News
20242023202220212020
Talk: Treatment Options for Headache Sufferers
Wednesday, December 17, 2014
The next Got Health?
talk Headaches: When to Get Help,
presented by Ann Ford Fricke, nurse practitioner at the Medical Center, will be held from 12:10 to 12:50 p.m. on Thursday, Dec. 18, in the Kate Gleason Auditorium of the Central Library's Bausch and Lomb Building, 115 South Ave. She will discuss headache causes, management, and treatments. The lecture is sponsored by the Center for Community Health. Parking is available in the Court Street garage, which is connected to the library.
Mice injected with human brain cells get smarter, scientists say
Tuesday, December 9, 2014
What would Stuart Little make of it? Mice have been created whose brains are half-human. As a result, the animals are smarter than their siblings. The idea is not to mimic fiction but to advance understanding of human brain diseases by studying them in whole mouse brains rather than in laboratory dishes.
The altered mice still have mouse neurons - the thinking
cells that make up around half of all their brain cells. But practically all their glial cells, the ones that support the neurons, are human.
It’s still a mouse brain, not a human brain,
says Steve Goldman of the University of Rochester Medical Center in New York. But all the non-neuronal cells are human.
Blows to Head Damage Brain's 'Garbage Truck', Accelerate Dementia
Tuesday, December 2, 2014
A new study out today in the Journal of Neuroscience shows that traumatic brain injury can disrupt the function of the brain's waste removal system. When this occurs, toxic proteins may accumulate in the brain, setting the stage for the onset of neurodegenerative diseases such as Alzheimer’s and chronic traumatic encephalopathy.
We know that traumatic brain injury early in life is a risk factor for the early development of dementia in the decades that follow,
said Maiken Nedergaard, M.D., D.M.Sc., co-director of the University of Rochester Center for Translational Neuromedicine and senior author of the article. This study shows that these injuries set into motion a cascading series of events that impair the brain's ability to clear waste, allowing proteins like tau to spread throughout the brain and eventually reach toxic levels.
The findings are the latest in a series of new insights that are fundamentally changing the way scientists understand neurological disorders. These discoveries are possible due to a study published in 2012 in which Nedergaard and her colleagues described a previously unknown system of waste removal that is unique to the brain which researchers have dubbed the glymphatic system.
2014 Shields Research Grant Recipient: Joana Osorio, MD
Friday, November 21, 2014

Joana Osorio, MD
Department of Neurology Instructor, Joana Osorio, MD has been chosen by the Child Neurology Foundation as the 2014 Shields Research Grant Recipient for her project, Cell-based therapy for Pelizaeus-Merzbacher disease
.
This research project aims to develop a cell-based treatment strategy for Pelizaeus-Merzbacher disease (PMD), a severe pediatric disorder of myelin caused by mutations in the proteolipid protein gene (PLP1). By transplanting genetically corrected cells from affected patients in a murine model of PMD, we will test their ability to rescue the phenotype and produce normal myelin. We will use induced pluripotent stem cells from patients with duplications and missense mutations in the PLP1 gene, correct the mutations by using gene-editing techniques and subsequently differentiate those to oligodendroglial fate. After intracerebral transplantation in a murine model of PMD, we will evaluate their motor performance and posteriorly the histology of engrafted cells. If this study is successful, this study will provide a proof of principle that autologous cell transplantation can be a feasible strategy for treatment of congenital disorders of myelin.
Researchers Using New Tools to Fight Brain Infection
Monday, November 17, 2014
Researchers have developed new insight into a rare but deadly brain infection, called progressive multifocal leukoencephalopathy (PML). This disease – which is caused by the JC virus – is most frequently found in people with suppressed immune systems and, until now, scientists have had no effective way to study it or test new treatments.
The JC virus is an example of an infection that specifically targets glia, the brain’s support cells,
said neurologist Steve Goldman, M.D., Ph.D., co-director of University of Rochester Center for Translational Neuromedicine and senior author of the paper. Because this virus only infects human glia and not brain cells in other species, it has eluded our efforts to better understand this disease. To get around this problem, we have developed a new mouse model that allows us to study human glia in live animals.
The new discovery – which appears today in the Journal of Clinical Investigation – was the result of research using a new tool developed at the University of Rochester. Last year, Goldman and Maiken Nedergaard, M.D., D.M.Sc., reported that they had created a mouse model whose brains consisted of both animal neurons and human glia cells. While the previous study focused on the fact that the human cells essentially made the mice smarter, at the same time it created a powerful new platform for researchers to study human glial cells in live adult animals, including diseases that impact these cells.
New Neurovascular Ultrasound Laboratory a Success
Saturday, November 8, 2014

Christina Clary and Dr. Holmquist
Through determination and teamwork with Neurosurgery and Imaging Sciences, the Department of Neurology’s vision of
having a dedicated Neurovascular Laboratory has been realized. The laboratory performs carotid ultrasounds on
patient's with suspected cerebrovascular disease. Since opening this past July, we have already performed over fifty
studies. The neurovascular laboratory will play an integral role in our department's mission of providing
comprehensive neurovascular care to our region and ultrasound education to our residents, students and fellows. Our
upcoming plans involve performing transcranial dopplers. I would like to take this time to especially thank Christy
Clary, Christy Miller, and Dr. Benesch for their time and effort to help make this happen.
The neurovascular laboratory is located at 2180 South Clinton Avenue, the site of the Comprehensive Stroke Center
clinic. Studies can be ordered through eRecord and by contacting Melissa Mack or Christina Holloway at 275-2530.
- Todd Holmquist, M.D.
PharmAdva Joins START-UP NY
Wednesday, October 22, 2014
PharmAdva, a medical device manufacturer, has been approved to participate in the START-UP NY economic development program. The company, which will locate in High Tech Rochester's Lennox Tech Enterprise Center in Henrietta, is commercializing a technology developed at the Medical Center by Michel Berg, associate professor of neurology and medical director of the Strong Epilepsy Center.
Józefowicz Honored for Serving Polish University
Thursday, October 16, 2014

Ralph Józefowicz, M.D. (left)
Ralph Józefowicz, professor of neurology, received the Merentibus Medal from Jagiellonian University, central Europe's second-oldest university, on Wednesday, Oct. 1, in Krakow, Poland. The medal is awarded each year for great services rendered to the Jagiellonian University.
Józefowicz established a medical exchange program between Jagiellonian University Medical College and the School of Medicine and Dentistry. Since the program’s inception in 1995, 111 Rochester medical students and 58 neurology residents have taught neurology in Krakow, and 170 Jagiellonian students have participated in clinical electives at Rochester.
A Reflection on the Increasing Importance of Private Capital in Medical Research
Wednesday, October 15, 2014
Private philanthropic foundations are emerging as a revolutionary source of innovative medical research and development funds. Though the amount of private philanthropic donations as a percentage of medical research spending, is still at a nascent stage, the reality of stagnating federal and state contributions to research and development enterprises is indicative of the future impact that private dollars may have on the field.
Funding for a disease is often scarce when the condition only affects a small portion of the population, or is considered to be less severe than other diseases in its class. Philanthropic medical research donations can target and drive medical advancements in these fields or with these diseases which are relatively neglected.
For example, Michael Goldberg, founding partner at the personal injury law firm Goldberg Weisman Cairo, and his family started the Goldberg Nathan Myotonic Dystrophy Type 2 Fund to encourage medical research into myotonic dystrophy type 2 (a rare genetic disorder characterized by muscular dystrophy).
The Goldberg endowment donated $1.25 million gift to the University of Rochester School of Medicine and Dentistry. The gift will be used to establish a center that will specifically study myotonic dystrophy type 2. Donations from private individuals who have loved ones or family members afflicted with rare genetic conditions are invaluable.
read more ...
URMC Tourette Center Named Tourette Syndrome Association Center of Excellence
Wednesday, October 8, 2014
The national Tourette Syndrome Association today announced the designation of 10 Tourette Syndrome Association
Centers of Excellence
at premier healthcare facilities, research centers and academic institutions located
across the United States.
Among them was the Tourette Center (affiliated with the Child Neurology division) here at URMC, headed by
unit chief, Jonathan Mink, M.D., Ph.D.
The designation of Tourette Syndrome Association Centers of Excellence in communities across the country,
particularly in underserved areas, is crucial to our mission,
said Annetta Hewko, President of the Tourette
Syndrome Association. Today, there is no standard model of care for Tourette's or Tic Disorders. Our aim is to
partner with the Centers of Excellence to set these standards and increase access to informed, evidence-based
treatment, compassionate care and guidance. We are genuinely excited to launch this initiative. It can significantly
impact our mission to serve to all people affected by Tourette’s and Tic Disorders.
The newly designated Centers will be the catalysts for cutting-edge scientific and clinical research aimed at
decreasing diagnostic variability, deciphering the cause(s) and improving treatment of both tic and non-tic
features. The Centers will also lead the way in training the next generation of experts in TS and Tic Disorders,
said Dr. Kevin St.P. McNaught, the Tourette Syndrome Association's Vice President for Medical and Scientific Programs.
read the
entire press release ...
Research Seeks to Break New Ground in Understanding of Schizophrenia
Tuesday, September 30, 2014
More than $6 million in funding from the National Institute of Mental Health (NIMH) is supporting new research that
could fundamentally alter the way we comprehend and, perhaps ultimately, treat schizophrenia.
The research - which is being led by University of Rochester Center for Translational
Neuromedicine co-directors Steve Goldman, M.D., Ph.D., and Maiken Nedergaard, M.D., D.M.Sc. - will explore
the role that support cells found in the brain, called glia, play in the disease.
The new research is possible because of findings published by Goldman and
Nedergaard last year that showed that glial cells play an important role in the complex signaling activity that
is unique to the human brain. In these experiments the researchers showed that when human glial cells were implanted
into the brains of newborn mice the human cells influenced communication within the animals' brains, allowing the mice
to learn more rapidly.
Moxley and Thornton Honored for Myotonic Dystrophy Research
Monday, September 22, 2014

Richard Moxley

Charles Thornton
University of Rochester neurologists Richard Moxley, M.D., and Charles Thornton, M.D., have been recognized by the Myotonic Dystrophy Foundation (MDF) with an Outstanding Research Achievement Award. The event took place at the U.S. Capitol earlier this month and honored their contribution to finding new treatments for myotonic dystrophy.
"This award is in recognition of the enduring and transformative collaboration that Drs. Moxley and Thornton have carried out in myotonic dystrophy research and clinical care, and the truly outstanding progress they have made possible in the search for treatments and a cure for the disease," said Molly White, executive director of MDF.
This recognition follows on the heels of a $7 million grant from the National Institute of Neurological Disorders and Stroke (NINDS) to renew funding for the University's Senator Paul D. Wellstone Muscular Dystrophy Cooperative Research Center, a designation that dates back to 2003. The team is also preparing -- in collaboration with Isis Pharmaceuticals -- to begin testing the first targeted treatment for the disease.
This research has brought scientists to the threshold of a potential new therapy that could reverse the genetic cause of DM1. Partnering with Isis Pharmaceuticals, the Rochester team developed a synthetic molecule -- called an antisense oligonucleotide -- that mimics a segment of the genetic code. In a study appearing in the journal Nature in 2012, Thornton and his colleagues showed that, when injected into mice with myotonic dystrophy, these molecules improved function. Isis Pharmaceuticals has recently completed Phase 1 testing and will soon advance to testing in people with the disease.
Read More: Moxley and Thornton Honored for Myotonic Dystrophy ResearchDr. Richard Satran, Founding Member of the Department of Neurology Dies
Monday, September 22, 2014

Dr. Richard Satran, M.D.
It is with a sad heart the department of Neurology announces that Dr. Richard Satran died Saturday morning.
Dr. Satran was a founding member of the department of Neurology arriving in Rochester in 1962 under the leadership of Paul Garvey. He never left and built his formidable career around patient care, teaching, and the history of neurology. He became Professor Emeritus in 1997.
From the first week I moved to Rochester in 1990 when he was my attending in resident clinic, to the very last discussions we had about health care and teaching, Dr. Satran was always a mentor to me and to many others,
said chair of Neurology, Robert G. Holloway, M.D., M.P.H.
He was a neurologist's neurologist and his passion, integrity and approach to neurology lives on in all of us. He was from the biopyschosocial era of the Medical School and was always a fierce advocate for patients and their quality of life - he taught many to always think about the broader context within which a patient's disease occurs, lessons that are more relevant today than ever
, continued Holloway.
We extend our deepest condolence to Rick's wife, Hilda and his entire family. He will be deeply missed. View Dr. Satran's obituary.
Gift Will Advance Research on Myotonic Dystrophy Type 2
Tuesday, September 9, 2014
A $1.25 million gift from Lilyan (Lil) and Albert (Alfy) Nathan of Florida and Michael and Sherry Goldberg of Chicago will create a new center dedicated to research on myotonic dystrophy type 2 (DM2) at the University of Rochester School of Medicine and Dentistry. The gift will be used to support a new research program that will be led by UR Medicine neurologist Chad Heatwole, M.D.
We are deeply grateful to the Nathan and Goldberg families for their extreme generosity,
said Robert Holloway, M.D., M.P.H., the chair of Department of Neurology and the Edward A. and Alma Vollertsen Rykenboer Chair in Neurophysiology. Due to the efforts of Chad Heatwole, Richard Moxley, Charles Thornton, and many others here in Rochester, we believe that new therapies for this disease are on the horizon. This gift will help accelerate these efforts.
Myotonic dystrophy has been characterized as one of the most diverse genetic diseases with a wide range of symptoms ranging from fatigue, muscle stiffness, muscle weakness, cognitive impairment, depression, difficulty sleeping, impaired vision, pain, difficulty swallowing, and gastrointestinal problems. The severity and onset of these symptoms vary from patient to patient.
Dr. Heatwole gave us the first glimmer of hope that someone was actually interested in helping people with this disease,
said Michael Goldberg, founding partner of the Chicago firm Goldberg Weisman Cairo. While our family had never made a major donation to a charity or medical institution before, we believed in Dr. Heatwole, the University of Rochester, and in the importance of helping find a cure for DM2 for our son and for the untold number of other people afflicted with this disease.
Researchers Identify Rare Neuromuscular Disease
Thursday, September 4, 2014
An international team of researchers has identified a new inherited neuromuscular disorder. The rare condition is the result of a genetic mutation that interferes with the communication between nerves and muscles, resulting in impaired muscle control.
The new disease was diagnosed in two families -- one in the U.S. and the other in Great Britain - and afflicts multiple generations. The discovery was published today in the American Journal of Human Genetics.
This discovery gives us new insight into the mechanisms of diseases that are caused by a breakdown in neuromuscular signal transmission,
said David Herrmann, M.B.B.Ch., a professor in the Department of Neurology at the University of Rochester School of Medicine and Dentistry and co-lead author of the study. It is our hope that these findings will help identify new targets for therapies that can eventually be used to treat these diseases.
Researchers Receive $3.4 million to Study Experimental Drug Combination in HIV
Thursday, August 28, 2014
Researchers at the University of Rochester Medical Center and University of Nebraska Medical Center have received a $3.4 million grant from the National Institutes of Health to study an experimental drug combination that appears to rid white blood cells of HIV and keep the infection in check for long periods. While current HIV treatments involve pills that are taken daily, the experimental drugs’ long-lasting effects suggest the possibility of an HIV treatment that could be administered monthly, or perhaps a few times a year.
Stem Cell Therapies Hold Promise, But Obstacles Remain
Thursday, August 21, 2014
In an article appearing online today in the journal Science, a group of researchers, including University of Rochester neurologist Steve Goldman, M.D., Ph.D., review the potential and challenges facing the scientific community as therapies involving stem cells move closer to reality.
The review article focuses on pluripotent stem cells (PSCs), which are stem cells that can give rise to all cell types. These include both embryonic stem cells, and those derived from mature cells that have been reprogrammed
or induced
- a process typically involving a patient's own skin cells -- so that they possess the characteristics of stem cells found at the earliest stage of development. These cells can then be differentiated, through careful manipulation of chemical and genetic signaling, to become virtually any cell type found in the body.
The article addresses the current state of efforts to apply PSCs to treat a number of diseases, including diabetes, liver disease, and heart disease. Goldman, a distinguished professor and co-director of the University of Rochester School of Medicine and Dentistry Center for Translational Neuromedicine, reviewed the current state of therapies for neurological diseases.
Suburban Outlaw: Total (Lack of) Recall
Monday, August 18, 2014
Mark Mapstone, an associate professor of neurology, says the best thing people can do for their brains as they age is to take care of their physical health.
Mapstone explained that we remember stories from our past so well because we've practiced remembering them by calling them up over the years and sharing them with others. Recent memories aren't as sticky for a lot of reasons, including how well we pay attention in the moment and even how much stress we have in our lives. So, in addition to eating right and exercise to cultivate a better memory, Dr. Mapstone advises something simple: Pay attention. What a concept.
Dr. Jonathan Mink Appears on ABC’s 20/20 to Discuss Tourette Syndrome in Athletes
Friday, August 15, 2014
Jonathan Mink, M.D., Ph.D., Frederick A. Horner, MD Endowed Professor in Pediatric Neurology, appeared on ABC's 20/20 on August 15the to discuss Tourette Syndrome in athletes and whether it gives them an advantage. Mink, who specializes in Tourette syndrome and other movement disorders at the University of Rochester, and is the co-chair of the National Tourette Syndrome Association's scientific advisory board, is more skeptical, citing conflicting studies. He said the science isn't there yet to definitively prove that Tourette's can help give athletes with the condition superior skills or make, say, a basketball player the next Lebron James.
The studies that have been done of people where actually measuring their movements, measuring how fast their movements are and the reaction times show that on average, people with Tourette Syndrome are about the same as people without,
Mink said.
Parkinson's Disease May Worsen Depression
Friday, August 15, 2014
A push from Parkinson’s disease could have put Robin Williams at risk of a perfect storm
of depression, medical experts said Thursday.
Although the disease is best known for its deleterious effects on the nerve cells that produce dopamine, a neurotransmitter that facilitates movement, Parkinson’s also affects a host of other chemical messengers, including serotonin and norepinephrine, which may explain why patients are more likely to develop depression.
The good news is that Parkinson’s-related depression responds well to currently available antidepressants that pump up the amount of serotonin and norepinephrine circulating in the brain, said Dr. Irene Richard, a professor of neurology and psychiatry at the University of Rochester Medical Center and a science adviser to the Michael J. Fox Foundation for Parkinson’s Research.
The bad news: Often doctors and even patients themselves do not recognize the depression. It’s just too easy to say that the patient is down because of the diagnosis, Richard said. Further, Parkinson’s and depression have overlapping symptoms, such as a blank facial expression and a monotone voice, she explained.
University Doctor to Cycle Across the U.S. for ALS
Thursday, August 14, 2014
Neurology's own Carly LaVigne (URMC Headache Center) is cycling across the USA in honor of her mother, Sally Hanan Oliver, who died of ALS at the age of 42. She will start her trip on August 24th in Astoria Oregon finishing 45 days later in Portland Maine. You can follow her progress at her 'Cycling for Sally' blog that Carly will keep throughout her journey. All proceeds raised will go to patient care services and support programs for the ALS clinic within our Division of Neuromuscular Disease.
UR Medicine Opens Doors on New NeuroMedicine ICU
Monday, July 28, 2014
UR Medicine today unveiled a new state-of-the-art unit dedicated to highly specialized care for people with serious and life-threatening neurological conditions, like strokes, seizures, brain and spinal tumors, and traumatic brain injury. The Neuromedicine Intensive Care Unit (ICU), which is the only unit of its kind in the region, is located on the eighth floor of Strong Memorial Hospital.
The $5.5 million, 5,500-square-foot unit consists of 12 beds and is staffed around the clock by an extended multidisciplinary team trained to treat the most challenging and difficult neurological disorders. The neurocritical care team members include neurointensivists, neurologists, neurosurgeons, physician assistants, nurse practitioners, critical care nurses, anesthesiologists, respiratory therapists, social workers, physical therapists, speech-language pathologists, occupational therapists, nutritionists, and clinical pharmacologists.
Diseases and injuries that impact the brain and central nervous system have a unique set of challenges and require expertise that is not commonly found in a traditional ICU setting. While brain function must be continuously monitored, providers also need to be trained to recognize that these conditions can potentially lead to other problems, such as cardiovascular, kidney, and respiratory complications or infections, particularly if a patient remains in an ICU setting for a long period of time. Also, once a patient has been stabilized, there must be continuity of care as they begin the process of recovery and transition to rehabilitation.
How Do You Identify Migraine Triggers?
Sunday, June 15, 2014
Do you know when a migraine is about to happen? Some are still trying to figure out what triggers a migraine since everyone is different. There are common triggers, which could be causing your migraines. Evan Dawson talked with Dr. Catherine LaVigne about these triggers and what you can do to find out what triggers your migraines. Dr. LaVigne is the former director of the URMC Headache Center, which is dedicated to providing the highest level of care for people who suffer from chronic headache disorders.
Profile of Excellence: Bob Holloway
Friday, June 13, 2014

Robert G. Holloway, M.D., M.P.H.
The 2013 Joynt Kindness Board Excellence Award in the Physician category is presented to Robert G. Holloway, M.D., M.P.H., the Edward A. and Alma Vollertsen Rykenboer Chair in Neurophysiology and Chair of the Department of Neurology.
Mark B. Taubman, M.D., dean of the URMC School of Medicine and Dentistry, calls Holloway the epitome of the academic 'triple threat.'
For his teaching excellence, Holloway has been recognized by his colleagues and students on numerous occasions. His role with the Clinical and Translation Science Institute, leadership of a NIH-funded research network for neurological disorders, and his authorship of numerous papers in publications like the New England Journal of Medicine and JAMA are testaments to his scientific contributions.
Holloway is also a true apostle of the principles of patient- and family-centered care, and it's for these principles that he is recognized with this award. He considers himself a general neurologist with broad interests in those serious neurological disorders that can greatly impact longevity and quality of life, including stroke, Parkinson's disease, dementia, multiple sclerosis, and epilepsy.
You can read the entire article here.
University Mourns the Loss of Nancy Benjamin
Friday, June 13, 2014

Nancy Benjamin (1960-2014)
University flags will be lowered June 19 in memory of Nancy Benjamin, administrative assistant in the Department of Neurology. Nancy joined the University staff in 1996. Her obituary appeared in the Democrat and Chronicle.
Nancy Benjamin died on May 31 at the age of 54 following a courageous struggle with metastatic cancer. She was my secretary, assistant and friend since 1996. Nancy was devoted to her work in our department and at the University. She ran the neurology clerkship and was instrumental in its becoming the best clinical clerkship at URSMD. She was always available to help Clara Vigelette with any resident related issues. She loved the residents and the medical students with whom she interacted. She always had a smile and enjoyed a good laugh.
Despite her medical problems, she came to work every day with a can-do attitude and refused to give in to her disease.
Nancy loved her children, Morgan and Adam, and was always so proud of them. She was a devoted daughter and was always there for her mother. She was a friend to so many staff at the University and was always willing to help out when asked.
Nancy was a very modest person and did not like any fuss. In place of a memorial service, she was remembered by her friends and family at a Happy Hour at McGinnity's Restaurant in Rochester last Friday. Nancy would have been so happy seeing all of her friends enjoying a beer in her memory.
Nancy touched the lives of everyone with whom she interacted. She was a gem of a person with a sincere devotion to her family, her friends, and her work. She will be terribly missed.
-Ralph F Józefowicz, MD
Medical Scientist Training Program Announces Leadership Changes
Sunday, May 18, 2014
The Medical Scientist Training Program (MSTP) in the School of Medicine will be undergoing leadership changes effective 7/1/14 with Marc Halterman, MD, PhD taking on the position of Associate Director.

Marc Halterman, MD, PhD
Douglas Turner, PhD, who has served the Program in many capacities since 1989, will be stepping down from his current position as Associate Director to take a well-deserved sabbatical. MSTP Director, Kerry O'Banion, MD, PhD commented, I am deeply indebted to Doug Turner for providing support and encouragement to me when I became Co-Director in 2000, and for his continued role as a key member of the MSTP Admissions Committee, thesis advisor, grant reviewer, and a clear example of the close relationship between the College and the Medical School. Notably, Doug has mentored six MSTP students in his laboratory. I wish him much success as he ventures into new areas of research inquiry.

Douglas Turner, PhD
Stepping into the MSTP Associate Director position on 7/1/14 will be Marc Halterman, MD, PhD. Dr. Halterman graduated from the MSTP at Rochester in 2002 and went on to complete a Neurology Residency and Research Fellowship at University of Rochester. He is now Associate Professor of Neurology and Pediatrics, and Director of the Neurology Academic Research Track, a research residency training program at University of Rochester. In addition, he serves on an NIH review panel for predoctoral NRSA (F) grants. Dr. Halterman has already generously given of his time serving the MSTP in several capacities. Since September 2011 he has acted as Course Director of MSTP-specific course Scientific Reasoning in Medicine. He joined the MSTP Admissions Committee in 2013 and is thesis advisor to one MSTP trainee conducting her PhD research in his laboratory. Dr. Halterman has also provided individual training and career advice to many MSTP students. As Associate Director, he will continue to be engaged in all of these activities and take on a broader role in helping trainees consider their options for research and residency selection. He will continue to serve as a member of the MSTP Admissions Committee and assist Dr. O'Banion in running an F30 Grant Writing Workshop for MSTP students.
Dr. O'Banion continued, I very much look forward to working with Marc Halterman as we enter a new five-year funded cycle of the MSTP training grant and prepare for the 40th anniversary celebration of MSTP funding in October, 2015.
The Doctor's in-Through Webcam, Smartphone
Tuesday, May 13, 2014
Mark Matulaitis holds out his arms so the Parkinson's specialist can check his tremors. But this is no doctor's office: Matulaitis sits in his rural Maryland home as a neurologist a few hundred miles away examines him via the camera in his laptop.
Welcome to the virtual house call, the latest twist on telemedicine. It's increasingly getting attention as a way to conveniently diagnose simple maladies, such as whether that runny nose and cough is a cold or the flu. One company even offers a smartphone app that lets tech-savvy consumers connect to a doctor for $49 a visit.
Why can't we provide care to people wherever they are?
asks Dr. Ray Dorsey, a neurologist at the University of Rochester Medical Center who is leading a national study of video visits for Parkinson's patients and sees broader appeal. Think of taking your mom with Alzheimer's to a big urban medical center. Just getting through the parking lot they're disoriented,
he adds. That's the standard of care but is it what we should be doing?
Drug Improves Vision in Individuals with Neurological Disorder
Tuesday, April 22, 2014
The drug acetazolamide, combined with a low-sodium weight reduction diet, improves vision in individuals with idiopathic intracranial hypertension (IIH), a condition brought about by abnormal pressure on the brain that is not the result of a tumor or other diseases.
he study, which appears this week in the journal JAMA, was coordinated by Karl Kieburtz, M.D. and Michael McDermott, Ph.D. with the University of Rochester's Center for Human Experimental Therapeutics (CHET) and also involved Steven Feldon, M.D. with the Flaum Eye Institute.
Global Burden of Neurological Diseases Requires New Approaches
Tuesday, April 22, 2014
A perspective piece appearing today in the journal JAMA focuses on the challenges and opportunities arising from the increasing global incidence of neurological disorders. The authors advocate for new approaches that will increase access, lower costs, influence lifestyle changes, and create international research and clinical partnerships that address overlooked neurological conditions and underserved global populations.
The piece is authored by University of Rochester School of Medicine and Dentistry neurologists Gretchen Birbeck, M.D. and Robert Griggs, M.D., and Michael Hanna, M.D. with University College London. Birbeck is also member of the Epilepsy Care Team at Chikankata Hospital in Mazabuka, Zambia.
Heart/Stroke Association Honors UR Medicine for Highest Quality Care
Tuesday, April 22, 2014
The American Heart Association/American Stroke Association (AHA/ASA) has once again recognized UR Medicine and its Strong Memorial Hospital for achieving its highest standards of care for stroke, heart failure, and resuscitation.
Strong Memorial Hospital has received the AHA/ASA Get With The Guidelines program’s highest honor, the Stroke Gold Plus Quality Achievement Award for a fifth consecutive year. The hospital was also tapped for the Target: Stroke Honor Roll, which recognizes hospitals that have consistently and successfully reduced door-to-needle time – the window of time between a stroke victim’s arrival at the hospital, the diagnosis of an acute ischemic stroke, and the administration of the clot-busting drug tPA.
“We are proud to earn this recognition, however we continue to work to improve time-to-treatment for people who are suffering a stroke. Early treatment is proven to preserve brain function and enhance recovery for each patient,” said neurologist Curtis Benesch, M.D., M.P.H., medical director of the UR Medicine Comprehensive Stroke Center.
Researchers Set to Launch Phase 3 Trial for Parkinson’s
Wednesday, April 2, 2014
A $23 million grant from the National Institutes of Health will support a new Phase 3 clinical trial to evaluate the drug isradipine as a potential new treatment for Parkinson’s disease. The study is being co-lead by the University of Rochester and Northwestern University.
Isradipine has been demonstrated to be safe and tolerable in patients with Parkinson’s disease,
said University of Rochester School of Medicine and Dentistry neurologist Kevin Biglan, M.D., M.P.H., co-principal investigator of the study. This new study will determine whether the drug can be an effective tool in slowing the progression of the disease and could, thereby, complement existing symptomatic treatments and improve the quality of life of individuals with the disease.
UR Medicine Helps Forge National Stroke Care Guidelines
Friday, March 28, 2014
A new statement from the American Heart Association (AHA) recommends that people recovering from a severe stroke receive tailored and coordinated care that optimizes quality of life and minimizes suffering. The statement -- which was published today in the journal Stroke -- represents the first attempt to establish a fundamental set of recommendations that can help guide physicians, patients, and their families through the difficult decisions that arise from this condition.
The majority of stroke patients require access to some form of palliative care,
said Robert Holloway, M.D., M.P.H., the chair of the Department of Neurology at the University of Rochester School of Medicine and Dentistry. Accomplishing this requires that a hospital's system of stroke care and its team of providers place the patient and their family at the center of the decision-making process and build a plan of care that is based on their values and informed by effective and constant communication.
Stroke Survivors Deserve Team Care
Thursday, March 27, 2014
Palliative care that minimizes suffering and improves quality of life should be provided to patients who've survived
a stroke, experts say. The care should be a team effort involving patients, families, stroke specialists and health
care providers such as neurosurgeons, neurologists, primary care doctors, nurses and therapists, according to the
new scientific statement from the American Heart Association (AHA) and American Stroke Association (ASA).
The majority of stroke patients need access to some form of palliative medicine,
statement lead author Dr. Robert Holloway, chairman of the neurology department at the University of Rochester Medical Center in Rochester,
N.Y., said in an AHA/ASA news release.
The stroke team and its members can manage many of the palliative care problems themselves. It encourages
patient independence and informed choices,
he explained.
Biomarker Points to Alzheimer’s Risk
Monday, March 10, 2014
A study involving Rochester-area seniors has yielded the first accurate blood test that can predict who is at risk for developing Alzheimer’s disease. This discovery – which appears today in the journal Nature Medicine – could be the key to unlocking a new generation of treatments that seek to head off the disease before neurological damage becomes irreversible.
The biomarker – which consists of 10 specific lipids found in blood plasma – predicted with greater than 90 percent accuracy which individuals would go on to develop Alzheimer’s disease or a precursor condition known as amnestic mild cognitive impairment (aMCI). The cost of the simple blood test required to detect these lipids is a fraction of other techniques and, unlike alternatives, it identifies risk early in the disease process before cognitive symptoms appears.
The ability to identify individuals who are at risk of developing Alzheimer’s before the clinical manifestation of cognitive impairment has long been a Holy Grail of the neuromedicine community,
said Mark Mapstone, Ph.D., a neuropsychologist with the University of Rochester School of Medicine and Dentistry and lead author of the study. Current efforts to develop a treatment for this disease are coming up short because they are probably being used too late. Biomarkers that can allow us to intervene early in the course of the disease could be a game-changer.
Dr. Laurie Seltzer Receives Award from Journal of Pediatric Neurology for the 2013 Best Paper
Wednesday, February 26, 2014
The Department of Neurology is pleased and proud to announce that Dr. Laurie Seltzer, DO, Senior Instructor of Child Neurology and Epilepsy recently received an award from the editors of Pediatric Neurology for the best paper submitted in 2013 by a resident or fellow. The paper, Intraoperative EEG Predicts Postoperative Seizures in Infants with Congenital Heart Disease was published online on December 23rd 2013 and will also appear in a forthcoming print issue of the journal. The research was supported in part by a NIH Institutional Research and Academic Career Development Award (K12 NS 066098).
In this prospective, observational study, Dr. Seltzer and her co-investigators reviewed preoperative, intraoperative and postoperative EEG of 32 infants who underwent cardiac surgery. Among 17 of the children, the surgery involved deep hypothermic circulatory arrest (DHCA). Specific intraoperative EEG patterns seen in two patients undergoing prolonged DHCA were predictive of postoperative seizure within 2 days after surgery. The results suggest that the intraoperative EEG may be used not only as a tool for monitoring current status during surgery, but also as a predictive tool to determine risk for postoperative seizure in infants undergoing surgery with DHCA.
Dr. Seltzer's accomplishment will be recognized at the 2014 Child Neurology Society Meeting in Columbus, OH.
UR Medicine Recognized for Stroke Care, Launches Neurocritical Care Program
Tuesday, February 4, 2014
Strong Memorial Hospital has been recognized by The Joint Commission and the American Heart Association/American Stroke Association as a Comprehensive Stroke Center. This designation, which has only been conferred on two other hospitals in New York State, places Strong among an elite group of institutions that provide highly-specialized complex stroke care.
"We are proud that the Joint Commission has recognized our dedicated team of neurologists, neurosurgeons, radiologists, emergency department physicians, nurses, therapists, and staff," said neurologist Curtis Benesch, M.D., M.P.H., the medical director of the URMC Stroke and Cerebrovascular Center. This certification is a testament to their commitment to provide the highest and most comprehensive level of stroke care to our community.
Goodnight. Sleep Clean.
Saturday, January 11, 2014
Sleep seems like a perfectly fine waste of time. Why would our bodies evolve to spend close to one-third of our lives completely out of it, when we could instead be doing something useful or exciting? Something that would, as an added bonus, be less likely to get us killed back when we were sleeping on the savanna?
Sleep is such a dangerous thing to do, when you’re out in the wild,
Maiken Nedergaard, a Danish biologist who has been leading research into sleep function at the University of Rochester’s medical school, told me. It has to have a basic evolutional function. Otherwise it would have been eliminated
.
To read more please see the NY Times article.
Workshop on JNCL Clinical Trials Outcomes
Wednesday, December 18, 2013
There are a number of recent and ongoing clinical trials in Batten Disease. Most of these are focused on asking if
these potential new treatments are safe. After safety studies are completed, the next stage of clinical trials
research is to learn if these or other interventions are effective. In order to answer this question, we will need a
way to measure whether or not an intervention actually makes a meaningful difference in disease course.
Therefore, the URBC hosted a workshop titled, Outcome Measures and Infrastructure for Phase III Studies in JNCL
(December 6-7, 2013). The workshop brought together experts in the clinical features of JNCL, experts from other
fields (clinical trials in rare diseases, statistics, etc.), and Batten family representatives. Each expert was
invited to bring trainee to accompany him/her, so that we can continue cultivating the next generation of
researchers who are focused on Batten Disease. Our goals were to:
- Identify possible outcome measures for future clinical trials
- Develop a roadmap for further research to test and refine outcome measures
- Strengthen research collaborations to support outcome measure development
Film Screening and Q&A on Huntington's Disease
Wednesday, December 11, 2013
There will be a film screening of the documentary Alive & Well followed by a Q&A with Kevin Biglan, neurologist and codirector of the Huntington's Disease Society of America Center of Excellence at the Medical Center. The screening starts at 7 p.m. Monday, Dec. 16 at the Little Theatre. Biglan will be joined by Billy Lawler, a former Rochester police officer and founder of Bill Lawler Annual Huntington's 5K. View the film trailer and purchase tickets in advance.
Jones Memorial and URMC Expand Neurology and Cardiology Services
Tuesday, December 10, 2013
Jones Memorial Hospital is expanding its collaboration with the University of Rochester Medical Center through new neurology and cardiology services in Wellsville, NY. URMC neurologists Richard Welles, M.D. and Su Kanchana, M.D., Ph.D., and internist Linda Welles, M.D. began seeing patients at the hospital beginning December 3.
Richard Welles is board certified in Psychiatry, Neurology, and Electrodiagnostic Medicine, and will offer on-site evaluation and treatment of neurological disorders. Kanchana is board certified in Psychiatry and Neurology, and specializes in treatment of adult movement disorders such as Parkinson's disease. Linda Welles is board certified in Internal Medicine and Geriatrics and specializes in gait and balance and geriatric disorders.
We are very pleased to be able to offer neurological care to patients in Wellsville and beyond,
said Eva Benedict, CEO of Jones Memorial Hospital. This collaboration between Jones Memorial and URMC will enable patients to access the necessary specialized care right here in our own community.
Telemedicine Brings Parkinson’s Care to Anyone, Anywhere
Wednesday, December 4, 2013
A new study shows that a neurologist in an office thousands of miles away can deliver effective specialized care to people with Parkinson’s disease. For individuals with the condition – many of whom have never seen a specialist – these virtual house calls
could allow them to live independently while effectively managing the symptoms of the disease.
The idea that we can provide care to individuals with Parkinson’s disease regardless of where they live is both a simple and revolutionary concept,
said University of Rochester Medical Center (URMC) neurologist Ray Dorsey, M.D., M.B.A., senior author of the study which appears today in the journal Neurology: Clinical Practice. This study demonstrates that, by employing essentially the same technology that grandparents use to talk to their grandchildren, we can expand access to the specialized care that we know will improve patients’ quality of life and health.
URMC Plays Role in New Epilepsy Technology
Monday, December 2, 2013
Physicians at the University of Rochester Medical Center (URMC) Strong Epilepsy Center were involved in the recent approval of a new treatment for epilepsy. The implantable medical device - called the Responsive Neurostimulator System (RNS) - monitors brain activity and can detect and counteract seizures.
URMC was one of only 28 sites in the country to conduct clinical trials of RNS, which was developed by the California-based company Neuropace. The research showed that the device decreases the number of monthly seizures by nearly 38 percent. URMC neurologists Michel Berg, M.D. and James Fessler, M.D., and neurosurgeon Web Pilcher, M.D., Ph.D. were involved in the study.
This is the first FDA-approved brain implant for epilepsy that responds to the brain's activity,
said Berg, an associate professor of Neurology. For patients who are unable to control their seizures with medications or are not eligible for resective surgery, this device could provide an important treatment option.
Neurology for the Primary Care Provider
Wednesday, November 27, 2013
The continuing medical education activity Neurology for the Primary Care Provider is scheduled for Thursday, Dec. 12. The program highlights the most recent diagnostic and treatment advances in the field of neurology. The conference runs from 8:30 a.m. to 4:15 p.m. in the School of Medicine and Dentistry.
Now it its twentieth year, Neurology for the Primary Care Provider continues to attract a large audience of clinicians who manage patients with acute and chronic neurologic disorders in diverse settings. Each year, over 100 health care professionals - approximately one half of whom are physicians - attend this conference. The program highlights the most recent diagnostic and treatment advances in the field of neurology, utilizing a highly interactive case-based format.
Drug Shows Early Promise in Treating Liver Failure-Related Seizures
Sunday, November 17, 2013
A study out today in the journal Nature Medicine suggests a potential new treatment for the seizures
that often plague children with genetic metabolic disorders and individuals undergoing liver failure. The
discovery hinges on a new understanding of the complex molecular chain reaction that occurs when the brain is
exposed to too much ammonia.
The study shows that elevated levels of ammonia in the blood overwhelm the brain's defenses, ultimately
causing nerve cells to become overexcited. The researchers have also discovered that bumetanide - a
diuretic drug used to treat high blood pressure - can restore normal electrical activity in the brains of
mice with the condition and prevent seizures.
Ammonia is a ubiquitous waste product of regular protein metabolism, but it can accumulate in toxic levels
in individuals with metabolic disorders,
said
Maiken Nedergaard, M.D., D.M.Sc.,
co-director of the University of Rochester Medical Center (URMC)
Center for Translational Neuromedicine and lead author of the
article. It appears that the key to preventing the debilitating neurological effects of ammonia toxicity is to correct a molecular malfunction which causes nerve cells in the brain to become chemically unbalanced.
Clinical Trial for Children with Juvenile Neuronal Ceroid Lipofuscinosis (JNCL)
Friday, November 1, 2013
The University of Rochester Medical Center is currently recruiting subjects with JNCL for a clinical trial. This research study will focus on evaluating whether an investigational drug is safe and well tolerated in children with JNCL. Mycophenolate mofetil (also known as Cellcept) is a medication that suppresses the immune system. The study is 22 weeks long with a total of 8 in-person visits and 4 telephone contacts. Four visits require travel to University of Rochester Medical Center in Rochester, New York, and four visits are with your child’s local physician. Four contacts take place by telephone. Travel costs are covered by the study. Children enrolled in the study will take mycophenolate syrup twice a day, and will have blood drawn at each study visit to monitor safety.
More information on the trial can be found at ClinicalTrials.gov, Time Warner Cable News (Rochester, NY television affiliate) and the URMC Newsroom.
For further information, please contact Amy Vierhile at (585) 275-4762.
URMC Expands Neuromedicine Teams for Rochester, Ithaca, Southern Tier
Tuesday, October 29, 2013
Four neuromedicine specialists have joined the University of Rochester Medical Center, enhancing programs for traumatic injury, cerebrovascular, spine and Parkinson's care.
Manjunath Markandaya, M.B.B.S., was named chief of the division of neurocritical care and assistant professor of Neurosurgery, Neurology and Medicine. He specializes in caring for some of the most challenging and critically ill neurosurgical and neurological patients.
James C. Metcalf Jr., M.D., was named assistant professor of Neurosurgery and serves Cayuga Medical Center in Ithaca. He specializes in spine disorders and cancer care.
Su Kanchana, M.D., Ph.D., a neurologist, was named assistant professor of Neurology and serves patients in the Southern Tier Neuromedicine office in Big Flats as well as in Rochester at 919 Westfall Road, Building C. She specializes in the diagnosis and management of complex movement disorders, with emphasis on Parkinson's disease, deep brain stimulation and Botulinum toxin therapy.
Amrendra Singh Miranpuri, M.D., joined the team as an assistant professor of Neurosurgery. He specializes in open and interventional neurosurgical procedures for cerebrovascular disease. He is also the surgical co-director of the Neuromedicine Critical Care Program.
URMC's neuromedicine programs - Neurosurgery and Neurology - are ranked 29th best in the nation by U.S. News & World Report.
Sleep 'Cleans' the Brain of Toxins
Thursday, October 17, 2013
The US team believe the waste removal system
is one of the fundamental reasons for sleep. Their study, in the journal Science, showed brain cells shrink during sleep to open up the gaps between neurons and allow fluid to wash the brain clean. They also suggest that failing to clear away some toxic proteins may play a role in brain disorders.
One big question for sleep researchers is why do animals sleep at all when it leaves them vulnerable to predators? It has been shown to have a big role in the fixing of memories in the brain and learning, but a team at the University of Rochester Medical Centre believe that housework
may be one of the primary reasons for sleep.
The brain only has limited energy at its disposal and it appears that it must choose between two different functional states - awake and aware or asleep and cleaning up,
said researcher Dr Maiken Nedergaard. You can think of it like having a house party. You can either entertain the guests or clean up the house, but you can't really do both at the same time.
Doctor Left Behind Story in Search of Ending
Wednesday, September 25, 2013
We live in the new age of Sherlock Holmes, what with movie and television versions of Sir Arthur Conan Doyle's moody but brilliant detective popping up like foggy nights in London town.
But it would seem that the late Dr. Robert J. Joynt, the former dean of the University of Rochester School of Medicine and Dentistry and an internationally recognized neurologist, was ahead of the Holmes revival. In addition to his formidable record of academic publication, Joynt, a Pittsford resident who died in April 2012 at age 86, had begun to turn out a series of short stories, five of which were published in Neurology, a medical journal.
Each mystery featured Holmes and his sidekick Dr. Watson confronted with a puzzler that had a solution grounded in neurology, the study of the nervous system. Joynt's sixth, and presumably last, Holmes mystery was found unfinished on his computer after his death.
Now the editors of Neurology are asking readers to complete the neurologist's story in 1,500 words or less. The winning entry will be published in Neurology. The author of the new material will share credit with Joynt. The uncompleted mystery and the contest rules can be found by going to Neurology.org and searching for The Case of the Locked House,
the title of the incomplete story. (When you get to the story, click on Full Text.)
Michael J. Fox Still Pushing to Find Parkinson's Cure
Tuesday, September 24, 2013
Actor Michael J. Fox once predicted that he would be cured of Parkinson disease's long before his 50th birthday. I know I won't have this. I will not have it,
he told Barbara Walters on national television. Now, 52, Fox is far from cured.
In a way, not much has changed in the 15 years since Fox first publicly acknowledged that he had the disease and the 22 years since his diagnosis. Most patients still rely on a medication, levodopa, first tested on Parkinson's the year Fox was born. In other ways and much to Fox's credit, many people say our understanding of the disease has been transformed since his diagnosis, bringing research closer to a cure even as scientists acknowledge that it will be far harder to achieve than they once believed.
Still, the only major new treatment in the last two decades is deep-brain stimulation, in which electrodes are implanted inside the brain to partially override the distorted signals that lead to the disease's tremors, stiffness and slowness. Like L-dopa, it only treats symptoms, and can't slow or stop the disease. Another recent advance, according to Irene Richard, a neurologist at the University of Rochester, is the attention now being paid to the emotional and mental toll of Parkinson's. Roughly half of Parkinson's patients are depressed, likely as a symptom of the condition.
Copper Identified as Culprit in Alzheimer's Disease
Monday, August 19, 2013
Copper appears to be one of the main environmental factors that trigger the onset and enhance the progression of Alzheimer's disease by preventing the clearance and accelerating the accumulation of toxic proteins in the brain. That is the conclusion of a study appearing today in the journal Proceedings of the National Academy of Sciences.
It is clear that, over time, copper's cumulative effect is to impair the systems by which amyloid beta is removed from the brain,
said Rashid Deane, Ph.D., a research professor in the University of Rochester Medical Center Department of Neurosurgery, member of the Center for Translational Neuromedicine, and the lead author of the study. This impairment is one of the key factors that cause the protein to accumulate in the brain and form the plaques that are the hallmark of Alzheimer's disease.
Kieburtz Appointed to Oversee URMC Clinical Research
Friday, August 9, 2013
Karl Kieburtz, M.D., M.P.H. has been tapped to serve as director of the University of Rochester Medical Center (URMC) Clinical and Translational Science Institute (CTSI) and to serve as the senior associate dean for Clinical Research. The appointment will be effective September 1, 2013.
As one of the leading academic experts in the design and operation of clinical trials, Dr. Kieburtz is the obvious choice to build upon the Medical Center’s history as an innovative national leader in the field of experimental therapeutics and translational medicine,
said Mark Taubman, M.D., dean of the URMC School of Medicine and Dentistry. We are deeply grateful that he has accepted this new leadership role and I look forward to working with him to continue to strengthen and grow our clinical research enterprise.
New Neurology Appointments to Focus on Expanding Access at Home and Abroad
Thursday, August 1, 2013
Gretchen Birbeck, M.D., M.P.H., and E. Ray Dorsey, M.D., M.B.A., have joined the University of Rochester Medical Center (URMC) Department of Neurology effective August 1. Birbeck, an epilepsy specialist, and Dorsey, a movement disorders specialist, will both focus on the global burden of neurological disorders and efforts to expand access to underserved populations.
The number of people with neurological disorders will grow at a rapid pace over the next several decades,
said Robert G. Holloway, Jr., M.D., M.P.H., chair of the URMC Department of Neurology. Expanding access to specialized care to patients in both the U.S. and the developing world will be one of the key challenges facing medicine. Drs. Birbeck and Dorsey are leaders and innovators in this field and we are thrilled to have them join our department.
Holloway Appointed New Chair of Neurology
Thursday, July 25, 2013
Robert G. Holloway, Jr., M.D., M.P.H. has been tapped as the next chair of the University of Rochester Medical Center (URMC) Department of Neurology. Holloway had been serving as interim chair of the department since last July and his permanent appointment is effective immediately.
Dr. Holloway is the epitome of the academic 'triple threat,'
said Mark Taubman, M.D., dean of the University of Rochester School of Medicine and Dentistry. His skills as a physician, researcher, and educator will enable the department to grow and meet the twin challenges of health care reform and an increasingly competitive national environment for research funding. Bob has played an integral role in many of the Medical Center's signature initiatives and I am deeply grateful that he has agreed to take on this new responsibility and lead the Department of Neurology.
In addition to his position in Neurology, Holloway is also a professor of Public Health Sciences, director of the Research, Education, and Career Development Function of the URMC Clinical and Translational Science Institute (CTSI), and principal investigator of the URMC's NIH-funded NeuroNEXT clinical research program.
Neurology and Neurosurgery Ranked as One of Best in Nation
Tuesday, July 16, 2013
Chair of Neurology, Robert Holloway, Jr., M.D., M.P.H. and Chair of Neurosurgery, Webster H. Pilcher, M.D., Ph.D.
When US News & World Report's 2014 Best Hospitals guidebook hits newsstands today, a record number of six University of Rochester Medical Center specialties will be ranked among the very best in the nation. That's the highest number of URMC programs ever to earn a seat in the magazine's list of the nation's top 50 in a single year, since US News began ranking hospitals in 1989.
The URMC adult specialties nationally ranked included Neurology and Neurosurgery as the 29th best. URMC's success in the U.S. News rankings reflects the hard work that our faculty and staff have invested to continuously improve quality, patient safety and satisfaction. It also reflects URMC's growing reputation for first-rate care,
said URMC CEO Bradford C. Berk, M.D., Ph.D.
Profile of Excellence: Unit 5-1600 Team Pioneers in Providing Exceptional Care to Patients and Families
Sunday, June 30, 2013
For their commitment to patient safety and satisfaction, the nursing staff in the Neurology
Inpatient Unit (5-1600) received a 2012 Board Excellence Award in the team category.
A key to the team's success has been their relentless focus on improving communication - both
among caregivers and with patients and their families. This goes far beyond the routine communication
between residents, attending physicians, and nurses as they hand off care during a shift change, to
include hourly huddles
among nursing staff to review patient status, and regular rounding by
nursing staff to check with patients and their families, ensuring that all of their needs are being met.
And, at the prodding of the nursing staff, attending physicians now round at a consistent time each
morning, so the families can plan to participate. Once daily, too, the unit's nurses, therapists,
social workers, and residents all come together to plan the day and develop comprehensive discharge
plans for patients leaving the hospital.
Our unit is home to one of the most challenging patient populations in the hospital, and
delivering timely and effective care requires a multidisciplinary team effort,
said
Todd Holmquist, M.D.,
the medical director of the Neurology Inpatient Unit. This requires cohesion, leadership,
accountability, and - above all - constant communication among providers.
Brain's 'Garbage Truck' May Hold Key to Treating Alzheimer's and Other Disorders
Thursday, June 27, 2013
In a perspective piece appearing today in the journal Science, researchers at University of Rochester Medical Center point to a newly discovered system by which the brain removes waste as a potentially powerful new tool to treat neurological disorders like Alzheimer's disease. In fact, scientists believe that some of these conditions may arise when the system is not doing its job properly.
Essentially all neurodegenerative diseases are associated with the accumulation of cellular waste products,
said Maiken Nedergaard, M.D., D.M.Sc., co-director of the URMC Center for Translational Neuromedicine and author of the article. Understanding and ultimately discovering how to modulate the brain's system for removing toxic waste could point to new ways to treat these diseases.
The body defends the brain like a fortress and rings it with a complex system of gateways that control which molecules can enter and exit. While this blood-brain barrier
was first described in the late 1800s, scientists are only now just beginning to understand the dynamics of how these mechanisms function. In fact, the complex network of waste removal, which researchers have dubbed the glymphatic system, was only first disclosed by URMC scientists last August in the journal Science Translational Medicine.
Neurologists Win Provost’s Multidisciplinary Award
Friday, June 14, 2013
Five diverse research projects at the University were selected as recipients of the sixth annual Provost's Multidisciplinary Awards. The initiative provides $250,000 each year to support faculty research that crosses disciplines. Among the recipients were Neurology professors, Jonathan Mink and Marc Schieber. Their project, entitled, Task-Specific Dystonia in Musicians is a collaboration with Ralph Manchester, in Medicine and Nicholas Goluses (Strings) and Peter Kurau (Woodwind, Brass & Percussion) at the Eastman School of Music.
Huntington's Brain Cells Regenerated, in Mice
Thursday, June 6, 2013
Huntington's disease, like other neurodegenerative diseases such as Parkinson's, is characterized by the loss of a particular type of brain cell. This cell type has been regenerated in a mouse model of the disease, in a study led by University of Rochester Medical Center scientists.
Mice whose received this brain regeneration treatment lived far longer than untreated mice. The study was published online Thursday in Cell Stem Cell.
We believe that our data suggest the feasibility of this process as a viable therapeutic strategy for Huntington's disease,
said senior study author Steve Goldman, co-director of Rochester's Center for Translational Neuromedicine, in a press release.
Researchers Identify Genetic Signature of Deadly Brain Cancer
Monday, June 3, 2013
A multi-institutional team of researchers have pinpointed the genetic traits of the cells that give rise to gliomas -- the most common form of malignant brain cancer. The findings, which appear in the journal Cell Reports, provide scientists with rich new potential set of targets to treat the disease.
This study identifies a core set of genes and pathways that are dysregulated during both the early and late stages of tumor progression," said University of Rochester Medical Center neurologist Steven Goldman, M.D., Ph.D., the senior author of the study and co-director of the Center for Translational Neuromedicine. "By virtue of their marked difference from normal cells, these genes appear to comprise a promising set of targets for therapeutic intervention.
URMC Honored for Stroke, Cardiac Programs
Tuesday, May 28, 2013
The American Heart Association/American Stroke Association (AHA/ASA) has once again recognized the University of Rochester Medical Center's (URMC) Strong Memorial Hospital as having met its highest standards of care for stroke, heart failure, and resuscitation.
This is the fourth consecutive year that Strong Memorial Hospital has received the AHA/ASA Get With The Guidelines program's highest honor, the Stroke Gold Plus Quality Achievement Award. The hospital was also tapped for the Target: Stroke Honor Role, which recognizes hospitals that have consistently and successfully reduced door-to-needle time -- the window of time between a stroke victim's arrival at the hospital, the diagnosis of an acute ischemic stroke, and the administration of the clot-busting drug tPA.
"This recognition is a testament to the hard work of our outstanding team of nurses, physicians, and therapists and their dedication to provide the highest quality of care to stroke victims," said URMC neurologist Curtis Benesch, M.D., Ph.D., the director of the Strong Stroke and Cerebrovascular Center.
Symposium Aims to Get Parkinson's Community Moving
Monday, May 13, 2013
URMC neurologists are participating in a daylong symposium that brings together local Parkinson's disease patients and nationally recognized movement disorders researchers, clinicians, and physical therapists to discuss the latest advances in research and treatment for the disease.
The symposium will be held on Saturday, May 18, 2013 from 10:00 AM to 4:15 PM at the Radisson Rochester Riverside Hotel. The event is free and open to the public.
"The Victory Summit is a fantastic opportunity to share the many ways in which individuals with Parkinson's can alter the course of the disease," said Michelle Burack, M.D., Ph.D., assistant professor in the URMC Departments of Neurology and Pediatrics. Things like daily physical activity, paying attention to mental well-being, and maintaining social connectedness are powerful 'medicine' for the brain, and are vital components of optimum management for this chronic condition.
Vietnam Veterans Could Hold Clue to Future for Today’s Soldiers
Thursday, April 25, 2013
Since 2001, more than two million service members have been deployed in Iraq and Afghanistan, and studies indicate nearly a third of them have suffered traumatic brain injury (TBI), post-traumatic stress disorder (PTSD), or both. The University of Rochester Medical Center is part of an investigation into whether these injuries put the soldiers at greater risk for a future battle -- against Alzheimer’s Disease. As they begin the study, researchers are turning to veterans of the Vietnam War for help.
"In order to predict what might happen, we wanted to look at a cohort that is about 40 years older to see what the brains of those individuals look like," says Anton P. Porsteinsson, M.D., who is overseeing the study at URMC. "Nobody paid much attention to this back in the Vietnam era, but do TBI and PTSD impact your risk of memory disease? Could this point toward additional studies into treatment and prevention of the long-term effects of these injuries?"
Stroke Survivors Share Experiences During March 28 Seminar
Monday, March 25, 2013
A three-time stroke survivor, whose perseverance allowed her to work, maintain her busy household and be courageous enough to take karate and surfing lessons, is among the speakers at a seminar for stroke survivors on Thursday, March 28, at the Hyatt Regency.
Christina Goodermote will share her personal story and lessons learned after surviving a stroke, at 39. The Chili woman will be joined by fellow survivor Lucy Sebastian during the Stroke Treatment Alliance of Rochester's community education event from 8:30 a.m. to 1:30 p.m. Registration is required for the free event, call 585-275-8344. Space is limited.
The Stroke Treatment Alliance of Rochester, or STAR, is a collaborative effort by University of Rochester Medical Center's Strong and Highland hospitals, Unity Hospital and Rochester General Hospital to improve and unify stroke care and raise awareness of the warning signs for this potentially devastating health emergency.
This initiative is led by URMC neurosurgeon Babak Jahromi, M.D., Ph.D., and neurologist Curtis Benesch, M.D., M.P.H., and funded by the Greater Rochester Health Foundation.
URMC Neuromedicine Pain Center Gets National Recognition for Excellence in Care
Monday, March 25, 2013
The Neuromedicine Pain Management Center at the University of Rochester Medical Center's Department of Neurosurgery was recently honored for its outcomes, multidisciplinary care and research by the American Pain Society, the leading organization dedicated to advancing pain care.
URMC was named a Clinical Center of Excellence for pain management, the only academic medical center in the nation to earn designation this year. To date, the APS has recognized just 20 academic medical centers in the country, and URMC is the only site in Upstate New York. People would have to travel to New York City or Cleveland for similar quality care.
The APS designation followed a rigorous review of the center’s systems, clinical and research innovation, commitment to education and leadership within the community.
‘Virtual’ House Calls for Parkinson’s Patients Effective
Monday, March 11, 2013
A study out today in the journal JAMA Neurology shows that telemedicine check-ups for people with Parkinson's disease can not only provide effective care but also generate a significant economic benefit. These 'virtual' visits with physicians -- in which the patient participates from the comfort of their own home -- demonstrate that quality specialized care can be effectively delivered to individuals in remote locations.
"This study shows that providing specialty care to people with Parkinson's disease directly into their homes is feasible, saves patients substantial time and travel, and may offer comparable clinical benefits to in-person care," said University of Rochester Medical Center neurologist Kevin Biglan, M.D., M.P.H., the senior author of the study.
NPR Features Current Nedergaard-Goldman Publication; Glial Research
Thursday, March 7, 2013
A human glial cell (green) among normal mouse glial cells (red). The human cell is larger, sends out more fibers and has more connections than do mouse cells. Mice with this type of human cell implanted in their brains perform better on learning and memory tests than do typical mice.
For more than a century, neurons have been the superstars of the brain. Their less glamorous partners, glial cells, can't send electric signals, and so they've been mostly ignored. Now scientists have injected some human glial cells into the brains of newborn mice. When the mice grew up, they were faster learners. The study, published Thursday in Cell Stem Cell by Maiken Nedergaard, M.D., D.M.Sc. and Dr. Steven Goldman, M.D., Ph.D., not only introduces a new tool to study the mechanisms of the human brain, it supports the hypothesis that glial cells - and not just neurons - play an important role in learning.
Today, glial research and Dr. Goldman were featured on National Public Radio (NPR) speaking about the glial research that is outlined in this current publication. I can't tell the differences between a neuron from a bird or a mouse or a primate or a human,
says Goldman, glial cells are easy to tell apart. Human glial cells - human astrocytes - are much larger than those of lower species. They have more fibers and they send those fibers out over greater distances.
In collaboration with the Nedergaard Lab, newborn mice had some human glial cells injected into their brains. The mice grew up, and so did the human glial cells. The cells spread through the mouse brain, integrating perfectly with mouse neurons and, in some areas, outnumbering their mouse counterparts. All the while Goldman says the glial cells maintained their human characteristics.
Support Cells Found in Human Brain Make Mice Smarter
Thursday, March 7, 2013
Glial cells -- a family of cells found in the human central nervous system and, until recently, considered mere housekeepers
-- now appear to be essential to the unique complexity of the human brain. Scientists reached this conclusion after demonstrating that when transplanted into mice, these human cells could influence communication within the brain, allowing the animals to learn more rapidly.
The study, out today in the journal Cell Stem Cell, suggests that the evolution of a subset of glia called astrocytes -- which are larger and more complex in humans than other species -- may have been one of the key events that led to the higher cognitive functions that distinguish us from other species.
The role of the astrocyte is to provide the perfect environment for neural transmission,
said Maiken Nedergaard, M.D., D.M.Sc., co-senior author of the study and director, along with Dr. Steven Goldman, M.D., Ph.D., of the URMC Center for Translational Neuromedicine. As the same time, we've observed that as these cells have evolved in complexity, size, and diversity -- as they have in humans -- brain function becomes more and more complex.
Cells Forged from Human Skin Show Promise in Treating MS, Myelin Disorders
Thursday, February 7, 2013
A study out today in the journal Cell Stem Cell shows that human brain cells created by reprogramming skin cells have the potential to be highly effective in treating myelin disorders, a family of diseases that includes multiple sclerosis and rare childhood disorders called pediatric leukodystrophies.
The study is the first successful attempt to employ human induced pluripotent stem cells (hiPSC) to produce a population of cells that are critical to neural signaling in the brain. In this instance, the researchers utilized cells crafted from human skin and transplanted them into animal models of myelin disease.
“This study strongly supports the utility of hiPSCs as a feasible and effective source of cells to treat myelin disorders,” said University of Rochester Medical Center (URMC) neurologist Steven Goldman, M.D., Ph.D., lead author of the study. “In fact, it appears that cells derived from this source are at least as effective as those created using embryonic or tissue-specific stem cells.”
Study: Model for Brain Signaling Flawed
Thursday, January 10, 2013
A new study out today in the journal Science turns two decades of understanding about how brain cells communicate on its head. The study demonstrates that the tripartite synapse -- a model long accepted by the scientific community and one in which multiple cells collaborate to move signals in the central nervous system -- does not exist in the adult brain.
Our findings demonstrate that the tripartite synaptic model is incorrect,
said Maiken Nedergaard, M.D., D.M.Sc., lead author of the study and co-director of the University of Rochester Medical Center (URMC) Center for Translational Neuromedicine. This concept does not represent the process for transmitting signals between neurons in the brain beyond the developmental stage.
Parents Create “Crosby’s Fund” to Finance Cancer Research in Son’s Honor
Wednesday, January 9, 2013
At just 13 months old, Crosby Wilmot was diagnosed with neuroblastoma, a rare cancer of the sympathetic nervous system that accounts for half of cancers diagnosed in infants. By the time of diagnosis, the disease has already spread throughout most children's bodies. The same was true for Crosby, who bravely battled for 11 months. He passed away on August 4, 2011, just one month shy of his second birthday. Crosby's spirit, however, continues to live on in many ways and has been honored by his family with the creation of Crosby's Fund, a local philanthropic initiative, through the James P. Wilmot Cancer Center and Golisano Children's Hospital at the University of Rochester Medical Center (URMC), that funds research in childhood cancer, with a focus on neuroblastoma.
"Crosby spent 85 percent of his illness in the hospital," said Zoe Wilmot, Crosby's mother. "We knew when he relapsed that we would want to one day help raise money for neuroblastoma research."
Prenatal Exposure to Fish Beneficial to Child Development
Thursday, January 3, 2013
A study published recently in the Journal of Nutrition adds to the growing scientific evidence that when expecting mothers eat fish often, they are giving their future children a boost in brain development even though they are exposing their children to the neurotoxin, methyl mercury, present in fish.
"This study shows that there are no adverse effects of prenatal mercury exposure from fish on children at 5 years old on 10 developmental outcomes when adjusted for maternal levels of polyunsaturated fatty acids. In fact, we found positive associations with those nutrients and children's language development," said Phil W. Davidson, Ph.D., professor emeritus of Pediatrics, principal investigator of the ongoing Seychelles Child Development Study and an author of the Journal of Nutrition paper.
Researchers Zero In on Cognitive Difficulties Associated with Menopause
Thursday, January 3, 2013
The memory problems that many women experience in their 40s and 50s as they approach and go through menopause are both real and appear to be most acute during the early period of post menopause. That is the conclusion of a study which appears today in the journal Menopause.
"Women going through menopausal transition have long complained of cognitive difficulties such as keeping track of information and struggling with mental tasks that would have otherwise been routine," said Miriam Weber, Ph.D. a neuropsychologist at the University of Rochester Medical Center (URMC) and lead author of the study. "This study suggests that these problems not only exist but become most evident in women in the first year following their final menstrual period."
"By identifying how these memory problems progress and when women are most vulnerable, we now understand the window of opportunity during which interventions -- be those therapeutic or lifestyle changes -- may be beneficial," said Weber. "But the most important thing that women need to be reassured of is that these problems, while frustrating, are normal and, in all likelihood, temporary."
Mini Strokes Can Cause Brain Damage, Lead To Dementia And Cognitive Impairment: Study
Thursday, December 13, 2012
Chances are if you're a senior managing your health, you've already had a conversation with your doctor about stroke risk. While many patients know the warning signs of stroke -- slurred speech, weakness on one side of the body, coordination problems, double vision, and headaches -- health care providers often fail to educate patients about their risk for silent or mini-strokes,
which can cause progressive, permanent damage and lead to dementia.
A new study published in the Journal of Neuroscience, examined the effects of these so-called mini-strokes. They frequently are not diagnosed or detected by a doctor because a patient does not immediately present with stroke signs. Mini-strokes may lead to permanent neurological damage and increase risk for full blown stroke.
Maiken Nedergaard, MD, lead author of the study and professor of neurosurgery at the University of Rochester Medical Center, says at least half of individuals over the age of 60 will experience one mini-stroke in their lifetime. She calls the prevalence of mini-strokes "an epidemic."
New Facility Will Bridge Research and Stem Cell Therapies
Wednesday, December 12, 2012
The University of Rochester Medical Center has opened the doors on a new facility that will enable researchers to create, study, and ultimately use stem cells and their offspring in early-phase experimental human therapies. The Upstate Stem Cell cGMP Facility – which will be used by academic and private-sector scientists from across the state – was created with $3.5 million in support from the Empire State Stem Cell Board.
“One of the critical barriers to moving cell-based therapies into clinical trials is the requirement that these cells be manufactured in a facility that meets strict federal requirements,” said Steve Dewhurst, Ph.D., chair of the URMC Department of Microbiology and Immunology and principal investigator for the state grant. “Without this resource, much of this science remains stuck in the lab.”
Dinner with the Doc at the Syracuse Parent Family Network
Tuesday, November 27, 2012
Join us as we celebrate November as National Epilepsy Awareness Month with a Dinner with the Doc. All who are affected by epilepsy are welcome. There are special activities provided for children.
Dr. James Fessler of the Strong Epilepsy Center will be presenting Current Medication and Treatment Options on Thursday, November 27th from 6-8pm at Rosamond Gifford Community Room (lower level) at the United Way of Central New York located at 518 James Street, Syracuse, NY.
For additional information, please call (877) 214-7715 or email Pamela Hunter at phunter@epilepsy-uny.org.
Scientists Create Endless Supply
of Myelin-Forming Cells
Thursday, November 1, 2012
In a new study appearing this month in the Journal of Neuroscience, researchers have unlocked the complex cellular mechanics that instruct specific brain cells to continue to divide. This discovery overcomes a significant technical hurdle to potential human stem cell therapies; ensuring that an abundant supply of cells is available to study and ultimately treat people with diseases.
One of the major factors that will determine the viability of stem cell therapies is access to a safe and reliable supply of cells,
said University of Rochester Medical Center (URMC) neurologist Steve Goldman, M.D., Ph.D., lead author of the study. This study demonstrates that -- in the case of certain populations of brain cells -- we now understand the cell biology and the mechanisms necessary to control cell division and generate an almost endless supply of cells.
Endless Supply
of Myelin-Forming CellsHighland Appoints Adam Kelly, M.D., Chief of Neurology
Thursday, October 25, 2012
Adam Kelly, M.D., has been named Highland Hospital's Chief of Neurology. Dr. Kelly has been involved in neurological care at the hospital since April 2010, serving as the Director of Highland's Stroke Center.
Under Dr. Kelly's guidance, Highland has experienced sustained improvement in all New York state performance measures for stroke care. The hospital earned the American Heart Association's Gold-Plus Award twice in two years as well. Dr. Kelly has also led Highland's involvement in the Stroke Treatment Alliance of Rochester (STAR) collaborative to improve stroke care at hospitals throughout the community.
"Neurology is a challenging field, but I embrace that challenge, and I love patient care," Dr. Kelly said. "I look forward to building on the programs and initiatives my predecessors have put into place."
Researchers at the Doorstep of Stem Cell Therapies for MS, Other Myelin Disorders
Thursday, October 25, 2012
When the era of regenerative medicine dawned more than three decades ago, the potential to replenish populations of cells destroyed by disease was seen by many as the next medical revolution. However, what followed turned out not to be a sprint to the clinic, but rather a long tedious slog carried out in labs across the globe required to master the complexity of stem cells and then pair their capabilities and attributes with specific diseases.
In a review article appearing today in the journal Science, University of Rochester Medical Center scientists Steve Goldman, M.D., Ph.D., Maiken Nedergaard, Ph.D., and Martha Windrem, Ph.D., contend that researchers are now on the threshold of human application of stem cell therapies for a class of neurological diseases known as myelin disorders -- a long list of diseases that include conditions such as multiple sclerosis, white matter stroke, cerebral palsy, certain dementias, and rare but fatal childhood disorders called pediatric leukodystrophies.
Stem cell biology has progressed in many ways over the last decade, and many potential opportunities for clinical translation have arisen,
said Goldman. In particular, for diseases of the central nervous system, which have proven difficult to treat because of the brain's great cellular complexity, we postulated that the simplest cell types might provide us the best opportunities for cell therapy.
Safety Harnesses Key to Prevent Falls while Deer Hunting
Wednesday, October 17, 2012
Tree stands give hunters a bird's-eye view of wild game, but some hunters continue to suffer serious injuries after failing to wear a safety harness, according to doctors at University of Rochester Medical Center.
"We are still seeing hunters who have taken unnecessary risks by not wearing the safety belt or harness and endure significant injuries from a fall," according to Jason Huang, M.D., chief of Neurosurgery at URMC's Highland Hospital. "Compared to a decade ago, we have made no progress in preventing these neurological injuries, despite safety advances -- which is unacceptable."
In a review of 54 hunting accidents or falls that resulted in neurologic injuries, doctors found that two hunters suffered paralysis. The most common reasons for the falls were poor tree-stand construction or maintenance, loss of balance, alcohol use, fatigue and dizziness. Most of the accidents were preventable if hunters, who were all men between the ages of 15 and 69, had worn a safety harness, Huang said.
Free Seminar for EMS Crews to Focus on Stroke Nov. 7
Monday, October 15, 2012
Highland Hospital invites local Emergency Medical Service (EMS) crews and Emergency Medical Technicians (EMTs) to its upcoming seminar, "Assessments and Acute Interventions for Stroke Patients," starting at 5:30 p.m. Wednesday, Nov. 7 in the Collins Auditorium at Highland. The event is free, but registration is required at (585) 341-6709.
Adam G. Kelly, M.D., Interim Chief of Neurology at Highland Hospital, will present on the common signs and symptoms of stroke and how Emergency Department and EMS personnel can partner to provide prompt evaluation of and treatment to stroke patients. Dr. Kelly also will discuss interventions physicians consider once the patient arrives, including the administration of IV tPA, a clot-dissolving medicine that can restore blood flow to parts of the brain affected by stroke. This can prevent parts of the brain from becoming permanently damaged.
Two Rochester Neurologists among Those Calling for Stronger Studies
Wednesday, October 10, 2012
Two neurologists at the University of Rochester Medical Center are part of an international team of scientists who call for greater rigor in the way that early-stage biomedical research is done and reported. The group, led by scientists at the National Institute of Neurological Disorders and Stroke, part of the National Institutes of Health, makes its recommendations in a paper published in Nature.
Among the authors are Robert A. Gross, M.D., Ph.D., and Richard T. Moxley, M.D. Gross took part through his position as editor in chief of Neurology Journals, the world's leading clinical neurology journal, while Moxley was asked to join the group because of his extensive experience working with patients and doing research on common neurological disorders.
The Nature publication is the result of a workshop organized by NINDS in June to discuss issues around preclinical research -- research on which subsequent studies in people are based. Scientists, patients, and pharmaceutical companies use this early information to make crucial decisions about what compounds to pursue to try to develop better treatments for conditions like stroke, Alzheimer's, and Parkinson's disease, and which compounds or efforts to wind down because they lack promise.
Rare Disease Researchers Notch a Win for Patients with Inherited Muscle Disease
Tuesday, October 2, 2012
An older medication originally approved to treat heart problems eases the symptoms of a very rare muscle disease that often leaves its sufferers stiff and in a good deal of pain, physicians and researchers report in the Oct. 3 issue of the Journal of the American Medical Association.
"This study can serve as a blueprint for future rare disease research," said neurologist Jeffrey Statland, M.D., senior instructor in Neurology and the first author of the paper. "This study shows that by bringing together experts and patients around the world and building a common infrastructure, we can tackle rare conditions that have eluded rigorous clinical study up to now."
Rochester neurologist Robert "Berch" Griggs, M.D., another author of the paper and the leader of a Rochester center devoted to studying rare neurological disorders, notes that, ironically, many people suffer from rare diseases.
"Each rare disease might affect only a few thousand people, but there are thousands of rare diseases. Current estimates are that perhaps 30 million people are affected by some form of rare disease," said Griggs.
Golisano Chief Named President of Child Neurology Society
Wednesday, August 29, 2012
Golisano Children's Hospital's pediatrician-in-chief has been elected president of the nation's largest organization of child neurologists. Nina F. Schor, M.D., Ph.D., William H. Eilinger chair of Pediatrics at the University of Rochester Medical Center, was voted into the presidency of this organization by fellow pediatric neurologists from around the world and will assume the position of President-elect following the annual meeting of the Child Neurology Society in November.
The Child Neurology Society is a non-profit professional association of 1,300 pediatric neurologists in the United States, Canada, and worldwide who are devoted to fostering the discipline of child neurology and promoting the optimal care and welfare of children with neurological and neurodevelopmental disorders. These disorders include epilepsy, cerebral palsy, mental retardation, learning disabilities, complex metabolic diseases, nerve and muscle diseases and a host of other highly challenging conditions.
Study Questions Validity of Quality Measure for Stroke Care
Monday, August 27, 2012
One of the key indicators of the quality of care provided by hospitals to acute stroke victims is the percentage of patients who die within a 30-day period. A new study shows that the decisions made by patients and their families to stop care may account for as many as 40 percent of these stroke-related deaths, calling into question whether it is a valid measure of a hospital’s skill in providing stroke care.
The study, which appears today in the journal Neurology, focuses on a quality measure proposed by the federal Centers for Medicaid and Medicare Services called the 30-day risk adjusted stroke mortality. While the measure is being developed as a part of federal health care reform, it is already commonly employed as an indicator of a hospital’s quality of care on websites that evaluate hospital performance.
"It is clear that a significant component of the overall mortality score as currently constructed does not tell the whole story and is predicated on the preference of patients and their families," said University of Rochester Medical Center (URMC) neurologist Adam Kelly, M.D., lead author of the study.
A Promising Step Forward Toward Muscular Dystrophy Treatment
Wednesday, August 1, 2012
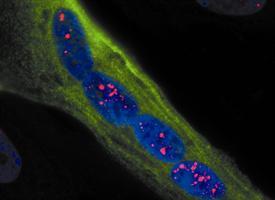
Deposits of toxic RNA (red) are seen here
inside muscle cell nuclei (blue) from an individual
with myotonic dystrophy.
Scientists have reversed symptoms of myotonic muscular dystrophy in mice by eliminating a buildup of toxic RNA in muscle cells. The work, carried out by scientists at the University of Rochester Medical Center, Isis Pharmaceuticals Inc. and Genzyme, is published in the August 2 issue of Nature.
After experimental antisense compounds were administered to mice twice a week for four weeks, symptoms of the disease were reduced for up to one year – a significant portion of a mouse's lifespan.
The investigators say that while the work is an encouraging step forward against myotonic dystrophy, one of the most common forms of muscular dystrophy, it's too soon to know whether the approach will work in patients. But they are cautiously optimistic, noting that the compound is extremely effective at reversing the disease – whose genetic underpinnings make it particularly vulnerable to an antisense approach – in a mouse model.
These results give us strong encouragement about the possibility of developing a treatment that could fundamentally alter the disease. It's an important step on a long path,
said senior author Charles Thornton, M.D., a neurologist at the University of Rochester Medical Center who has been pursuing new treatments for the disease for more than two decades.
In Muscular Dystrophy, What Matters to Patients and Doctors Can Differ
Wednesday, July 25, 2012
Complex, multi-system diseases like myotonic dystrophy -- the most common adult form of muscular dystrophy -- require physicians and patients to identify which symptoms impact quality of life and, consequently, what treatments should take priority. However, a new study out this month in the journal Neurology reveals that there is often a disconnect between the two groups over which symptoms are more important, a phenomenon that not only impacts care but also the direction of research into new therapies.
"In order to design better therapies we must first develop a clear understanding of what patients think are the key mental and physical burdens of this disease," said University of Rochester Medical Center (URMC) neurologist Chad Heatwole, M.D., lead author of the study. "It is clear from this study that, in the case of myotonic dystrophy, researchers have not always been concentrating on the symptoms that are most important to the patient."
In Muscular Dystrophy, What Matters to Patients and Doctors Can Differ
Wednesday, July 25, 2012
Complex, multi-system diseases like myotonic dystrophy -- the most common adult form of muscular dystrophy -- require physicians and patients to identify which symptoms impact quality of life and, consequently, what treatments should take priority. However, a new study out this month in the journal Neurology reveals that there is often a disconnect between the two groups over which symptoms are more important, a phenomenon that not only impacts care but also the direction of research into new therapies.
URMC Neurology Chair Returns to Research Lab; Acting Chair Appointed
Thursday, July 19, 2012
After four years as chair of the Department of Neurology, Steven Goldman, M.D., Ph.D., is stepping down to resume research duties full time as Co-Director of the Center for Translational Neuromedicine.
Dr. Goldman will remain an active member of the Neurology faculty, increasing his research focus and commitment, while Robert G. Holloway Jr., M.D., M.P.H., Professor of Neurology, will serve as Acting Chair of the Department as a national search for permanent leadership is launched.
New Huntington’s Treatment Shows Promise
Wednesday, July 18, 2012
A new study shows that the compound Coenzyme Q10 (CoQ) reduces oxidative damage, a key finding that hints at its potential to slow the progression of Huntington disease. The discovery, which appears in the inaugural issue of the Journal of Huntington’s Disease, also points to a new biomarker that could be used to screen experimental treatments for this and other neurological disorders.
"This study supports the hypothesis that CoQ exerts antioxidant effects in patients with Huntington’s disease and therefore is a treatment that warrants further study," says University of Rochester Medical Center neurologist Kevin M. Biglan, M.D., M.P.H., lead author of the study. "As importantly, it has provided us with a new method to evaluate the efficacy of potential new treatments."
Huntington’s disease is a genetic, progressive neurodegenerative disorder that impacts movement, behavior, cognition, and generally results in death within 20 years of the disease’s onset. While the precise causes and mechanism of the disease are not completely understood, scientists believe that one of the important triggers of the disease is a genetic "stutter" which produces abnormal protein deposits in brain cells. It is believed that these deposits – through a chain of molecular events – inhibit the cell’s ability to meet its energy demands resulting in oxidative stress and, ultimately, cellular death.
Study Links PTSD to Hidden Head Injuries Suffered in Combat
Wednesday, June 6, 2012
Even when brain injury is so subtle that it can only be detected by an ultra-sensitive imaging test, the injury might predispose soldiers in combat to post-traumatic stress disorder, according to a University of Rochester Medical Center study.
The research is important for physicians who are caring for troops in the years following deployment, as they try to untangle the symptom overlap between PTSD and mild traumatic brain injury (mild TBI) and provide the appropriate treatment. Until now, the nature of the interaction between TBI and PTSD was unclear. URMC researchers believe they are the first to find an association that can be demonstrated with advanced imaging techniques.
The study is published online by the Journal of Head Trauma Rehabilitation.
“Most people believe that, to a large extent, chronic stress from intense combat experiences triggers PTSD. Our study adds more information by suggesting that a physical force such as exposure to a bomb blast also may play a role in the genesis the syndrome,” said lead author Jeffrey J. Bazarian, M.D., M.P.H., associate professor of Emergency Medicine at URMC, and a member of the 2007 Institute of Medicine committee that investigated brain injuries among war veterans.
U.S. News Ranks Golisano Children's Hospital Among Best in Four Programs
Tuesday, June 5, 2012
Golisano Children's Hospital at the University of Rochester Medical Center is steadily moving up the list of U.S. News & World Report's Best Children's Hospital rankings. The hospital has been listed among the nation's best hospitals for four pediatric specialties -- gastroenterology, neonatology, orthopaedics and neurology/neurosurgery. The annual rankings, which are available online today and will be published in the U.S. News Best Hospitals 2013 guidebook in August, are based on data submitted by nearly 180 pediatric institutions nationwide.
Each of the past four years, Golisano Children's Hospital has added a specialty to the U.S. News rankings, starting in 2009 with orthopaedics, which ranked #38 this year. Neonatology ranked #27; Gastroenterology, which is new to the list this year, ranked #41, and Neurology and Neurosurgery ranked #44.
Grant to Improve Training for Professionals Caring for Those with Alzheimer’s Disease
Tuesday, May 22, 2012
The Finger Lakes Geriatric Education Center (FLGEC) at the University of Rochester Medical Center was awarded grant funds to enhance training and education for professionals who assess and care for people with Alzheimer's Disease.
FLGEC earned a Supplemental Funding Grant for Education from the Health Resources and Services Administration. Funding consists of approximately $135,000 over two years, made possible through the federal National Alzheimer's Project Act. The award will help FLGEC develop additional training that incorporates new materials and information developed under the National Plan to Address Alzheimer's Disease, including guidelines for care and new screening and assessment tools.
FLGEC is led by Jurgis Karuza, Ph.D., is program director, and Thomas Caprio, M.D., M.P.H., Project Co-Director.
Stroke Victims Not Receiving Timely Diagnosis, Care
Wednesday, May 2, 2012
The mantra in stroke care is “time is brain.” With each passing minute more brain cells are irretrievably lost and, because of this, timely diagnosis and treatment is essential to increase the chances for recovery. While significant strides have been made to improve the response time of caregivers, a new study shows that a critical step in the process – imaging of the brain to determine the nature of the stroke – is still occurring too slowly at too many hospitals.
A study out this month in the journal Stroke shows that only 41.7 percent of stroke patients underwent brain imaging within the recommended 25 minutes of their arrival at a hospital. It also found that certain individuals, including people with diabetes, those over 75 years of age, women, those that did not arrive by ambulance, non-whites, and those with certain cardiac conditions were less likely to receive a timely brain scan. These delays mean that treatment often comes either too late or not at all.
"We were struck by the fact that less than half of patients with acute stroke symptoms did not receive a brain scan within recommended guidelines,” said University of Rochester Medical Center neurologist Adam Kelly, M.D., lead author of the study. “This was the performance of hospitals who are actively participating in a national quality improvement program, so rates in non-participating hospitals may be even worse."
University Life Trustee, Neurosciences Benefactor Ernest J. Del Monte Dies
Monday, April 23, 2012
Ernest J. Del Monte, 87, real estate and hotel developer, philanthropist and University of Rochester Life Trustee, died Saturday, April 21, 2012. His generosity to the University of Rochester leaves a legacy of innovation and collaboration to help eradicate brain diseases.
Mr. Del Monte, of Pittsford, was a visionary in business and industry. With a $10 million gift to the University in 2009, he and his wife, Thelma, helped establish the E.J. Del Monte Neuromedicine Institute to expand the study and treatment of Alzheimer's disease, stroke, spinal cord and brain injuries, and brain cancers at the University of Rochester Medical Center.
The gift was the catalyst for the establishment of the Del Monte Neuromedicine Institute, which serves as an umbrella for several vibrant research centers and growing clinical care programs throughout the Medical Center and River Campus. It has also reinvigorated the scientists and physicians who treat patients with neurological conditions.
Ernie was a force of nature who touched so many of our lives at the University. I am proud to have spent time with him and his late wife, Thelma, and continue to be deeply moved by his commitment to the Del Monte Neuromedicine Institute. When I last spoke with him, he was still planning deals, always imaginative, always determined, right up to the end,
said Joel Seligman, president of the University of Rochester.
A Pillar of Modern Neurology, Robert J. Joynt, Dies
Monday, April 16, 2012
Robert J. Joynt, M.D., Ph.D.
Robert J. Joynt, M.D., Ph.D., one of the most influential neurologists of the last half century and the founder of the Department of Neurology at the University of Rochester Medical Center, died April 13 at Strong Memorial Hospital. He was 86.
Dr. Joynt was a towering figure in international circles of neurology and headed both leading societies in neurology, the American Academy of Neurology and the American Neurological Association. He also served as president of the American Board of Psychiatry and Neurology. Beyond that, he was a beloved member of the Medical Center's community, which he had served through several top-level posts, including dean of the School of Medicine and Dentistry.
Meds Ease Depression in Parkinson’s Patients Without Worsening Other Symptoms
Wednesday, April 11, 2012
Today's anti-depressant medications can ease depression in Parkinson's patients without worsening other symptoms of the disease, according to a study published online in Neurology Journals, the medical journal of the American Academy of Neurology.
"Depression is the number-one factor negatively affecting the quality of life for people with Parkinson's disease," said Irene Hegeman Richard, M.D., who led the study. "It causes a great deal of suffering among patients. The great news here is that it's treatable. And when the depression is treated adequately, many of the other symptoms become much more manageable for patients," added Richard, a neurologist at the University of Rochester Medical Center.
The findings are good news for patients with Parkinson's disease, a chronic neurologic disorder best known for causing slow movement, stiffness, balance problems and other motor difficulties. However, about half of Parkinson's patients also struggle with depression.
‘Brain Fog’ of Menopause Confirmed
Wednesday, March 14, 2012
The difficulties that many women describe as memory problems when menopause approaches are real, according to a study published today in the journal Menopause, the journal of the North American Menopause Society.
The findings won't come as a surprise to the millions of women who have had bouts of forgetfulness or who describe struggles with "brain fog" in their late 40s and 50s. But the results of the study, by scientists at the University of Rochester Medical Center and the University of Illinois at Chicago who gave women a rigorous battery of cognitive tests, validate their experiences and provide some clues to what is happening in the brain as women hit menopause.
"The most important thing to realize is that there really are some cognitive changes that occur during this phase in a woman's life," said Miriam Weber, Ph.D., the neuropsychologist at the University of Rochester Medical Center who led the study. "If a woman approaching menopause feels she is having memory problems, no one should brush it off or attribute it to a jam-packed schedule. She can find comfort in knowing that there are new research findings that support her experience. She can view her experience as normal."
Early Surgery Controls Seizures, Improves Quality of Life
Tuesday, March 6, 2012
A new study out today in the Journal of the American Medical Association finds that the vast majority of patients with previously uncontrolled temporal lobe epilepsy who underwent surgical intervention early in the course of their disease where not only seizure free, but experience a significantly higher quality of life compared to those who only manage their condition medically. The results demonstrate that, instead of being considered a last resort, early surgery could help epilepsy patients avoid decades of disability.
"The results of this study are very clear: early surgical intervention works, it stops seizures, and it improves quality of life," said University of Rochester Medical Center neurologist Karl Kieburtz, M.D., the senior author of the study. "Individuals with temporal lobe epilepsy that is not controlled with medicine should be evaluated for surgical intervention at a comprehensive epilepsy center not after decades of poor response to medicine but within two years. And if they are a surgical candidate they should give strong consideration to that approach."
Each Flick of a Digit Is a Job for All 5
Monday, February 27, 2012
You may think you're pretty familiar with your hands. You may think you know them like the back of your hand. But as the following exercises derived from the latest hand research will reveal, your pair of bioengineering sensations still hold quite a few surprises up their sleeve.
Our fingers can seem like restless Ariels, so fast and dexterous you'd think they had plans and options of their own. Yet as scientists who study the performance, circuitry and evolution of the human hand have lately determined, the appearance of digital independence is deeply deceptive.
Even when you think you're moving just one finger,
said Marc H. Schieber, a professor of neurology and neurobiology at the University of Rochester Medical Center, you're really controlling your entire hand.
The pianist playing Ravel or the typist clacking on Blogspot? People tend to think, they're hitting one key at a time, so they must be moving one finger at a time to hit that key,
Dr. Schieber said. But really, all the fingers are in motion all the time.
Some Muscular Dystrophy Patients at Increased Risk for Cancer
Tuesday, December 13, 2011
People who have the most common type of adult muscular dystrophy also have a higher risk of getting cancer, according to a paper published today in the Journal of the American Medical Association.
The team found that patients who have myotonic muscular dystrophy are at increased risk primarily for four types of cancer: brain, ovary, colon, and the uterine lining known as the endometrium. The team also found a possible increased risk for some other types of cancer, including cancer of the eye, thyroid, pancreas, and other female reproductive organs.
Physicians estimate that approximately 40,000 Americans have myotonic dystrophy, an inherited disease that is marked by progressive muscle weakness. While the course of the disease varies from patient to patient, symptoms can include muscle stiffness, difficulty speaking and swallowing, problems walking, and in some patients, heart problems and cataracts.
Routine Head Hits in School Sports May Cause Brain Injury
Monday, November 14, 2011
The brain scans of high school football and hockey players showed subtle injury - even if they did not suffer a concussion – after taking routine hits to the head during the normal course of play, according to a University of Rochester Medical Center study.
The research, reported online in the journal Magnetic Resonance Imaging, is preliminary, involving a small sample of athletes, but nonetheless raises powerful questions about the consequences of the mildest head injury among youths with developing brains, said lead author Jeffrey Bazarian, M.D., M.P.H., associate professor of Emergency Medicine at URMC with a special interest in sports concussions.
Scientists Explore Whether What Heals the Head Can Also Heal the Heart
Wednesday, November 2, 2011
Handy Gelbard, Stephen Dewhurst, Burns Blaxall
A diverse group of scientists -- experts in cardiology, neurology, immunology, microbiology and chemistry -- are teaming up to study drugs that show promise in the treatment of dementia for the treatment of an equally debilitating disease -- heart failure. In this case, the connection between the head and the heart lies in a particular enzyme that they believe plays a role in the development of both conditions.
The team, headed by Burns C. Blaxall, Ph.D., Harris A. "Handy" Gelbard, M.D., Ph.D., and Stephen Dewhurst, Ph.D., recently won the largest grant awarded to date by the University's Clinical and Translational Science Institute (CTSI) -- $250,000 over two years. The grant, part of the CTSI's newly initiated Incubator Program, is larger than most awarded by the Medical Center.
Thomas Pearson, M.D., Ph.D., who heads the CTSI and helped develop the new program, says tremendous weight was given to forming new teams that had never worked together before, and for these teams to study things they had never addressed before. The Blaxall/Gelbard/Dewhurst team fit the bill on both counts.
New Network Will Advance Neurological Care
Thursday, October 27, 2011
The University of Rochester Medical Center has been tapped by the National Institutes of Health (NIH) to play a critical role in a new national initiative to accelerate the process of turning promising discoveries into new ways to treat neurological diseases.
"The complexity and often rare nature of diseases of the central nervous system present a unique set of challenges in terms of developing new treatments," said Robert Holloway, M.D., M.P.H., professor of Neurology at the Medical Center. "This new initiative by the NIH will create the economies of scale and coordination necessary to rapidly and efficiently move novel therapies closer to the point where they can ultimately benefit patients."
Neurologist’s Talk Aimed at Parkinson’s Patients, Caregivers
Thursday, October 13, 2011
A physician who specializes in treating patients with Parkinson's disease and related disorders will speak about the condition and take questions from patients, family members and caregivers in a free public talk next week.
Michelle Burack, M.D., Ph.D., a neurologist at the University of Rochester Medical Center, will speak from 9:30 to 11 a.m. Thursday, Oct. 20, at Lifetime Care, 3111 S. Winton Road. The discussion is aimed especially at patients who have recently been diagnosed with Parkinson's, along with family members, though all are welcome.
The talk is part of a series of public discussions Burack has initiated across New York State, as part of educational outreach efforts through the Parkinson Support Group of Upstate New York. The talks are a way for Burack, who is part of a medical team that treats hundreds of patients with the disease, to educate people about Parkinson's and at the same time learn more about the disease, enabling her to treat patients more effectively. Three talks per year in the Rochester area are planned.
Precision with Stem Cells a Step Forward for Treating M.S., Other Diseases
Thursday, October 13, 2011
Areas in red indicate mouse brain cells coated with myelin, a crucial substance lacking in patients with M.S.
A diverse group of scientists -- experts in cardiology, neurology, immunology, microbiology and chemistry -- are teaming up to study drugs that show promise in the treatment of dementia for the treatment of an equally debilitating disease -- heart failure. In this case, the connection between the head and the heart lies in a particular enzyme that they believe plays a role in the development of both conditions.
The team, headed by Burns C. Blaxall, Ph.D., Harris A. "Handy" Gelbard, M.D., Ph.D., and Stephen Dewhurst, Ph.D., recently won the largest grant awarded to date by the University's Clinical and Translational Science Institute (CTSI) -- $250,000 over two years. The grant, part of the CTSI's newly initiated Incubator Program, is larger than most awarded by the Medical Center.
Thomas Pearson, M.D., Ph.D., who heads the CTSI and helped develop the new program, says tremendous weight was given to forming new teams that had never worked together before, and for these teams to study things they had never addressed before. The Blaxall/Gelbard/Dewhurst team fit the bill on both counts.
Has Your Brain Already Crystallized?
Tuesday, October 4, 2011
As it turns out, keeping pace in ever-more-electronic world is no small feat for the aging brain. That's because our mental circuitry – the most frequently used neuron pathways, like well-traveled roads – tends to crystallize
into a series of expressways over time. But that doesn't mean paving new paths (by, say, learning in middle age) is a lost cause – it just demands special learning techniques and a little more patience.
That's heartening news for adults who are headed back to school, shifting careers in later life, or simply want to be lifelong learners, says neuropsychologist Dr. Mark Mapstone. In the clip below, he sheds more light on our amazing (and aging) brains.
Stop Stroke Before it Stops You - 4 Things You Should Know
Tuesday, September 27, 2011
Ask any number of men what they think their odds of having a stroke are, and you might find many of them believe stroke is frighteningly unpredictable and can attack like a bolt from the blue – without warning, trailing death and disability in its wake.
That idea is dangerously wrong. The truth is that a stroke is the bullet at the end of a very long barrel and there is a lot you can do to dodge it.
The path to stroke can be started by heart disease – especially if you have an irregular heartbeat. It also can be started by arterial disease – especially if there is a build-up of plaque in the arteries of the neck. The chain of events that begins with cardiovascular disease and ends in stroke can take years, or even decades to evolve. You probably will not know that it is happening.
Need More Memory (No, We’re Not Talking RAM)
Tuesday, September 20, 2011
Searching frantically for misplaced car keys. Fumbling for the name of a new acquaintance. Providing an accurate eye-witness testimony. Treasuring past moments with a loved one lost. What, exactly, is this thing we call “memory”? How do our brains manage to process, store and recall so much sensory footage – even lifeless data, like phone numbers – almost reflexively?
Neuropsychologist Dr. Mark Mapstone co-directs URMC's memory care clinic, which features a team of neurologists, psychiatrists, a geriatrician, a neuropsychologist, a psychometrician (expert in measuring psychological function), a social worker and a nurse practitioner. He weighs in on these and other burning questions in the clip below.
Stem Cell Efforts to Treat Neurological Disease Bolstered With $4.5 Million
Wednesday, September 7, 2011
Human oligodendrocytes and astrocytes generated from human neural progenitor cells.
The endeavor to find better treatments or perhaps even one day a cure for a host of debilitating and fatal neurological diseases has been bolstered by an influx of funding from a mix of private and public sources.
he laboratory headed by Steven Goldman, M.D., Ph.D., chair of the Department of Neurology at the University of Rochester Medical Center, has received $4.5 million in new funding to further its efforts to use stem cells and related molecules to treat several feared disorders for which there are currently no cures – including multiple sclerosis, Huntington's disease, and fatal childhood diseases known as pediatric leukodystrophies.
Event to Benefit Parkinson Disease Research
Friday, July 29, 2011
A fundraising event to benefit research in Parkinson disease is being held in honor of a former Rochester resident who had the disease. Vicki Aspridy and Janice Corea are hosting "Funk & Waffles for Parkinson’s," featuring delicious waffles, live music, and more, in memory of their mother, Tarpa Aspridy, who had the disease late in life and passed away three years ago.
Funds raised from the event will benefit the Michael J. Fox Foundation for Parkinson’s Research (MJFF). MJFF’s mission is to discover a cure for Parkinson disease and develop improved therapies for those living with the condition today.
Health Gains from MS Drugs Come at a High Price
Wednesday, July 20, 2011
A new study shows that the health gains associated with a category of medications commonly used to treat Multiple Sclerosis (MS) -- know as disease modifying drugs -- come at a very high cost when compared to therapies that address the symptoms of MS and treatments for other chronic diseases.
The study -- which appears today in the journal Neurology Joournal -- analyzed data from 844 individuals with early stage MS and projected health care costs, including the cost of the drugs, and lost productivity over a 10 year period. The study found that while MS patients using disease- modifying drugs experience modest health gains, the cost associated with using these drugs is more than 8 times higher than what is considered "reasonable" from a health economics cost-effectiveness perspective.
"While it is clear that disease-modifying drugs are beneficial to some MS patients, those gains come at a tremendous economic cost," said Katia Noyes, Ph.D., M.P.H., associate professor in the Department of Community and Preventive Medicine at the University of Rochester Medical Center and lead author of the study. "These results point to the need to continually evaluate the cost-effectiveness of new treatments in the interest of controlling health care costs."
Is the Internet Replacing Your Memory?
Thursday, July 14, 2011
Google, Facebook, Internet Movie Database, and many other sources of information on the Internet are changing the way in which we remember. As a result of this instant access, growing numbers of us may actually be outsourcing our memories. It's called the Google effect
and it is documented online in the journal Science.
Google is just another form of external memory,
says Betsy Sparrow, Ph.D., an assistant professor in the department of psychology at Columbia University in New York City. Neuropsychologist Mark Mapstone, Ph.D., University of Rochester Medical Center in Rochester, N.Y., isn't sure the Google effect is such a good thing for our memories. This is not as good for us from a brain perspective,
he says. If you download your information to a device, you are not using your brain to make connections as you should be.
That said, When you don't burden your memory with rote remembering, it does free up activity for more complex thinking,
he says.
Two Rochester Scientists among Top Parkinson Researchers
Wednesday, July 13, 2011
Two scientists at the University of Rochester Medical Center are among the world’s top researchers in the area of Parkinson disease, according to a recent study.
Karl Kieburtz, M.D., M.P.H., and Kim Tieu, Ph.D., are among the researchers cited in a recent study published last month in the Journal of Parkinson’s Disease. The study was done by Aaron Sorensen of GE Healthcare and publishing consultant David Weedon.
The study analyzed the number of times a scientist’s work has been cited by other scientists, the amount of new research that the person has published, and the ripple effect of the work in Parkinson disease as well as other areas.
Both Kieburtz and Tieu are among the 100 scientists whose work has been cited most during the last decade by other scientists doing research on the disease. Also on the list is Ira Shoulson, M.D., a former University of Rochester neurologist who is now at Georgetown. Altogether, research by the three was cited more than 6,500 times during the last decade by other scientists.
First Controlled Clinical Trial for Juvenile Batten Disease to Start
Tuesday, May 31, 2011
After years of building hope for a treatment, Rochester researchers and clinicians will begin the first controlled clinical trial for Juvenile Batten disease this summer, thanks to $1 million in grants from the Food and Drug Administration (FDA) and the Batten Disease Support and Research Association (BDSRA). The trial will examine whether mycophenolate mofetil, a drug FDA-approved to suppress the immune system and prevent organ rejection in children, is safe for these children and whether it can slow or halt the progression of the fatal neurodegenerative disease.
“Families have been anxiously awaiting word on when we could launch this clinical trial,” said Frederick Marshall, M.D., principal investigator of the trial and Associate Professor of Neurology. “Juvenile Batten Disease is very rare, but the families are very close and well-informed about potential treatments. They have been watching the progress of this research and hoping for the day when we could launch the trial.”
Juvenile Batten disease is a lysosomal-storage disease that strikes seemingly healthy children and progressively robs them of their abilities to see, reason and move. It ultimately kills them in late adolescence or young adulthood. Batten disease is in the same family of diseases as Krabbe disease to which former Buffalo Bills quarterback Jim Kelly lost his son, Hunter, in 2005.
$10 Million Gift from Philip Saunders Advances URMC’s Neuromuscular Program, Other Initiatives
Monday, April 4, 2011
Philip Saunders, a Rochester businessman and a major supporter of the neuromuscular disease program at the University of Rochester Medical Center, has donated an additional $10 million – one of the largest gifts ever in the history of the Medical Center – for the program as well as other URMC research initiatives.
The gift boosts dramatically one of the signature programs of the Medical Center – neuromedicine, an area in which its scientists and physicians excel in both patient care and research.
Some of the funds will be used to support cancer research, particularly URMC's proposed research collaboration with Roswell Park Cancer Institute in Buffalo. Saunders' support also boosts the University's commitment to clinical and translational science, accelerating the development of new treatments for many diseases based on discoveries in University of Rochester laboratories.
US News & World Report Ranks URMC Hospital #1 in Metro Area
Tuesday, March 29, 2011
The University of Rochester Medical Center’s Strong Memorial Hospital has been ranked first in the greater Rochester area in US News & World Report’s first-ever Best Regional Hospitals 2010-11 ranking. The new rankings include selected hospitals in 52 metropolitan areas with over one million residents.
The Best Regional Hospitals listing recognizes hospitals that score within the top 25 percent of all 4,852 eligible hospitals ranked in at least one of 16 medical specialties. URMC’s scores reached that high-performance threshold in 11 of 16 specialties, including cancer, diabetes and endocrinology, gastroenterology, geriatrics, gynecology, heart and heart surgery, kidney disorders, neurology and neurosurgery, orthopaedics, pulmonology, and urology.
Study: African Americans Have Better Stroke Survival Rates
Monday, January 31, 2011
A study published today shows that African Americans have a better survival rate compared to whites after being hospitalized for a stroke. This conclusion contradicts prevailing wisdom and is one piece in a growing body of evidence that points to the important role that patients -- and the decision they and their families make in terms of treatment -- may play on mortality rates.
The study found that -- after adjusting data for variables such as age, socioeconomic status, and risk factors -- that African Americans who were hospitalized for acute ischemic stroke had a significantly lower mortality rate than whites. The survival advantage was most pronounced early after the stroke but persisted for up to one year. The study also found that African Americans were also more likely during their hospitalization to have received more aggressive treatment measures, such as kidney dialysis, a tracheostomy, or cardiopulmonary resuscitation. They were also less likely to use hospice care. These results were published today in the Annals of Internal Medicine.
"These results fly in the face of conventional wisdom that says that black patients with strokes have worse outcomes," said University of Rochester Medical Center neurologist Robert Holloway, M.D., M.P.H. a co-author of the study. "Even though we do not know the exact reasons for these differences, these data highlight the potential importance of treatment intensity, and the expression of patient preference for different treatments on survival and mortality. This is not such a far-fetched idea for physicians who take care of a lot of stroke patients."
Study: Get Thee to a Stroke Center
Tuesday, January 25, 2011
Hospitals with designated stroke centers are associated with up to 20 percent higher survival rate for patients with ischemic stroke and significantly greater use of acute stroke therapy. That is the conclusion of a study appearing today in the Journal of the American Medical Association which compares treatment and outcomes in stroke care between hospitals in New York State.
"The basic premise of stroke centers and stroke care -- that coordinated care delivered around a specific disease can likely improve outcomes -- is widely accepted," said University of Rochester Medical Center neurologist Robert Holloway, M.D., M.P.H., a co-author of the study. However, there has been limited empirical evidence demonstrating that admission to a stroke center is associated with lower mortality. This study shows that designated stroke centers not only have a greater adherence to evidence based practices but they also save lives.
Neuroscientist to Discuss Action Video Games as Learning Tool
Monday, January 10, 2011
Cognitive scientist Daphne Bavelier, Ph.D., will discuss her work using video games to explore the remarkable capacity of the brain to adapt as part of a lecture series highlighting biological and biomedical research at the University of Rochester.
Bavelier will discuss her research this Friday, Jan. 14, in the Class of '62 Auditorium (Room G-9425) at the Medical Center. The talk, part of the “Second Friday Science Social” lecture series, is geared mainly to faculty, staff and students at the University, though the general public is welcome as well.
Bavelier, professor of Brain and Cognitive Sciences, is an expert on the brain's ability to learn and adapt to an ever-changing environment. For the past decade, she has employed video games as a way to explore the brain's ability to adapt – a capability crucial for people trying to recover from a stroke or a traumatic brain injury or for people seeking to keep their mind as sharp as possible as they age.
Medical Mystery: Doctor's Diagnosis Drew Laughs, But It Saved Woman's Life
Tuesday, December 7, 2010
Donna Landrigan - with her husband, Dan, and children, Kyle, left, Emma and Zach - says, "I'm so thankful to be back with my family" after surviving an illness that could have killed her. (George Bates For The Washington Post Kevin Rivoli)
As the all-too-familiar number flashed on his cellphone shortly before 9 p.m., Dan Landrigan reflexively braced himself for bad news. The caller was one of the doctors treating his wife, Donna, who had been in a coma for four months. She sounded pretty choked up,
Landrigan recalled.
I think we've found out what's making your wife sick,
the specialist at the University of Rochester's Strong Memorial Hospital told him, as a wave of relief flooded his body. I was completely shocked,
said the telecommunications executive, now 37. My hope for so long was that this was the phone call I was going to get.
Doctors at three Upstate New York hospitals had been stymied by Donna Landrigan, whose case was unlike any they had seen. The previously healthy 35-year-old mother of three had initially become so psychotic she had to be tied to her hospital bed to keep her from hurting herself or attacking others. A few weeks later she had been placed in a medically induced coma to protect her from the continuous seizures wracking her brain, spasms that could have killed her.
Canandaigua Woman’s Ordeal Illuminates Rare Form of Seizures
Tuesday, October 19, 2010
The remarkable story of a Canandaigua, N.Y. woman who emerged from a more than six month long coma is now being used to educate physicians about how to recognize and treat her extremely rare condition. The elusive source of her uncontrolled seizures, which physicians at the University of Rochester Medical Center (URMC) ultimately traced to ovarian cancer, and her subsequent recovery are the subject of a paper appearing today in the journal Neurology.org.
Researchers Target HIV-Related Brain Difficulties
Thursday, October 7, 2010
During the last two decades, scientists and doctors have developed a potent mix of medications that nearly stops HIV in its tracks for most patients. This combination antiretroviral therapy, or cART, can knock down levels of the virus in the body to a thousandth or less of what it would otherwise be. That means more years of a healthy life for many HIV patients.
But that success does not extend fully to the brain, where an assault triggered by the virus continues despite treatment. About half of patients infected by HIV experience symptoms, such as difficulty thinking or concentrating, as a result of the effects of the virus on the brain. So far, nearly a dozen studies in people have failed to identify a drug useful for treating the condition, which is known as HIV-associated neurocognitive disorder.
At the University of Rochester Medical Center, neurologist Harris A. Handy
Gelbard, M.D., Ph.D., leads a team of scientists intent on developing the world’s first treatment designed specifically to prevent or ease the neurological effects of HIV. This week, Gelbard – whose team has spent a decade exploring novel ways to treat the condition – received word that the project would continue for another five years, thanks to $6.7 million in new funding from the National Institute of Mental Health.
Rochester Helps Lead Global Parkinson’s Study
Wednesday, October 6, 2010
Patients, doctors and nurses in Rochester will be a key part of a major national research study initiated by the Michael J. Fox Foundation to identify biomarkers to track the progression of Parkinson's disease in a precise way that is impossible to do today.
The study, known as the Parkinson's Progression Markers Initiative, seeks to fill a crucial gap: While doctors can generally predict the course that the disease takes in patients, there is no reliable, objective way to actually measure how the disease is progressing. A measure known as a biomarker, based on a biological measure that would be consistent among all patients, would help researchers measure the effectiveness of current treatments on their patients.
A reliable biomarker is also a critical tool to have in hand for scientists trying to identify new drugs to treat the disease. Currently there is no known biomarker for Parkinson's disease.
The study of approximately 600 people around the world will include up to 30 people at the University of Rochester Medical Center, which is one of 18 participating sites worldwide. The Rochester site is led by neurologist Irene Richard, M.D.
Rochester Leads International Effort To Improve Muscular Dystrophy Treatment
Friday, September 3, 2010
A large international study aimed at improving the care of muscular dystrophy patients worldwide is being launched by physicians, physical therapists, and researchers at the University of Rochester Medical Center.
Neurologist Robert “Berch” Griggs, M.D., is heading the study of treatments for Duchenne muscular dystrophy, the most common form of the disease that affects children. The condition, which affects boys almost exclusively, progresses rapidly. Boys’ symptoms start when they are toddlers; untreated, they end up in a wheelchair before they become teenagers. With today’s best treatments, the disease, which affects about 28,000 boys and young men in the United States, is often fatal by the time a patient reaches his 20s or early 30s.
Rochester’s Pinpoint Gene Control Boosts Parkinson’s Research
Tuesday, August 24, 2010
Top: The dark area shows a part of the mouse brain where dopamine neurons have died when toxic LRRK2 is active. Below: Dopamine neurons (in red) thrive when toxic gene activity is blocked.
A technology developed at the University of Rochester Medical Center that enables scientists to turn on genes exactly when and where they want in the nervous system is helping scientists in the hunt for an agent to stop Parkinson's disease.
The work employs the herpes virus – the bane of so many people, but in this instance an aid to researchers – to help mimic in mice the activity of a gene that plays a role in some cases of Parkinson's disease in people. Scientists used the virus to carry a copy of the faulty gene into mice, creating brain conditions identical to Parkinson's disease. The step allowed researchers to then screen compounds in the search for one that might stop the toxicity of the gene.
The team of scientists, led by investigators at Johns Hopkins University, found two promising candidates and reported its results August 22 in Nature Medicine.
“While there are many drugs to treat symptoms of Parkinson's disease, there is currently no drug available to stop the death of nerve cells that is at the core of the disease,” said neuroscientist William Bowers, Ph.D., of the University of Rochester Medical Center. “This study identifies a few viable candidates that show promise against one form of the disease.”
Scientists Pinpoint Earliest Steps of Common Form of Muscular Dystrophy
Thursday, August 19, 2010
Nearly two decades after they identified the specific genetic flaw that causes a common type of muscular dystrophy, scientists believe they have figured out how that flaw brings about the disease. The finding by an international team of researchers, including scientists at the University of Rochester Medical Center, settles a longstanding question about the roots of facioscapulohumeral muscular dystrophy or FSHD. The work was published online August 19 in the journal Science Mag.
Unraveling how the genetic defect causes FSHD has been especially challenging for scientists. Unlike with many genetic diseases, their identification of the mutation that is the basis of FSHD did not quickly lead to a deeper understanding of how the disease actually comes about. The lack of clarity has posed a significant barrier to researchers hoping to turn the knowledge of the genetic flaw into significant progress for patients.
Acupuncture’s Molecular Effects Pinned Down
Sunday, May 30, 2010
Scientists have taken another important step toward understanding just how sticking needles into the body can ease pain.
In a paper published online May 30 in Nature Neuroscience, a team at the University of Rochester Medical Center identifies the molecule adenosine as a central player in parlaying some of the effects of acupuncture in the body. Building on that knowledge, scientists were able to triple the beneficial effects of acupuncture in mice by adding a medication approved to treat leukemia in people.
The new findings add to the scientific heft underlying acupuncture, said neuroscientist Maiken Nedergaard, M.D., D.M.Sc., who led the research. Her team is presenting the work this week at a scientific meeting, Purines 2010, in Barcelona, Spain.
URMC’s First Chief of Child Neurology Dies
Monday, May 24, 2010
Frederick A. Horner, M.D., the first chief of Child Neurology at the University of Rochester School of Medicine and Dentistry, died April 20, 2010, at the age of 90.
Dr. Horner graduated in 1947 from the University of Rochester School of Medicine and Dentistry and went on to complete a pediatric internship and an assistant residency here at Strong Memorial Hospital. After specialty training elsewhere, he joined the faculty in 1968 to become the first chief of Child Neurology at the University of Rochester.
Dr. Horner is survived by his wife, Marjorie; sister, Kathryn Altmas; brother, David Horner; nieces and nephews. Services will be private. Contributions in memory of Dr. Horner may be made to the Dr. Frederick A. Horner Social Work Emergency Fund, University of Rochester, P.O. Box 270032, Rochester, NY 14627.
URMC Named Batten Disease Center of Excellence
Wednesday, May 12, 2010
The largest Batten Disease research and support organization in North America named the University of Rochester Medical Center as a Batten Disease Center of Excellence today. The Ohio-based organization, Batten Disease Support and Research Association, has chosen URMC because of its comprehensive services for patients and its long clinical and research history with the disease.
Batten Disease is a rare neurodegenerative syndrome that erupts with little warning. It first steals sight, then cripples cognitive and motor capacities, and while different variations of the disease brings a difference age of onset and progression, it is, ultimately, terminal. The most common form is juvenile, in which symptoms begin between 5 and 8 years of age. There are between 500 and 1,000 people with Batten Disease in the United States and only a few thousand in the world.
"Finding treatment with a comprehensive team that has experience with the disease is incredibly hard for families," said Jonathan Mink, M.D., Ph.D., chief of Child Neurology and professor of Neurology, Neurobiology & Anatomy and Pediatrics at URMC. "The Batten Disease Support and Research Association is hoping to streamline families' search for expertise by endorsing centers like ours."
URMC Named Batten Disease Center of Excellence by BDSRA
Wednesday, May 12, 2010
Lance Johnston, Executive Director of the BDSRA, awarding Dr. Jonathan Mink with the Batten Disease Center of Excellence plaque.
The largest Batten Disease research and support organization in North America named the University of Rochester Medical Center (URMC) as a Batten Disease Center of Excellence today. The Ohio-based organization, Batten Disease Support and Research Association, has chosen URMC because of its comprehensive services for patients and its long clinical and research history with the disease.
Batten Disease is a rare neurodegenerative syndrome that erupts with little warning. It first steals sight, then cripples cognitive and motor capacities, and while different variations of the disease brings a difference age of onset and progression, it is, ultimately, terminal. The most common form is juvenile, in which symptoms begin between 5 and 8 years of age. There are between 500 and 1,000 people with Batten Disease in the United States and only a few thousand in the world.
Finding treatment with a comprehensive team that has experience with the disease is incredibly hard for families,
said Jonathan Mink, M.D., Ph.D., chief of Child Neurology and professor of Neurology, Neurobiology & Anatomy and Pediatrics at URMC. The Batten Disease Support and Research Association is hoping to streamline families’ search for expertise by endorsing centers like ours.
Variations in Decisions for Care of Patients with Brain Injury “Disturbing”
Wednesday, May 12, 2010
Treatment decisions involving patients with severe brain injury vary widely between medical institutions, and appear to be more driven by hospital and physician practices and priorities. In an article appearing today in the New England Journal of Medicine, physicians at the University of Rochester Medical Center argue that providers must take steps to develop a process of communication and decision-making that gives greater weight and voice to the informed preferences of patients and their families.
"The decision whether or not to continue aggressive medical treatment for patients with severe brain injury requires tough discussions about the benefits and burdens," said URMC neurologist Robert Holloway, M.D., co-author of the article. "Such decisions are often made without a clear understanding of the patient's medical prognosis and with suboptimal input from the patient and family. The possibility that decisions of this magnitude are being overly influenced by factors other than patient values and preferences informed by an understanding of the medical options and potential outcomes should make us cringe."
Heart Drug Effective for Treating Symptom of Muscular Dystrophy
Tuesday, May 4, 2010
A medication most often used to treat heart arrhythmias also reduces a central symptom of myotonic dystrophy, the most common type of muscular dystrophy in adults. The findings about the medication mexiletine -- a chemical cousin of lidocaine -- were published May 4 in the journal Neurology, a publication of the American Academy of Neurology.
Currently there is no drug approved to treat myotonic dystrophy, an inherited disease that is marked by progressive muscle weakness. While the course of the disease can vary dramatically from patient to patient, symptoms besides weakness can include muscle stiffness, difficulty speaking and swallowing, problems walking, and in some patients, heart problems and cataracts. Physicians estimate that approximately 40,000 Americans have the condition.
URMC Receives $4.5 Million in NYS Stem Cell Grants
Thursday, March 25, 2010
The University of Rochester Medical Center (URMC) has received a total of $4.5 million in funding from the Empire State Stem Cell Board for research in neurological disease, cancer, cardiovascular disease, and bone repair.
“Stem cell and regenerative medicine represents one of the scientific foundations of the Medical Center’s strategic plan for growth in biomedical research,” said Bradford C. Berk, M.D., Ph.D., CEO of URMC. “These grants represent critical resources necessary to advance our understanding of stem cells and bring these discoveries into new therapies for a host of diseases.”
Berk is also a member of Funding Committee of the Empire State Stem Cell Board.
The awards to URMC were part of $34.7 million in grants recently announced by Governor David Paterson. To date, URMC scientists have received $8.1 million in research grants from the Empire State Stem Cell Board.
Hickok Center for Brain Injury hosts Epilepsy Panel
Wednesday, March 17, 2010
The Hickok Center for Brain Injury hosts a free Brown Bag Educational Panel entitled “The Brain – Living With Epilepsy” on Monday, March 29, 2010 at their Rochester Center located at 114 South Union Street, Rochester, NY 14607 from 11:30 a.m. - 1 p.m.
The panel will feature: J. Craig Henry, MD, Assistant Professor of Neurology, Strong Epilepsy Center; A. James Fessler, III, MD, Assistant Professor of Neurology at University of Rochester and Director of Clinical Research and Assistant Director, Strong Epilepsy Center; and Michael Radell, Community Educator & Camp EAGR Director, Epilepsy Foundation of Rochester-Syracuse-Binghamton.
This is the first of four brown bag educational events the Hickok Center will host throughout 2010. Bring your lunch and learn about the medical and social issues of living with epilepsy. If you or someone you love has epilepsy, here is an opportunity to learn and ask questions of area professionals. Lot and street parking available.
Reservations strongly suggested as seating is limited. To make a reservation, please call (585) 271-8640 x207 or email ghewson@hickokcenter.org to reserve a seat.
New Center to Focus on Early Stage Clinical Research
Tuesday, March 2, 2010
A new initiative at the University of Rochester Medical Center will provide academic and industry researchers the expertise and scientific collaboration necessary to conduct early stage clinical studies. The Center for Human Experimental Therapeutics (CHET) represents the first university-based program focused on accelerating the development of novel medical therapies.
This Center consists of both infrastructure and a group of people with decades of combined experience in conducting experimental human therapeutics and running some of the more complex clinical studies in the world,
said URMC neurologist Karl Kieburtz, M.D., director of CHET. It is a unique approach that represents a marriage of scientific expertise and logistical competence, with a focus on the early stage of drug development.
Drug Shows Promise for Huntington’s Disease
Monday, February 8, 2010
An early stage clinical trial of the experimental drug dimebon (latrepirdine) in people with Huntington's disease appears to be safe and may improve cognition. That is the conclusion of a study published today in the Archives of Neurology.
This is the first clinical trial that has focused on what is perhaps the most disabling aspect of the disease,
said University of Rochester Medical Center neurologist Karl Kieburtz, M.D., the lead author of the study. While more investigation needs to be done, these results are encouraging and show, for the first time, a statistically significant benefit in terms of improved cognitive function in patients with Huntington's disease.
Huntington's disease is a progressive neurodegenerative disorder that impacts movement, behavior, cognition, and generally results in death within 20 years of the disease's onset. The disease steadily erodes a person's memory and their ability to think and learn. Over time, this cognitive impairment contributes to the loss of the ability to work and perform the activities of daily life. There are no treatments currently available that effectively alter the course of the disease or improve cognition.
New Multiple Sclerosis Drug has URMC Ties
Friday, January 22, 2010
The Food and Drug Administration has approved the drug fampridine-SR for the treatment of multiple sclerosis. Researchers at the University of Rochester Medical Center (URMC) have been evaluating the effects of the drug in MS for more than 10 years– it is the first medication shown to enhance some neurological functions in people with the disease – and their efforts helped pave the way for today’s action by the FDA.
“This is a good day for people who suffer from multiple sclerosis,” said Andrew Goodman, M.D., chief of the URMC Multiple Sclerosis Center. “Physicians will now have a new tool at their disposal that complements existing disease modifying therapies. For some patients, this drug will be a way to improve walking and help regain some independence in their daily lives.”
Study: Era of Rapid Growth in Biomedical Research Over
Tuesday, January 12, 2010
After a decade of remarkable growth, total annual funding for biomedical research in the U.S. has decelerated and may have even fallen when adjusted for inflation. That is the conclusion of a study today published in the Journal of the American Medical Association.
"The era of rapid expansion in biomedical research funding that began in the 1990's has ended," said Ray Dorsey, M.D., a neurologist at the University of Rochester Medical Center and lead author of the study. "Looking back at this period, one of the striking observations is that while research funding increased, the number of novel treatments entering the market remained steady. If research funding levels are to return to a phase of growth, we should examine funding priorities, particularly in health services research, and barriers to the development of new therapies."
Impact of FDA Safety Warnings Examined
Monday, January 11, 2010
A study published today in the Archives of Internal Medicine examines the impact of a safety warning issued by the Food and Drug Administration for commonly prescribed antipsychotic medications. The results show the warnings resulted in a decline in usage among the elderly with dementia, yet raise the question as to whether the FDA's system of communicating these warnings is sufficiently targeted and effective.
"Because this medication class has limited evidence of benefit among the elderly with dementia and significantly increases their risk of death, the 'right' magnitude of decline in usage is not clear," said University of Rochester Medical Center neurologist Ray Dorsey, M.D., the study's lead author. "More generally, the study raises larger issues about appropriate prescribing, particularly among the elderly, and the need to improve risk communication to patients and providers."
Rochester Neurologist Takes a Lead Role Tackling Charcot-Marie-Tooth
Thursday, December 31, 2009
A Meissner corpuscle, a tiny structure in the skin that allows us to feel light touch. David Herrmann monitors these structures to gauge the extent of a patient's neuropathy.
Neurologist David Herrmann, MBBCh, associate professor of Neurology and of Pathology and Laboratory Medicine at the University of Rochester Medical Center, is taking part in a newly funded nationwide study focusing on a condition known as Charcot-Marie-Tooth disease, a painful nerve condition that affects more than 100,000 Americans.
Herrmann, director of the Peripheral Neuropathy Clinic at Strong Memorial Hospital, is part of a team that has been awarded $6.25 million from the National Institutes of Health. The project is based at Wayne State University in Detroit and includes Herrmann and other collaborators from around the world.
The new funding, part of NIH's Rare Diseases Clinical Research Network, will support the Inherited Neuropathies Consortium for the next five years.
UR Study Reveals Chemo’s Toxicity to Brain, Possible Treatment
Thursday, December 17, 2009
Researchers have developed a novel animal model showing that four commonly used chemotherapy drugs disrupt the birth of new brain cells, and that the condition could be partially reversed with the growth factor IGF-1.
Published early online in the journal Cancer Investigation, the University of Rochester Medical Center study is relevant to the legions of cancer survivors who experience a frustrating decline in cognitive function after chemotherapy treatment, known as chemo brain.
"It is not yet clear how our results can be generally applied to humans but we have taken a very significant step toward reproducing a debilitating condition and finding ways to treat it," said Robert Gross, M.D., Ph.D., professor of Neurology and of Pharmacology and Physiology at URMC and principal investigator of the study.
Rochester Physician Named Editor of Leading Neurology Journal
Thursday, November 5, 2009
A neurologist and epilepsy expert at the University of Rochester Medical Center has been named editor in chief of one of the world's leading journals devoted to issues involving the brain and central nervous system.
Robert A. Gross M.D., Ph.D., professor of Neurology and of Pharmacology and Physiology, was named today to lead the medical journal Neurology, the world's leading clinical neurology journal. As editor, Gross assumes a major leadership role in the world of neurology, helping set the direction and focus for the discipline worldwide. He will contribute to decisions about which issues are of most importance to physicians and patients, and which new findings and new research avenues are most worthy of attention.
Gross has been involved with the journal for 20 years, first as a reviewer, then associate editor for the past eight years. During the last two he has also been deputy editor and most recently served as interim editor in chief.
Gross succeeds another Rochester neurologist, Professor Robert Griggs, M.D., who is now president of the American Academy of Neurology, an association of more than 21,000 neurologists and neuroscience professionals that publishes Neurology. Griggs himself served as the editor of the journal from 1997 to 2007.
Cost Effectiveness of Blood Pressure Device Evaluated
Thursday, October 15, 2009
A study conducted by the University of Rochester Medical Center demonstrates that, for certain patient populations, an experimental device that lowers blood pressure may be a cost effective treatment. The implantable device, called Rheos, is in advanced stages of testing for individuals with drug resistant hypertension.
The study – which appears this month in the Journal of Clinical Hypertension – used data from two large population-based studies and compared the incidence of adverse health events such as stroke and heart attack for groups of individuals with and without the blood pressure lowering benefit of the device. Researchers then projected the health care costs associated with those events over a patient’s lifetime. The results show that if Rheos continues to perform at a level consistent the initial findings in ongoing clinical trials, then the device is a cost effective way to control hypertension.
Our goal was to determine whether or not the benefit of Rheos would offset the higher upfront costs,
said Kate C. Young, Ph.D., MPH, an instructor in the departments of Surgery and Neurology at URMC and lead author of the study. What we found is that the device’s cost effectiveness is dependent upon the degree to which it can reduce blood pressure and the starting point of the patient.
Rochester-Led Parkinson’s Study Pays Off Again, Two Decades Later
Monday, October 12, 2009
Parkinson’s disease progresses more slowly in patients who have higher levels of urate, a chemical that at very high level is associated with gout, scientists have found. While it’s unknown whether the high levels actually somehow protect patients or simply serve as a marker of protection, the finding supports the idea that patients and doctors may one day be able to better predict the course of the illness.
The study, led by scientists at Massachusetts General Hospital and the Harvard School of Public Health and including physicians at the University of Rochester Medical Center, was published online in the Archives of Neurology.
Emmy Awarded to ABC News Primetime
Story Featuring Jonathan Mink, M.D., Ph.D.
Tuesday, September 29, 2009
ABC News was recognized with an Emmy Award from the National Academy of Television Arts and Sciences for a Primetime
story featuring URMC pediatric neurologist Jonathan Mink, M.D., Ph.D. Dr. Mink, a professor of Neurology, Neurobiology & Anatomy, Pediatrics, and Brain & Cognitive Sciences, focuses his research on the function of the basal ganglia in normal control of movement and the pathophysiology of basal ganglia disorders characterized by abnormal involuntary movements.
Genetic Source of Muscular Dystrophy Neutralized
Thursday, July 16, 2009
Researchers at the University of Rochester Medical Center have found a way to block the genetic flaw at the heart of a common form of muscular dystrophy. The results of the study, which were published today in the journal Science, could pave the way for new therapies that essentially reverse the symptoms of the disease.
The researchers used a synthetic molecule to break up deposits of toxic genetic material and re-establish the cellular activity that is disrupted by the disease. Because scientists believe that potentially all of the symptoms of myotonic dystrophy – the most common form of muscular dystrophy in adults – flow from this single genetic flaw, neutralizing it could potentially restore muscle function in people with the disease.
This study establishes a proof of concept that could be followed to develop a successful treatment for myotonic dystrophy,
said URMC neurologist Charles Thornton, M.D., the senior author of the study and co-director of the URMC Wellstone Muscular Dystrophy Cooperative Research Center. It also demonstrates the potential to reverse established symptoms of the disease after they have developed, as opposed to simply preventing them from getting worse.
Study in Nature: MicroRNAs Hold Promise For Treating Diseases in Blood Vessels
Sunday, July 5, 2009
The pictured microRNA molecule (green) may prevent the thickening of blood vessels walls that leads to clogged vessels and heart attacks.
A newly discovered mechanism controls whether muscle cells in blood vessels hasten the development of both atherosclerosis and Alzheimer's disease, according to an article published online today in the journal Nature.
The study was led by the Gladstone Institute of Cardiovascular Disease in San Francisco, with key contributions from the Aab Cardiovascular Research Institute at the University of Rochester School of Medicine and Dentistry.
Thanks to stem cells, humans develop from a single cell embryo into a complex being with about 250 unique cell types. As the fetus develops, cells divide and multiply (proliferate) in many generations and specialize (differentiate) with each generation until millions of functional cells result (bone, nerve, blood, skin, muscle, etc.). To serve specific roles in the body, some stem cells also switch back and forth between primitive, rapidly proliferating precursors and their mature, functioning, non-proliferating counterparts, a quality called plasticity.
Telemedicine Expands Reach of Care for Parkinson’s Patients
Wednesday, June 17, 2009
A unique and innovative telemedicine project is providing distant nursing home patients with Parkinson's disease access to neurologists at the University of Rochester Medical Center. A pilot study of the project -- the results of which were released this month at the International Congress of Parkinson's Disease and Movement Disorders in Paris -- demonstrates that the system can improve the quality of life and motor function of patients.
This study shows that we can effectively deliver care for Parkinson's patients via telemedicine,
said URMC neurologist Ray Dorsey, M.D. This system enables us to reach and provide a high level of care to patients who might otherwise not have access to a specialist.
Dorsey and his colleague Kevin Biglan, M.D. oversee the project and divide patient responsibilities between them. The effort is a joint initiative between URMC and the Presbyterian Home for Central New York in New Harford, a 250 bed nursing home near Utica and about 150 miles from Rochester.
Protein Regulates Movement of Mitochondria in Brain Cells
Monday, June 15, 2009
Scientists have identified a protein in the brain that plays a key role in the function of mitochondria – the part of the cell that supplies energy, supports cellular activity, and potentially wards off threats from disease. The discovery, which was reported today in the Journal of Cell Biology, may shed new light on how the brain recovers from stroke.
Understanding the molecular machinery that helps distribute mitochondria to different parts of the cell has only recently begun to be understood,
said University of Rochester Medical Center neurologist David Rempe, M.D., Ph.D., the lead author of the study. We know that in some disease states that mitochondria function is modified, so understanding how their activity is modulated is important to understanding how the brain responds to a pathological state.
Brain Protein Central to Both Parkinson’s, Drug Addiction Identified
Thursday, April 30, 2009
Scientists have identified a protein that appears not only to be central to the process that causes Parkinson’s disease but could also play a role in muting the high from methamphetamine and other addictive drugs.
The action of the protein, known as organic cation transporter 3 or oct3, fills a longstanding gap in scientists’ understanding of the brain damage that causes symptoms like tremor, stiffness, slowness of movement and postural instability. While these are found mainly in patients with Parkinson’s disease, there are more than three dozen other known causes of this array of symptoms, known as parkinsonism.
In a paper published online this week in the Proceedings of the National Academy of Sciences, scientists at the University of Rochester Medical Center and Columbia University have shown that oct3, a protein that shepherds molecules into and out of cells, plays a critical role, bringing toxic chemicals to the doorstep of the brain cells that die in patients with Parkinson’s disease. The team found that oct3 is involved in the brain’s response to addictive drugs like methamphetamine as well.
URMC Physician Elected President of American Academy of Neurology
Thursday, April 30, 2009
University of Rochester Medical Center neurologist Robert C. Griggs, M.D. has been elected president of the American Academy of Neurology (AAN), the world’s largest professional organization of neurologists.
Griggs, who was elected at the AAN’s annual meeting this week in Seattle, will lead an organization that was established 1948 and consists of more than 21,000 neurologists and neuroscience professionals. Griggs has also served as chair of the AAN Education Committee and editor-in-chief of the Academy’s prestigious scientific journal Neurology for 10 years.
Dr. Griggs is a visionary and has made extraordinary contributions to the field of neurology,
said Catherine M. Rydell, executive director and CEO of the AAN. His decades of leadership with the Academy and the respect of his peers position him well to lead the organization. The AAN relies on outstanding continued leadership as we look ahead toward furthering research and treatments for the neurology patient and professional.
Neurologists Establish Professorship in Honor of Robert J. Joynt
Wednesday, April 29, 2009
Colleagues and friends in the Department of Neurology at the University of Rochester Medical Center are more than halfway toward their goal of raising $1.5 million to honor the physician who founded the department.
The professorship will honor neurologist Robert J. Joynt, M.D., Ph.D., one of the most influential neurologists of the last half century, who is now Distinguished University Professor at the University of Rochester Medical Center. Joynt founded the University’s Department of Neurology in 1966 and guided the department for 18 years, laying the foundation for what is today one of the nation’s leading neurology departments.
The professorship, to be known as the Robert J. Joynt Chair in Experimental Therapeutics in Neurology, is designed to further development of treatments to treat neurological diseases. The Joynt Chair will support research to treat disorders like Parkinson’s, Huntington’s, and Alzheimer’s diseases. Friends, alumni, colleagues and grateful patients have contributed to the fund thus far.
Poor Sleep Quality Leads to Poorer Prognosis after Stroke
Tuesday, April 28, 2009
Stroke victims tend to do worse if they also have diagnosed or undiagnosed obstructive sleep apnea prior to having the stroke, according to a study presented April 28, 2009, at the American Academy of Neurology (AAN) annual meeting in Seattle.
Latha Stead, M.D., professor and chair of the Department of Emergency Medicine at the University of Rochester Medical Center, and professor of Neurosurgery, reported the findings at AAN, along with several other stroke studies measuring the factors that lead to a poor prognosis.
We know that obstructive sleep apnea has been linked to a multitude of cardiovascular problems, yet it is concerning that the vast majority of cases remain undiagnosed,
Stead said. In the context of recovering from a stroke, sleep apnea can have a serious impact, and for that reason we encourage people to become more aware of obstructive sleep apnea and to get treatment.
3 Events Offer Hope for People with Brain Tumors
Thursday, April 16, 2009
A PET scan allows doctors to see a brain tumor in an elderly man.
People with brain tumors, and those who love and care for them, will observe Brain Tumor Awareness Week with three educational and celebratory events sponsored by the University of Rochester Medical Center and James P. Wilmot Cancer Center.
On Friday, May 1, there will be a seminar for patients, their families, and physicians that focuses on the latest research and treatment approaches in brain and spinal tumors. Then on Thursday, May 7, patients, families and clinicians will gather for the Community Sharing Hope Picnic at Kings Bend Park in Pittsford. And on Saturday, May 9, there will be an education and supportive program for caregivers.
Each year, approximately 500 people with brain tumors are treated at the Medical Center and Wilmot Cancer Center, making it the largest program in the region. The events are offered by the Program for Brain and Spinal Tumors at the Medical Center and the Wilmot Cancer Center.
Rochester Scientist Wins Major Award for Alzheimer’s Research
Wednesday, April 15, 2009
A Rochester researcher whose work has opened up a whole new avenue in Alzheimer’s disease research has received a major prize from the American Academy of Neurology.
Berislav Zlokovic, M.D., Ph.D., director of the Center for Neurodegenerative and Vascular Brain Disorders at the University of Rochester Medical Center, will receive the 2009 Potamkin Prize for Research in Pick’s, Alzheimer's, and Related Diseases during the AAN annual meeting later this month in Seattle.
Zlokovic will split the $100,000 prize with two other researchers, Michael Wolfe, Ph.D., of Brigham and Women’s Hospital and Harvard Medical School, and Robert Vassar, Ph.D., of Feinberg School of Medicine at Northwestern University. The prize, which honors researchers for their work on Alzheimer’s disease and related disorders, will go toward the investigators’ Alzheimer’s research.
Oxycodone Effective Against Shingles Pain
Wednesday, March 25, 2009
The painkiller oxycodone is effective at treating the acute pain of shingles, an illness that often causes severe pain which can become long-lasting and sometimes even permanent.
The study, published in the April issue of the journal Pain, is one of the first to carefully evaluate different methods to relieve pain during a course of shingles, which many patients say causes the worst pain they have ever experienced. Effective pain treatment is crucial. Not only can the pain of shingles disrupt people’s quality of life, but it is also possible that the less effectively the pain is treated, the more likely it will become a long-term problem that can change a person’s life forever.
Abnormal EKG Can Predict Death in Stroke Patients
Friday, March 20, 2009
People who suffer an ischemic stroke and also have an abnormality in the heart’s electrical cycle are at a higher risk of death within 90 days than people who do not have abnormal electrical activity at the time of emergency treatment, according to new research.
The study also provides a threshold at which the threat of death is highest: QTc intervals greater than 440 milliseconds in women and 438 milliseconds in men have the worst prognosis. The findings are published online March 20, 2009, in the Journal of Stroke and Cerebrovascular Diseases.
Weighing the Options after Life-Altering Stroke
Thursday, March 12, 2009
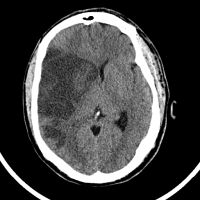
Choosing to have aggressive brain surgery after suffering a severe stroke generally improves the patients' lives and allows them to live longer, according to research by neurologists at the University of Rochester Medical Center.
The findings should help patients and families put into perspective a decision that is nearly always painful and difficult to make – whether putting a patient through aggressive surgery after a catastrophic stroke is worth it.
For families facing this difficult choice, the more information we can provide, the better for their decision-making,
said neurologist Adam G. Kelly, M.D., who has helped hundreds of families chart a course after severe stroke. Kelly presented the findings last month at the International Stroke Conference in San Diego.
Long-Term Effects of Early Parkinson’s Treatments Similar
Tuesday, March 10, 2009
A study published online today in the Archives of Neurology involving two common drugs used to treat early-stage Parkinson's disease shows that, while the drugs each have advantages and disadvantages, the overall impact tends to even out over a long period of treatment.
Clinicians and patients often struggle with what is the right initial approach to treating Parkinson's disease,
said University of Rochester Medical Center neurologist Kevin Biglan, M.D., M.P.H., the lead author of the paper and a member of the Parkinson's Study Group, an international network of researchers that oversaw the clinical trial. This study tells us that, over the long haul, patients on the different drugs end up at roughly the same place in terms of their level of disability and quality of life.
Event to Benefit Those Affected by Neuromuscular Disorders
Monday, February 16, 2009
An arts and crafts show to be held in Batavia later this month will benefit patients and their families who have been affected by neuromuscular disorders like neuropathy, muscular dystrophy, and amyotrophic lateral sclerosis (Lou Gehrig’s disease).
The show will be from 9 a.m. to 5 p.m. Saturday, Feb. 28, at the Batavia Holiday Inn at 8250 Park Road, immediately off Thruway Exit 48. Admission is free.
Tingling Hands, Burning Feet? Rochester Neurologist an Expert in Tracking Down Neuropathy
Monday, January 5, 2009
Hands that feel like they're burning; feet that make it feel like you're walking on pins and needles; numbness that spreads gradually up the limbs. These are among the most vexing of symptoms for patients and their doctors alike. Many patients spend years going from doctor to doctor seeking a diagnosis, and many doctors order test upon test, with no firm conclusion.
Now a Rochester neurologist has helped compile a national set of guidelines that aim to help doctors better diagnose the most common cause of such symptoms more quickly and efficiently and with less expense.
David Herrmann, MBBCh, director of the Peripheral Neuropathy Clinic at Strong Memorial Hospital, is an author of the guidelines for a painful nerve condition known as neuropathy, which affects millions of people with diabetes and many other patients as well. The new practice parameters were published last month in the journal Neurology.
Two Cardiovascular Proteins Pose a Double Whammy in Alzheimer's
Sunday, December 21, 2008
Amyloid is visible as white around the blood vessels in the brain of a mouse with a condition like Alzheimer's.
Researchers have found that two proteins which work in tandem in the brain's blood vessels present a double whammy in Alzheimer's disease. Not only do the proteins lessen blood flow in the brain, but they also reduce the rate at which the brain is able to remove amyloid beta, the protein that builds up in toxic quantities in the brains of patients with the disease.
The work, described in a paper published online Dec. 21 in the journal Nature Cell Biology, provides hard evidence directly linking two processes thought to be at play in Alzheimer's disease: reduction in blood flow and the buildup of toxic amyloid beta. The research makes the interaction between the two proteins a seductive target for researchers seeking to address both issues.
Scientists were surprised at the finding, which puts two proteins known for their role in the cardiovascular system front and center in the development of Alzheimer's disease.
This is quite unexpected,
said Berislav Zlokovic, M.D., Ph.D., a neuroscientist and a senior author of the study. On the other hand, both of these processes are mediated by the smooth muscle cells along blood vessel walls, and we know that those are seriously compromised in patients with Alzheimer's disease, so perhaps we shouldn't be completely surprised.
Breaking the Silence After a Study Ends
Monday, December 8, 2008
While an estimated 2.3 million people in the U.S. take part in clinical trials every year, there currently exists no formal requirement to inform them of study results; an oversight that leaves participants confused, frustrated, and, in some cases, lacking information that may be important to their health. In an article published today in the Archives of Neurology, researchers at the University of Rochester Medical Center have proposed a novel and effective approach to disseminate the results of clinical trials to study volunteers.
Industry, government, and academic researchers are dependent upon the willing participation of millions of individuals to fill the estimated 50,000 clinical trials conducted every year that evaluate the safety and efficacy of experimental drugs and medical devices.
Researchers are only required to inform participants in instances when new information arises that may affect their willingness to continue participation. However, neither federal guidelines nor institutional review boards generally require disclosure of results at the conclusion of a study -- even if the study is halted. Consequently, many research participants never learn the outcome of studies in which they volunteer.
Individuals who volunteer to participate in clinical research frequently expose themselves to risks, both known and unknown,
said URMC neurologist Ray Dorsey, M.D., the report's author. Because of their participation, they should be informed of the results of these studies in a timely and personalized manner.
URMC Leads Study for New Treatment for Tourette’s
Tuesday, December 2, 2008
The University of Rochester Medical Center is leading a multi-center clinical research study of a new experimental treatment for Tourette’s syndrome. The study will examine whether or not a drug that alters the chemical activity in the brain can alleviate the symptoms of the disease.
Tourette’s syndrome (TS) is a neurological disorder characterized by multiple, repeated tics. These tics generally consist of abrupt and involuntary vocal outbursts or muscular jerks. Symptoms usually begin at an early age and can increase in frequency and severity over time. Many individuals with TS have a mild form of the disease and do not require medical intervention unless the tics interfere with normal daily function. Patients with more severe forms of TS are currently treated with various antipsychotic drugs.
While the precise mechanism that causes Tourette’s is unknown, we have long observed that the neuro-chemical dopamine is overly active in individuals with the disease,
said URMC neurologist Roger Kurlan, M.D., the study’s principal investigator. This chemical imbalance in the brain may play a role in the disease and, consequently, the drugs that are currently used to treat the disease are known to suppress dopamine production. However, these drugs are also associated with severe side effects that often deter their use.
Scientists Exploring New Compounds to Target Muscular Dystrophy
Wednesday, November 19, 2008
The CUG triplet repeat at the root of myotonic muscular dystrophy
Scientists have identified a promising set of new compounds in the fight against muscular dystrophy. Using a drug-discovery technique in which molecules compete against each other for access to the target – the strand of toxic RNA that causes the most common form of muscular dystrophy in adults – a team at the University of Rochester Medical Center has identified several compounds that, in the laboratory, block the unwanted coupling of two molecules that is at the root of the disease.
The work was published online November 7 by the Journal of the American Chemical Society.
This discovery gives us, for the first time, a molecule that targets the wayward RNA at the root of myotonic muscular dystrophy,
said Benjamin Miller, Ph.D., the chemist who led the study. This is a first step toward developing a drug-like molecule that perhaps could be used someday to treat the disease. This lead molecule provides a framework for moving forward.
Researchers Identify Toehold for HIV’s Assault on Brain
Friday, November 14, 2008
Scientists have unraveled in unprecedented detail the cascade of events that go wrong in brain cells affected by HIV, a virus whose assault on the nervous system continues unabated despite antiviral medications that can keep the virus at bay for years in the rest of the body.
The new research reveals key steps taken in the brain by Tat, a protein that is central to HIV’s attack on cells called neurons. Researchers discovered the receptor that Tat uses to attack neurons, and they were able to reverse the effects of Tat in the laboratory by blocking the receptor.
The discovery of a major molecular player in the process opens up a new avenue for researchers to explore in their efforts to prevent or treat HIV’s neurological effects, for which there is no currently approved treatment. Researchers say that much of the molecular action that underlies HIV’s attack on the brain also occurs in other diseases, such as Parkinson’s and Alzheimer’s diseases, and that the results spell progress for those conditions as well.
The team from the University of Rochester Medical Center and other institutions published its results online Nov. 13 in the journal PloS One.
Alzheimer's Gene Slows Brain's Ability to Export Toxic Protein
Thursday, November 13, 2008
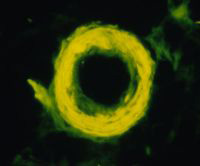
A ring of amyloid in the wall of an arteriole
in the brain of a patient who had Alzheimer's disease
(Courtesy of James M. Powers, M.D.)
The only known genetic risk factor for Alzheimer's disease slows down the brain's ability to export a toxic protein known as amyloid-beta that is central to the damage the disease causes, scientists have found.
The research, published Nov. 13 by the Journal of Clinical Investigation, provides new clues into the workings of a protein known as apolipoprotein E4, or ApoE4. People who carry two copies of the gene have roughly eight to 10 times the risk of getting Alzheimer's disease than people who do not.
The new results are in line with a body of research amassed over the last 15 years by the leader of the team, Berislav Zlokovic, M.D., Ph.D., of the University of Rochester Medical Center, that blood circulation plays a key role in the disease. His team has identified much of the molecular machinery that allows amyloid-beta to sidestep the body's safeguards and enter the brain, and he has discovered molecules that falter when the toxic protein accumulates in the brain.
Our latest findings help explain one of the major risk factors for Alzheimer's disease,
said Zlokovic. ApoE4 changes the brain's ability to rid itself of amyloid-beta. It's becoming more and more apparent that the brain's ability to clear out amyloid-beta, through the vascular system and across the blood-brain barrier, is central to the development of Alzheimer's disease.
Music on My Mind Chamber Orchestra Set to Debut
Tuesday, November 11, 2008
More than 30 health care professionals from throughout the University of Rochester Medical Center are getting ready for their inaugural orchestral performance tomorrow afternoon. The Music on My Mind Chamber Orchestra, which includes a broad cross section of health care disciplines, including an emergency medicine physician, a scientist in the Laboratory for Laser Energetics, and an athletic trainer, will play at 4:30 p.m. Wednesday, Nov. 12 in the Flaum Atrium.
Conducted by David Harman, who also conducts the University of Rochester’s Symphony Orchestra and Chamber Orchestra, as well as the Penfield Symphony and the Rochester Philharmonic Youth Orchestra, the group will perform selections by Mozart, Beethoven and von Weber.
Pearson Lands Two National Leadership Appointments
Friday, November 7, 2008
International heart and stroke prevention expert Thomas Pearson, M.D., Ph.D., has been tapped by two national organizations to lead efforts aimed at decreasing the incidence of two of the nation's leading causes of death and disability: cardiovascular disease and stroke. Pearson is the Albert D. Kaiser Professor in the Department of Community and Preventive Medicine and Professor of Medicine at the University of Rochester School of Medicine and Dentistry.
For the past three decades, Pearson has been a driving force behind the development of many of our nation's policies and guidelines as they relate to heart disease and stroke. He has participated on dozens of policy panels for national organizations including The National Institutes of Health, the Centers for Disease Control and Prevention, the Institute of Medicine, the American College of Cardiology and the American Heart Association.
URMC Expert on Stroke to Give Free Talk
Wednesday, October 15, 2008
Curtis Benesch, M.D., director of the Strong Stroke Center at the University of Rochester Medical Center, will give a free talk on Treatment and Prevention of Stroke
from 4 to 5:30 p.m. Monday, Nov. 3, at the Hahnemann Club, 301 Stoutenburgh Lane, located on the campus of The Highlands at Pittsford, off of Route. 31, just east of the village Pittsford.
Benesch will discuss how to recognize the symptoms of a stroke, what to do when those symptoms occur and how to prevent a stroke in high-risk individuals. Also discussed will be the treatment of acute stroke and the many ways patients can decrease their risk.
Neurologist to Discuss Pioneering Stem Cell Research
Friday, October 3, 2008
Steven Goldman, M.D., Ph.D., professor and chair of the Department of Neurology, will discuss his pioneering efforts to use stem cells to treat human disease as part of a lecture series highlighting biological and biomedical research at the University of Rochester.
Goldman will speak at 4 p.m. Friday, Oct. 10, in the Class of 1962 Auditorium at the Medical Center. It's the latest installment of the Second Friday Science Social
lecture series geared mainly to faculty, staff and students at the University, though the general public is welcome as well.
Goldman, who is also professor of Neurosurgery, is internationally recognized for advancing our understanding of stem cells and their use to treat human disease. He began his studies of the brain's stem cells more than 25 years ago, and his doctoral thesis in 1983 was the first report of neurogenesis -- the production of new brain cells -- in the adult brain and opened the door to the idea of neural stem cells as the source.
Out of Iraq Emerges Hope for Those with the Severest of Head Injuries
Wednesday, September 24, 2008
There may be more hope than has been recognized for some people with severe brain injuries, according to a U.S. neurosurgeon who earlier this year spent four months in Iraq treating soldiers and civilians. Jason Huang, M.D., this week presented his results from his experience in Iraq at the annual meeting of the Congress of Neurological Surgeons in Orlando, Fla.
Huang discussed blast injuries, a type of wound that has affected thousands of U.S. soldiers and others in Iraq. The term includes injuries caused by roadside bombs or improvised explosive devices (IEDs
), as well as car bombs, suicide bombs, and other blasts.
This is a type of injury unlike anything seen regularly here in the United States,
said Huang, an assistant professor of Neurosurgery at the University of Rochester Medical Center who is also a major in the U.S. Army Reserve.
Here we might see gunshot wounds to the head, or severe injuries from motor vehicle accidents, but we don't see blast injuries, and so neurosurgeons haven't really had much experience treating them. What we're seeing in Iraq is different even from injuries suffered by soldiers in previous wars. The extent of the blast injuries was far worse than I ever would have imagined,
Huang said.
Rochester Neuroscientist Honored By Danish Academy
Tuesday, September 23, 2008
Maiken Nedergaard, M.D., D.M.Sc., has been elected a member of the Royal Danish Academy of Sciences, the premier scientific society in Denmark. The society elects only six new members worldwide every other year.
Nedergaard has been a pioneer in brain research, demonstrating that brain cells known as astrocytes play a role in a host of human diseases. For decades, much of the attention of neuroscientists had been focused on brain cells known as neurons, which send electrical signals. Astrocytes were long considered cells whose primary function was to support the neurons.
Nedergaard has turned that notion on its head, showing that astrocytes themselves play an important role in epilepsy, spinal cord disease, migraine headaches, stroke, and Alzheimer's disease.
Researchers Disclose Key Advance in Treating Spinal Cord Injuries
Friday, September 19, 2008
Researchers in Rochester, NY and Colorado have shown that manipulating stem cells prior to transplantation may hold the key to overcoming a critical obstacle to using stem cell technology to repair spinal cord injuries.
Research from a team of scientists from the University of Rochester Medical Center and the University of Colorado Denver School of Medicine, published online today in the Journal of Biology, may lead to improved spinal cord repair methods that pave the way for victims of paralysis to recover the use of their bodies without the risk of transplant-induced pain syndromes.
The research focuses on a major support cell in the central nervous system called astrocytes. When nerve fibers are injured in the spinal cord, the severed ends of the nerve fibers fail to regenerate and re-connect with the nervous system circuitry beyond the site of the injury. During early development, astrocytes are highly supportive of nerve fiber growth and scientists believe that, if properly directed, these cells could play a key role in regenerating damaged nerves in the spinal cord.
University of Rochester and The Highlands at Pittsford Present To Your Health!
Friday, September 19, 2008
The free To Your Health! series featuring health experts from the University of Rochester Medical Center resumes in September, with programs offering advice on learning more about your health and preventing and treating common age-related health issues.
Offered at convenient times, the afternoon programs are taught by URMC’s distinguished physicians and other providers affiliated with Strong Memorial Hospital, Highland Hospital, the Eastman Dental Center, Visiting Nurse Service and other affiliates of the Medical Center.
All lectures through November will be held at the Hahnemann Club, 301 Stoutenburgh Lane, located on the campus of The Highlands at Pittsford, off of Rt. 31, just east of the village of Pittsford. The Club is an ideal setting for learning and socializing with curious, like-minded peers, and parking is conveniently located right outside the clubhouse, along the street.
All seminars are free but registration is limited. Register by calling 585-275-2838.
Gelbard Named Director of Center for Neural Development and Disease
Thursday, September 18, 2008
Harris A. Gelbard, M.D., Ph.D., professor of neurology, pediatrics and of microbiology and immunology, has been named director of the Center for Neural Development and Disease at the University of Rochester Medical Center.
The center, which brings together a broad array of physicians and scientists, targets a complex system rather than a single disease. Center researchers investigate stroke, traumatic brain injury, brain tumors, nerve injuries, HIV-1 associated neurologic disorders, Alzheimer's and other diseases with the goal of creating treatments and therapies.
We think it is most crucial to understand the development of the nervous system — how it is put together — so we can better understand how diseases of the brain and peripheral nervous system take away function,
said Gelbard. This kind of understanding is what translates into treatments and better care.
Steven Goldman to Lead University’s Department of Neurology
Thursday, September 4, 2008
After an extensive national search, a neurologist who is a leading international figure in efforts to use stem cells to treat human disease has been tapped to lead the Department of Neurology at the University of Rochester Medical Center.
Steven Goldman, M.D., Ph.D., a professor of Neurology who has been with the University since 2003, will become the Edward A. and Alma Vollertsen Rykenboer Professor of Neurophysiology Chair, Department of Neurology within the School of Medicine and Dentistry beginning October 1. He will lead a department known nationally for its research and the education it provides its students and young doctors.
Dr. Goldman’s efforts will be central to the advancement of the field of neuromedicine, an area we’ve targeted in our strategic plan for significant growth and future investment in faculty and resources,
said Bradford C. Berk, M.D., Ph.D., Medical Center CEO. His experience as an outstanding researcher and clinician is a perfect fit for the position.
Wilmot Cancer Center Answers Calls to Stand up to Cancer Sept. 4
Wednesday, September 3, 2008
Doctors from the James P. Wilmot Cancer Center will answer questions about cancer screening, diagnoses, treatment and ways to reduce your risk during a special call-in program set from 5 to 6:30 p.m. Thursday, Sept. 4. The event is part of the Wilmot Cancer Center’s participation in the national Stand Up To Cancer effort.
URMC & NIH Partner to Expand, Accelerate Clinical Research in Neurological Diseases
Thursday, August 14, 2008
The University of Rochester Medical Center and the National Institute of Neurological Disorders and Stroke are hosting a week-long training session designed to create a new generation of researchers with the specialized skills necessary to conduct clinical trials in neurological disorders.
The session, which is titled the Clinical Trial Methods Course in Neurology,
is part of a push on the part of the National Institutes of Health to beef up the nation’s translational research capabilities by increasing the ranks of clinical researchers and focusing more resources on clinical research skills, technologies, and systems that will accelerate medical discoveries.
Neurological disorders are a critical area of need in terms of expanding our ability to design and conduct trials that have maximum efficiency at the lowest possible cost,
said URMC neurologist Bernard Ravina, M.D., the director of the course. Participants in this course consist of a select group of individuals who are committed to being clinical researchers and conducting clinical trials and will benefit from hands-on training that they really cannot get anywhere else.
AHA Recognizes Quality of URMC Cardiac, Heart Failure, Stroke Programs
Tuesday, July 15, 2008
The American Heart Association/American Stroke Association has honored Strong Memorial Hospital of the University of Rochester Medical Center with a Triple Performance Achievement Award for meeting its high standards for coronary artery disease, heart failure and stroke care.
Strong Memorial is the only Rochester-area hospital to receive this honor, and the only Rochester-area hospital to receive any level of American Heart Association recognition for its coronary artery disease and heart failure care.
The achievements of Strong Memorial in three program modules of the AHA/ASA Get With the Guidelines program consist of: coronary artery disease and stroke care, which each earned a Gold Sustained Performance Award to celebrate two or more years of adherence to all measures of AHA/ASA performance standards; and heart failure care, which received a Silver Performance Achievement Award for 12 consecutive months of compliance of performance measures.
Quick Formula Could Forecast Which Cancers Chemo Could Kill
Tuesday, July 15, 2008
Researchers at the University of Rochester Medical Center have coined a simple formula that predicts how well a certain chemotherapy will work for targeting brain and other nervous system cancers. The formula, which will publish in mid-July in Cancer Chemotherapy and Pharmacology, is pegged to two important proteins that compose such hard-to-kill tumors – one of which, ironically, makes them so drug-resistant in the first place.
We’re unraveling the mysterious, even paradoxical, ways chemotherapies interact with various cancers,
said one of the study’s investigators Nina F. Schor, M.D., Ph.D., the William H. Eilinger professor and chair of the Department of Pediatrics at Rochester. From this, we’re developing techniques that will help us more quickly predict which medicines are most effective for each tumor.
Doctors Testing New Treatments for Lower Back Pain
Wednesday, June 11, 2008
Physicians are testing two drugs approved to treat other conditions to see whether they might also help patients who have severe pain in their lower back and in their legs. The research studies at the University of Rochester Medical Center are part of an effort to come up with new treatments for pain caused by a condition known as lumbar spinal stenosis. Doctors are looking for up to 75 people to take part in the studies.
Lumbar spinal stenosis is the most common reason that people older than 65 choose to have back surgery. Nerve roots in the spinal canal are put under pressure as age causes the bones in our back to degenerate. The pressure on the nerves results in pain, sometimes very severe, in the lower back and the legs when patients stand or walk.
Doctors turn to a variety of drugs to treat the pain, but no drug has ever been proven to relieve the pain effectively. Even the most effective solution, surgery, does not significantly relieve pain in approximately one-third of patients. A study recently published in the New England Journal of Medicine found that the pain relief experienced by many patients after surgery often did not translate into better mobility and function in their daily lives.
Neurologist John Markman, M.D., assistant professor and director of Translational Pain Research in the Department of Neurosurgery, designed the new studies to study the benefit of non-surgical treatments.
World Experts in Specialized Radiation Therapy to Gather at URMC
Wednesday, June 11, 2008
Cancer survivor Jarod Finlay will share his experiences as the first patient to undergo an investigational procedure – stereotactic body radiation therapy – during a conference of world experts on the procedure this Friday and Saturday at the University of Rochester Medical Center.
Finlay, who had metastatic tumors in his lungs, received the groundbreaking therapy more than seven years ago when his doctors treated his lung tumors using technology originally designed to destroy brain tumors. This technique and scientists’ research to support its expanded use will be discussed by more than 100 experts attending the Scientific Conference on Stereotactic Body Radiation Therapy. Finlay will deliver the opening address by describing his care and perspective.
Human Stem Cells Show Promise Against Fatal Children’s Diseases
Wednesday, June 4, 2008
Scientists have used human stem cells to dramatically improve the condition of mice with a neurological condition similar to a set of diseases in children that are invariably fatal, according to an article in the June issue of the journal Cell Stem Cell.
With a one-time injection of stem cells just after birth, scientists were able to repair defective wiring throughout the brain and spinal cord – the entire central nervous system – of mutant shiverer mice,
so called because of the way they shake and wobble. The work marks an important step toward the day when stem cells become an option for the treatment of neurological diseases in people.
Neuroscientists at the University of Rochester Medical Center injected a type of fetal human stem cell known as glial stem cells into newborn mice born with a condition that normally claims their lives within about 20 weeks of birth, after a lifetime of seizures and other serious consequences. While most of the 26 mice that received transplanted glial stem cells still died, a group of six lived far beyond their usual lifespan, and four appeared to be completely cured – a first for shiverer mice. The scientists plan to gather more evidence before trying the approach in sick children.
It’s extremely exciting to think about not only treating but actually curing a disease, particularly an awful disease that affects children,
said neurologist Steven Goldman, M.D., Ph.D., a leader in manipulating stem cells to treat diseases of the nervous system.
Conference to Highlight Rochester Stem Cell Research
Monday, May 12, 2008
A half-day symposium showcasing research in the field of stem cell biology at the University of Rochester will be held on May 23. The symposium, titled Frontiers in Stem Cell Medicine,
is being sponsored by the University’s Clinical and Translational Science Institute and the Stem Cell and Regenerative Medicine Institute.
Speakers at the symposium include: biomedical geneticist Mark Noble, Ph.D., director of the Stem Cell and Regenerative Medicine Institute; neurologist Steven Goldman, M.D., Ph.D., chief of the Division of Cell and Gene Therapy; cancer researcher Craig Jordan, Ph.D., director of Translational Research for Hematologic Malignancies at the James P. Wilmot Cancer Center; Edward Puzas, Ph.D., with the Department of Orthopaedics, and Rocky Tuan, Ph.D., chief of the Cartilage Biology and Orthopaedics Branch of the National Institute of Arthritis and Musculoskeletal and Skin Diseases.
May 1 Picnic to Celebrate Brain Tumor Awareness Week
Wednesday, April 30, 2008
Brain tumor survivors and their families, friends and University of Rochester Medical Center staff will celebrate Brain Tumor Awareness Week with a picnic from 5 to 8 p.m. Thursday, May 1, at Kings Bend Park in Pittsford.
Many in attendance at the picnic will be members of Brainstormers and the Adult Brain Tumor Network at Strong Memorial Hospital and the James P. Wilmot Cancer Center, which provide support for brain cancer survivors and their families. Every year, more than 185,000 people will be diagnosed with brain tumors in the United States.
Brain Tumor Care, Treatment in Spotlight
Thursday, April 24, 2008
Patients, physicians, and those caring for loved ones with brain tumors will have an opportunity to attend two full days of programs hosted by health care professionals from the University of Rochester Medical Center. The efforts, co-sponsored by the James P. Wilmot Cancer Center, are offered through the recently enhanced brain tumor treatment program at the University, where approximately 500 brain tumor patients are treated each year.
A seminar Saturday, April 26, will focus on people caring for patients with brain tumors. One week later, on Friday, May 2, another full-day session is geared toward patients, their families, and physicians, covering the latest research and treatment approaches in brain and spinal tumors.
Neurologist Wins Fellowship to Support Parkinson’s Research
Thursday, April 24, 2008
A physician at the University of Rochester Medical Center has been recognized for her work aiming to ease the side effects of medications widely used to treat patients with Parkinson's disease.
Michelle Burack, M.D., Ph.D., instructor of Neurology and Pediatrics, received a clinical research training fellowship from the American Academy of Neurology. The fellowship covers her salary and related costs for two years.
Burack is studying ways to try to alleviate some of the troublesome consequences of treatment that many patients with Parkinson's disease face. The disease is marked by shaky, stiff and slow movements, a result of the death of key nerve cells in the brain known as dopamine neurons. Early treatment with a medication designed to boost the amount of the signaling molecule dopamine in the brain is usually very effective.
Promising Parkinson's Finding Spurs New Clinical Study
Tuesday, April 15, 2008
The progression of Parkinson’s disease is slower in patients who have high blood levels of urate, a close chemical cousin of the molecule that causes gout, researchers have found. The finding could lead to a way to predict how a given patient with the disease will fare, and it opens the door to a new approach for treating or preventing the disease.
The findings were made public - posted online by the Archives of Neurology on April 14 - the same day that the Michael J. Fox Foundation announced a new study aimed at slowing the disease by continuing the research in people. The foundation is funding a $5.6 million study, the largest award in the foundation’s history, to investigate the potential of boosting urate levels to slow or stop the disease.
The project is being led by physicians at Harvard and Massachusetts General Hospital together with neurologists at the University of Rochester Medical Center.
Leaky Blood Vessels Open up Nerve Cells to Toxic Assault In Lou Gehrig’s Disease
Monday, April 7, 2008
Leaky blood vessels that lose their ability to protect the spinal cord from toxins may play a role in the development of amyotrophic lateral sclerosis, better known as ALS or Lou Gehrig’s disease, according to research published in the April issue of Nature Neuroscience.
The results mark the first time that scientists have witnessed molecular changes occurring long before key nerve cells start dying. The unexpected finding opens up a new front in studies of ALS, a disease in which motor neurons in the spinal cord die off for unknown reasons, resulting in dramatically weakened muscles. Patients lose their strength, their ability to move or swallow, and eventually lose their ability even to breathe. Most patients live only a few years after diagnosis.
We believe these changes contribute to or possibly initiate the onset of ALS,
said lead author Berislav Zlokovic, M.D., Ph.D., of the University of Rochester Medical Center. It’s clear that these changes occur before the loss of neurons, and it’s well known that the types of changes we are seeing certainly injure or kill these types of cells, which are extremely sensitive to their biochemical environment.
Stopping a Receptor Called 'Nogo' Boosts the Synapses
Tuesday, March 18, 2008
Changing dendritic spines on a neuron - evidence of brain rewiring
New findings about a protein called the nogo receptor are offering fresh ways to think about keeping the brain sharp. Scientists have found that reducing the nogo receptor in the brain results in stronger brain signaling in mice, effectively boosting signal strength between the synapses, the connections between nerve cells in the brain. The ability to enhance such connections is central to the brain's ability to rewire, a process that happens constantly as we learn and remember. The findings are in the March 12 issue of the Journal of Neuroscience.
The work ties together several research threads that touch upon the health benefits of exercise. While those benefits are broadly recognized, how the gains accrue at a molecular level has been largely unknown. The new research gives scientists a way to produce changes in the brain that mirror those brought about by exercise, by reducing the effect of the nogo receptor.
The find comes as a surprise, because for much of the last decade, the nogo receptor has been a prime target of researchers trying to coax nerves in the spinal cord to grow again. They named the protein after its ability to stop neurons from growing. Its action in the brain has not been a hot topic of study.
Friday Open House for New Neurology Outpatient Clinic
Wednesday, March 12, 2008
The Department of Neurology is holding an open house for its new outpatient clinic located on the first floor of the Ambulatory Care building. The open house will be held on Friday, March 14 from 11:00 a.m. to 1:00 p.m.
This new clinic is the culmination of years of growth and planning and will now enable us to provide our patients with the level of care they require in a setting that is far more convenient and designed to their needs,
said Robert C. Griggs, M.D., chair of the Department of Neurology.
Our Understanding of Movement Is on the Move
Monday, January 14, 2008
How our brain controls our movements is a bit more complex and varied than scientists have previously recognized, according to research recently published in Science by a team of scientists and physicians at the University of Rochester Medical Center.
The team led by neurologist Marc Schieber, M.D., Ph.D., professor of Neurology and of Neurobiology & Anatomy, showed that at least occasionally, the brain is able to bypass the usual route of nerve fibers it uses for controlling hand and finger movements, using an alternate route to send its signals. Such flexibility in controlling movement has been suspected but not actually shown before.
Copper Damages Protein that Defends Against Alzheimer’s
Wednesday, November 7, 2007
The research by neuroscientists at the URMC was presented at the annual meeting of the Society for Neuroscience in San Diego Nov. 3-7. The work was highlighted as part of a press conference on potential environmental influences on Alzheimer's disease.
The team found that copper damages a molecule known as LRP (low-density lipoprotein receptor-related protein), a molecule that acts like an escort service in the brain, shuttling amyloid-beta out of the brain and into the body. The molecule's role in Alzheimer's was revealed more than a decade ago by another author of the work, Berislav Zlokovic, M.D., Ph.D., professor of Neurosurgery and Neurology and director of the Frank P. Smith Laboratory for Neuroscience and Neurosurgery Research. Zlokovic is widely recognized for demonstrating that blood vessels, blood flow, and the blood-brain barrier are central to the development of Alzheimer's disease.
Study of New Epilepsy Treatment Underway at URMC
Saturday, September 15, 2007
The University of Rochester Medical Center is participating in a multi-center study of a new medical device to treat epilepsy. The Rochester study is being overseen by neurologists Michel Berg, M.D. and James Fessler, M.D., and neurosurgeons Web Pilcher, M.D., Ph.D. and Jason Schwalb, M.D.
Uncontrolled seizures related to epilepsy are generally treated with medications,
said Berg, medical director of the Strong Epilepsy Center. However, many individuals treated with medication alone continue to experience seizures or have unacceptable medication side effects. If these patients are not candidates for epilepsy surgery, then options to effectively control their seizures are limited.
Study of New Epilepsy Treatment Underway at URMC
Friday, September 14, 2007
The University of Rochester Medical Center is participating in a multi-center study of a new medical device to treat epilepsy. The Rochester study is being overseen by neurologists Michel Berg, M.D. and James Fessler, M.D., and neurosurgeons Web Pilcher, M.D., Ph.D. and Jason Schwalb, M.D.
Uncontrolled seizures related to epilepsy are generally treated with medications,
said Berg, medical director of the Strong Epilepsy Center. However, many individuals treated with medication alone continue to experience seizures or have unacceptable medication side effects. If these patients are not candidates for epilepsy surgery, then options to effectively control their seizures are limited.
The Responsive Neurostimulator System (RNS) is an implantable device that is designed to suppress seizures in patients with epilepsy before any symptoms appear, much like implantable cardiac pacemakers are intended to detect abnormal heart rhythms and then deliver electrical stimulation to correct them. Neuropace, the California-based developer and manufacturer of the RNS system, is funding the trial. URMC is one of 28 centers across the country testing the new technology.
Alzheimer’s Project Focuses on Role of Brain Inflammation
Thursday, August 30, 2007
Scientists at the University of Rochester Medical Center have received $1.37 million to continue their work looking at some of the earliest events that occur at the start of Alzheimer's disease - a condition that now generally goes undetected until the death of key brain cells has been underway for decades.
The team led by William Bowers, Ph.D., associate professor of Neurology and a scientist in the Center for Neural Development and Disease, is focusing on the role of inflammation in the evolution of the disease. Just as rheumatoid arthritis can ravage the body's joints because of the inflammation it causes, scientists are realizing that the same thing happens to the brain in patients with Alzheimer's disease. The brain can be under assault for decades as the body attempts to fend off some perceived threat.
Rochester Awarded New MS Research Center
Monday, June 12, 2006
A new research center whose scientists are working on better ways to treat multiple sclerosis has been established in Rochester by the National Multiple Sclerosis Society.
The University of Rochester Medical Center is bringing together experts who normally focus on Alzheimer’s disease, HIV vaccines, and spinal cord repair, as well as multiple sclerosis, in a unique center designed to stimulate MS research by drawing on the expertise of scientists from a wide array of disciplines. The new Collaborative Multiple Sclerosis Research Center Award – the only one in the nation established by the society this year – is headed by neurologist Benjamin Segal, M.D., associate professor of Neurology and director of Neuroimmunology Research. Segal has enlisted several of his colleagues to direct their attention on new ways to investigate the disease.
Also taking part in the project are neurologists Steven Schwid, M.D., and Andrew Goodman, M.D., who have extensive experience with clinical trials in MS; and Howard Federoff, M.D., Ph.D., and Tim Mosmann, Ph.D., who head research centers in aging and in vaccine biology, respectively.
New Findings About Brain's 'Compass' Offer Clues About Alzheimer's
Thursday, March 28, 2002
A tiny section of the brain that is ravaged by Alzheimer's disease is more important for our ability to orient ourselves than scientists have long thought, helping to explain why people with the disease become lost so easily. The findings by neuroscientists at the University of Rochester Medical Center are reported in the March 29 issue of Science.
Neurologist Charles Duffy, M.D., Ph.D., previously discovered that a small section of brain tissue slightly above and behind the ear - known as the medial superior temporal area (MST) - acts much like a compass, instantly updating your mental image of your body's movements through space. In new research, Duffy and graduate student Michael Froehler show that the MST acts not only as a compass but also as a sort of biological global positioning system, providing a mental map to help us understand exactly where we are in the world and how we got there.
Road Skills Hint At "Motion Blindness" Of Alzheimer's
Thursday, January 31, 2002
Doctors have added to the evidence that patients with Alzheimer's disease lose their way not simply because their memory is failing but because they are subject to a unique form of brain damage that causes symptoms doctors call "motion blindness." Some of the new data comes from driving tests of a small number of patients, where researchers have linked the condition to the loss of one specific driving skill: the ability to stay in one's lane while driving.
While it's obvious that people with Alzheimer's disease are losing their memory, that's only part of the reason why they become lost,
says neurologist Charles Duffy, M.D., Ph.D., who leads the research team at the University of Rochester Medical Center. These patients also lose their ability to perceive their own motion. That's ultimately what puts them at much greater risk than others of becoming lost.
New Mouse Marks Latest Stride in Muscular Dystrophy Research
Thursday, September 7, 2000
Most days, neurologist Charles Thornton, M.D., spends some time away from his patients and heads for the laboratory, where he works with mice. It might seem an unlikely action for a doctor ultimately concerned with human health. But his forays in the laboratory have helped Thornton and his team develop a new kind of mouse that may someday help doctors around the world treat patients with myotonic dystrophy, the most common form of muscular dystrophy in adults.
Two Scholars Win Sloan Fellowships
Tuesday, April 18, 1995
Charles J. Duffy, professor of neurology and ophthalmology, and Turan Erdogan, assistant professor of optics, have been awarded 1995 Sloan Research Fellowships.
The two University of Rochester professors were among 100 scientists and economists selected from a field of 400 nominees. Each Sloan Research Fellowship recipient is awarded $30,000 over a two-year period. Sloan Research Fellows are engaged in pioneering research in physics, chemistry, computer science, mathematics, neuroscience and economics. Once they have been selected, Fellows are free to pursue whatever line of inquiry interests them. The Alfred P. Sloan Foundation created the fellowship program in 1955 to encourage research by young scholars at a critical time in their careers.