambulatory clinical setting, where working with physicians in internal medicine, family medicine, and/or pediatric ambulatory practices is supplemented with interactive large and small group clinical skills sessions. On average, students are scheduled for PCC activities three afternoons per week. Physical diagnosis sessions early in Phase 2 reinforce and build upon earlier learning of the physical exam, with attention to identifying and interpreting abnormal findings. Other classroom activities focus on health prevention and management of acute and chronic illnesses, organized around common presenting concerns (e.g. chest pain), and presented in the context of organ system pathophysiology being taught in DPT (e.g. cardiovascular system). Assessment methods include preceptor evaluations, course quizzes, standardized patient encounters, graded clinical notes, and the NBME Customized Assessment.
Disease Processes & Therapeutics. DPT Disease Processes and Therapeutics (DPT) are two separate systems based courses that integrate the pathology, pathophysiology, and pharmacology of human disease over 17-weeks. The first course, DPT: Cardiopulmonary-Renal Interrelationships teaches pulmonary, cardiac and renal pathophysiology and their interrelationships. The blocks in DPT 2 consist of infectious diseases, gastroenterology and hepatology, rheumatology, hematology and endocrinology. All block include pathophysiology instruction integrated pathology and pharmacology. Instruction methods in these courses include lectures, problem based learning, team based learning, patient, simulation and laboratory experiences. Assessment is done through multiple choice and short answer examinations and PBL performance.
Women’s Health Course. WH is a two-week course that follows DPT and provides a foundation for understanding female reproductive disorders across the life stages with a reproductive justice lens. Each topic is approached by reviewing the normal state before exploring the disorders and differences. Topics covered include sexual development, puberty, menstruation, reproduction, pregnancy, gynecologic disorders, breast disorders and menopause. Topics are explored using flipped classroom exercises, lectures, pathology labs; team based learning exercises and a simulation experience for labor and delivery. Students perform self-assessment through multiple choice questions provided on each topic and complete a comprehensive NBME Customized Assessment.
Disorders of Childhood. DoC is a 2-week course focusing on conditions and illnesses that specifically present in, are confined to, or manifest differently in childhood. Using a systems-based approach, the course focuses on increasing knowledge of important diagnoses as well as understanding key concepts related to how growth and development, embryonal through adolescence, impacts the occurrence and presentation of disorders, treatment decisions, and long-term outcomes. Team based learning, small and large group interactive sessions, and a congenital heart disease lab complement the lectures. Assessment is via a multiple-choice exam at the end of the course.
The Phase 2 Assessment is a multi-day experience that emphasizes the integration of medical knowledge, communication, synthesis of information, and professionalism. Distinct from other aspects of the curriculum, the Phase 2 Assessment is designed to provide students with formative feedback on their knowledge, skills and attitudes as a physician in training through a series of structured activities including: standardized patient encounters, physical examination sessions, mock board examinations, written-assignments, self-reflection exercises, small group experiences, and multi-source feedback. The Phase 2 assessment culminates in the creation of an Individual Development Plan to guide students’ personal, professional, and career development goals.
Transitions to Licensure. Transitions to Licensure is a six-week independent study course to provide Phase 2 students with unscheduled, independent study time to prepare for and successfully pass Step 1, which is compulsory for progressing to Phase 3 of the curriculum. Student success in Transitions to Licensure is maximized with a defined study plan, close monitoring of student progress, and modifications based upon assessments of progress. Assessment includes a reflection on life-long learning skills and self-directed learning.
Phase Three
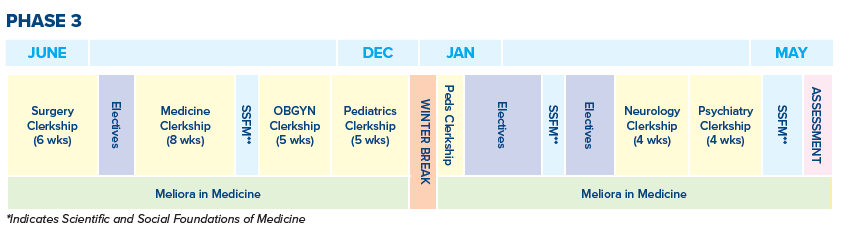
Three clinical clerkship blocks together have six required experiences in Phase 3. These are:
Adult Inpatient Medicine:Medicine and Surgery
Mind Brain Behavior:Neurology and Psychiatry
Women and Children’s Health: Obstetrics and Gynecology and Pediatrics
Three Scientific & Social Foundations of Medicine (SSFM) one-week courses are linked to each of the three clinical blocks. Each SSMF includes case conferences, lectures, laboratories, and self‐study to teach advanced topics related to corresponding clinical specialties.
Adult Inpatient Clerkship: Medicine and Surgery
Internal Medicine. The medicine clerkship is eight weeks long, and consists of one education week followed by seven weeks of inpatient internal medicine. The goal is to give a broad experience in the evaluation, diagnosis, and management of hospitalized adults. During the education week, students attend a number of workshops and conferences, and have time for independent study for completion of virtual assignments. During the first three weeks of their seven clinical weeks, students meet in groups of three or four with a faculty preceptor twice a week to present and discuss cases, and have student focused bedside teaching with hospitalized patients. Students typically rotate through two or three inpatient teams and/or sites during the clerkship.
Surgery Clerkship. The six-week surgery clerkship is one component of the adult inpatient experience. The surgery clerkship, in the double helix curriculum, achieves established goals and objectives by conducting a series of conferences and presentations, which address the core curriculum. At the same time it is important to maintain the apprenticeship type learning environment, which is essential for the achievement of clinical competence. Students are expected to attend both the team’s clinics and operative procedures. This experience provides students an overview of the diagnosis, treatment and management of surgical conditions.
Scientific & Social Foundations of Medicine: Principles of ICU Science and Ethics (POISE). The POISE Course is an integrated approach to teaching the material that bridges the medical sciences and clinical medicine, which are the foundations of medicine and surgery. Critical Care Medicine is the core topic used to develop the above principles.
Mind Brain Behavior: Neurology and Psychiatry
Psychiatry Clerkship. Psychiatry is a four-week experience that provides broad teaching about clinical psychiatry with focused clinical experiences in a particular area. The student works with a preceptor, and the clinical site placement may be inpatient psychiatry in adult, child and adolescent, forensic, or geriatric services; emergency psychiatry; child and adolescent partial hospitalization; or consultation/liaison psychiatry in adult or pediatric services.
Neurology Clerkship. This clerkship is a four-week introduction to clinical neurology that builds upon the second year Mind, Brain and Behavior course. The clerkship consists of two 2‐week experiences on the various inpatient adult and child neurology services at Strong Memorial Hospital and Highland Hospital. Students work as integral members of the patient care teams and are closely supervised by neurology residents, fellows and attending physicians.
An integrated seminar series is required of all students on both psychiatry and neurology across the eight weeks.
Scientific & Social Foundations of Medicine: Mind, Brain and Behavior. The Mind, Brain and Behavior II Basic Science Course provides an advanced perspective of how basic science research contributes to the practice of clinical neurology and psychiatry. The overriding theme is “Development, Degeneration, and Dysfunction: A Life-Long Balance Influencing Brain Function”.
Women and Children's Health: Obstetrics and Gynecology and Pediatrics
Obstetrics and Gynecology Clerkship. This five-week clerkship is designed to provide the third year medical student with solid foundational knowledge in the diagnosis and management of common obstetric and gynecologic conditions as well as preventive medicine for this patient population, regardless of the student's future specialty. This Clerkship provides clinical exposure and experience to obstetric and gynecologic physiology and pathophysiology. Students will evaluate and provide care for patients in the inpatient environment or in both the inpatient and the outpatient environment. Students will perform supervised breast and pelvic examinations and develop skills in assessing and managing the obstetric and gynecologic patient, from taking the specialty-specific history to developing the care plan. Students will also participate in the operating room as assistants and will attend vaginal and cesarean births.
Pediatrics Clerkship. This five‐week clerkship provides students a breadth and depth of exposure to pediatric medicine. Students spend the core of their time on inpatient pediatric services with ward and newborn nursery teams. The balance of time is devoted to pediatric sub-specialty and acute ambulatory experiences.
Scientific & Social Foundations of Medicine: Genes, Ecology, & Culture (GEC). Evolutionary biology provides the basis of our understanding of both the function an organism and its relationship with its physical, social and biotic environment. GEC explores evolutionary principles, such as epigenetic mechanisms, life history theory and evolutionary-developmental biology and applies these principles to our understanding of the impact of climate change on health, reproduction, nutrition and metabolism. In addition, GEC examines our cultural evolution in ethics, law, public policy and technology impacts our biological evolution.
The Phase 3 Assessment is a multi-day experience that emphasizes the integration of medical knowledge, communication, synthesis of information, and professionalism. Distinct from other aspects of the curriculum, the Phase 3 Assessment is designed to provide students with formative feedback on their knowledge, skills and attitudes as a physician in training through a series of structured activities including: standardized patient encounters, physical examination sessions, mock board examinations, written-assignments, self-reflection exercises, small group experiences, and multi-source feedback. The Phase 3 assessment culminates in the creation of an Individual Development Plan to guide students’ personal, professional, and career development goals.
Phase 3 or Phase 4
Students are required to complete:
Emergency Medicine. In this four-week experience, students gain experience evaluating undifferentiated adult and pediatric patients in a high volume, Level I Trauma Emergency Department. Exposed to stabilization of adult/pediatric emergent conditions, pre‐hospital care of patients, and procedures related to care of these patients, student education also includes simulation, ultrasound and procedural skills sessions.
Family Medicine. This primary care specialty provides first contact, ongoing, and preventive care to all patients regardless of age, gender, culture, care setting, or type of problem. The 4-•‐week experience will give students an opportunity to understand how context influences the diagnostic process and management decisions. Students learn the fundamentals of an approach to the evaluation and management of frequently occurring, complex, concurrent and ill-defined problems across a wide variety of acute and chronic presentations. Over the four weeks, students study the principles and methods of Family Medicine in a primary care setting and learn essential patient care knowledge and skills necessary for general medical school development, regardless of ultimate career choice.
Surgical Subspecialty - These two weeks can be done in phase 3 or year 4. This selective is focused on understanding and participating in one aspect of the team that cares for the surgical patient (general or subspecialty surgery, anesthesia, surgical pathology).
Phase Four
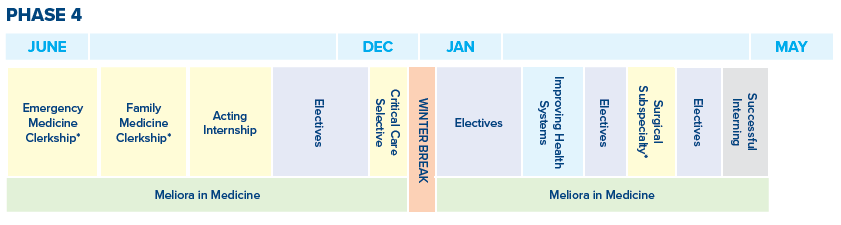
Acting Internship – This required four-week experience can be completed in either Family Medicine, Medicine, Surgery, Pediatrics, Obstetrics and Gynecology, Emergency Medicine, or Neurology as well as intensive care settings. Students are given greater responsibility in the care of hospitalized patients that replicates an intern’s experiences and skill sets.
Critical Care Selective—Choosing between a two-week experience in intensive care or anesthesia, students are actively involved in the management of patients with multi-organ health problems, recognizing the role interplay of healthcare teams in these settings. Intensive care unit opportunities include medical, surgical and neurology ICUs. Those choosing the anesthesia experience refine airway and hemodynamic management skills.
Improving Health Systems (IHS) is a three-week course that presents, through a series of lectures, guided self-study and facilitated small group sessions, how an evolving third pillar of medical education (Health Systems Science) changes clinical care and the systems of care. Emphasis is placed on the relationships with value-based care, non-clinician/community partners and the translation to improved patient safety and quality. Students work in groups, by their planned medical specialty, to develop and present a research plan that addresses how a clinical problem could be addressed through quality improvement and/or implementation science initiatives.
Successful Interning SI is a two‐week capstone course prior to graduation. Large group sessions on topics relevant to the transition to internship are complemented by small group sessions, which students select from a variety of offerings. Small group sessions are case‐based and highly interactive to promote active, learner‐ centered learning of topics and skills focused on internships. Students also attend a one-day boot camp session in one or more of the following specialties: Emergency Medicine, Family Medicine, Medicine, Obstetrics & Gynecology, Pediatrics, or Surgery.
Meliora in Medicine is a course in the first two years and a thread throughout the four years of the Double Helix Curriculum: Transitions and Translations. Including Medical Humanities, the thread emphasizes three pillar content areas, each with specific topics and activities occurring at developmentally appropriate times in the curriculum.
Health System Science | Technology in Medicine | Professional Identify Formation |
Health Care Policy and Economics | Electronic Medical Record | Bioethics |
Interprofessional Education and Teamwork | Ultrasound | Wellness and Resilience |
Patient Safety/Quality | Telehealth | Unconscious Bias |
Social Determinants of Health |
| Advocacy |
Elective Pathways are mentored programs that run-in conjunction with the Double Helix Curriculum—Translations and Transitions. Pathways provide students opportunity to work with like-minded students and faculty to explore nuances, address needs of underserved, create curriculum, institute policy, and explore entrepreneurship. We offer seven different elective pathways:
Deaf Health Pathway
For students with interests in the health, language and culture of the Deaf community, this student-centered curriculum provides an appreciation for the health disparities between the Deaf community and the general population and greater awareness of unique Deaf health needs. Drawing on the large Deaf population in Rochester, this pathway provides engagement with the community with linguistic and cultural immersion to prepare graduates to better care for Deaf patients.
Global Health Pathway
Students gain additional knowledge and skills in the health problems and solutions of populations that transcend socioeconomic and ethnic status and national borders. Didactic lecture series, direct experience and an independent project complement volunteer work and patient interactions to foster compassion and appreciation for the plights of underserved populations. Participants develop a deep understanding of global health advocacy, appreciating the role of the physician as an agent for change in local and international communities.
Health and Incarceration Pathway
The Health and Incarceration Pathway (HIP) develops the student’s deeper knowledge and skills in the care of patients with a history of incarceration and other criminal legal system involvement. Participants will gain a foundation to develop medical, community, and/or research leadership expertise in addressing the health needs and experiences of this population.
Health, Equity, and Law Policy Pathway
Designed for students who understand social determinates of health, want to influence health inequalities, and are interested in the formation and implementation of health policies, participants work local and nationally. Students will learn and experience how policy makers control health, everything from finances to pre-authorization requirements for procedures and medication, to the cost of prescription drugs. The HELP Pathway enables participants to find and use their voice to influence policy and help shape their future patients’ experiences related to health and healthcare.
Health Humanities and Bioethics Pathway
Drawing on the medical schools’ strengths in health humanities and bioethics, this pathway provides students with an enriched experience. Students have numerous opportunities to pursue interests in areas of health humanities from writing to art as well as gain expertise in bioethics. These are achieved through a variety of clinical and research experiences, electives, and special projects and events.
Healthcare Innovation and Economics Pathway
For students with interest in the health economics, alternate career pathways in industry, business administration, medical startups, and healthcare innovation that will revolutionize the delivery of healthcare. Longitudinal courses are offered throughout medical school in conjunction with faculty at the University of Rochester Medical Center, the Center for Health + Technology, and the Innovation Center at the Simon Business School.
LatinX Health Pathway
Students with intermediate and advanced Spanish language proficiency have an enriched learning experience throughout medical school. Through the pathway, participants further develop their language, cultural, and clinical skills through didactic sessions, clinical electives, and special projects. They are better positioned to work with Spanish speaking patients, families, and communities.
Medical Education Pathway
Preparing students to be academic medical educators, the pathway provides knowledge in educational theory and develops skills in teaching. Activities include serving as a problem based learning tutor, leading a small group, developing learning objectives and delivering a lecture. In addition, students write high quality examination questions, perform assessments, and provide feedback.
Assessment in the ‘Double Helix Curriculum – Translations and Transitions’ mirrors the school’s Biopsychosocial approach to patient care and education and strives to optimize the capabilities of all students by providing motivation and direction for continuous learning, reflective practice, personal improvement, and professional accountability.
At Rochester, we believe that assessment is an ongoing and interactive process that drives student learning and development. To this end, we provide students with multiple opportunities for direct observation, feedback, and assessment of progress in key knowledge, skills, and behavioral areas that are linked to the school’s overall educational objectives.
Throughout their medical training, students will receive formative and summative feedback in required courses, clinical experiences, and end-of-phase assessments. Other defining components of assessment in the ‘Double Helix Curriculum – Translations and Transitions’ include:
- Development of Individual Learning Plans (ILP)
- Small group/team feedback
- Standardized patient feedback
- Formalized peer feedback
M.D./Ph.D.
Students interested in careers in medical science undertake training in both clinical medicine and research. The Medical Scientist Training Program (MSTP) at Rochester is funded by a grant from the National Institutes of Health, and provides an outstanding faculty and a wide range of research training opportunities found only in our nation's leading biomedical research and clinical training centers.
M.D./M.B.A.
In conjunction with the university’s Simon Business School, we offer a dual degree M.D./M.B.A. program in Healthcare Management. Matriculants complete their first year of study at the Simon School then begin medical school taking electives in their final year that apply to both degrees.
M.D./M.S. in Medical Neurobiology
The Masters of Science degree combines coursework in the medical curriculum with experimental studies in preparation for careers in research and education.
M.D./M.P.H.
The M.P.H. is offered in association with our Department of Public Health Sciences and some students have chosen to do this during a year out through our Academic Research Track..
M.D./M.S. in Medical Humanities
The Masters of Science degree in Medical Humanities provides a foundation in the use of perspectives and tools from humanities and arts to study the human contexts of health care.
M.D./Combined Masters
These programs in basic and translational sciences are available to medical students by special arrangement and can often be done through the Academic Research Track.
Please visit the Admissions Dual/Joint Degrees page for more information.