Helmets Protect Patients from Falls
With research showing that hospitalized patients are at least twice, possibly three times, as likely to fall as people in the general population, teams at Strong Memorial Hospital have been eagerly investigating fresh ways to keep patients safe.
 "Falls can be devastating setbacks, especially for patients who are already well on the road to recovery,” said Jennifer Harris, R.N., a senior clinical nurse specialist tasked with championing many of the hospital’s safety improvement projects. “For some, a fall could even mean the difference between returning home and needing care for the rest of their lives.”
"Falls can be devastating setbacks, especially for patients who are already well on the road to recovery,” said Jennifer Harris, R.N., a senior clinical nurse specialist tasked with championing many of the hospital’s safety improvement projects. “For some, a fall could even mean the difference between returning home and needing care for the rest of their lives.”
Since early 2011, Harris has been collaborating with critical care clinical nurse specialist Mark Ott, R.N., on a hospital-wide falls-reduction project. The effort is, in part, a response to the Joint Commission’s recently targeting in-hospital falls as one of their top priority National Patient Safety Goals.
The challenge requires a fair bit of detective work, Harris said, as the reasons behind such falls are unique to each unit.
“If you want to decrease injuries from falls, you have to really work to understand what causes them in the first place,” she said. "The reasons that orthopaedic patients fall are vastly different from those that cause elderly patients to fall. What’s more, many of the falls that injure patients are not ‘grand falls,’ but just simple stumbles. Patients catch their heel and go down.”
Most of these falls take place within the patient’s own room, studies show. Half occur en route to the bathroom.
A Dual Approach
When it comes to protecting patients against harmful falls, Ott and Harris’s team has taken a dual approach: Avoiding falls outright, of course, but also mitigating injury in the unfortunate event that they do happen.
“Obviously, we’d like to prevent the falls altogether,” Ott said. “We take special care when prescribing a medicine that has delirium as a known side-effect, and we work hard to keep rooms clutter-free. We’re also enhancing our protective equipment, installing night lights to improve visibility, and adding bed alarms that sound when a patient gets up.”
Harris and Ott have recently worked to replace 100 hospital beds with newer models featuring built-in bed alarms. “Our goal, over time, is to replace our entire hospital fleet with these beds,” he said. “Of course, in some very special cases, we still employ bedside sitters to make absolutely sure patients don’t get up unassisted.”
They’re also extending more robust education to patients and families--underscoring the importance of notifying a staff member before attempting to get up, and reinforcing this message with signage. What’s more, they’re working hard to train nurses to consistently pre-empt patients’ needs.
“For a couple of years now, we’ve been putting a keen emphasis on rounding hourly, making a point to address patients’ requests--like toileting or needing to change position--well before they become urgent,” Harris said. Some studies have shown that this practice alone can cut the risk for falls in half.
"Of course, falls aren’t perfectly preventable. People fall in real life,” Harris said. “That’s why the second prong of our effort--figuring out which patients, if they did fall, would be most susceptible to serious injury, and finding ways to minimize that harm--is so important.” One of the most novel approaches, at first blush, seems almost obvious: Encouraging certain groups of high-risk patients (for instance, only 40 percent to 50 percent of cancer patients qualify) to wear protective helmets.
In September, Harris and Ott worked with 6-3400’s (a hematology-oncology unit) nurse manager Elizabeth Conderman, R.N., to debut a pilot program encouraging patients to wear the headgear both while in the hospital and after they’re discharged.
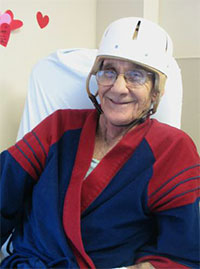
“These patients are often on medication that suppresses their platelet counts, magnifying their risk for bleeds. We take time to explain to them that the helmets are intended to empower them, to preserve their independence,” she said. “Patients even get to keep the helmets when they leave.”
Surprisingly, many patients have embraced the idea, personalizing their helmets and decorating them with stickers.
“One patient even put holiday lights on hers,” Ott said. “Another patient, who faithfully wore her helmet after discharge, fell in the ramp garage while returning for an outpatient appointment. Thanks to her helmet, she was fortunate and didn’t suffer a head injury. And that’s indicative of a broader trend; so far, among patients who have accepted helmets and worn them consistently, we’ve not had a single head bleed.”
There are no published studies demonstrating that the helmet approach works, but the anecdotal evidence is convincing, and Harris and Ott hope to ultimately gather data and publish their findings. In the meantime, the concept is catching, rolling out to other hospital areas in which patients are at high-risk for bleeding (such as patients with kidney and liver conditions). Harris and Ott are now turning their attention to protective equipment meant to blunt potential hip injuries--like deadly fractures--that can follow a fall.
One possible solution, currently used in some nursing homes, is “hipsters,” which resemble bike shorts, but with padding sewn-in to cushion the bone.
“We really need to tailor interventions to each patient, and that may mean putting several safety measures in place at once,” Ott said. Regardless, it’s exciting to see the change we’re making, and the way patients and providers are really partnering with us, embracing these new ideas.
Molly Miles |
5/1/2012
You may also like