Formal Didactics
Orientation Boot Camp
The first two weeks of fellowship are devoted to didactics on core critical care topics coupled with instruction in common procedures. Senior fellows cover the clinical services during this time so first-years do not have competing responsibilities. Components include…
- the Society of Critical Care Medicine's Fundamentals of Critical Care Support Course
- ultrasound workshop, including hands-on scanning with live models
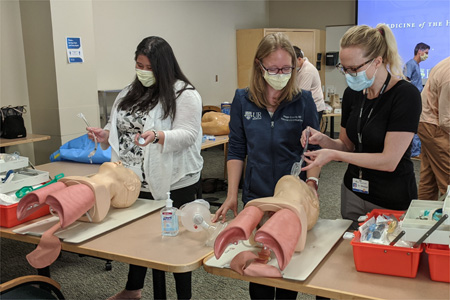
- airway workshop, with bag valve mask ventilation, endotracheal intubation, and rescue devices using mannequins
- vascular access workshop, including placing central venous, intraosseous, and arterial lines into mannequins
- bronchoscopy workshop, including hands-on practice with the scopes using mannequins
- mock codes in the high-fidelity simulator
- shadowing experiences with nurses in the medical ICUs
Teaching Conferences
Daily
- Critical Care Teaching Session: Faculty intensivists from all departments, critical care pharmacists, and university ethicists present to residents and fellows on core critical care topics every weekday. Sessions are open to trainees from all intensive care units.
Weekly
- Department of Medicine Grand Rounds: In addition to talks from institutional and visiting scholars, each division presents one fellow-led session per year on new developments in the specialty that are relevant to a general internal medicine audience.
- City-Wide Conference: Fellows discuss interesting cases together with a literature review that informs patient care. The series also includes faculty talks on current research and guest speakers presenting on cutting-edge pulmonary or critical care topics.
- Fellows' Lecture Series: Designed specifically for fellows, the series covers fundamental concepts in critical care practice. Speakers include intensivists and faculty from other disciplines who have expertise in conditions frequently encountered in the ICU.
Monthly
- Fellows' Morbidity and Mortality: Senior fellows present a case with a negative outcome to peers and faculty while engaging the group in a discussion of decisions in patient management. This is followed by a literature review pertinent to the undesired result.
- Journal Club: Senior fellows select landmark or new articles relevant to critical care practice and lead the audience in discussion. The goal is to simultaneously become familiar with new developments in the field and to learn the skills of evidence critique.
Yearly
- Society of Critical Care Medicine Critical Care Congress: Fellows are assisted by faculty to submit case presentations or original research to this national meeting. All trainees are provided with protected time and funding to attend the conference.
 Procedure Training
Procedure Training
- Fellows perform vascular access, thoracentesis, paracentesis, and lumbar puncture for their patients in the ICU. Initially these require supervision but with experience and faculty attestation to competence fellows may perform them independently.
- Fellows complete endotracheal intubation, bronchoscopy, and the placement of pleural catheters in the ICUs and during rotations dedicated to these skills. While we require supervision for these throughout training, fellows become proficient by graduation.
- Additional procedures including (but not limited to) elective cardioversion, pericardiocentesis, and the placement of transvenous pacemakers or pulmonary artery catheters are within the fellow's purview as long as a faculty supervisor is available.
Specialty Courses
- Basic Certificate in Quality and Safety: Fellows complete modules from the Institute for Health Care Improvement to develop their skills in quality improvement and patient safety. This is the foundation for later work on institutional and individual projects.
- Difficult Airway Course: Developed and presented by anesthesia department, this course builds upon basic airway skills by providing hands-on practice with rescue devices, including emergency cricothyroidotomy. Fellows participate during the first year.
- Emergency Neurological Life Support: The neuromedicine ICU delivers an in-person version of the national Neuro Critical Care Society's ENLS course. Fellows complete this course during their second year of training.
Hospital Committees
- Resuscitation Council: This inter-professional group includes critical care, anesthesiology, and emergency medicine. It meets monthly to oversee the rapid response and code teams as well as the medical emergency response team for visitors.
- Critical Care Morbidity and Mortality: A multi-disciplinary group meets periodically to review patient management when requested by entities outside critical care. The group also evaluates quality metrics like DVT prophylaxis and CLABSI rates.
- Root Cause Analysis: When warranted, critical care may convene a root cause analysis or participate an analysis initiated by others. Fellows are routinely asked to participate, both for educational purposes and to add perspective to the review.
- Critical Care Quality Council: Providers, nurses, pharmacists, and allied professionals from all ICUs meet monthly to develop shared protocols and work on quality improvement initiatives. Fellows often leverage this group for help with their QI projects.