Bone Regeneration and Infection Management using 3D Printed Scaffolds
 Chronic osteomyelitis (OM) is a serious clinical problem in orthopaedic surgery, as approximately 112,000 orthopaedic device-related infections occur every year in the US alone, with an estimated overage in hospital costs of $15,000-30,000 per incident. While the infection rates over the past decade have been only 2% and 5% for joint prosthesis and fracture-fixation devices, respectively, these problems typically require a very costly and complicated multi-stage reconstruction techniques to first remove the infected devices and tissues and control the infection using antibiotic-laden cement spacers or bead, before attempting to replace the hardware and induce bone regeneration. Moreover, this multi-stage approach is associated with failure rates as high as 50% with catastrophic results that could lead to amputation or death.
Chronic osteomyelitis (OM) is a serious clinical problem in orthopaedic surgery, as approximately 112,000 orthopaedic device-related infections occur every year in the US alone, with an estimated overage in hospital costs of $15,000-30,000 per incident. While the infection rates over the past decade have been only 2% and 5% for joint prosthesis and fracture-fixation devices, respectively, these problems typically require a very costly and complicated multi-stage reconstruction techniques to first remove the infected devices and tissues and control the infection using antibiotic-laden cement spacers or bead, before attempting to replace the hardware and induce bone regeneration. Moreover, this multi-stage approach is associated with failure rates as high as 50% with catastrophic results that could lead to amputation or death.
Our lab is developing alternative fabrication technologies of spacers that can enhance the reproducibility of sustained release of antibiotics over a sufficient period to ensure eradication of bone infections and osteomyelitis, and potentially eliminate the need for the costly reconstruction procedures. Our hypothesis is that image-guided 3D printing of antibiotic-loaded, osteoinductive ceramic scaffolds can be effective in a single-stage reconstruction of infected nonunions with segmental bone loss.
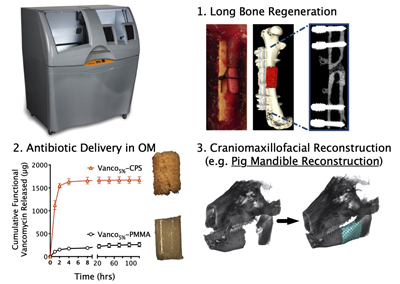
Specifically, our work has led to the development of innovative strategies for adapting low- temperature 3D printing technology to fabricate osteoconductive calcium phosphate (CaP) scaffolds for applications in preclinical models of bone regeneration and infection. This technology has translational potential in medical image-guided reconstruction of massive bone loss in scenarios involving extremity bone and craniomaxillofacial trauma or infections. Some specific foci of research include:
- Development of novel mouse models with an established bone S. aureus infection in association with a fracture fixation plate to explore 3D printing alternatives to PMMA spacers n single- and two-stage reconstruction procedures of massive bone defects.
- Adapting different modalities of low-temperature 3D printing of antibiotic-laden CaP scaffolds for sustained bactericidal delivery.
- High-throughput screens (HTS) to identify candidates that are not only bactericidal against S. aureus normal colony phenotype (NCP) and biofilm, but also bactericidal to small-colony variant strain (SCV) and S. aureus colonization of canaliculi and submicron cracks in cortical bone.
- μSiM-CA (Microfluidic - Silicon Membrane - Canalicular Array) as an in vitro screening platform for the genetic mechanisms of S. aureus invasion of the osteocyte lacuno-canalicular network (OLCN) of cortical bone during chronic osteomyelitis.
- Stem cell strategies to vitalize and vascularize 3D printed scaffolds for bone regeneration in craniofacial bones including mandible and jaw.
Collaborators: Edward Schwarz, Paul Dunman, James McGrath
Funding: NIH/NIAMS P50 AR072000