Additional Curricular Priorities
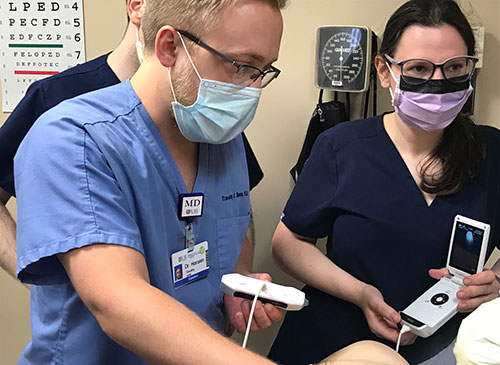 Point of Care Ultrasound
Point of Care Ultrasound
Training in the use of ultrasound guidance for invasive procedures such as central lines, paracentesis, and thoracentesis is standard in our program. Additionally, we believe that in the near future portable ultrasound machines will have earned a place in our pockets next to our stethoscopes to help us perform certain aspects of the physical exam more effectively.
Given this, we are rapidly expanding and integrating training for all Internal Medicine residents in the use of diagnostic point-of-care ultrasound (POCUS) with the goal of using it to assist with real-time bedside clinical assessment and decision-making. We have a robust faculty development effort underway to help faculty learn POCUS skills and how to incorporate findings into medical decision-making.
We are also working to improve residents’ access to pocket ultrasound machines, including having a number of machines assigned to different medicine resident teams at Strong and Highland Hospitals. Cardiac, thoracic, and abdomen POCUS knowledge and skills are being interwoven throughout the curriculum for all Internal Medicine residents, including didactics, on-line training, small group workshops, and bedside team ultrasound rounds.
For residents interested in further expanding and refining their POCUS skills, an exciting elective rotation through a wide variety of ultrasound venues is available. The ultrasound elective includes hands-on experiences with very enthusiastic faculty from our Cardiology, Critical Care Medicine, and Hospital Medicine divisions as well as the Departments of Emergency Medicine, Anesthesiology, Imaging Sciences, and our First Responder Training Program.
Procedures
A resident-led effort over the past few years greatly expanded procedural opportunities for residents at SMH. This effort ultimately led to the creation of a dedicated procedure service that is staffed with an attending, advanced practice providers, and residents. The service performs large numbers of procedures at the bedside, including paracentesis, thoracentesis, central line placement, lumbar puncture, and ultrasound-guided peripheral IV placement. Residents rotate onto the Procedure Service as PGY2s.
Social Determinants of Health
We have an interactive, experience-based curriculum to help all Internal Medicine residents learn about and advocate for patients with barriers that impact their ability to live to their fullest potential. Every intern in our categorical, primary care, and physician scientist programs will go out into the community to learn about resources available to patients in addition to the services provided within our institution. Upper-level Internal Medicine residents have the opportunity to continue this exploration within the community through our Community Outreach elective. We also offer the Community Health and Advocacy Resident Education (CARE) track, where residents have the opportunity to develop their own community partnerships. Finally, all residents have the opportunity to embed social determinant filters into their ambulatory clinic dashboards, allowing them to explore important health elements (e.g., HbA1C for diabetic patients, BP control for those with hypertension, cancer screening completion, etc.) for their personal panel of patients and/or patients in the whole practice by various identity filters (e.g., gender, SES, race, etc.).
Quality Improvement and Patient Safety
In 2016 the University of Rochester Medical Center (URMC) was selected by the ACGME to be one of 8 institutions nationally to be a CLER (Clinical Learning Environment Review) Innovator site. This has helped URMC become a leader in improving medical centers’ Clinical Learning Environments. From a practical perspective, our residents benefit from multiple ongoing initiatives that improve the care of patients (e.g., improving hand-offs and transitions of care); improve the learning, supervision, and professionalism culture; and integrate residents into the patient safety and quality improvement (QI) initiatives underway throughout the medical center.
All of our residents are taught basic and advanced QI and patient safety knowledge and skills. In addition, senior residents all participate in ongoing multidisciplinary QI teams working on real-world QI projects in areas of their choosing (e.g., ambulatory primary care vs. general medicine inpatient vs. intensive care vs. specialty projects).
Communication Skills
Communicating effectively with patients, their families, and other healthcare team members is absolutely critical to providing the highest quality patient care. A portion of our curriculum is dedicated to communication skills training, including in the ambulatory education sessions (e.g., building relationships, motivational interviewing, shared decision-making, etc.) and in clinical rotations (e.g., running a family meeting in the palliative care rotation). In addition, we are very fortunate to have a PhD psychologist, Dr. Andrea Garroway, who spends the majority of her time working on one-on-one coaching our internal medicine residents in communicating with their patients, families, and teams.