Beta Thalassemia
What is beta thalassemia?
Thalassemia is a blood disorder that is inherited. This means it's passed down from
one or both parents through their genes. When you have thalassemia, your body makes
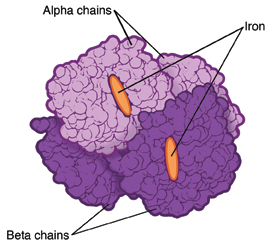
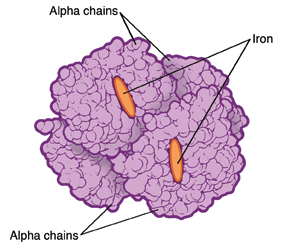
less hemoglobin than normal. Hemoglobin is an iron-rich protein in red blood cells.
It carries oxygen to all parts of the body.
There are 2 main types of thalassemia: alpha and beta. Different genes are affected
for each type.
Thalassemia can cause mild or severe anemia. Anemia occurs when your body doesn't
have enough red blood cells or hemoglobin. The severity and type of anemia depends
on how many genes are affected.
How to say it
thal-uh-SEE-mee-uh
What causes beta thalassemia?
Beta thalassemia is caused by changed (mutated) or missing genes. The types of the
disorder are based on how severe the anemia is:
-
Beta thalassemia minor. This is also called beta thalassemia trait. It may cause no symptoms or only mild
anemia. People with this mild form may not need treatment.
-
Thalassemia intermedia. This causes moderate to severe anemia. You may sometimes need transfusions and other
treatment.
-
Beta thalassemia major (Cooley anemia). This is the most severe form. People with this condition may have life-threatening
anemia. They will need regular blood transfusions and other treatment.
Many people with this disorder are given iron replacement by mistake. This happens
when a lack of iron is believed to cause their anemia. Too much iron can be harmful.
So it's important to get the right diagnosis. You may need to see a blood disorder
specialist (hematologist).
Who is at risk for beta thalassemia?
Beta thalassemia is a genetic disease inherited from one or both parents. The only
risk factor is having a family history of the disease.
What are the symptoms of beta thalassemia?
Different people will have different symptoms based on which type of the disorder
is inherited.
Beta thalassemia major
This is the most severe type of this disorder. Children born with this type will have
symptoms early in life that include:
-
Pale skin
-
Fussy
-
Having a poor appetite
-
Having many infections
Over time, more symptoms will appear, including:
Without treatment, the spleen, liver, and heart become enlarged. Bones can also become
thin, brittle, and deformed.
People with this condition will need frequent blood transfusions. They may not live
a normal lifespan. Iron builds up in the heart and other organs from blood transfusions.
This can cause heart failure as early as the teens or early 20s.
Thalassemia intermedia
This type can cause symptoms of moderate to severe anemia. These include:
Thalassemia minor
This type often causes no symptoms.
How is beta thalassemia diagnosed?
Beta thalassemia is most often found in people who are of Greek, Italian, African,
or Asian origin. The diagnosis is most often made between ages 6 and 12.
These tests may be able to tell if you are a carrier and can pass the disorder on
to your children:
-
Complete blood count (CBC). This test checks the size, number, and maturity of different blood cells in a set
volume of blood.
-
Hemoglobin electrophoresis. This lab test differentiates the types of hemoglobin.
All of these studies can be done from a single blood sample. During pregnancy, the
baby may be diagnosed using CVS (chorionic villus sampling) or amniocentesis.
How is beta thalassemia treated?
Treatment will depend on your symptoms, age, and general health. It will also depend
on how severe the condition is.
Treatment may include:
-
Regular blood transfusions
-
Medicines to reduce extra iron from your body (called iron chelation therapy)
-
Surgery to remove the spleen, if needed
-
Daily folic acid
-
Surgery to remove the gallbladder
-
Regular checks of heart and liver function
-
Genetic tests
-
Bone marrow transplant
Do not take any iron supplements.
What are possible complications of beta thalassemia?
Complications of beta thalassemia vary depending on the type:
-
Thalassemia minor. This is mild and causes no problems. But you will be a carrier of the disorder.
-
Thalassemia intermedia. This type can cause problems based on the severity of the anemia. These problems
include delayed growth, weak bones, and enlarged spleen.
-
Beta thalassemia major. This causes major problems and can result in early death. Complications may include
delayed growth, bone problems causing facial changes, liver and gallbladder problems,
enlarged spleen, enlarged kidneys, diabetes, hypothyroidism, and heart problems.
Living with beta thalassemia
If you have beta thalassemia major or intermedia, living with the disorder may be
challenging. Work with your healthcare provider to make a treatment plan that includes
blood transfusions. Your plan may also include treatment to remove extra iron from
your body (iron chelation therapy). You will also have regular blood tests and physical
exams. It's important to prevent infections. Wash your hands often and stay away from
others who are sick. You may also need emotional support. Talk with your provider.
They can help you find support.
Key points about beta thalassemia
-
Thalassemia is an inherited blood disorder. It causes the body to make less hemoglobin.
-
There are several types of beta thalassemia.
-
Different people will have different symptoms. They depend on which type of beta thalassemia
is inherited.
-
Treatment of beta thalassemia may include medicines and regular blood transfusions.
-
Work with your healthcare provider to stay healthy and reduce complications of the
disease.
Next steps
Tips to help you get the most from a visit to your healthcare provider:
-
Know the reason for your visit and what you want to happen.
-
Before your visit, write down questions you want answered.
-
Bring someone with you to help you ask questions and remember what your provider tells
you.
-
At the visit, write down the name of a new diagnosis and any new medicines, treatments,
or tests. Also write down any new instructions your provider gives you.
-
Know why a new medicine or treatment is prescribed and how it will help you. Also
know what the side effects are.
-
Ask if your condition can be treated in other ways.
-
Know why a test or procedure is recommended and what the results could mean.
-
Know what to expect if you do not take the medicine or have the test or procedure.
-
If you have a follow-up appointment, write down the date, time, and purpose for that
visit.
-
Know how you can contact your provider if you have questions.