Case of the Month: Increasing Pressure in the Abdomen
Case Authors: Cansu Karakas, MD (PGY-2), Aaron R. Huber, DO
Clinical History
An elderly woman presented with one month of pressure in her abdomen for which she was referred for surgical oncology evaluation. This pressure was worse when walking and improved when sitting.
Past Medical History
The patient had no significant known past medical or surgical history.
Recent History
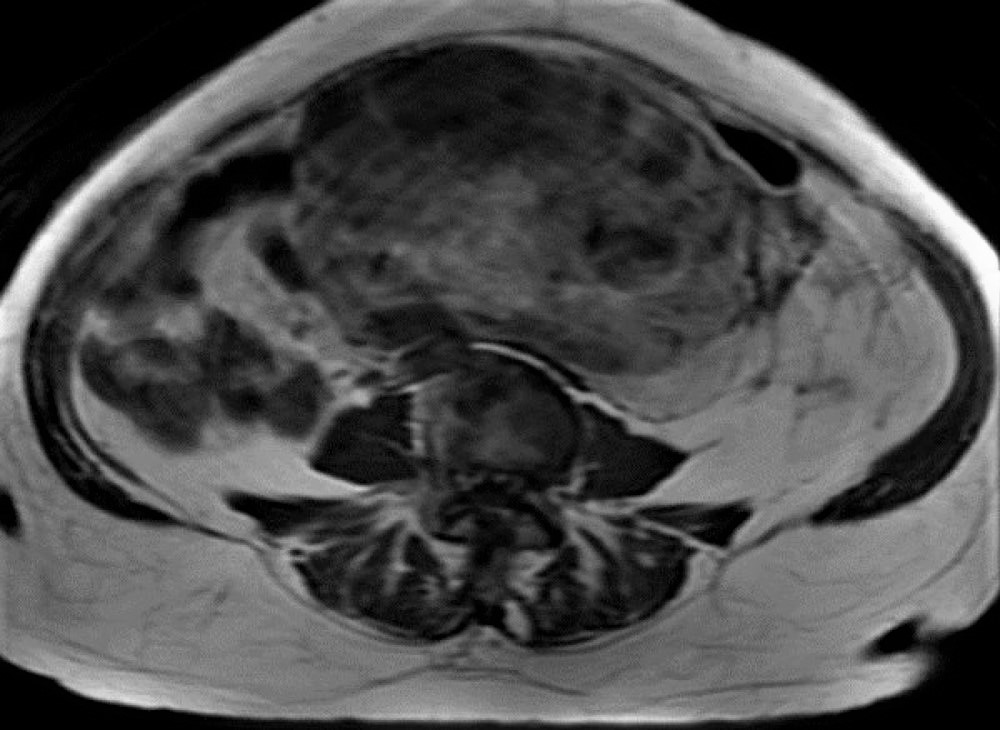
Magnetic resonance (MR) scan of the abdomen and pelvis revealed a large (27.2 cm) retroperitoneal, complex, infiltrative, heterogeneous lesion involving predominantly the mid and left abdominal and pelvic region. Within the mass, there is a circumscribed, complex component with multiple solid heterogeneous nodular foci (Figure 1). The patient had a needle biopsy to establish the diagnosis and subsequently had the mass resected.
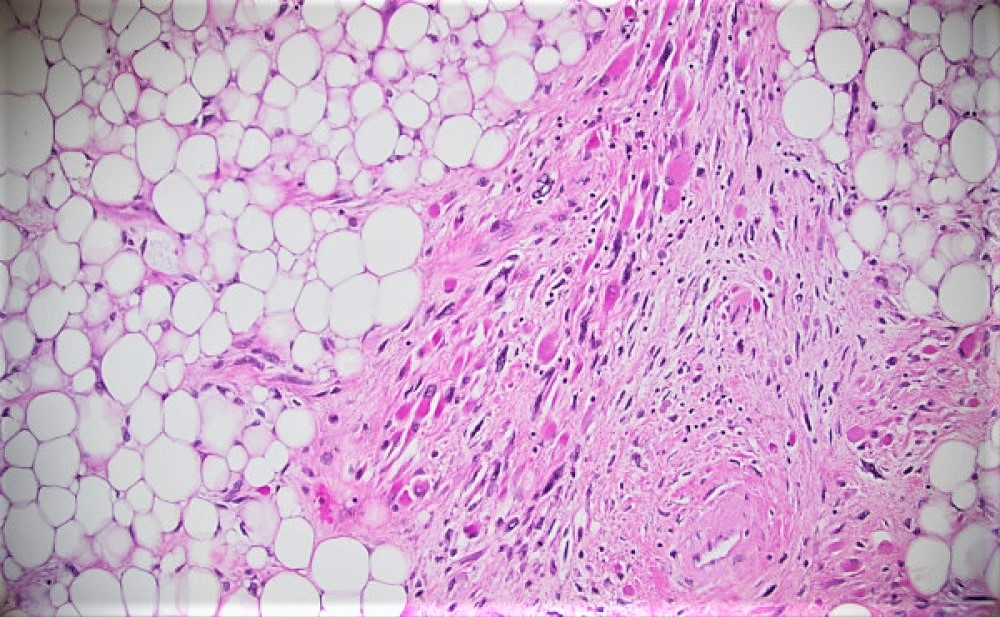
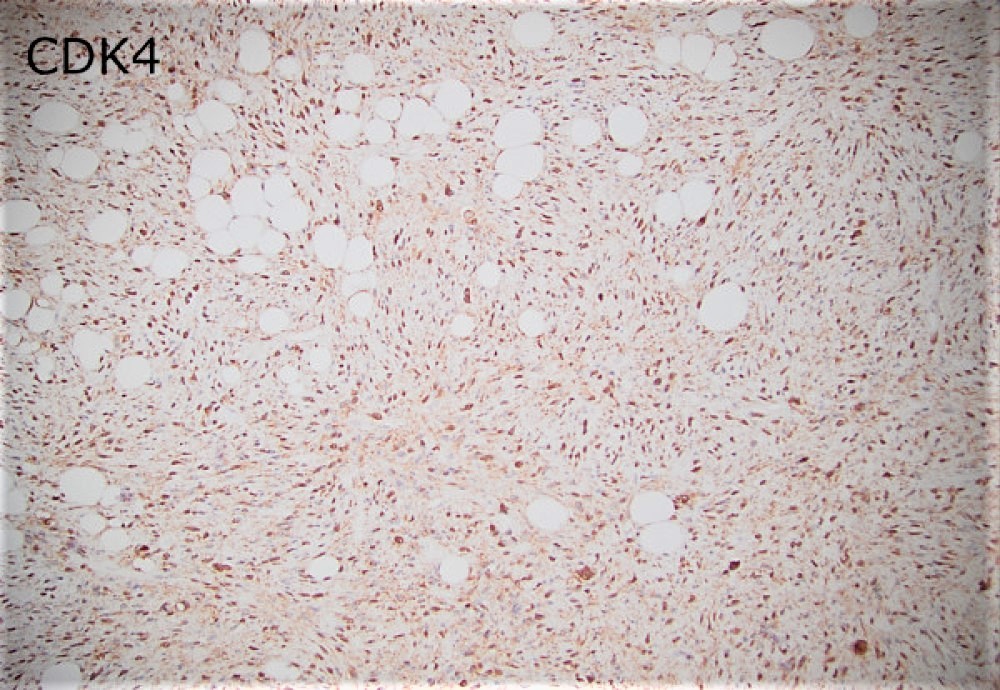
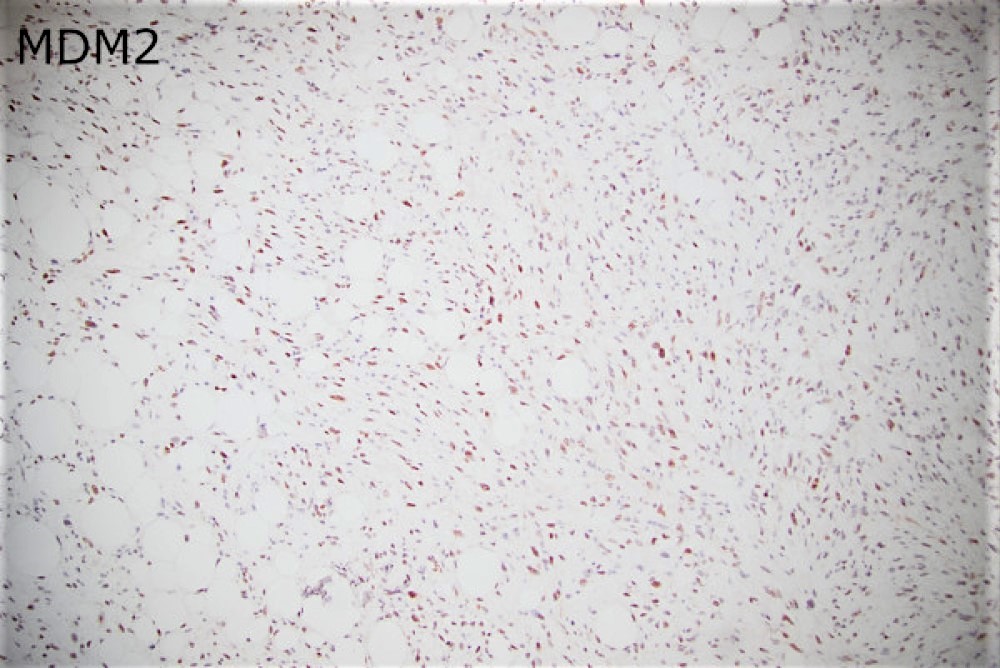
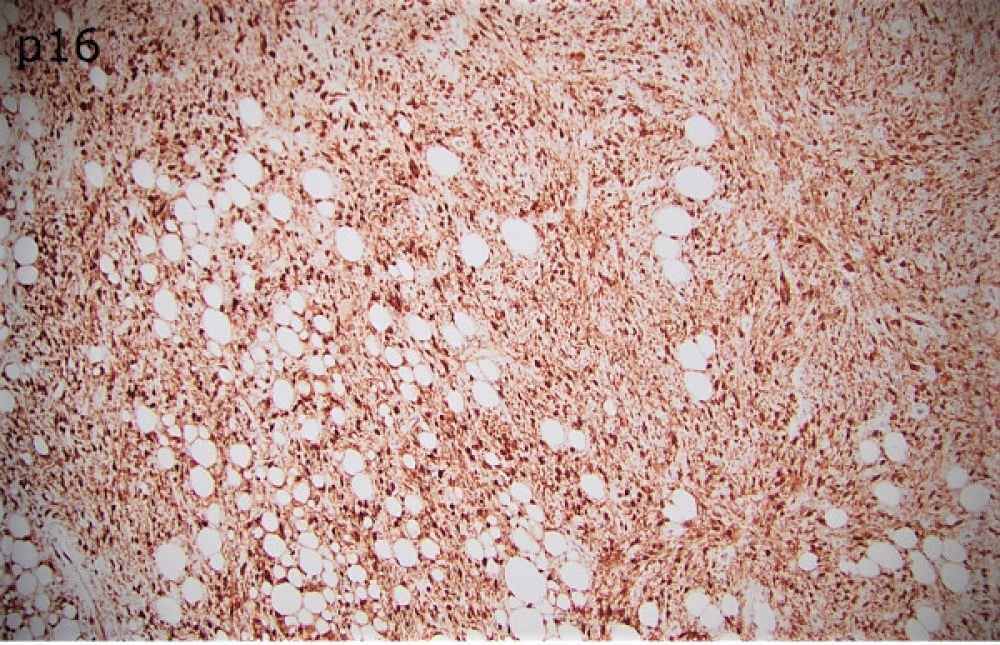
Sections of the biopsy revealed lobules of adipocytes admixed with the areas of an atypical spindle cell proliferation with moderately to markedly pleomorphic cells arranged in loose fascicles or storiform pattern within a fibrotic, focally myxoid stroma. Approximately 60-70% of the tumor was replaced by necrosis. Ki-67 proliferation index was 5-10%. Immunohistochemical staining demonstrated strong positivity with MDM2, CDK4 and p16 which supported the diagnosis.
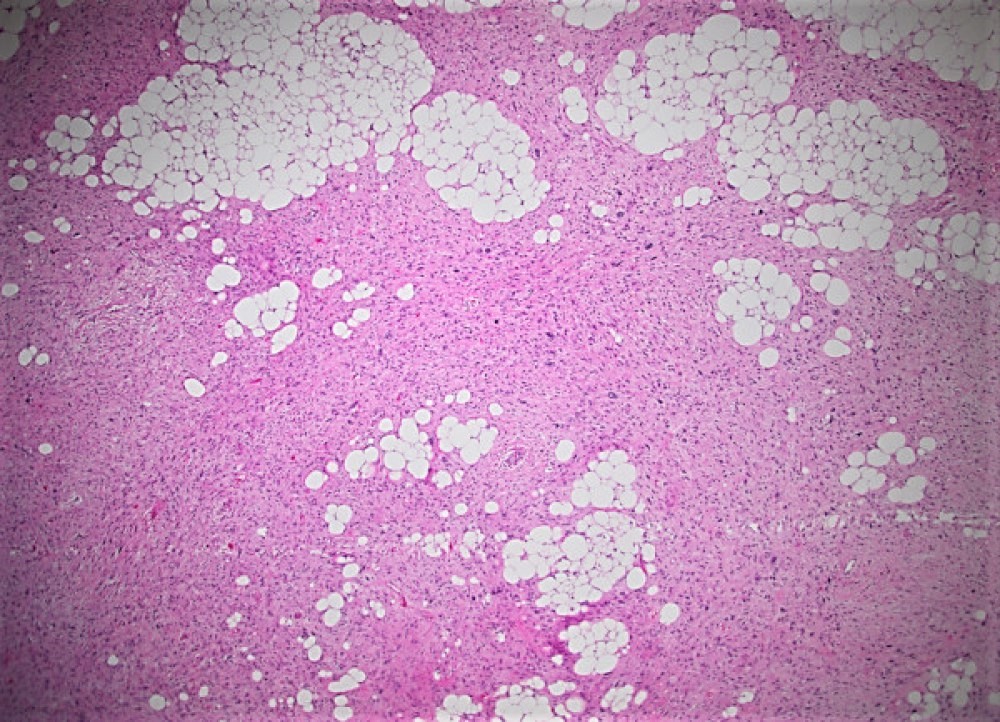
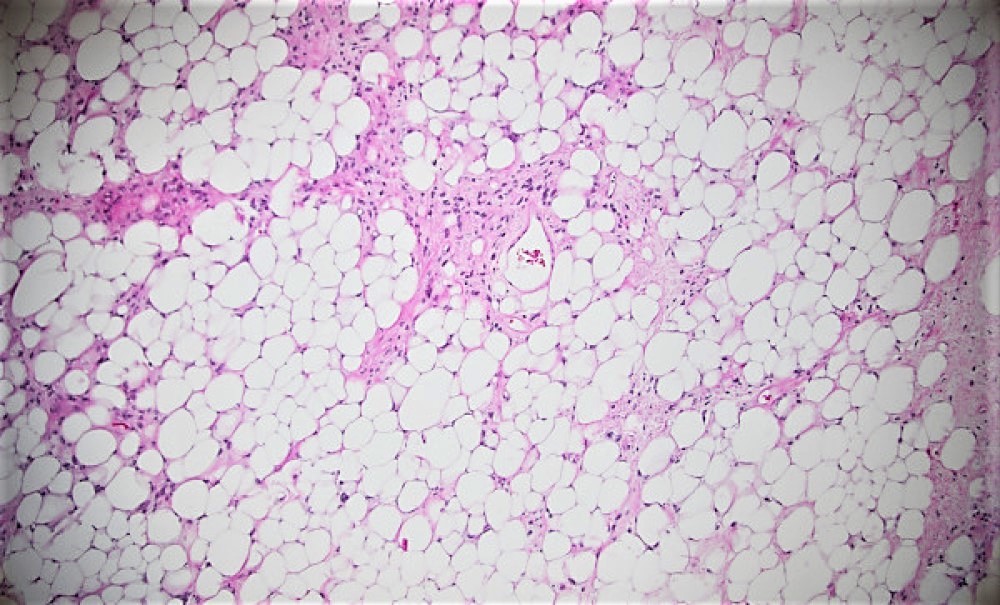
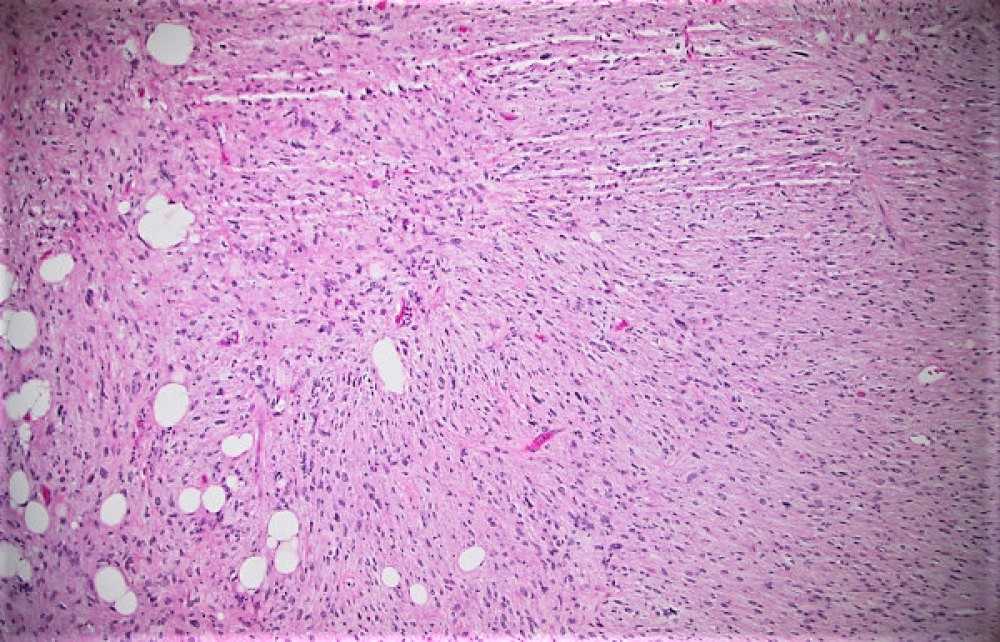
Grossly, the resection specimen demonstrated a large nodular yellow-tan mass with firm, pink-tan fleshy foci (Figure 2). Histologically, there was a transition between lobules of a well-differentiated atypical adipocytic neoplasm (Figures 3 and 4) to a high-grade pleomorphic and spindle cell sarcoma (Figures 5 and 6). There were foci of myxoid change and cells with rhabdoid-like morphology (Figure 7). Both the low-grade and high-grade components expressed CDK4, MDM2, and p16 (Figures 8-10), while immunohistochemical stains for myogenin and MyoD1 were negative.